US Pharm. 2009;34(4):26-37.
Acne is a common skin condition that affects patients of all ages. Although estimates reveal that 85% of adolescents will experience the condition, a significant number of patients develop acne as adults.1 The mean age at which patients present for treatment of acne is 24 years, with 10% of visits attributed to patients ranging in age from 35 to 44 years. While most studies focus on acne in adolescents, a recent study evaluating prevalence of acne in adults found that the condition continues to be problematic even after the teenage years, with women 20 years of age and older being most affected.2
Even without treatment, acne associated with adolescence generally resolves as patients approach young adulthood. For adult-onset acne, however, the need for treatment to prevent scarring can last well into middle age.3 The most commonly employed therapeutic tools for treatment of acne include topical retinoids, benzoyl peroxide, salicylic acid, topical and oral antibiotics, estrogen-containing oral contraceptives, oral antiandrogens, and isotretinoin.
Dietary modification as a treatment option for acne continues to be controversial. Myths surrounding diet and acne have persisted for many years (e.g., greasy foods or chocolate cause breakouts). Treatment guidelines for patients with acne that were published in 2007 state that studies fail to show a link between dietary consumption and development of acne, referencing literature more than 30 years old.4 However, the link between dietary intake and its effect on acne continues to be an area of interest, as understanding of the pathogenesis of this condition evolves.
Pathogenesis
Several factors are known to play a role in the pathogenesis of acne: 1) hyperkeratinization, along with plugging of sebaceous follicles, results from abnormal desquamation of the follicular epithelium; 2) increased sebum production as a result of androgen stimulation; 3) colonization of the follicular duct by Propionibacterium acnes, an organism that is part of normal skin flora and causes inflammation commonly seen in patients with acne.1 As scientists uncover more detail regarding hormonal pathways under the influence of diet, the role of dietary intake in the development of acne becomes more important to study as a treatment option.
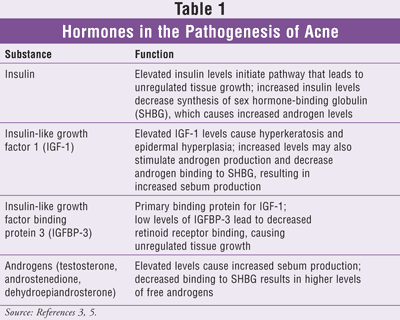
The endocrine system also plays a role in the pathogenesis of acne. Elevated blood levels of insulin, whether acute or chronic, trigger activation of a hormonal pathway, causing a response that results in increased androgen production and tissue growth. The hormones and proposed mechanisms by which they contribute to formation of acne are listed in TABLE 1. These substances, through a cascade of events, cause elevated levels of insulin-like growth factor 1 (IGF-1) and decreased levels of insulin-like growth factor binding protein 3 (IGFBP-3), the primary binding protein for IGF-1.5 Low levels of IGFBP-3 caused by hyperinsulinemia result in lower levels of naturally occurring retinoids in the body. These retinoids bind to retinoid receptors to activate genes responsible for keeping tissue growth in check; therefore, decreased levels may result in follicular cell proliferation.3,5
Increased androgen synthesis results in greater sebum production. Both elevated levels of insulin and IGF-1 stimulate androgen production in the ovaries and testicles. Patients with polycystic ovary syndrome (PCOS) often struggle with acne. This disorder is characterized by hyperinsulinemia, insulin resistance, and elevated levels of circulating androgens. Studies show that lowering levels of androgens by improving insulin sensitivity with medication and/or a low glycemic load diet may be effective for treating acne in these patients.5,6 For patients without PCOS, researchers continue to focus not only on the effect of a low glycemic load diet on acne but also on dairy intake and the development of acne.
Glycemic Load Theory
Glycemic index and glycemic load are important elements in the link between acne and dietary intake, as both values are closely related to the insulin response that occurs when blood glucose surges after eating.7 Glycemic index compares the potential for foods to cause increases in blood glucose. Calculation of glycemic index for any given food is based on equal amounts of carbohydrate and does not consider the quality of the carbohydrate.
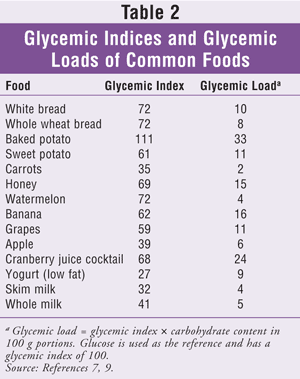
More recently, scientists introduced the concept of glycemic load, which considers the potential for a food to raise blood glucose based not only on the quantity of carbohydrate consumed but also on the quality of carbohydrate in the food.7-9 Examples of common foods with their respective glycemic indices and glycemic loads are listed in TABLE 2. Typically, a low glycemic load diet is high in protein and low in fats and sugars. Carbohydrates are consumed in the form of fruits and vegetables, as opposed to pastas and breads. Foods with lower glycemic indices and glycemic load values result in lower insulin response in the body. One notable exception is milk, which, despite having a low glycemic index and glycemic load, causes a large insulin response after ingestion. The insulin response seen with milk is similar to that of white bread.7
Since elevated levels of insulin in the body trigger a hormonal cascade that leads to increased production of substances known to contribute to acne formation, research on the association between dietary intake and acne focuses on evaluating the effect of a low glycemic load diet on acne as well as the consumption of milk. Better understanding of both the pathophysiology of acne and contributing hormonal mechanisms have lead to a renewed interest in studying the influence of diet on acne.
Effectiveness of the Low Glycemic Load Diet
Research evaluating hormonal influences on acne often uses the intervention of a specific glycemic load diet to determine effect on hormonal pathways. One such study, a prospective cohort trial in Turkey, evaluated the effect of low, moderate, and high glycemic load diets on acne.8 This trial enrolled male and female college students between the ages of 19 and 34, divided into two groups based on the presence or absence of acne (control group). Investigators asked participants via questionnaire about food intake of varying glycemic loads. The responses were then used to calculate overall glycemic index and glycemic load values. Additionally, blood samples were taken to assess levels of glucose, insulin, IGF-1, IGFBP-3, and leptin. The study authors also calculated an insulin resistance index for participants.
No significant variations in serum glucose, insulin, and leptin levels were found between the groups. Analysis of dietary intake between the groups also showed that dietary glycemic index and glycemic load did not translate to significant differences between the groups with regard to acne. From these results, the authors concluded that dietary intake does not appear to have an effect on acne in younger patients.8
Another recent study compared the effect of a low glycemic load diet to that of a conventional (defined as carbohydrate-dense) diet.10 This randomized, investigator-masked, controlled trial enrolled 43 male patients (ages 15-25 years) with acne for a 12-week evaluation of a low glycemic load diet compared to a high glycemic load (conventional) diet. Lesion counts, as well as serum hormone levels (sex hormone-binding globulin [SHBG], IGF-1, testosterone, insulin, IGFBP-3), were measured. This study found that while both groups had fewer acne lesions at the end of 12 weeks, participants in the low glycemic load diet group had a significant reduction in lesions. Of note, the low glycemic load diet group also lost weight, had less body fat, had a smaller waist circumference, and had better endocrine laboratory results at the end of the study. The investigators readily acknowledge that the results may not reflect just the diet intervention, but may also be influenced by weight loss in the low glycemic load diet group.10
Acne occurs primarily in Western societies, which makes the link between dietary intake and the development of acne more compelling. Investigators studied the prevalence of acne among two non-Westernized populations, one in New Guinea and the other in Paraguay, along with environmental factors such as diet.2 Many foods found in Western diets, such as alcohol, oils, sugar, salt, dairy products, and processed foods, were essentially nonexistent in the diets of the people studied. These groups naturally consumed a low glycemic load diet composed primarily of fish, nuts, wild game, fresh fruits, and vegetables. No cases of acne were observed among the 1,300 people examined. In addition to a lower prevalence of acne, these groups had much lower rates of insulin resistance, obesity, and hypertension.2
As noted above, those who eat non-Western, low glycemic load diets tend to eat more fish. Although research is limited, case report data suggest that increased consumption of fish, and the resultant increase in omega-3 fatty acids, may reduce the inflammatory response seen with acne.11 Omega-3 fatty acids are thought to inhibit leukotriene B4 (LTB4), a substance known to cause inflammation in the body.11 However, given the paucity of data, additional research is necessary to determine if a link between omega-3 fatty acid consumption and acne exists.
Effectiveness of Moderating Dairy Consumption
Since milk causes a significant insulin response after intake, the effect of limiting milk and dairy on development of acne has been an area of interest for scientists. Three published studies explored dairy consumption during adolescence and the prevalence of acne.12-14 All three studies used cohorts from either the Nurses Health Study II (NHS II) or a study group composed of children of participants in the NHS II, known as the Growing Up Today Study (GUTS).
One study evaluating the relationship between milk consumption and acne in adolescent females used questionnaire data gathered from 6,094 girls in the GUTS cohort.12 Participants, who ranged in age from 9 to 15 years, were asked to quantify how often they consumed a portion of milk or other dairy product on two different questionnaires, presented 2 years apart. They were then queried about problems with acne in a final survey completed 3 years after the first survey. Based on questionnaire responses, the study authors analyzed dairy intake, nutrient intake, and the number of participants reporting acne. The results indicated that consumption of milk was associated with a higher prevalence of acne.12 Prevalence of acne did not differ, however, based on the fat content of the milk. The study authors considered bioactive molecules in milk, such as androgens not removed during processing, a contributing factor in the link between milk and acne.12
Another prospective cohort study, using the same methods as the GUTS cohort that enrolled adolescent females, evaluated the effect on milk consumption with respect to acne in 4,273 adolescent males.13 Participants ranged in age from 9 to 15 years and again completed three questionnaires—two that evaluated intake of dairy and one that asked about acne 3 years after the first questionnaire was completed. Dairy intake, nutrient intake, and numbers of respondents reporting acne were analyzed. The study found only a very weak association between milk intake and acne in adolescent males.13 As in the previous GUTS cohort study, the investigators felt bioactive substances not removed in milk processing contributed to acne. Explaining the difference in the outcomes between the two studies, the authors stated that normal developmental differences between adolescent boys and girls contributed to the variance.13
Finally, using questionnaires completed by almost 48,000 registered nurses, the investigators for the NHS II group retrospectively examined information provided by the nurses about physician-diagnosed severe acne during high school.14 The participants also submitted information about milk consumption, as well as intake of dairy foods such as cream cheese, instant breakfast drink, sherbet, and cottage cheese during the same time frame. As with the studies using the GUTS cohort, intake of nutrients such as vitamin D, calcium, and fats was analyzed using the information provided on the questionnaire. The study authors found an association between milk consumption during adolescence and acne, and again hypothesized that hormones contained in milk and their effect on endogenous hormone production contributed to the results found in this study.14 Interestingly, the prevalence of acne was higher with skim milk when compared to whole milk. Intake of instant breakfast drink, cottage cheese, and cream cheese were also found to be associated with teenage acne in the study group.14
Conclusion
Much remains to be discovered about the link between diet and the development of acne. Older studies that found no association between the two were often not well controlled and the methods not well described. Therefore, their conclusions are to be cautiously interpreted.7,15,16 Recent studies explore the effect of a low glycemic load diet and dairy consumption on acne.12-14 These more recently published data establish an association between dietary intake and the prevalence of acne, but most are not randomized, controlled trials and rely very heavily on questionnaire data. Thus, their results should be approached carefully when applied to patient care.
Role of the Pharmacist
Pharmacists often receive questions from patients that pertain to treating acne. At this time, for patients with hard-to-control acne, reducing carbohydrate intake is safe and may be beneficial when used in combination with other available treatments. Patients concerned specifically about milk or dairy products contributing to acne should be counseled that while some available information shows an association between the two, until better information is available, withholding milk or dairy is not recommended.17 It is important to stress to patients that based on current evidence, dietary intake is not a significant factor in the development of acne, and until more scientifically solid information is available, the value of dietary intervention as a means to treat or control acne remains controversial.
REFERENCES
1. James WD. Clinical practice. Acne. N Engl J Med. 2005;352:1463-1472.
2. Collier CN, Harper JC, Cafardi JA, et al. The prevalence of acne in adults 20 years and older. J Am Acad Dermatol. 2008;58:56-59.
3. Keri JE, Nijhawan RI. Diet and acne. Exp Rev Dermatol. 2008;3:437-440.
4. Strauss JS, Krowchuk DP, Leyden JJ, et al. Guidelines for care of acne vulgaris management. J Am Acad Dermatol. 2007;56:651-663.
5. Cordain L, Lindeberg S, Hurtado M, et al. Acne vulgaris: a disease of Western civilization. Arch Derm. 2002;138:1584-1590.
6. Farshchi H, Rane A, Love A, Kennedy RL. Diet and nutrition in polycystic ovary syndrome (PCOS): pointers for nutritional management. J Obstet Gynaecol. 2007;27:762-773.
7. Cordain L. Implications for the role of diet in acne. Semin Cutan Med Surg. 2005;24:84-91.
8. Kaymak Y, Adisen E, Ilter N, et al. Dietary glycemic index and glucose, insulin, insulin-like growth factor-1, insulin-like growth factor binding protein 3, and leptin levels in patients with acne. J Am Acad Dermatol. 2007;57:819-823.
9. Atkinson FS, Foster-Powell K, Brand-Miller JC. International tables of glycemic index and glycemic load values: 2008. Diabetes Care. 2008;31:2281-2231.
10. Smith RN, Mann NJ, Braue A, et al. The effect of a high-protein, low glycemic-load diet versus a conventional, high glycemic-load diet on biochemical parameters associated with acne vulgaris: a randomized, investigator-masked, controlled trial. J Am Acad Dermatol. 2007;57:247-256.
11. Rubin MG, Kim K, Logan AC. Acne vulgaris, mental health and omega-3 fatty acids: a report of cases. Lipids Health Dis. 2008;7:36.
12. Adebamowo CA, Spiegelman D, Berkey CS, et al. Milk consumption and acne in adolescent girls. Dermatol Online J. 2006;12:1.
13. Adebamowo CA, Spiegelman D, Berkey CS, et al. Milk consumption and acne in teenaged boys. J Am Acad Dermatol. 2006;12:787-793.
14. Adebamowo CA, Spiegelman D, Danby FW, et al. High school dietary dairy intake and teenage acne. J Am Acad Dermatol. 2005;52:207-214.
15. Fulton JE Jr, Plewig G, Kligman AM. Effect of chocolate on acne vulgaris. JAMA. 1969;210:2071-2074.
16. Anderson PC. Foods as the cause of acne. Am Fam Physician. 1971;3:102-103.
17. Webster GF. Diet and acne [commentary]. J Am Acad Dermatol. 2008;58:794-795.
To comment on this article, contact rdavidson@jobson.com.





