US Pharm.
2007;32(10)(Diabetes suppl):17-20.
Gestational diabetes mellitus (GDM) is defined as
onset or first recognition of carbohydrate intolerance during pregnancy;
1-3 this definition does not encompass women who are known to have
diabetes prior to conception. Approximately 2% to 7% of all pregnancies are
complicated by GDM, although the prevalence may be as high as 15% depending
upon the population evaluated.1,2,4 Ethnic groups at greater risk
for GDM include populations with an inherently higher rate of type 2 diabetes
mellitus, such as African Americans, Hispanics, Native Americans, and those of
South Asian, East Asian, or Pacific Islander descent.2,3,5
Unrecognized or inappropriately treated GDM can result in serious
consequences, including fetal macrosomia and shoulder dystocia, neonatal
hypoglycemia, hyperbilirubinemia and hypocalcemia, and an increased incidence
of type 2 diabetes in the mother later in life.1,6 Appropriate
identification and management of GDM is crucial to ensuring optimal outcomes
for both the mother and neonate.
Pathophysiology
The full spectrum of metabolic abnormalities that contribute to hyperglycemia
in GDM has not been fully elucidated. In general, human pregnancy is
associated with insulin resistance; insulin sensitivity begins to decline in
mid-pregnancy, progressively diminishing throughout the latter half of
pregnancy.7,8 Insulin resistance in pregnancy has been attributed
to a number of factors, including effects of human placental lactogen, human
placental growth hormone, progesterone, prolactin, and cortisol.9,10
Recently, adipokines (proteins synthesized and secreted by adipocytes) such
as leptin, tumor necrosis factor alpha, adiponectin, and resistin have also
been implicated.8-10 Regardless of the cause, insulin resistance in
pregnancy serves to decrease glucose utilization by the mother and facilitate
the provision of energy substrate for the fetus.9,10 In normal
pregnancy, insulin secretion may increase by as much as 200% to 250% to
counteract the increased insulin resistance seen in late gestation.8
Insulin secretion in GDM is insufficient to offset the increased insulin
resistance, and hyperglycemia results.
In addition to impaired
compensatory secretion of insulin, a number of other proposed mechanisms may
play a role in GDM. Adiponectin is an endogenous insulin–sensitizing hormone
that decreases hepatic glucose production and stimulates glucose uptake in
skeletal muscle.8 Adiponectin levels are reduced in women with GDM,
as compared to those without it.7,8 Additionally, glucose uptake in
skeletal muscle of patients with GDM may be impaired due to defective insulin
receptor signaling. Insulin resistance may also occur in adipose tissue due to
downregulation of GLUT4, a glucose transport protein responsible for
insulin-mediated glucose disposal. GLUT4 becomes downregulated in adipocytes
of pregnant women, but the downregulation is more pronounced in women with GDM.
8 Further study is needed to fully characterize the scope of metabolic
defects seen in GDM.
Screening and Diagnosis
Women who are severely obese or have a history of GDM, a strong family history
of type 2 diabetes, impaired glucose tolerance, glucosuria, or a previous
delivery of a large-for-gestation age infant are considered to be at high risk
for GDM.1,11 After pregnancy is confirmed, individuals with these
risk factors should be screened for GDM as soon as possible. If the initial
screening is negative, follow-up testing should be performed between 24 and 28
weeks' gestation. Testing should also occur at 24 to 28 weeks' gestation for
women at average risk for GDM. Women at low risk for GDM include those who
meet all of the following criteria: age younger than 25 years, normal
prepregnancy weight, normal weight at birth, ethnicity with a low prevalence
of GDM, no family history of diabetes in first-degree relatives, no history of
glucose intolerance, and no history of poor obstetric outcome.1,2,11
The benefit of screening for GDM in low-risk women is controversial.
Recommended screening for GDM
consists of administration of a 50-g oral glucose load, followed by
measurement of plasma glucose one hour later.1,2,12 A glucose
threshold value of more than 140 mg/dL identifies approximately 80% of
individuals with GDM, and a threshold of greater than 130 mg/dL increases the
sensitivity to approximately 90%. According to the American Diabetes
Association, use of either threshold for the screening test is acceptable.
1,2,13 Women with one-hour glucose values exceeding the screening test
threshold are candidates for a diagnostic oral glucose tolerance test (OGTT).
The OGTT involves administration of a 100-g glucose load and measurement of
fasting plasma glucose and glucose levels at one, two, and three hours
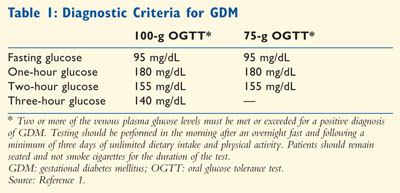
post–glucose ingestion.1-3,12 Specific diagnostic criteria
can be found in Table 1. Although not as well validated as the 100-g
OGTT, a 75-g OGTT with fasting, one-hour, and two-hour glucose measurements is
an alternative diagnostic test.
Treatment
Therapeutic interventions available for the treatment of GDM include medical
nutrition therapy and pharmacologic therapy. Potential pharmacologic options
include insulin and glyburide. Metformin and rosiglitazone have both been
shown to cross the placenta, and use of these agents in GDM is not recommended
until further information on teratogenic potential and risk/benefit ratio in
pregnancy can be ascertained.14-16 Initial studies with acarbose,
an alpha-glucosidase inhibitor, have shown promise in the treatment of GDM,
but limited data exist. Although acarbose exhibits minimal systemic
absorption, the transplacental passage of this medication has not been
thoroughly investigated.11,16 The adverse effect of
gastrointestinal discomfort in the mother may limit the utility of acarbose in
the treatment of GDM. Safety and efficacy of other agents used for diabetes,
such as incretin mimetics, synthetic amylin analogs, meglitinides,
glucagon-like peptide-1 agonists, and the dipeptidyl peptidase-4 inhibitors,
have not been established in GDM. Regardless of the chosen mode of therapy,
the ultimate goal is achieving glycemic control to prevent perinatal and
maternal complications. Currently, no consensus exists regarding glycemic
goals in GDM. Controlled trials are needed to establish optimal target ranges
for glucose.
Medical Nutrition Therapy:
Medical nutrition therapy (MNT) is the cornerstone of therapy for GDM, and
the majority of women can be managed with MNT alone.1,17 The
primary goal of MNT is to achieve adequate glycemic control while maintaining
sufficient nutritional intake to support a healthy pregnancy. Patients with
GDM have individualized requirements for MNT, depending on prepregnancy weight
and micronutrient needs.11,17 As such, MNT is best managed by a
registered dietitian or other health care practitioner skilled in the area of
GDM. Success of MNT is measured by frequent monitoring of glucose levels and
assessment of weight gain throughout the pregnancy. Weight gain should be
appropriate for the stage of pregnancy, but should not be excessive.
In general, patients should limit
carbohydrates to 35% to 40% of total calories and should distribute
carbohydrate intake over three meals and two to four snacks per day.
1,14,18,19 In addition to the quantity of carbohydrates in the diet, the
type of carbohydrate may also be important. Eating carbohydrates with a low
glycemic index has been shown to lower postprandial glucose levels in
nonpregnant patients with diabetes. However, to date, no studies have
investigated the effects of glycemic index in women with GDM.17
Physical activity of 30 minutes per day is recommended as an adjunct to MNT in
women with GDM.11,17 Women should closely monitor fetal activity
and glucose levels pre- and post-exercise.
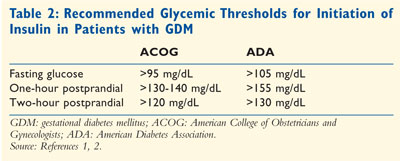
Insulin: Women who
do not achieve glycemic control from MNT alone should be placed on insulin
therapy.19 Recommendations for when to initiate insulin are
provided in Table 2. Insulin is classified into four categories:
rapid-acting, short-acting, intermediate-acting, and long-acting. Rapid-acting
insulins are most appropriate for targeting postprandial glucose levels, and a
basal-bolus regimen is recommended for patients with both elevated fasting and
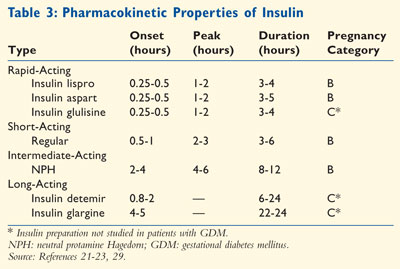
postprandial glucose.20 The pharmacokinetic properties of the
various insulin preparations are found in Table 3.21-23
Of the
insulin preparations, human regular insulin and human neutral protamine
Hagedorn (NPH) insulin have been the most extensively studied in pregnancy.
When compared to human regular insulin, the rapid-acting analogs lispro and
aspart have demonstrated comparable safety and efficacy in the management of
GDM.11,20 The two rapid-acting analogs may provide better
postprandial glycemic control and may be associated with fewer hypoglycemic
episodes. No data are available regarding the use of the rapid-acting analog
glulisine in pregnancy. A few case reports describe the use of long-acting
insulin glargine during pregnancy in women with type 1 diabetes; however, no
results of randomized, controlled trials examining the use of insulin glargine
in pregnancy are available.11,14,20,23 Likewise, controlled studies
of the long-acting analog insulin detemir in pregnancy have not been
performed. At this time, human NPH insulin remains the preferred basal insulin
for patients with GDM.11
Insulin requirements generally increase as pregnancy progresses and are often
much greater in morbidly obese women.13 As such, total daily dosing
requirements for insulin should be based on body weight and gestational week.
Insulin regimens should be individualized and adjusted to achieve glycemic
targets.
Sulfonylureas:
Sulfonylureas work by increasing insulin secretion from the pancreas. None of
the sulfonylureas are currently approved by the FDA for the treatment of GDM.
Of the sulfonylureas, glyburide has been the most extensively investigated in
the management of GDM.15 Langer et al. conducted a prospective
study comparing the use of glyburide and insulin in women with GDM.24
Glyburide levels were undetectable in the cord blood, indicating minimal
transfer across the placenta. In addition, glycemic control and perinatal
outcomes were comparable between the two groups.24 Several
retrospective reports have also documented the use of glyburide in GDM.
Approximately 80% of subjects treated with glyburide achieved successful
glycemic control, and the remainder required treatment with insulin therapy.
25 Based on these data, glyburide may be a reasonably safe alternative
to insulin therapy for women with GDM. However, larger randomized studies are
needed to fully assess neonatal outcomes and optimal dosing regimens.25
Glyburide is currently classified as pregnancy category C.22 Data
are lacking regarding the use of glipizide and glimepiride in pregnancy.
15,22
Biguanides: The only drug in the biguanide class is metformin, which
is FDA approved for use in type 2 diabetes, but not for use in GDM. Metformin
acts by reducing hepatic glucose production, increasing peripheral glucose
disposal, and reducing intestinal glucose absorption.15 Metformin
is a pregnancy category B drug.22 When used in pregnant patients,
metformin crosses the placenta readily, resulting in significant exposure to
the fetus. As human studies are limited, it is unknown if metformin is
teratogenic or beneficial to the fetus.16,22 To address issues
concerning metformin, the Metformin in Gestational Diabetes (MiG) trial is an
ongoing prospective, randomized multicenter trial designed to compare the use
of metformin and insulin in women with GDM.26 The primary outcome
measure of the trial is neonatal morbidity. In addition, the trial will assess
maternal glycemic control and follow offspring for five years after delivery.
Until data from studies such as the MiG trial are available, there is
inadequate evidence to recommend metformin for the treatment of GDM.
11,15,16
Postpartum Care
Women with GDM have an increased risk of developing diabetes after giving
birth.1,27 Finger-stick glucose should be measured in the immediate
postpartum period to rule out persistent hyperglycemia and a diagnosis of
diabetes.28 If early postpartum testing is negative, patients
should have a follow-up 75-g OGTT six to 12 weeks after delivery.1,11,28
Because 35% to 60% of women with GDM will develop type 2 diabetes within 10
years, a repeat OGTT should be conducted in one year and at least every three
years thereafter.11 Additionally, offspring of women with GDM are
at risk of developing obesity and abnormal glucose tolerance. Children should
have regular check-ups to evaluate height, weight, and blood glucose levels.
27
Pharmacist's Role
Pharmacists have a key role in helping to achieve
optimal outcomes for patients with GDM. They can educate high-risk patients on
the importance of obtaining screening for GDM as soon as possible after
pregnancy is established. Patients at average risk should also be counseled on
the benefits of screening for GDM at 24 to 28 weeks' gestation. For patients
who are diagnosed with GDM, pharmacists may provide information on how to
maximize diet and lifestyle modifications to achieve target glucose levels.
Additionally, pharmacists should ensure that patients are educated on the
appropriate technique for glucose monitoring. Pharmacists should inform
patients of consequences of uncontrolled GDM and the importance of controlling
blood glucose to minimize the risk of complications in the mother and fetus.
Although only a minority of patients with GDM require insulin therapy,
pharmacists should be prepared to advise these patients on proper
administration and timing of insulin injections. Lastly, pharmacists should
educate women with GDM on the significant risk of developing type 2 diabetes
later in life and should emphasize the need for continued follow-up to assess
the status of glucose metabolism.
Conclusion
GDM is characterized by onset or first recognition of glucose intolerance
during pregnancy. The underlying mechanisms of insulin resistance in GDM are
complex and have not yet been fully characterized. Glucose targets in GDM are
more stringent compared with other types of diabetes; however, most patients
with GDM can be successfully managed with a combination of MNT and exercise.
For patients who fail to achieve adequate glucose control with MNT,
pharmacologic therapy with insulin is indicated. Glyburide may be a reasonable
alternative to insulin therapy in the management of GDM. Risks of uncontrolled
GDM include fetal macrosomia, shoulder dystocia, and neonatal hypoglycemia. In
addition, a significant number of women with GDM will later develop type 2
diabetes. By educating patients with GDM, pharmacists can have a significant
impact on the health outcomes of both the mother and baby.
References
1. American Diabetes Association. Gestational diabetes mellitus (position statement). Diabetes Care. 2004;27(Suppl 1):S88-S90.
2. ACOG Practice Bulletin. Clinical management guidelines for obstetrician-gynecologists. Number 30, September 2001 (replaces Technical Bulletin Number 200, December 1994). Gestational diabetes. Obstet Gynecol. 2001;98:525-538.
3. Metzger BE, Coustan DR; The Organizing Committee. Summary and recommendations of the Fourth International Workshop-Conference on Gestational Diabetes Mellitus. Diabetes Care. 1998;21(Suppl 2):B161-B167.
4. King H. Epidemiology of glucose intolerance and gestational diabetes in women of childbearing age. Diabetes Care. 1998;21(Suppl 2):B9-B13.
5. Gabbe SG, Graves CR. Management of diabetes mellitus complicating pregnancy. Obstet Gynecol. 2003;102:857-868.
6. Evans E, Patry R. Management of gestational diabetes mellitus and pharmacists' role in patient education. Am J Health Syst Pharm. 2004;61:1460-1465.
7. Buchanan TA, Xiang A, Kjos SL, Watanabe R. What is gestational diabetes? Diabetes Care. 2007;30(Suppl 2):S105-S111.
8. Barbour LA, McCurdy CE, Hernandez TL, et al. Cellular mechanisms for insulin resistance in normal pregnancy and gestational diabetes. Diabetes Care. 2007;30(Suppl 2):S112-S119.
9. Ryan EA. Hormones and insulin resistance during pregnancy. Lancet. 2003;362:1777-1778.
10. Kaaja RJ, Greer IA. Manifestations of chronic disease during pregnancy. JAMA. 2005;294:2751-2757.
11. Metzger BE, Buchanan TA, Coustan DR, et al. Summary and recommendations of the Fifth International Workshop-Conference on Gestational Diabetes Mellitus. Diabetes Care. 2007;30(Suppl 2):S251-S260.
12. Brody SC, Harris R, Lohr K. Screening for gestational diabetes: a summary of the evidence for the U.S. Preventive Services Task Force. Obstet Gynecol. 2003;101:380-392.
13. Jovanovic L. Achieving euglycaemia in women with gestational diabetes mellitus: current options for screening, diagnosis, and treatment. Drugs. 2004;64:1401-1417.
14. Langer O. Management of gestational diabetes: pharmacologic treatment options and glycemic control. Endocrinol Metab Clin North Am. 2006;35:53-78, vi.
15. Feig DS, Briggs GG, Koren G. Oral antidiabetic agents in pregnancy and lactation: a paradigm shift? Ann Pharmacother. 2007;41:1174-1180.16. Coustan DR. Pharmacological management of gestational diabetes. Diabetes Care. 2007;30(Suppl 2):S206-S208.
17. Reader DM. Medical nutrition therapy and lifestyle interventions. Diabetes Care. 2007;30(Suppl 2):S188-S193.
18. American Diabetes Association. Nutrition principles and recommendations in diabetes (position statement). Diabetes Care. 2004;27(Suppl 1):S36-S46.
19. Jovanovic L, Pettitt DJ. Gestational diabetes mellitus. JAMA. 2001;286:2516-2518.
20. Jovanovic L, Pettitt DJ. Treatment with insulin and its analogs in pregnancies complicated by diabetes. Diabetes Care. 2007;30(Suppl 2):S220-S224.
21. Triplitt CL, Reasner CA, Isley WL. Diabetes mellitus. In: Dipiro JT, Talbert RL, Yee GC, et al. Pharmacotherapy: A Pathophysiologic Approach. 6th ed. New York, NY: McGraw-Hill; 2005:1345, 1357.
22. Briggs GG, Freeman RK, Yaffe SJ. Drugs in Pregnancy & Lactation. 7th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2005.
23. Homko CJ, Reece EA. Insulins and oral hypoglycemic agents in pregnancy. J Matern Fetal Neonatal Med. 2006;19:679-686.
24. Langer O, Conway DL, Berkus MD, et al. A comparison of glyburide and insulin in women with gestational diabetes mellitus. N Engl J Med. 2000;343:1134-1138.
25. Moore TR. Glyburide for the treatment of gestational diabetes: a critical appraisal. Diabetes Care. 2007;30(Suppl 2):S209-S213.
26. Rowan JA (for the MiG Investigators). A trial in progress: gestational diabetes. Treatment with metformin compared with insulin (the Metformin in Gestational Diabetes [MiG] trial). Diabetes Care. 2007;30(Suppl 2):S214-S219.
27. Kjos SL, Buchanan TA. Gestational diabetes mellitus. N Engl J Med. 1999;341:1749-1756.
28. Kitzmiller JL, Dang-Kilduff L, Taslimi MM. Gestational diabetes after delivery. Diabetes Care. 2007;30(Suppl 2):S225-S235.
29. Levemir [package insert].
Princeton, NJ: Novo Nordisk Inc.; 2005.
To comment on this article, contact editor@uspharmacist.com.





