US Pharm. 2012;37(9):HS17-HS20.
Dyslipidemia is a major risk factor for coronary heart disease (CHD), and current guidelines support low-density lipoprotein cholesterol (LDL-C) as a primary target of therapy.1 Previous studies suggest that increasing high-density lipoprotein cholesterol (HDL-C) and reducing triglycerides and small LDL particles may also have a positive impact in prevention.2 These factors are considered secondary targets of lipid management. Most lipid-altering drugs have a sound overall safety profile and are generally well tolerated.1
Episodes of severe hepatotoxicity remain rare for most drugs. The exception is high-dose, sustained-release (SR) niacin. Overall, the incidence of drug-induced hepatotoxicity may be prevented if both providers and patients are aware of potential contributing factors.
Clinical Presentation
Drug-induced hepatotoxicity secondary to lipid-altering agents includes acute liver failure, hepatitis, cholestasis, and most commonly transaminitis, an asymptomatic elevation in serum transaminases.3 Acute liver failure is extremely rare, and data suggest that minor asymptomatic elevations of aspartate transaminase (AST) and alanine transaminase (ALT) do not necessarily precede acute liver failure.3 Possible signs and symptoms of liver problems include unusual fatigue or weakness, loss of appetite, upper abdominal pain, dark-colored urine, and yellowing of the skin or whites of the eyes (jaundice).4
Hepatotoxicity by Drug Class
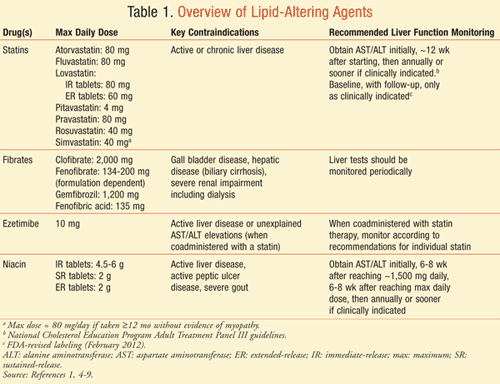
The major classes of lipid-altering agents include the statins, bile acid resins (BARs), fibric acid derivatives (fibrates), cholesterol absorption inhibitors, niacin, and fish oil (TABLE 1).1,4-9 Because reports of hepatotoxicity are extremely limited with fish oil and BARs, these drug classes will not be a focus of this review. Additionally, red yeast rice (RYR) is an available supplement with potential lipid-altering properties. Reports of hepatotoxicity with this agent are also limited and will not be discussed. However, practitioners should be aware that RYR typically contains varying amounts of lovastatin, and therefore should be utilized with applicable precautions.10
Cholesterol agents cause hepatotoxic effects through various mechanisms. For instance, statins undergo hepatic metabolism following gastrointestinal (GI) absorption, while other classes such as BARs and the cholesterol absorption inhibitor ezetimibe primarily target the GI tract but indirectly affect the liver.11
Statins
Statins (e.g., atorvastatin, fluvastatin, lovastatin, pitavastatin, pravastatin, rosuvastatin, simvastatin) produce marked reductions in LDL-C by inhibiting 3-hydroxy-3-methylglutaryl-coenzyme A (HMG-CoA) reductase, the rate-limiting step in cholesterol synthesis.1 This inhibition decreases cholesterol production, causing an increase in LDL-receptor expression and enhanced removal of LDL-C from the circulation. Although statins have moderate effects on lowering triglycerides and increasing HDL-C, they remain first-line therapy because of their LDL-C lowering. More importantly, results from multiple clinical trials have demonstrated that statins significantly reduce major coronary events and overall mortality among primary and secondary prevention populations.1,12 Statins also reduce inflammation, improve endothelial function, and stabilize atherosclerotic plaque, independent of their lipid effects.3,12
Clinical trial findings indicate that the overall risk of hepatotoxicity with statins is low. The most common hepatic adverse event involves asymptomatic increases in ALT and AST. This dose-dependent reaction usually occurs within the first year of therapy, but may present at any time.3,13 It has been noted that elevations are usually reversible with a dose reduction and may normalize with the same continued dosage.1
The National Cholesterol Education Program (NCEP) Adult Treatment Panel III (ATP-III) guidelines provide specific recommendations for monitoring hepatic function including transaminase elevations (TABLE 1).1 For patients with AST/ALT ≤3 times the upper limit of normal (ULN), statin therapy can be continued. If elevations exceed 3 times the ULN, a second liver function evaluation should be conducted. If elevated levels persist, the statin should be discontinued, but attempting a rechallenge or switching to a different statin may be considered.1 Overall elevated transaminase levels ≥3 times the ULN occur in <2% of patients treated with statin monotherapy.1,3
Statin-induced transaminase elevations rarely progress to irreversible liver damage. In 2003, a meta-analysis of 164 statin trials reported no cases of liver failure.14 From 1987 to 2000, the FDA recorded 30 cases of statin-induced liver failure, equal to approximately one case per 1 million person-years of use.14 There have been isolated case reports describing statin-associated cholestatic hepatotoxicity, autoimmune hepatitis, fulminant hepatitis, and cirrhosis.5 If transaminase levels are elevated and statin-induced hepatotoxicity is suspected, the National Lipid Association’s (NLA) Liver Expert Panel recommends obtaining a fractionated bilirubin level.15 When no biliary obstruction is present, bilirubin is a more reliable indicator of drug-induced liver injury. Elevated transaminase and bilirubin levels likely indicate ongoing liver injury, prompting the need for more tests to determine etiology.15 Hepatotoxicity may be increased with high statin doses, concomitant administration of CYP450 enzyme inhibitors or inducers, combination lipid-altering regimens, or impaired renal function, and among elderly patients.13
The value of routine transaminase monitoring in treated patients has been called into question because of the rarity of statin-induced irreversible liver damage.16 In a 2006 report, the NLA stated there is no evidence linking elevated AST/ALT with subsequent serious liver injury, nor data supporting the effectiveness of routine monitoring in identifying patients likely to progress to liver failure.15 Concerns with frequent monitoring include unnecessary costs and the potential of elevated transaminase levels leading to inappropriate statin discontinuation. Statin refusal and nonadherence are also of concern due to patients’ perception of potential liver damage.15
In support of the NLA Liver Expert Panel, the FDA recently revised statin labeling by removing the recommendation for routine periodic monitoring of liver enzymes. Baseline tests are still suggested, but follow-up monitoring is only necessary if clinically indicated, as the FDA has determined that frequent monitoring plays little to no role in detecting or preventing serious liver injury.4
Fibric Acid Derivatives (Fibrates)
Fibrates (e.g., clofibrate, fenofibrate, gemfibrozil, fenofibric acid) are primarily prescribed to reduce triglycerides, with usual reductions of 25% to 50%.1 The agents have mixed effects on LDL-C.1 With hypertriglyceridemia, fibrates typically increase LDL-C, whereas modest reductions may be observed when triglyceride levels are normal.1 Fibrates are often used in combination with statins, but an increased risk of myopathy and elevated transaminase levels have been observed. This is more likely with gemfibrozil, secondary to this agent increasing serum levels of most statins.17 However, if the concomitant statin dose remains low to moderate, adverse events including hepatotoxicity generally remain low.18 In instances of transaminase elevations, levels normalized within weeks after drug discontinuation.8
The NLA or NCEP ATP-III guidelines do not provide specific recommendations for liver function monitoring with fibrate therapy.1 However, baseline measures, periodic follow-up monitoring, and reduction or discontinuation of therapy with transaminase levels ≥3 times the ULN is prudent. Additionally, clinicians should be cognizant of factors that may increase risk of hepatotoxicity such as drug interactions or pre-existing liver disease.
Cholesterol Absorption Inhibitor (Ezetimibe)
Ezetimibe decreases LDL-C by inhibiting cholesterol absorption at the brush border of the intestine.5 This agent is not metabolized by the CYP450 enzyme system and does not interact with CYP3A4 inhibitors. Following absorption, ezetimibe is glucuronidated to produce an active metabolite that undergoes enterohepatic recirculation.16
Clinical trial data indicate that the incidence of asymptomatic elevated transaminase levels ≥3 times the ULN is 0.7%, which is similar to placebo.7 Because of the infrequency, no specific recommendations are available for monitoring hepatic function with ezetimibe monotherapy.19 Transaminase levels may be slightly higher with combination ezetimibe-simvastatin compared to simvastatin alone.20 Safety results from a trial involving atorvastatin monotherapy versus atorvastatin-ezetimibe showed no significant difference in transaminase elevations.21 The value of monitoring liver function among patients receiving a statin-ezetimibe regimen is similar to that of statin therapy; obtain measures at baseline and thereafter when clinically indicated, such as in dose titration.19
Niacin
Niacin, also known as vitamin B3 or nicotinic acid, has positive effects on all major lipid parameters including LDL-C, non-HDL, and triglycerides, when given at appropriate therapeutic doses.1 It is also the most efficacious drug for raising HDL-C.22 Niacin therapy may lead to regression in mean carotid intima-media thickness in patients with CHD whose LDL-C is at goal with statin therapy.23 However, findings from a recent clinical trial indicate that niacin did not produce further reductions in vascular events when added to statin therapy.24
There are primarily three different formulations of niacin: immediate-release (IR) or crystalline, extended-release (ER), and SR, with approximate absorption rates of 1 hour, 8 hours, and 12 hours, respectively.22 A considerable amount of confusion exists regarding the various dosages, drug-delivery systems, effects on the lipid profile, and potential adverse events, including hepatotoxicity. IR niacin is available as a supplement and as prescription Niacor. Niacin is also available as a prescription ER product, Niaspan. Various long-acting formulations are available as supplements and marketed as “time-released” or “sustained-release.” Monitoring hepatic function is recommended for all niacin formulations (TABLE 1).
Adverse events for IR niacin include flushing, chills, pruritus, and GI upset, with a very low incidence of hepatotoxicity.22 Extended-release niacin is associated with lower flushing rates and a low incidence of hepatotoxicity at doses ≤2,000 mg/day. Conversely, SR is commonly associated with more dose-dependent transaminase elevations.22 A comparative study indicated that approximately 50% of those receiving SR niacin experienced hepatotoxicity, especially with doses >2,000 mg/day, compared to none in the IR niacin group.25
The differences in hepatotoxicity among formulations are likely explained by two metabolic pathways.22 Conjugation of niacin with glycine to form nicotinuric acid is a low-affinity, high-capacity system, which leads to flushing. The second nonconjugative pathway involves multiple reactions that convert niacin to nicotinamide, and is a high-affinity, low-capacity system with greater potential for hepatotoxicity. IR products will quickly saturate the nonconjugative pathway, with most of the drug being metabolized by conjugation, resulting in increased flushing and a low incidence of hepatotoxicity. Slowly absorbed preparations (e.g., SR niacin) are metabolized primarily by the high-affinity nonconjugative pathway, resulting in less flushing but increased hepatotoxicity.
Pharmacists must inform patients that maximum dosages vary among formulations and dose-dependent hepatotoxicity is possible, especially when patients choose SR formulations in an effort to avoid flushing, reduce cost, or self-treat. Additionally, products may not be interchangeable. For example, if a patient has been maintained on IR niacin at a dose >2,000 mg/day, switching to an equivalent dose of SR niacin would likely result in hepatotoxicity. Lastly, “flush-free” and “no flush” formulations contain very little to no active niacin but list ingredients such as inositol hexanicotinate. These products have not shown the same cardiovascular and lipid-lowering benefits as niacin.22
Conclusion
Severe drug-induced hepatotoxicity is rare for most lipid-altering agents. However, the incidence increases with certain agents and in the presence of other contributing factors. Appropriate monitoring may limit hepatotoxic events. Asking pertinent questions and gathering needed information will help determine the risk for hepatotoxicity with lipid-altering therapy. Key information includes identifying disease states that may predispose the patient to increased risk for liver damage and obtaining a complete medication and supplement list to check for potential interactions. Pharmacists may also educate patients on the importance of reporting any unusual signs or symptoms of hepatotoxicity and adhering to laboratory and clinic appointments.
The pharmacist in the community setting has the opportunity to identify patients who self-treat with supplements and OTC medications. Education on appropriate use is essential. Specific opportunities include those patients on statins who self-treat with RYR, and patients switching from IR or ER niacin to equivalent doses of SR niacin. For a provider, it is important to be vigilant in identifying patients who may be at increased risk of hepatotoxicity secondary to lipid-altering agents. In such cases the pharmacist may recommend a dose reduction, discontinuation of therapy, or selection of an alternative agent.
REFERENCES
1. Third Report of the National Cholesterol Education
Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of
High Blood Cholesterol in Adults (Adult Treatment Panel III) final
report. Circulation. 2002;106:3143-3421.
2. Sang ZC, Wang F, Zhou Q, et al. Combined use of
extended-release niacin and atorvastatin: safety and effects on lipid
modification. Chin Med J. 2009;122:1615-1620.
3. Vasudevan AR, Hamirani YS, Jones PH. Safety of statins: effects on muscle and the liver. Cleve Clin J Med. 2005;72:990-993, 996-1001.
4. Jefferson E. FDA news release: FDA announces safety
changes in labeling for some cholesterol-lowering drugs. February 28,
2012. www.fda.gov/NewsEvents/Newsroom/PressAnnouncements/ucm293623.htm.
Accessed July 5, 2012.
5. Bhardwaj SS, Chalasani N. Lipid-lowering agents that cause drug-induced hepatotoxicity. Clin Liver Dis. 2007;11:597-613, vii.
6. FDA drug safety communication: new restrictions,
contraindications, and dose limitations for Zocor (simvastatin) to
reduce the risk of muscle injury. December 15, 2011.
www.fda.gov/Drugs/DrugSafety/ucm256581.htm. Accessed July 5, 2012.
7. Dujovne CA, Suresh R, McCrary Sisk C, et al. Safety and
efficacy of ezetimibe monotherapy in 1624 primary hypercholesterolaemic
patients for up to 2 years. Int J Clin Pract. 2008;62:1332-1336.
8. Athyros VG, Papageorgiou AA, Hatzikonstandinou HA, et
al. Safety and efficacy of long-term statin-fibrate combinations in
patients with refractory familial combined hyperlipidemia. Am J Cardiol. 1997;80:608-613.
9. Jones PH, Bays HE, Davidson MH, et al. Evaluation of a
new formulation of fenofibric acid, ABT-335, co-administered with
statins: study design and rationale of a phase III clinical programme. Clin Drug Inves. 2008;28:625-634.
10. Lachenmeier DW, Monakhova YB, Kuballa T, et al. NMR
evaluation of total statin content and HMG-CoA reductase inhibition in
red yeast rice (Monascus spp.) food supplements. Chin Med. 2012;7:8.
11. Pugh AJ, Barve AJ, Falkner K, et al. Drug-induced hepatotoxicity or drug-induced liver injury. Clin Liver Dis. 2009;13:277-294.
12. Girotra S, Murarka S, Migrino RQ. Plaque regression
and improved clinical outcomes following statin treatment in
atherosclerosis. Panminerva Med. 2012;54:71-81.
13. Parra JL, Reddy KR. Hepatotoxicity of hypolipidemic drugs. Clin Liver Dis. 2003;7:415-433.
14. Law MR, Wald NJ, Rudnicka AR. Quantifying effect of
statins on low density lipoprotein cholesterol, ischaemic heart disease,
and stroke: systematic review and meta-analysis. BMJ. 2003;326:1423.
15. Cohen DE, Anania FA, Chalasani N. An assessment of statin safety by hepatologists. Am J Cardiol. 2006;97:77C-81C.
16. Hou R, Goldberg AC. Lowering low-density lipoprotein
cholesterol: statins, ezetimibe, bile acid sequestrants, and
combinations: comparative efficacy and safety. Endocrinol Metab Clin North Am. 2009;38:79-97.
17. Backes JM, Howard PA, Ruisinger JF, Moriarty PM. Does simvastatin cause more myotoxicity compared with other statins? Annals Pharmacother. 2009;43:2012-2020.
18. Murdock DK, Murdock AK, Murdock RW, et al. Long-term
safety and efficacy of combination gemfibrozil and HMG-CoA reductase
inhibitors for the treatment of mixed lipid disorders. Am Heart J. 1999;138:151-155.
19. Zetia (ezetimibe) package insert. Whitehouse Station, NJ: Merck & Co., Inc; June 2012.
20. Goldman-Levine JD, Bohlman LG. Ezetimibe/Simvastatin (vytorin) for hypercholesterolemia. Am Fam Physician. 2005;72:2081-2082.
21. Conard S, Bays H, Leiter LA, et al. Ezetimibe added to
atorvastatin compared with doubling the atorvastatin dose in patients
at high risk for coronary heart disease with diabetes mellitus,
metabolic syndrome or neither. Diabetes Obes Metab. 2010;12:210-218.
22. Backes JM, Padley RJ, Moriarty PM. Important
considerations for treatment with dietary supplement versus prescription
niacin products. Postgrad Med. 2011;123:70-83.
23. Taylor AJ, Villines TC, Stanek EJ, et al. Extended-release niacin or ezetimibe and carotid intima-media thickness. N Engl J Med. 2009;361:2113-2122.
24. Boden WE, Probstfield JL, Anderson T, et al. Niacin in
patients with low HDL cholesterol levels receiving intensive statin
therapy. N Engl J Med. 2011;365:2255-2267.
25. McKenney JM, Proctor JD, Harris S, Chinchili VM. A
comparison of the efficacy and toxic effects of sustained- vs.
immediate-release niacin in hypercholesterolemic patients. JAMA. 1994;271:672-677.
To comment on this article, contact rdavidson@uspharmacist.com.






