US Pharm. 2010;36(4)(Compliance & Adherence suppl):6-10.
Medication nonadherence or noncompliance, defined as the failure to take medications on time, in the prescribed dose, and by the correct patient, is costly in terms of economic loss and poor health outcomes. As shown in a meta-analysis by Einarson, approximately 1% of hospital admissions in industrialized nations are due to medication noncompliance.1
Scope of the Problem and Consequences of Medication Nonadherence
Einarson specifically studied hospital admissions prompted by adverse drug reactions (ADRs), including the subset of those ADR admissions specifically related to a patient’s noncompliant or unintentionally inappropriate drug use (cases involving drug abuse, alcoholism, suicide attempts, intoxication, or inadequate prescribing were excluded). Einarson reviewed ADR rates from 49 hospital systems as published in 36 articles. The weighted meta-analysis showed that 5.1% (95% confidence interval [CI] 4.4-5.8) of all hospitalizations were due to ADRs.1 The mortality rate of patients admitted for ADRs was 3.7%.1 Eleven studies in the meta-analysis showed that 22.7% of ADR hospitalizations were a consequence of medication noncompliance.1 In general, of all medication-related hospital admissions in the United States, 33% to 69% are due to poor medication adherence, with an estimated cost of approximately $100 billion a year.2
The problem of medication nonadherence in the elderly results in higher rates of hospital admissions than that found by Einarson in the general population. Col et al demonstrated that 28.2% of 315 consecutive elderly hospital admissions at a single acute-care hospital were related to medication issues; 16.8% of the hospitalizations were due to ADRs, and 11.4 % were due to medication noncompliance.3 Several factors were statistically associated with a higher risk of hospitalization in the elderly due to noncompliance, including poor recall of medication regimen, seeing numerous physicians, being female, falling into the medium income category, using numerous medications, and having the opinion that medications are expensive. In this study, 32.7% of the patients had a history of noncompliance.3
Estimates of medication nonadherence rates in the elderly range from 40% to as high as 75%.4 The most commonly identified problems leading to nonadherence in the elderly are overuse and abuse, forgetting, and alteration of schedules and doses.4 It has been estimated that 23% of nursing home admissions are related to the inability of patients to properly self-administer medications.5
The World Health Organization (WHO) has estimated that, even in affluent countries with well-developed health care infrastructure, adherence to long-term medication therapy for chronic illness averages only 50%.6
Jackevicius et al demonstrated that survivors of myocardial infarction who filled all of their hospital discharge medications had a significantly improved likelihood of survival at 1 year.7 There were 4,591 post-acute myocardial infarction (AMI) patients, age 65 years or greater, who were included in this retrospective data analysis. Of the 12,832 discharge prescriptions written, 21% remained unfilled at 120 days (primary noncompliance). The vast majority of patients who filled prescriptions did so within 1 week of discharge. Primary nonadherence was associated with an increased risk of death at 1 year. Patients who did not fill any discharge medications by 120 days after an AMI had an 80% increased odds of death at 1 year.7 Patients who demonstrated partial nonadherence had a 44% increased odds of death.7 Despite the proven life-saving benefits of the post-AMI medication regimen (e.g., aspirin, beta blockers, statins, ACE inhibitors), only 74% of the patients in the study had filled all of their discharge prescriptions by 120 days. These data underscore the need for reinforcement of adherence to medication regimens within the first several weeks of hospital discharge. The authors recommend a routine follow-up call to the patient 1 to 2 weeks post discharge.
Interventions to Improve Medication Adherence in Patients With Chronic Diseases
The WHO has outlined five dimensions and associated activities that can be deployed to improve medication adherence in patients with chronic diseases, such as hypertension, diabetes, and asthma.6 As illustrated in TABLE 1, three of the dimensions are good candidates for intervention with electronic tools.
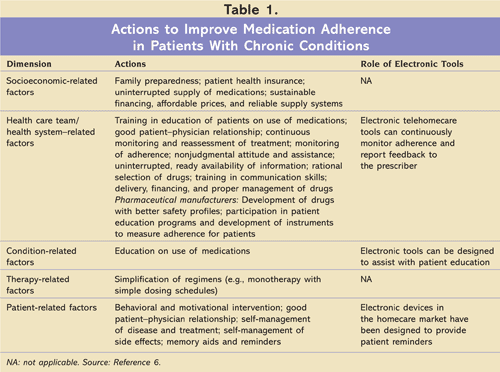
Electronic Homecare Devices and Telehomecare Functions
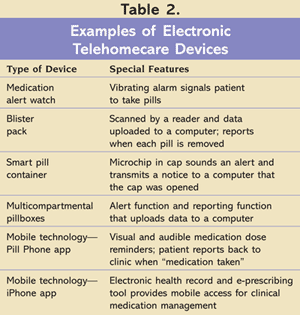
A number of homecare devices are available to remind patients that it is time to take their medication. These include special watches with alarms, pillbox timers, “smart pill” containers, and automated pill dispensers. A medication alert watch with a vibrating alarm may be used to privately signal the patient that it is time to take the medication. Some of these devices are primarily for use by the patient as a reminder, but more sophisticated devices incorporate reporting and analytic functionality. The reporting and analytic functionality is typically transmitted via computer over the Internet; this type of reporting service is called telehomecare. TABLE 2 details several examples of such devices.
For example, one type of device is a blister pack that can report when each individual pill is removed. The blister pack is scanned by a reader and the data uploaded to a computer. A smart pill container features a cap linked to a microchip that sounds an alert when it is time to take the medication. When the cap is opened, the chip will date- and time-stamp the opening and closing of the container. At any time, the chip can send a radio signal to a reader that records the stored events on a Windows-based computer. The computer can transfer the adherence monitoring data over the Internet to the patient’s health care team. One such device, the Medication Event Monitoring System (MEMS) 6, has a memory capacity of 3,968 events and a battery life of 36 months.8
Multicompartmental pillboxes have similar functionality, with an alert function that signals to the patient which compartment to open. When the compartment is opened, the device transmits a signal to a receiver and into a computer. Another similar device has a feedback loop to the patient. If the medication is not removed from the device within the specified time window, the computer will send a prearranged reminder message to the patient. This could be in the form of a text message, a call to the patient’s cell phone, or an e-mail.
The above-noted homecare devices are most useful when the patient is intent on taking the medication, but is forgetful or only moderately motivated. If the patient is intent on being noncompliant, these devices can be defeated by opening them and then wasting the medication. “Patients may open a container and not take the medication, take the wrong amount of medication, or invalidate the data by placing the medication into another container or taking multiple doses out of the container at the same time.”2 In other words, the reporting functionality demonstrates only that the cap was opened or the medication was removed; it does not prove that the patient actually ingested the correct dose of the correct medication.
Despite these drawbacks, electronic monitoring is believed by many authorities to provide the most accurate and valuable data on adherence, especially in difficult clinical situations.2,9 Electronic monitoring tools such as MEMS have now replaced pill counts as the reference standard for measuring medication adherence.10
Data from electronic monitoring systems have revealed that there are six patterns of patient adherence—resulting in the rule of 1/6. Approximately 1/6 of patients come close to perfect adherence; 1/6 take nearly all doses, but with irregular timing; 1/6 miss an occasional single daily dose and have some timing irregularity; 1/6 take drug holidays every 3 to 4 months, with occasional omissions of doses; 1/6 have one or more drug holidays monthly, with frequent omissions of doses; and 1/6 take few or no doses, but may report that they are compliant.10 Electronic reporting data also reveal that simple regimens, such as once-daily dosing, help improve adherence.9
Mobile Apps
An emerging technology space is the use of mobile applications (apps) to medication adherence, known as mHealth technology. One such application, the wireless Pill Phone, has been used to improve medication adherence in management of hypertension. A press release issued by the George Washington University Medical Center, One Economy, Cricket Communications, VOCEL, and Qualcomm Incorporated reported that the George Washington University Medical Center studied 3G wireless phones equipped with the Pill Phone app in a population of underserved hypertensive patients in Washington, DC.11 The phone provided patients with visual and audible reminders to take medications. Patient were trained to use the software and educated about the importance of treating hypertension. When patients took their medication, they could report this through an app back to the clinic. The study reported a trend toward increased prescription refill rates in individuals who used the phone. There was no indication as to whether hypertension control actually improved.
The Allscripts iPhone app has been deployed as an all-purpose tool for medication management by physicians and nurse practitioners.12 The clinician can access medical records, medication lists, and e-prescribing functionality using the iPhone. This allows the clinician in any location to manage the patient’s medication renewals and review the patient’s medical records, thereby enabling the clinician to respond to the patient’s requests for refills at any time. This access to the clinician may help patients maintain adherence.
Formal Published Clinical Studies: Proof of Concept
Despite the rapid advances in technology, there are only a few published studies in peer-reviewed literature demonstrating that electronic reminder and reporting devices, when appropriately used, can improve compliance rates. For example, only a few controlled studies have actually been designed, implemented, and published to demonstrate whether such devices actually improve medication adherence. More rigorous controlled studies are needed to study clinical outcomes in patients who are employing the technology described in this review. Several existing studies will be discussed.
Asthma: Charles et al investigated whether an audiovisual reminder function could improve adherence to inhaled corticosteroid therapy in asthma.13 This is an area of particular importance since chronic management of asthma is typically associated with adherence rates of less than 50%, with increased risk of mortality.
In this randomized, open-label, parallel group study of 110 adult and adolescent subjects (ages 13-65 years) with asthma, the subjects were randomized to receive 24 weeks of inhaler therapy via a metered dose inhaler with or without an audiovisual reminder function.13 The inhaler with the audiovisual reminder function was programmed to emit an audible signal and a visual cue at predetermined times. The inhaler was also equipped with a covert electronic reporting function that allowed investigators to determine whether a dose was actually activated. The control inhalers were also equipped with the reporting function. Of the 55 patients assigned to each group, 44 completed the study arm, and 46 completed the control arm. The electronic monitoring was also designed to detect “dose dumping,” in which the inhaler was activated 10 or more times within a 3-hour period. The study was adequately powered to detect an adherence difference of 10% at the 5% level of significance. The level of adherence was defined as the proportion of medication taken as prescribed over the final 12 weeks of the study. Adherence was also assessed according to the proportion of subjects who took >50%, >80%, or >90% of the prescribed inhaler medication.13
The study demonstrated a positive benefit of the reminder system. The absolute difference in median percentage between the two groups was 18% (95% CI, 10%-26%; P <.0001).13 Furthermore, the proportion of subjects taking >50% of their medication was 95.5% in the intervention group compared with 71.7% in the control group. The proportion of subjects taking >80% of their medication was 88.6% in the intervention group, compared with 39.1% in the control group. Finally, the proportion of subjects taking more than 90% of their medication was 63.6% in the intervention group compared with 19.6% in the control group, an approximately three-fold improvement.13 This is an important result, as it demonstrates clinically significant improvement in adherence to inhaled corticosteroid therapy; this is likely to translate to significant cost avoidance in emergency room visits and inpatient admissions.
Glaucoma: Laster et al studied 13 subjects with open-angle glaucoma who were receiving 1 drop of pilocarpine solution 4 times a day in both eyes.14 Each patient served as his or her own control. Patients used a medication alarm device (TimeCap) for 30 days and underwent a 30-day control period without the device. This study also demonstrated a major improvement in adherence. Subjects using the intervention administered an average of 2.867 g (P <.0001) more pilocarpine over the 30 days than during the control period.14
Schizophrenia: Patients with schizophrenia and other behavioral health conditions typically demonstrate poor medication adherence rates, but have the potential for significant benefit if adherence can be improved. Depot formulations are often the treatment of choice for patients with schizophrenia who are not adhering to an oral regimen. In a pilot study at the Baltimore VA Hospital, Ruskin et al investigated the use of the Med-eMonitor System (InforMedix, Rockville, MD) in an outpatient setting in patients suffering from schizophrenia.15 Twenty-two patients and 16 caregivers were trained in the use of the system in the clinic, and 14 patients used the monitor at home for 2 months.15 Medication compliance and symptom data were uploaded each day from the Med-eMonitor to an Internet-enabled database. The major result illustrated by this pilot study was the feasibility of central evaluation by treating professionals using an electronic reporting device. However, more studies in this area are warranted.
Hypertension: Burnier and colleagues used microchip technology for monitoring adherence to hypertension treatment.16 One goal was to differentiate noncompliance from truly resistant hypertension so that the therapeutic intervention could be appropriately tailored. Forty-one patients who were apparently resistant to a three-drug hypertension regimen (baseline average blood pressure 156/106 +/- 23/11 mmHg) were included in the study. An electronic reporting device was then provided to the patients, without any change in the medication regimen, for a period of 2 months. Patients were then invited to continue on the protocol for another 2 months, during which time any indicated adjustments would be made to the regimen. Remarkably, the study showed that electronic monitoring alone over a period of 2 months resulted in significant improvement in blood pressure (145/97 +/- 20/15 mmHg, P <.01).16 Blood pressure was normalized (systolic <140, diastolic <90) in one-third of the patients merely as a result of the electronic monitoring.16 Monitoring for up to 4 months was carried out in 30 patients, with adjustments in the regimen as needed. This resulted in further improvements (from 150/100 +/- 18/15 to 143/94 +/- 22/11 mmHg, P = .04/.02).16
Hence, electronic monitoring of compliance is useful in the management of patients with refractory hypertension. The objective compliance data received by the clinician can help with rational adjustments in the regimen to further improve control. It appears that the mere act of monitoring helps patients achieve greater compliance.
Summary
Electronic devices can be deployed to improve medication adherence in several ways. The simplest function is to provide timing cues regarding the appropriate times to take the medication. Electronic reporting from microchip devices, such as smart pill containers via the Internet, also known as telehomecare, is an attractive option and provides objective feedback to the prescriber. These electronic interventions have been demonstrated to have significant impact in improving medication adherence in several chronic diseases, including asthma, glaucoma, and hypertension. One drawback is the relative expense of the devices and the fact that third-party insurers typically do not cover the cost, although in some states, such as New York, these devices are covered by Medicaid.17
Further confirmatory studies will be needed to determine whether improved outcomes, avoided emergency room visits, and fewer inpatient admissions will recoup the costs of these systems. Nevertheless, from the available data, it is clear that the microchip electronic devices and innovative applications that constitute telehomecare—audio-visual reminders; text, voice, or e-mail messaging through smart phones and cell phones, including mobile apps; smart pill containers; and Internet-based reporting systems—have great potential in improving medication adherence in patients with chronic illness.
REFERENCES
1. Einarson TR. Drug-related hospital admissions. Ann Pharmacother. 1993;27:832-840.
2. Osterberg L, Blaschke T. Adherence to medication. N Engl J Med. 2005;353:487-497.
3. Col N, Fanale JE, Kronholm P. The role of medication noncompliance and adverse drug reactions in hospitalizations of the elderly. Arch Intern Med. 1990;150:841-845.
4. Salzman C. Medication compliance in the elderly. J Clin Psychiatry. 1995;56(suppl 1):18-22.
5. Strandberg LR. Drugs as a reason for nursing home admissions. J Am Health Care Assoc.
6. World Health Organization. Adherence to Long-Term Therapies: Evidence for Action. Geneva, Switzerland: World Health Organization; 2003. http://whqlibdoc.who.int/ 1984;10:20-23.
7. Jackevicius CA, Li P, Tu JV. Prevalence, predictors, and outcomes of primary nonadherence after acute myocardial infarction. Circulation. 2008;117:1028-1036.
8. MEMS products. Medication Event Monitoring System (MEMS) 6. Union City, CA: Aprex, a division of AARDEX. www.aardexgroup.com/aardex_
9. Urquhart J. The electronic medication event monitor: lessons for pharmacotherapy. Clin Pharmacokinet. 1997;32:345-356.
10. Farmer KC. Methods for measuring and monitoring medication regimen adherence in clinical trials and clinical practice. Clin Ther. 1999;21:1074-1090.
11. The George Washington University Medical Center, One Economy, Cricket Communications, VOCEL, and Qualcomm Incorporated. Research study looks at benefits of 3G wireless technology for hypertensive patients in underserved urban communities. PR Newswire. February 9, 2011. www.marketwatch.com/story/
12. Misra S. Triage and treat patients from anywhere with Allscripts remote iPhone App—an electronic health record and ePrescribing tool. iMedicalApps. March 5, 2010. www.imedicalapps.com/2010/03/
13. Charles T, Quinn D, Weatherall M, et al. An audiovisual reminder function improves adherence with inhaled corticosteroid therapy in asthma. J Allergy Clin Immunol. 2007;119:811-816.
14. Laster SF, Martin JL, Fleming JB. The effect of a medication alarm device for medical adherence research. J Am Optom Assoc. 1996;67:654-658.
15. Ruskin PE, Van Der Wende J, Clark CR, et al. Feasibility of using the Med-eMonitor system in the treatment of schizophrenia: a pilot study. Drug Inform J. 2003;37:283-291.
16. Burnier M, Schneider MP, Chiolero A, et al. Electronic compliance monitoring in resistant hypertension: the basis for rational therapeutic decisions. J Hypertens. 2001;19:335-341.
17. In New York, Section 3621 of the Public Health Law authorizes a telemedicine demonstration program in Medicaid.
To comment on this article, contact rdavidson@uspharmacist.com.






