US Pharm. 2013;38(11):51-56.
ABSTRACT: The Diagnostic and Statistical Manual of Mental Health Disorders, Fifth Edition (DSM-5), the authoritative guide for practitioners in establishing diagnoses and seeking reimbursement, was published in May 2013. Previous editions of the handbook established the well-known multiaxial diagnostic system that organized all medical and psychiatric conditions requiring attention by all members of the healthcare team. The new edition includes a number of changes that can affect pharmacy practice—including, but not limited to, the elimination of the multiaxial system. In this article, changes to some of the major mental health conditions are summarized, as well as treatment interventions that may be recommended. Pharmacists should expect prescribing trends to be influenced by DSM-5, so gaining a basic familiarity with these changes is important.
The Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5), which replaces DSM-IV-TR (Fourth Edition, Text Revision; published in 2000), is the authoritative handbook on diagnosis of mental disorders that is used by healthcare professionals in the United States and around the world.1 Published by the American Psychiatric Association (APA) in May 2013, this clinical resource is a guide for practitioners in establishing diagnoses, requesting reimbursement, and—for researchers—investigating and evaluating statistical health outcomes. Treatment recommendations and insurance payments to healthcare providers are often determined by DSM classifications, so the changes reflected in DSM-5 are expected to have significant clinical and practical impact. Prior to publication, critics of DSM-5 developed and circulated a petition, sponsored and signed by many mental health organizations, that called for an outside review of the document.
Insurance Implications
Insurance companies are currently revising their reporting and billing procedures to address the changes detailed in DSM-5. Some companies may require older DSM-IV-TR diagnoses and codes for a while, as guidelines are still being developed by the Centers for Medicaid and Medicare Services (CMS) and private insurers. The CMS has weighed in on these diagnostic inconsistencies and billing concerns, noting that DSM-IV and DSM-5 have been crosswalked to reflect compatibility with the old International Statistical Classification of Diseases, Ninth Revision, Clinical Modification (ICD-9-CM), and the new ICD-10-CM diagnosis codes. The ICD-10-CM codes will be the only accepted HIPAA-adopted standard and will be required for diagnosis reporting for dates of service beginning October 1, 2014. The CMS encourages providers to continue to use DSM-IV/DSM-5 criteria for diagnostic decision making, quality management, and communication with patients. Eventually, the APA will establish a date by which DSM-IV will no longer be acceptable for use by mental health providers. In the meantime, the transition to DSM-5 will include review and revisions of practitioner board-certification examinations and standards to measure quality of medical-record documentation.2
Impact on Medication Therapy
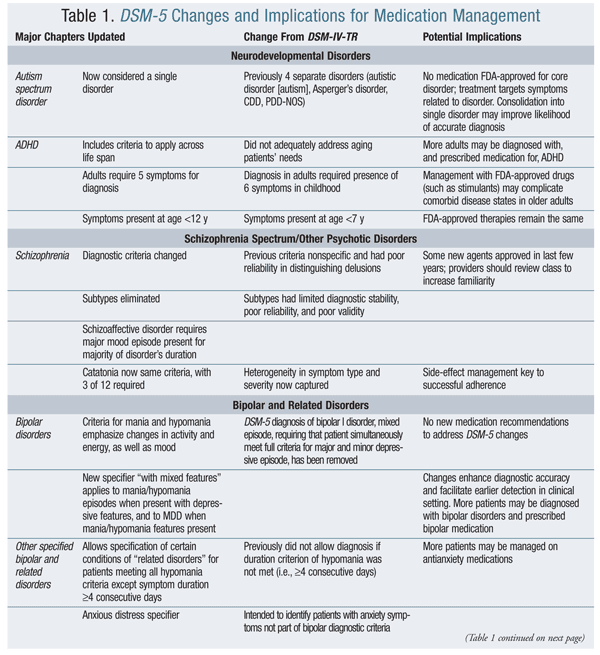
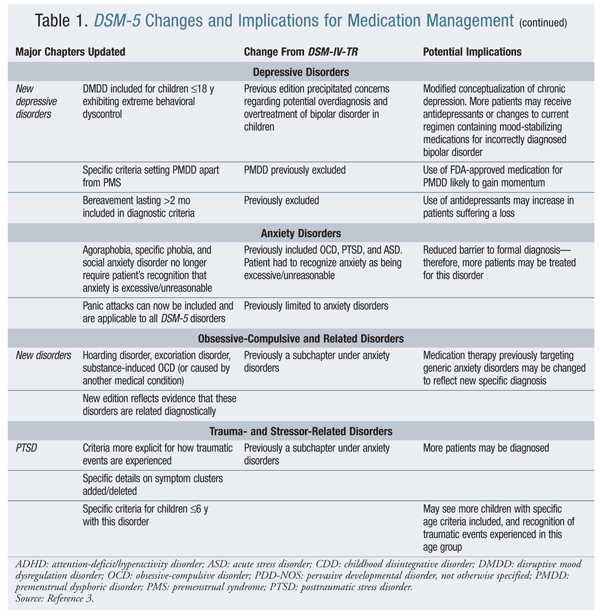
DSM-5 includes a number of new diagnoses, and the diagnoses of some disorders have been combined or eliminated entirely. Most diagnosed mental health conditions are treated based on consensus guidelines and FDA-approved medication therapy; however, for some disorders, there are no formally approved medications to treat the core disorder. Some conditions, despite available approved therapy, are subject to off-label prescribing. In the case of disorders that have no approved treatment, therapy targets symptoms resulting from the primary condition. See TABLE 1 for a summary of major changes and their potential impact on medication management.
Another key change in DSM-5 is the discontinuation of the
familiar multiaxial diagnostic system. Prior to the new edition,
practitioners could address patients’ medical needs by assessing the
Axis III medical diagnoses and evaluating the psychiatric needs in Axes I
and II. In the five-axis system, the total score served as a guide for
assessing need for treatment, measuring treatments over time, and
predicting treatment outcomes. DSM-5 moves to a nonaxial
documentation of diagnosis, combining former Axes I, II, and III and
providing separate notations for psychosocial factors (formerly Axis IV)
and global assessment of function and disability (formerly Axis V).
Expert Remarks on the Revision
As stated in the APA Board of Trustees’ press release announcing the release of the approved final diagnostic criteria for DSM-5, “The trustees’ action marks the end of the manual’s comprehensive revision process, which has spanned over a decade and included contributions from more than 1,500 experts in psychiatry, psychology, social work, psychiatric nursing, pediatrics, neurology, and other related fields from 39 countries.”3 David J. Kupfer, MD, Task Force chair, answered some questions for U.S. Pharmacist.4
Q: How were the Task Force and Work Group members selected?
A: The president of the APA nominated individuals with expertise in their fields to be Task Force members. The nominees were reviewed by a subcommittee of the APA Board of Trustees to evaluate their relevant expertise and potential for real or perceived conflicts of interest. Final approval was granted by the full Board of Trustees. The Work Group members were also nominated by the president of the APA in consultation with the Task Force leadership and the Work Group chairs. Again, the nominees were reviewed and approved by the Board of Trustees in the same manner as Task Force nominees.
DSM-5’s Task Force and Work Group members included more than 160 world-renowned scientific researchers and clinicians with expertise in mental disorders, neuroscience, biology, genetics, statistics, epidemiology, and public health. Numerous experts also served as advisors to the DSM-5.
Q: Can you share the types of comments you received during the public comment period? Were these influential in some decisions to change?
A: The first draft of proposed changes was posted publicly on the DSM-5 website in February 2010, and the site also posted two subsequent drafts. With each draft, the site accepted feedback on proposed changes, receiving more than 13,000 comments on draft diagnostic criteria from mental health clinicians and researchers, the overall medical community, and patients, families, and advocates. Following each comment period, the DSM-5 Task Force and Work Groups reviewed each comment and made revisions where warranted.
In addition to the three public comment periods, Task Force members worked closely with advocacy groups, consumers, and other non–psychiatric care providers in face-to-face meetings and regular briefings. For example, in the autism community, there was some concern that diagnostic changes would result in individuals losing their diagnosis and, thus, being left without critical services. By the time the criteria were approved in late 2012, autism advocates listed the changes among the top 10 autism research advances of 2012.
Q: What was the main reason for moving away from the Global Assessment of Functioning score? Pharmacists found Axis III very helpful in ensuring that patients’ medical needs were addressed.
A: Over the years, problems emerged with the multiaxial approach, suggesting that the use of axes was unnecessarily complex and outdated and served to complicate the diagnosis process and impede global health information-sharing.
With the new single-axis approach, clinicians will still take note of the same mental, physical, and social considerations as under the multiaxial system to provide comprehensive assessments. They’ll just go about it differently. For example, in DSM-5, we recommend the World Health Organization’s Disability Assessment Schedule (WHO-DAS) as a global measure of disability. Using the WHO-DAS, disorders and their associated disabilities are conceptually distinct and assessed separately. This measure is based on an international classification of functioning and disability that is currently used throughout the rest of medicine, thereby bringing DSM-5 into greater alignment with other medical disciplines and into greater harmonization with international measures.
Q: What is the reason you stopped using roman numerals?
A: This change represents APA’s goal of creating a clinical manual that incorporates timely updates based on a preponderance of supportive research evidence. Incremental updates will be identified with decimals (i.e., DSM-5.1, DSM-5.2, etc.) until a new edition is required.
Q: Is there anything else you want to add now that the negative bloggers are out there?
A: I would add that DSM reflects the state of our scientific knowledge. When we started the process of developing this manual 14 years ago, I think we were all optimistic that there would be biomarkers and other breakthroughs of that magnitude. That hasn’t happened yet, but DSM-5 provides the best guidebook possible to diagnosing mental disorders. As breakthroughs occur, they will be incorporated into next editions to further strengthen patient care.
Q: Were any medication guidelines changed or recommended?
A: DSM has never been a manual guiding treatment or medication guidelines. As with past editions, DSM-5 is intended to be a manual for assessment and diagnosis of mental disorders and will not include information or guidelines for treatment of any disorder. That said, determining an accurate diagnosis is the first step toward being able to appropriately treat any medical condition, and mental disorders are no exception. DSM-5 will also be helpful in measuring the effectiveness of treatment, as dimensional assessments will assist in evaluating changes in severity levels as a response to treatment.4
Brief Review of Treatment Options for the Major Disorders
Although DSM is not a guideline for medication therapy, the diagnostic clarity that characterizes DSM-5 may influence prescribing trends. Pharmacists should not only be familiar with the DSM-5 changes, but also review general treatment guidelines for the major mental health conditions.
Neurodevelopmental disorders such as autism spectrum disorder do not have FDA-approved therapies to treat the core disorder. However, as is the case with a number of other mental health diagnoses, medication therapy targets the associated symptoms. Based on individual patient needs and past medical and/or psychiatric history, agitation and anxiety are symptoms that may be managed with antipsychotics, benzodiazepines, and sedating antihistamine products.
FDA-approved treatment for attention-deficit/hyperactivity disorder consists of stimulant and nonstimulant medications. DSM-5 highlights the expert consensus that this disorder may—and often does—encompass the patient’s life span. Pharmacists must be mindful of therapeutic considerations in aging patients when stimulant medications are used. These considerations include, but are not limited to, increased cardiac risks. Newly branded older agents, such as clonidine and guanfacine, are now available. Pharmacists must also be familiar with pharmacologic and nonpharmacologic treatment options for common concurrent conditions, such as insomnia.
Schizophrenia spectrum and other psychotic disorders have a wide array of medication therapy options, including first- and second-generation antipsychotics. A wide arsenal of new medications have been launched in the last few years, owing to an unusually increased pace for new mental health medications brought to market during that time. As is the case with other mental health disorders, co-occurring symptoms such as agitation, anxiety, and insomnia are common and must be treated accordingly.
Of the mental health disorders with FDA-approved treatments, bipolar and related disorders can benefit from one of the largest arrays of treatment options. Mood stabilizers include lithium, antiepileptics, and second-generation antipsychotics. Additionally, medications may be required to treat symptoms of agitation, anxiety, and insomnia, as previously noted for other psychiatric diagnoses. Adasuve (loxapine) inhalation powder was approved by the FDA in December 2012 for the acute treatment of agitation associated with bipolar I disorder or schizophrenia in adults.5
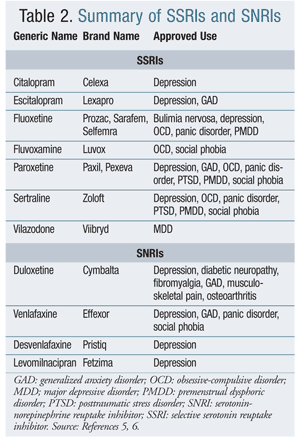
Depressive disorders, anxiety disorders, and posttraumatic stress
disorder are all distinct in their diagnostic criteria and therapeutic
timeline; however, they share a common medication class as first-line
treatment. Serotonin reuptake inhibitors (SSRIs) and
serotonin-norepinephrine reuptake inhibitors (SNRIs) have emerged as the
treatment of choice based on efficacy, lack of dependence, and
tolerable side-effect profile. The FDA-approved uses may guide
prescriber treatment choice; however, the mechanism of action is the
same for all agents within each drug class (TABLE 2). When
recommending these agents as a new treatment intervention or managing a
patient currently on an SSRI/SNRI regimen, it is important for the
provider to consider the side effects and drug interactions. The
side-effect profiles of these agents may appear similar, but the degree
of severity often differs with the agent chosen, the specific CYP450
profile of the drug, and potential individual genetic polymorphisms in
individuals receiving treatment. In July 2013, the FDA approved
levomilnacipran (Fetzima) as the newest SNRI for major depressive
disorder in adults, making the drug the fourth SNRI to be approved in
the U.S.6
REFERENCES
1. American Psychiatric Association. DSM-5 implementation and support. www.dsm5.org/Pages/Default.aspx. Accessed August 1, 2013.
2. CMS.gov. Frequently asked questions. https://questions.cms.gov/faq.php?id=5005&faqId=1817. Accessed August 1, 2013.
3. American Psychiatric Association Board of Trustees approves DSM-5.
http://dsmfacts.org/materials/american-psychiatric-association-board-of-trustees-approves-dsm-5.
Accessed August 1, 2013.
4. In-person interview with David J. Kupfer, MD, on July 3, 2013.
5. Clinical Pharmacology [online database]. Tampa, FL: Gold Standard,
Inc; 2013. www.clinicalpharmacology.com. Accessed August 1, 2013.
6. New and generic drug approvals. www.fda.gov/Drugs/NewsEvents/ucm130961.htm. Accessed August 1, 2013.
To comment on this article, contact rdavidson@uspharmacist.com.