US Pharm. 2015;40(2):44-48.
ABSTRACT: Digoxin, a cardiac glycoside, has inotropic effects in addition to effects on cardiac output. It is used to treat heart failure and atrial fibrillation and has other off-label uses. Digoxin has been shown to reduce hospitalization rates without affecting mortality rates in patients with heart failure. Digoxin is effective for rate control in patients with atrial fibrillation, but its influence on mortality rates is a source of controversy. The use of digoxin is limited because the drug has a narrow therapeutic index and requires close monitoring. Digoxin can cause many adverse events, is involved in multiple drug interactions, and can result in toxicity. Despite its limitations, however, digoxin has a place in therapy.
Digoxin is a cardiac glycoside derived from the purple foxglove flower. In 1785, the English chemist, botanist, and physician Sir William Withering published his findings that Digitalis purpurea could be used to treat cardiac dropsy (congestive heart failure; CHF).1 Digoxin has been in use for many years, but was not approved by the FDA for treatment of heart failure (HF) until the late 1990s.2,3 Another FDA indication for digoxin is atrial fibrillation (AF).3 Digoxin also has numerous off-label uses, such as in fetal tachycardia, supraventricular tachycardia, cor pulmonale, and pulmonary hypertension.3
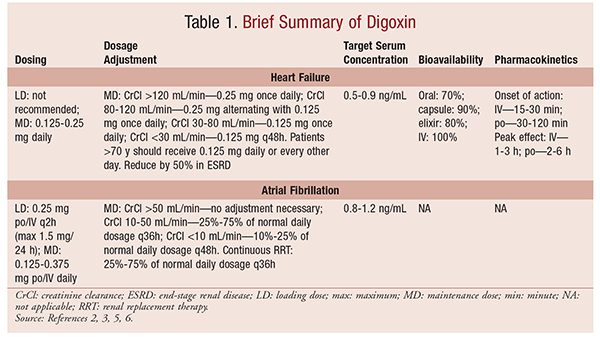
Digoxin acts by inhibiting the sodium-potassium adenosine triphosphatase pump, promoting sodium-calcium exchange; this results in an upsurge of intracellular calcium, thereby increasing myocardial contractility. Digoxin also has parasympathomimetic properties. By increasing vagal tone in the sinoatrial and atrioventricular (AV) nodes, it slows the heart rate and AV nodal conduction.4 TABLE 1 provides a brief overview of digoxin.
Digoxin has been around for centuries, but its use has been limited by several factors. Because of its narrow therapeutic window, digoxin requires close monitoring. Also, two major drawbacks of digoxin are its adverse effects (AEs) and multiple drug interactions. Despite these limitations, digoxin still plays a role in therapy for HF, AF, and several off-label uses. It is considered adjunctive therapy, rather than first-line therapy, for these indications.5,6
According to current guidelines, digoxin may be used as additive therapy with beta-blockers and/or ACE inhibitors/angiotensin receptor blockers (ACEIs/ARBs) in the management of CHF.5 Digoxin possesses negative chronotropic properties and has been shown to decrease morbidity in patients with AF. It is used mainly as add-on therapy in AF patients whose heart rates are not adequately controlled on beta-blockers alone.6 Because of its positive inotropic effects, digoxin may have benefits in pulmonary arterial hypertension (PAH), but more studies are needed to assess long-term effects in this patient population.7
Digoxin and HF
CHF is a myocardial dysfunction caused by the contractile performance of the heart, ventricular relaxation/filling of the heart, or both. In CHF, contractility is decreased, which in turn reduces cardiac output. Digoxin is effective in patients with CHF because of its positive inotropic properties. Although studies have shown that digoxin reduces hospitalizations and improves symptoms of HF, it has not been proven to decrease mortality.
Digoxin’s role in HF has been assessed in numerous trials. One double-blind, controlled trial of digoxin for CHF treatment randomized subjects with cardiac dysfunction to digoxin or placebo for 7 weeks.8 Placebo subjects deteriorated more quickly than those taking digoxin. Cardiac function, as measured by ejection fraction (EF), was significantly improved in digoxin patients.8 Many other clinical trials showed that digoxin’s positive inotropic effects were useful in the management of CHF.
According to the 2013 American College of Cardiology Foundation/American Heart Association (ACCF/AHA) guideline on managing HF, digoxin improves symptoms, quality of life, and exercise tolerance in patients with mild-to-moderate HF, regardless of the underlying rhythm (normal sinus rhythm or AF).5 Therefore, digoxin may be considered as add-on therapy for patients who have persistent symptoms of HF despite treatment with ACEI/ARBs and/or beta-blockers. Digoxin may also be considered in patients with stage C HF (structural heart disease with prior or current symptoms of HF) or stage D HF (HF symptoms at rest and recurrent hospitalizations despite therapy). HF patients should not take digoxin without an ACEI or beta-blocker. Although digoxin is prescribed for patients with HF and AF, concomitant beta-blocker therapy is usually more effective at controlling ventricular response, particularly during exercise.5,6
The initial dosage of digoxin is 0.125 mg to 0.25 mg by mouth daily. The dosage must be adjusted based on renal function and age (TABLE 1). The target serum level of digoxin in HF is 0.5 ng/mL to 0.9 ng/mL.5
Morbidity and Mortality in HF
Digoxin has been shown effective for decreasing HF symptoms, and its effect on morbidity and mortality has been assessed as well. A randomized, double-blind, placebo-controlled trial was conducted to examine mortality and morbidity in HF patients with a left ventricular EF of 0.45 who were receiving digoxin therapy.9 There were no baseline between-group differences, and follow-up was a mean of 37 months. The primary outcome was mortality; secondary outcomes were a composite of mortality from cardiovascular causes, death from worsening HF, and hospitalization for other causes (digoxin toxicity). In the intent-to-treat analysis, there were 1,181 deaths in the digoxin group and 1,194 deaths in the placebo group (34.8% vs. 35.1%, 95% CI 0.91-1.07, P = 0.8 [nonsignificant]). Fewer digoxin patients than placebo patients were hospitalized (910 and 1,180, respectively; risk ratio 0.72, 95% CI 0.66-0.79, P <.001). Also, the risk associated with the combined outcome of death due to worsening HF or hospitalization was lower in the digoxin group (1,041 vs. 1,291, P <.001). The conclusion was that although digoxin had no effect on overall mortality, it significantly decreased the overall number of hospitalizations attributed to worsening HF.9
Digoxin and AF
AF is a common arrhythmia in which irregular electrical impulses are conducted through the heart. These irregular electrical impulses lead to uncoordinated and inefficient heart contractions. As a result, blood pools in the heart, increasing the likelihood of a blood clot, which may lead to serious consequences such as myocardial infarction or stroke. AF can be managed by utilizing either rate or rhythm control agents. Digoxin exhibits its benefit in AF by controlling the heart rate.6
One multicenter, randomized, double-blind, crossover trial evaluated the benefit of digoxin versus placebo in 43 patients with paroxysmal AF.10 Patients were aged 18 years and had one or more symptomatic episodes of self-terminating AF per month. The study endpoint was time to occurrence of one or two AF episodes as documented by patient-activated monitors. The median time to two episodes was 13.5 days for placebo and 18.7 days for digoxin (P <.05). The median time to one episode was 3.5 days for placebo, compared with 5.4 days for digoxin (P <.05). Mean ventricular rates during an AF episode were 138 ± 32 beats per minute (bpm) and 125 ± 35 bpm on placebo and digoxin, respectively (P <.01). It was concluded that digoxin reduced the frequency of symptomatic AF episodes and that the effect, although small, may be due to a reduction in ventricular rate rather than an antiarrhythmic action.10
A recent retrospective cohort study of 122,465 newly diagnosed AF patients (mean age 72 years) found a higher cumulative mortality rate in those treated with digoxin than in those who were untreated (P <.001).11 Digoxin treatment was an independent predictor of mortality despite confounders such as age, kidney function, drug adherence, and history of cardiovascular complications.11 The impact of digoxin on mortality in AF patients needs further investigation.
According to the ACCF/AHA guideline, clinical results with regard to symptoms are similar whether AF is managed by rate control or rhythm control.6 Although symptom relief is comparable with both methods, rhythm-control therapy confers increased exercise tolerance. Digoxin is one of the medications used to manage heart rate, which is considered controlled when the ventricular response is 60 to 80 bpm at rest and 90 to 115 bpm during moderate exercise. First-line therapies for rate control include diltiazem, verapamil, esmolol, and other beta-blockers.6 Compared with digoxin, these medications have stronger recommendations and better evidence. Digoxin is not considered first-line therapy, owing to its narrow therapeutic index (which requires monitoring) and numerous drug interactions. Patients at higher risk for digoxin toxicity (i.e., renal impairment, elderly, multiple drug interactions) should be monitored more frequently than healthy, young patients with no comorbidities or concomitant medications.
Digoxin and PAH
PAH is a progressive disease in which restricted blood flow through the pulmonary arteries leads to increased pulmonary vascular resistance and, ultimately, right HF. PAH is defined by an increase in pulmonary arterial pressure of >25 mmHg at rest or 30 mmHg with exercise.7 Current treatment options for PAH include supportive therapy and concurrent medications including digoxin, diuretics, warfarin, and calcium channel blockers (CCBs).
Pulmonary hypertension is often associated with neurohormonal sympathetic activation, so digoxin may be used because of its sympatholytic properties. Current PAH guidelines briefly mention the use of digoxin for its beneficial effects on cardiac output and on circulating norepinephrine. Hence, the use of digoxin in PAH patients is based on the physician’s clinical judgment.11 The use of digoxin in PAH has not been evaluated extensively, and its mechanism of action is unknown.12,13 No prospective, randomized trials have been conducted.13,14
Warnings and Precautions
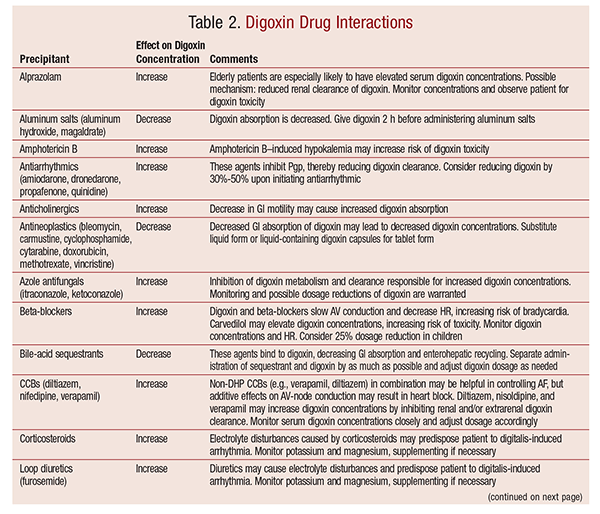
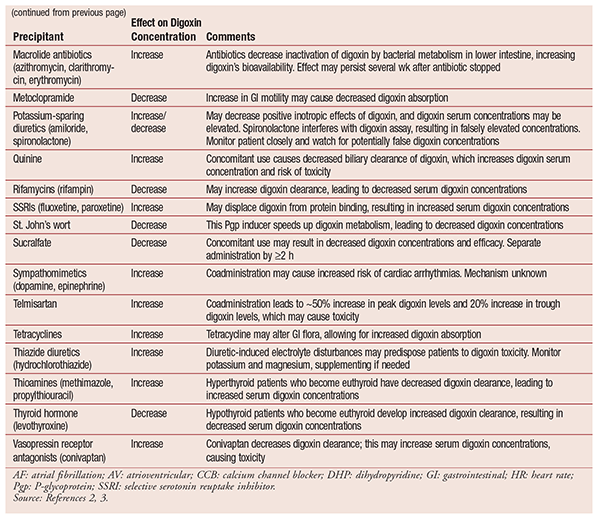
Patients with significant sinus or AV block should not be given digoxin without first having a permanent pacemaker implanted. Digoxin should be used with caution with other agents that can depress sinus or AV nodal function (e.g., beta-blockers, nondihydropyridine CCBs). Digoxin also has numerous other drug interactions, which are outlined in TABLE 2. Clinicians should be aware of such interactions and monitor for digoxin toxicity, as well as check levels frequently.5
If administered with careful attention to dosage and factors that may alter the drug’s metabolism, digoxin is well tolerated by most patients with HF.15 AEs occur mainly when digoxin is administered in higher dosages, especially in the elderly, and it should be noted that larger dosages have not been found clinically beneficial.5
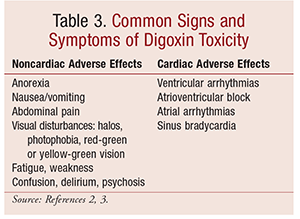
The major AEs of digoxin (TABLE 3) include cardiac arrhythmias (ectopic and heart block), gastrointestinal symptoms (nausea, vomiting, anorexia), and neurologic complaints (visual disturbances, disorientation, confusion). Although overt digoxin toxicity occurs when serum levels are >2 ng/mL, toxicity may occur with lower digoxin levels, especially if electrolyte abnormalities such as hypokalemia and hypomagnesemia coexist.5
Digoxin Toxicity
Owing to its narrow therapeutic index, digoxin toxicity is quite common. Clinical manifestations of acute digoxin toxicity include arrhythmias, anorexia, confusion, and hyperkalemia.3 Chronic digoxin toxicity presents similarly, with the addition of halos, green-yellow vision, blindness, lethargy, and fatigue (TABLE 3).3 Digoxin-specific antibody (DigiFab) is used to treat digoxin poisoning. DigiFab binds to free digoxin, forming a complex that is excreted renally, thereby reducing serum digoxin concentrations.3
Conclusion
The use of digoxin has been limited because the agent has a narrow therapeutic index and requires close monitoring. Digoxin can lead to many AEs and has multiple drug interactions. Despite its limitations, digoxin still has a place in therapy for HF, AF, and numerous off-label uses. It is considered adjunctive therapy, rather than first-line therapy.
REFERENCES
1. Withering W. An Account of the Foxglove and Some of Its Medical Uses: With Practical Remarks on Dropsy, and Other Diseases. Birmingham, England: M. Swinney; 1785.
2. Maron BA, Rocco TP. Pharmacotherapy of congestive heart failure. In: Brunton LL, Chabner BA, Knollmann BC, eds. Goodman & Gilman’s The Pharmacological Basis of Therapeutics. 12th ed. New York, NY: McGraw-Hill; 2011.
3. Micromedex Healthcare Series: DRUGDEX System. Digoxin. Greenwood Village, CO: Truven Health Analytics; 2013.
4. Ehle M, Patel C, Giugliano RP. Digoxin: clinical highlights: a review of digoxin and its use in contemporary medicine. Crit Pathw Cardiol. 2011;10:93-98.
5. Yancy CW, Jessup M, Bozkurt B, et al. 2013 ACCF/AHA guideline for the management of heart failure: a report of the American College of Cardiology Foundation/American Heart Association Task Force on practice guidelines. Circulation. 2013;128:e240-e327.
6. Fuster V, Rydén LE, Asinger RW, et al. ACC/AHA/ESC guidelines for the management of patients with atrial fibrillation. Circulation. 2001;104:2118-2150.
7. Rich S, Seidlitz M, Dodin E, et al. The short-term effects of digoxin in patients with right ventricular dysfunction from pulmonary hypertension. Chest. 1998;114:787-792.
8. Guyatt GH, Sullivan MJ, Fallen EL, et al. A controlled trial of digoxin in congestive heart failure. Am J Cardiol. 1988;61:371-375.
9. Digitalis Investigation Group. The effect of digoxin on mortality and morbidity in patients with heart failure. N Engl J Med. 1997;336:525-533.
10. Murgatroyd FD, Gibson SM, Baiyan X, et al. Double-blind placebo-controlled trial of digoxin in symptomatic paroxysmal atrial fibrillation. Circulation. 1999;99:2765-2770.
11. Turakhia MP, Santangeli P, Winkelmayer WC, et al. Increased mortality associated with digoxin in contemporary patients with atrial fibrillation: findings from the TREAT-AF study. J Am Coll Cardiol. 2014;64:660-668.
12. British Cardiac Society Guidelines and Medical Practice Committee. Recommendations on the management of pulmonary hypertension in clinical practice. Heart. 2001; 86(suppl 1):i1–i13.
13. Barst RJ, Gibbs JS, Ghofrani HA, et al. Updated evidence-based treatment algorithm in pulmonary arterial hypertension. J Am Coll Cardiol. 2009;54:S78-S84.
14. Humbert M, Sitbon O, Simonneau G. Treatment of pulmonary arterial hypertension. N Engl J Med. 2004;351:1425-1436.
15. Steiner JF, Robbins LJ, Hammermeister KE, et al. Incidence of digoxin toxicity in outpatients. West J Med. 1994;161:474-478.
To comment on this article, contact rdavidson@uspharmacist.com.





