US Pharm. 2018;43(6):15-18.
ABSTRACT: Hyperhidrosis, or excessive sweating, is a medical condition that adversely affects the patient’s daily life. The current goal in working with patients with hyperhidrosis is to recommend effective coping skills and treatment options. Diagnosis is made primarily through patient history and physical examination; however, laboratory studies may reveal the distribution and severity of the condition. Treatment options are typically based on the condition’s severity and the appropriateness for the patient. Therapy generally consists of antiperspirants or anticholinergics, but surgical intervention may be required in severe cases. Management depends on the type of hyperhidrosis and the extent of the signs and symptoms, and it should be tailored to the patient.
Many people live daily with the symptom of excessive sweating. Hyperhidrosis is excessive sweating that is usually unrelated to heat or exercise.1 Although sweating is a normal bodily function, excessive sweating is the production of sweat in amounts exceeding the body’s requirement for normal thermoregulation processes. Nearly 5% of the world’s population has hyperhidrosis.2
Hyperhidrosis may be classified as primary or secondary.3,4 In primary hyperhidrosis, the patient is considered healthy and has no underlying conditions that could contribute to the excessive sweating.4 Secondary hyperhidrosis, which is less common, may be caused by certain drugs, neurologic disorders or other systemic diseases, or anxiety. Complications in patients with hyperhidrosis may be physical (e.g., infection caused by increased moisture on the skin) or psychological (e.g., embarrassment and anxiety about potential body odor or sweat spots on clothing).2 Treatment options for hyperhidrosis are generally effective; however, severe cases may require surgical removal of sweat glands or disconnection of the nerves responsible for sweating.2
Symptoms
Sweating is a normal bodily function that helps regulate the temperature of the body.2 The sweating experienced with hyperhidrosis far exceeds normal sweating.2 Often, individuals with hyperhidrosis experience noticeable symptoms that may have an impact on their social life, including a whitish discoloration of the skin, skin peeling, and skin infections.2 Symptoms are usually dependent on the type of hyperhidrosis the person has. Although primary and secondary hyperhidrosis are symptomatically similar, there are some distinct differences between them. The sweating that takes place in primary hyperhidrosis is typically described as focal, meaning that it affects only one or a few areas of the body.4 These areas are generally symmetrical and most commonly include the underarms, hands, and/or feet.4 The sweating that occurs with primary hyperhidrosis typically occurs while the individual is awake.4 The sweating that takes place in secondary hyperhidrosis presents over the entire body while the individual is sleeping.1
Causes and Complications
Hyperhidrosis involves the overproduction of sweat. The causes of primary hyperhidrosis are poorly understood; however, studies have indicated that genetics may play a role.1,5 A family history of primary hyperhidrosis is seen in an average of 65% of cases, which suggests that the condition is linked to a genetic disorder.5 Secondary hyperhidrosis has been associated with a variety of known causes.5 Associated underlying medical conditions include diabetes, frostbite, gout, head trauma, menopause, overactive thyroid, pregnancy, and opioid withdrawal. Additionally, some medications, such as antidepressants (e.g., venlafaxine), acetylcholinesterase inhibitors (e.g., donepezil), pilocarpine, and propranolol, have been shown to cause excessive sweating.1,3,5
The complications of hyperhidrosis are very well defined. Untreated hyperhidrosis may lead to finger and toenail infections, warts, bacterial infections (i.e., around hair follicles and between the toes), and heat rash.2,5 The psychological impact of excessive sweating usually involves the patient’s self-confidence, personal relationships, and social life. In some cases, patients can become socially withdrawn, emotionally stressed, and sometimes depressed.1,5 Studies have shown that, on average, individuals live with hyperhidrosis for 9 years before seeking medical assistance.5 Therefore, it is vital to spread hyperhidrosis awareness to enable patients to obtain appropriate treatment.
Diagnosis
Patients presenting with signs and symptoms of hyperhidrosis should be evaluated to determine whether they have primary hyperhidrosis or secondary hyperhidrosis. Gathering a comprehensive history—age at onset, family history, impact on quality of life, the time of day that sweating occurs, current medications, existing disease states, and pattern and location of sweating—is the best way to start when diagnosing an individual with hyperhidrosis.6 Primary hyperhidrosis often occurs early in life, with a mean age of onset of 14 years.7,8 Primary hyperhidrosis is diagnosed by the presence of visible, excessive sweating on specific areas of the body, including the axillae, palms, soles, and craniofacial regions, for at least 6 months without an underlying cause.9 Additionally, the patient must present with at least two of the following: symmetrical presentation, impaired activities of daily living, occurrences more than once a week, onset before age 25 years, positive family history, or excessive sweating not happening while asleep.9
The impact of hyperhidrosis on a patient’s daily activities can be determined by the Hyperhidrosis Disease Severity Scale. This four-point questionnaire rates the severity of hyperhidrosis as never interfering, sometimes interfering, frequently interfering, or always interfering with daily activities.6,10 There is currently no confirmatory laboratory test for hyperhidrosis; however, ruling out other disease states can aid diagnosis.3 The Minor starch-iodine test and gravimetric analysis may be administered to glean information on the location of the sweating and the rate of sweat production.8,9 In the Minor starch-iodine test, a 3.5% iodine and alcohol solution is applied to clean, hairless skin, followed by the application of dry starch powder. Sites that turn blue indicate areas affected by sweat.9 Gravimetric analysis is performed by placing filter paper over the affected area for 60 seconds and then measuring the filter paper to determine how much sweat was collected during that time.9
Treatment
The United States currently has no guidelines for treating hyperhidrosis. However, the International Hyperhidrosis Society offers treatment algorithms for primary axillary hyperhidrosis, primary craniofacial hyperhidrosis, generalized or multiple focal area of hyperhidrosis, gustatory hyperhidrosis (Frey syndrome), primary palmar hyperhidrosis, and primary plantar hyperhidrosis.11 Proper treatment depends on the region(s) affected and potential treatment risks and benefits.6 A variety of treatments are available for hyperhidrosis, including topical, oral, and injectable forms and medical devices.6 See FIGURE 1 for a treatment algorithm for hyperhidrosis.
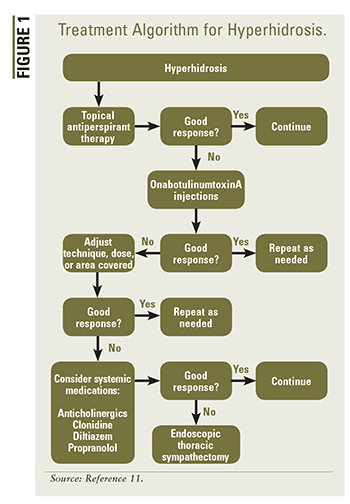
Topical aluminum salts, which are considered first-line treatment for axillary hyperhidrosis, are thought to work by blocking the distal eccrine sweat-gland ducts.6 Aluminum chloride is available OTC in several strengths ranging from 12% to 25%.9 Xerac AC, Drysol, and Hypercare are topical-solution forms of aluminum chloride hexahydrate used to treat palmar, axillary, and plantar hyperhidrosis.6,9 To avoid possible skin irritation, it is important to counsel patients using high concentrations of aluminum chloride to apply it to dry skin at bedtime and wash it off 6 to 8 hours later.9 If skin irritation persists, it is recommended that hydrocortisone cream be applied the morning prior to bedtime application of aluminum chloride.6 Notably, the use of aluminum chloride has been associated with the development of breast cancer and Alzheimer’s disease; however, the evidence is inconclusive.3 Topical glycopyrrolate 0.5% may be used in patients experiencing gustatory hyperhidrosis (sweating of the forehead, face, scalp, and neck soon after ingesting food) from Frey syndrome or secondary to diabetes.9
Patients with axillary hyperhidrosis who are unresponsive to topical therapies may consider botulinum toxins as an alternative.9 OnabotulinumtoxinA (Botox) is an FDA-approved intradermal injection used for primary axillary hyperhidrosis. Botulinum toxins may also be used for the treatment of palmar hyperhidrosis.9 Treatment consists of 50 U injected intradermally in each axilla in multiple sites 1 to 2 cm apart, and the dose remains effective for up to 16 weeks.9,12 As with many injections, the most common side effect is injection-site pain. This effect can be minimized by applying ice or topical anesthetics approximately 45 minutes prior to the procedure or diluting the botulinum toxin with lidocaine.9
An iontophoresis device may be used to treat severe cases of idiopathic palmar, plantar, and axillary hyperhidrosis.9 The device delivers an ionized substance into the skin via electric current and is believed to work by inhibiting sympathetic nerve transmission, obstructing sweat glands with ion deposits, and altering pH, which, in turn, inhibits sweat glands.6 Iontophoresis treatment consists of eight initial sessions followed by as-needed maintenance sessions.6 Common adverse effects from this therapy include discomfort, vascularization, and erythema.6
The newest treatment for axillary hyperhidrosis, named miraDry, is a handheld device that destroys sweat glands via electromagnetic therapy.3 This noninvasive procedure corrects both hyperhidrosis and body odor.13 Some patients see results after one treatment, although most patients require two treatments administered 3 months apart.13
Several oral anticholinergic agents are used in the treatment of hyperhidrosis, the most common ones being oxybutynin, glycopyrrolate, and benztropine.14 In order to have an effect on sweating, most of these medications have high dosage requirements; therefore, the potential for anticholinergic side effects may be a concern.9 Class-wide effects patients may experience include constipation, blurry vision, dry mouth, and urinary retention. There is no superior anticholinergic drug for treating hyperhidrosis, so selection of therapy should take into account side effects of the medication, the patient’s existing medical conditions and current medications, and, in some cases, the patient’s preference. Anticholinergic therapy should be a last resort for elderly patients because of the risk of dementia development, and patients with gastric-emptying issues, glaucoma, and/or urinary retention should not be started on an anticholinergic agent.14 Both oxybutynin and glycopyrrolate are available in liquid formulations, which are useful for children and adults with difficulty swallowing.14
According to the International Hyperhidrosis Society, beta-blockers and benzodiazepines are effective for treating episodic or event-driven hyperhidrosis.14 Propranolol is the most common beta-blocker, but it should be used with caution in patients with cardiac conditions, elderly patients, and diabetic patients because it can mask symptoms of hypoglycemia in diabetic patients. Common side effects of propranolol include fatigue, dizziness, hypotension, and constipation. Sweating due to stage fright would the best indication for propranolol, and benzodiazepines help lessen sweating caused by acute anxiety.14 Lorazepam, oxazepam, and temazepam are preferred in elderly patients because these drugs have shorter half-lives and, therefore, shorter-acting side effects. Benzodiazepines often cause sedation, fatigue, and confusion, and they have high abuse and dependence potential.14
None of the oral medications has a specific indication for hyperhidrosis, and no standard treatment guidelines with dosages are available. The physician should start with a low dose and titrate up until the desired effect has been achieved, being careful not to exceed the maximum allowable dose for the medication. Endoscopic thoracic sympathectomy, which entails cutting the nerves to the part of the body that sweats too much, such as the face or palms, may be used in severe cases.2
Prevention
The key to preventing hyperhidrosis is the avoidance of sweat triggers. Triggers include excessive heat, spicy foods, stress, alcohol, caffeine, tobacco, monosodium glutamate (occurring naturally in foods such as tomatoes and cheese), exercise, and medications.1,8 Minimizing the consumption of trigger foods and beverages decreases the incidence of overproduction of sweat. Although stress can be a trigger for hyperhidrosis, relaxation techniques, such as meditation and yoga, have minimal to no effect on prevention.15 Given that certain medications and medical conditions are common causes of secondary hyperhidrosis, it is important to request a list of the patient’s current medications and review it for drugs that could potentiate hyperhidrosis as an adverse effect.16 Patients who are unwilling to seek pharmacologic interventions may benefit from a discussion of the use of an antiperspirant rather than a deodorant.1
For individuals who experience nighttime sweats, Wicked Sheets and Cool-jams offer sheets that can keep the person cool and wick away moisture throughout the night.17 Other companies, such as Thompson Tee and Sutran Garments, offer sweat-proof clothing designed to block underarm sweat, odor, and staining.17 Similar to the wicking sheets, these garments will not prevent hyperhidrosis, but they may improve the individual’s quality of life and minimize embarrassment over underarm odor and stains. Persons who experience excessive sweating of the soles of the feet should take precautions against athlete’s foot by wearing sandals and clean, moisture-wicking socks.17 They should also avoid wearing the same pair of shoes for consecutive days, in order to allow adequate drying time.1 It is important to note that these preventive methods will not rid the individual of hyperhidrosis, but they may be beneficial as add-on therapy to the previously discussed treatment options.
Conclusion
Both primary and secondary hyperhidrosis cause excessive sweating that can affect patients’ quality of life. Although the pathophysiology of hyperhidrosis is not fully understood, numerous treatment options are available. Pharmacists can be helpful in directing patients toward OTC treatment options, and they can also recognize potential disease states and medications that may contribute to secondary hyperhidrosis. Helping patients and clinicians become more aware of the disease and treatment options can help reduce patients’ physical and psychological complications.
REFERENCES
1. American Academy of Dermatology. Hyperhidrosis. www.aad.org/public/diseases/dry-sweaty-skin/hyperhidrosis. Accessed February 27, 2018.
2. Cole GW. Hyperhidrosis. www.medicinenet.com/hyperhidrosis/article.htm#hyperhidrosis_facts. Accessed February 27, 2018.
3. American Osteopathic College of Dermatology. Hyperhidrosis. www.aocd.org/?page=Hyperhidrosis. Accessed February 27, 2018.
4. International Hyperhidrosis Society. Focused on sweating? So are we! www.sweathelp.org/. Accessed February 27, 2018.
5. Nordqvist C. What is hyperhidrosis? Medical News Today. www.medicalnewstoday.com/articles/182130.php. Accessed February 27, 2018.
6. Grabell DA, Hebert AA. Current and emerging medical therapies for primary hyperhidrosis. Dermatol Ther (Heidelb). 2017;7:25-36.
7. International Hyperhidrosis Society. Diagnosing hyperhidrosis. https://sweathelp.org/home/diagnosing-hyperhidrosis.html. Accessed February 23, 2018.
8. Benson RA, Palin R, Holt PJ, Loftus IM. Diagnosis and management of hyperhidrosis. BMJ. 2013;347:f6800.
9. DynaMed Plus [online database]. Hyperhidrosis. www.dynamed.com/topics/dmp~AN~T116001/Hyperhidrosis. Accessed February 23, 2018.
10. International Hyperhidrosis Society. Hyperhidrosis disease severity scale. www.sweathelp.org/pdf/HDSS.pdf. Accessed February 16, 2018.
11. International Hyperhidrosis Society. Hyperhidrosis treatment algorithms. www.sweathelp.org/treatments-hcp/clinical-guidelines/hyperhidrosis-treatment-algorithms.html. Accessed April 27, 2018.
12. Lexicomp Online [online database]. OnabotulinumtoxinA. https://online.lexi.com/lco/action/doc/retrieve/docid/patch_f/6465#f_dosages. Accessed February 15, 2018.
13. International Hyperhidrosis Society. miraDry. www.sweathelp.org/hyperhidrosis-treatments/miradry.html. Accessed February 13, 2018.
14. International Hyperhidrosis Society. Medications. www.sweathelp.org/hyperhidrosis-treatments/medications.html. Accessed April 23, 2018.
15. Epocrates [online database]. Hyperhidrosis. https://online.epocrates.com/diseases/85644/Hyperhidrosis/Prevention. Accessed March 12, 2018.
16. International Hyperhidrosis Society. Drugs/medications known to cause hyperhidrosis. www.sweathelp.org/pdf/drugs_2009.pdf. Accessed March 10, 2018.
17. International Hyperhidrosis Society. Fan fave product deals. www.sweathelp.org/taking-action/deals.html. Accessed March 10, 2018.
To comment on this article, contact rdavidson@uspharmacist.com.





