US Pharm. 2013;38(7):HS10-HS14.
ABSTRACT: Anaphylaxis is a severe allergic reaction that often presents in an outpatient setting. Currently, there is limited literature on the prevalence, cause, and risk factors of anaphylaxis in a hospital setting. However, it has been found that certain medications, latex, food, and contrast media may increase a patient’s risk for anaphylaxis. With the influence of clinical pharmacists and more patient-based care teams, hospital-induced anaphylaxis can be prevented.
Anaphylaxis is considered a medical emergency, which requires immediate treatment due to its potentially fatal outcomes.1,2 This condition is often seen in the outpatient setting, with limited literature describing the incidence and cause of hospital-induced anaphylaxis. Severe anaphylaxis occurs relatively infrequently among hospitalized patients, with an average risk of about 1 case per 5,000 admissions.3 However, studies report that anaphylaxis is not as rare as previously considered, with an estimated 1.2% to 1.5% of the total U.S. population being affected and 0.002% experiencing a fatal event.4
RISK FACTORS
There are many triggers that have been shown to increase the risk of hospital-induced anaphylaxis. Previous studies have shown an increased risk in females, patients under 20 years of age, and those admitted into the vascular surgery unit.2,4 TABLE 1 further introduces the risk factors of anaphylaxis.4-7

PATHOPHYSIOLOGY
Anaphylaxis, or type 1 hypersensitivity reaction, can be classified as immuno-logic, idiopathic, or nonimmunologic.8 Immunologic reactions are the most commonly observed type of anaphy-laxis in a hospital setting. These reactions are often triggered by an exposure to immunoglobulin-dependent factors such as foods, venoms, latex, and drugs, or by other factors such as blood products or immune aggregates. They can be classified as immunoglobulin E (IgE)-dependent or IgE-independent reactions.9,10 IgE-dependent anti-bodies, which are commonly seen in hospital-induced anaphylaxis, are the main activators of the allergic response shown in FIGURE 1.1,8-11 This reaction is caused by the cross-linking between the antibody and the high affinity Fc (fragment crystallizable) receptor, which is present on mast cells and basophils. This binding, in addition to calcium influx, causes mast cells and/or basophils to induce degranulation. The degranulation further results in the vascular permeability and smooth muscle contraction seen in anaphylaxis.8,10
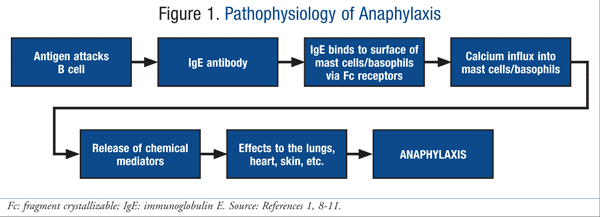
During the degranulation phase, multiple biochemical mediators and chemotactic substances are released. Common substances include cytokines, prostaglandins, and histamine.8,10 Histamine is a major mediator that has the potential of causing tachycardia, bronchospasm, and hypotension. A diagnosis of anaphylaxis can be made based on a patient’s clinical symptoms. However, during an attack, histamine and tryptase are the most commonly monitored mediators when evaluating the severity of a reaction.8 In contrast to histamine, tryptase can be used to determine both the severity and the cause of the anaphylactic reaction (i.e., drug, insect, food).8
SIGNS AND SYMPTOMS
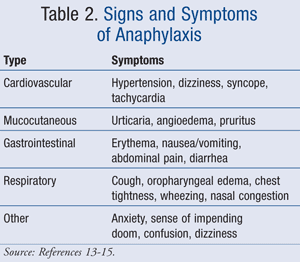
The clinical presentation of hospital-acquired anaphylaxis is similar to the presentation experience in an outpatient setting.2,3 Anaphylaxis symptomology may affect a variety of systems that include, but are not limited to, the cardiovascular, respiratory, gastrointestinal, and mucocutaneous systems.12 Symptoms involving the cardiovascular system include syncope, tachycardia, and hypotension, which in turn affects perfusion to certain organs. Symptoms involving the respiratory system include wheezing, chest tightness, and dyspnea.
The International Collaborative Study of Severe Anaphylaxis (ICSA), which evaluated severe anaphylactic reactions among hospitalized patients, documented that approximately 79% of patients with hospital-acquired anaphylaxis presented with a respiratory component, 70% presented with a cardiovascular component, and 49% presented with both respiratory and cardiovascular symptoms.3 Other common symptoms noted in this and previous studies are outlined in TABLE 2.13-15 It is important to note that the presentation of anaphylaxis may vary from person to person; therefore the absence of common symptoms should not rule out the possibility of anaphylaxis.12
CAUSES OF ANAPHYLAXIS
Drug-Induced Anaphylaxis in a Hospital Setting
Various studies have documented possible triggers for anaphylaxis in a hospital and surgical setting. While there are many causes for anaphylaxis in a nonsurgical hospital setting, medications have been found to be the most frequent cause.2,3 The ICSA grouped medications and other agents into three major categories based on their risk of causing anaphylaxis in a nonsurgical hospital setting (TABLE 3).16 These categories included the following: relatively low risk, 5 to 15 episodes per 100,000 exposed patients; intermediate risk, 30 to 100 episodes per 100,000 exposed patients: and high risk, 100 episodes per 100,000 exposed patients. The ICSA observed that streptokinase, platelet concentrates, and snake antivenom posed the highest risk for anaphylaxis in a hospital setting. This was followed by parenteral penicillin, iodinated radiologic contrast, blood products, and dextran, which carried an intermediate risk, while nonsteroidal anti-inflammatory drugs (NSAIDs) and antibiotics, excluding parenteral penicillin, carried the lowest risk.16
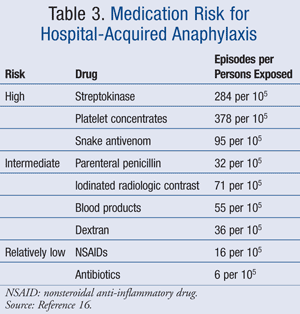
Within these categories, the ICSA found that of the NSAIDs evaluated, diclofenac suppositories were found to have the highest risk of anaphylaxis (16 per 100,000) when compared to aspirin (2.1 per 100,000) and oral and parenteral formulations of diclofenac (7.2 per 100,000 and 9.0 per 100,000, respectively).2,16 This study also documented that ionic contrast media (71 per 100,000) had a higher risk for inducing anaphylaxis than nonionic contrast media (35 per 100,000).16 This finding is consistent throughout a number of studies documenting the risk of anaphylaxis induced by contrast media.17-19
Surgical procedures requiring general anesthesia pose a major risk for life-threatening anaphylactic reactions.20 Similar to anaphylaxis in the nonsurgical setting, anaphylaxis in the surgical setting is also associated with the use of certain medications. Neuromuscular blocking agents (NMBAs), such as rocuronium, have the highest correlation with anaphylaxis while under general anesthesia (61.6%).21,22 This is followed by latex (16.6%), antibiotics (8.3%), colloids (2.7%), and opioids (2.7%).
Medications that are derived from an animal source can also trigger an anaphylactic reaction. Although there is limited literature on the prevalence of medication-induced anaphylaxis from animal-derived products in a hospital setting, there are some animal-derived medications that have been associated with anaphylaxis, such as insulin.23 Of the insulin-induced anaphylaxis cases that have been documented, porcine insulin was found to be less allergenic than bovine insulin.24,25 Other animal-derived products that have been associated with an immune response include bovine thrombin (IgG mediated) and porcine gut heparin (IgG and IgE).24,25
Nondrug-Induced Anaphylaxis
Latex: Outside of medication-induced anaphylaxis, hospital-acquired anaphylaxis can also be triggered by other factors. One factor in particular is natural rubber latex (NRL). As mentioned earlier, latex has been found to be the second most common cause for anaphylaxis in a surgical setting. It has been found that extended periods of exposure to NRL can lead to sensitization, which is a prerequisite to type I immediate hypersensitivity reactions such as anaphylaxis. Because of this, individuals who have undergone multiple surgical procedures and those with long-term bladder care (i.e., use of urinary catheters) are at greater risk for developing anaphylaxis to NRL.22,26,27 Commonly used NRL products, which include balloon-tipped catheters used in arterial catheterization, should not be used with patients who have been sensitized to latex or those who have had a past reaction to latex. A list of NRL products is presented in TABLE 4.28,29

Food and Other: As with anaphylaxis in an outpatient setting, food allergies can also trigger a reaction in hospitalized patients.2 In contrast to medication- and latex-induced anaphylaxis, there are limited data analyzing food-induced anaphylaxis in hospital settings. However, though the data are limited, it should be noted that all foods have the potential to cause anaphylaxis. Studies have found that peanuts are associated with the majority of severe food-induced anaphylaxis, followed by tree nuts and animal-related food products (i.e., cow’s milk and hen’s eggs).12,30 If a patient has a recorded history of a severe food allergy, it could be hypothesized that food contamination within the hospital setting could possibly hinder food allergen avoidance.
In addition to ingestion of certain foods, physical contact with allergens could lead to a reaction. Allergens that are present on sheets, surgical equipment, and other materials within the hospital could trigger a response. Therefore, health professionals should aim to be more vigilant to limit potential exposure to allergens.
TREATMENT
The treatment of anaphylaxis is similar in both an outpatient and an inpatient setting.31 Retrospective evaluations of anaphylaxis episodes indicate that epinephrine, oxygen, and fluid resuscitation are the cornerstones for any successful treatment.29 A stepwise approach to treating anaphylaxis follows.
1. Removal of Trigger
The first step in treating any form of anaphylaxis is to remove the offending agent.
2. Epinephrine
Epinephrine is considered the first-line drug of choice for anaphylaxis.5 It targets alpha1-adrenergic receptors throughout most of the body, which gives it the ability to relieve airway swelling, hypotension, and shock.5 Epinephrine is dosed at 0.01 mg/kg with a maximum dose of 0.5 mg in adults and 0.3 mg in children. In more severe cases of anaphylaxis, the dose can be repeated every 5 to 15 minutes as needed. If cardiac arrest is imminent or has already occurred, an IV bolus dose of epinephrine is indicated. The use of IV epinephrine has potentially fatal consequences (i.e., fatal cardiac arrhythmias) and should be avoided, if possible.5,32
3. Oxygen
All patients with respiratory distress and those receiving repeated doses of epinephrine should be given oxygen at a flow rate of 6 to 8 L/min.5 Oxygen is also suggested in patients with concomitant asthma, other chronic respiratory disease, or cardiovascular disease.
4. Patient Placement
Patients with anaphylaxis should be placed on their back or in a comfortable position with their lower extremities elevated.5 The proper placement of the patient during anaphylaxis preserves circulation. Furthermore, observations of victims of fatal anaphylactic shock suggest that postural changes might have contributed to a fatal outcome.33
5. Fluid Resuscitation
During anaphylaxis, large amounts of fluid are secreted from a patient’s circulation, therefore requiring IV infusion of normal saline.5 The rate of administration is dependent upon the blood pressure, cardiac rate, cardiac function, and urine output.
6. Observation
After the treatment of an anaphylactic reaction, an observation period lasting 4 to 6 hours is suggested, since an anaphylactic reaction might recur once the effect of the epinephrine wears off.5 Prolonged observation periods are suggested for patients with severe or refractory symptoms.33
7. Adjunct Medications
Potent vasopressors (i.e., norepinephrine, vasopressin, or metaraminol) may be used to overcome vasodilation and shock if epinephrine and fluid resuscitation have failed in maintaining a systolic blood pressure >90 mm Hg.33
Antihistamines have been reported to be effective in attenuating the cutaneous manifestations of anaphylaxis.33 Intravenous or intramuscular diphenhydramine (H1-antagonist) can be given at 25 to 50 mg for adults and 1 mg/kg (max 50 mg) for children.33 Treatment with a combination of H1- and H2-antagonists has been reported to be more effective than treatment with H1-antagonists alone.33 Two common H2-antagonists used in combination with H1-antagonists are ranitidine and cimetidine.33
PHARMACISTS’ ROLE
With the increased presence of clinical pharmacists in the hospital setting, pharmacists can play a major role in the prevention and treatment of anaphylaxis. Pharmacists may contribute to the prevention of anaphylaxis by identifying medications that can be cross-reactive with documented allergies. There are many medications that are cross-reactive to certain allergies. This knowledge allows pharmacists to better assist hospital providers, as they can recommend safer medication alternatives that have a lower chance of inducing a possible life-threatening anaphylaxis.34
It is also important that pharmacists be aware of the “desensitization protocol” that is used at their facility by an allergist. During the desensitization process, patients can be given repeated doses in larger quantities with a chance of a severe reaction, so immediate access to emergency medications is required.34
Pharmacists can also ensure that there is an accurate, up-to-date list of the patient’s medication, latex, and food allergies. In a hospital setting, it is common for either the nurse or provider to document allergy information. Pharmacists, however, may play a vital role by verifying and/or clarifying allergy information from numerous sources such as patient records, their outpatient pharmacy, or the patient or a family member.34 Additional roles include assisting health care providers with proper documentation of reactions, providing knowledge of medications or other agents that have a high risk for inducing anaphylaxis, and being fully informed about the drugs that are used to treat and/or manage anaphylaxis.
CONCLUSION
Although there is limited literature evaluating hospital-acquired anaphylactic reactions, it has been documented that they occur less frequently than observed in an outpatient setting.35 Due to its potential unpredictability and seriousness, anaphylaxis should never be labeled as minor in severity.36 Reports have shown that medications are the most frequent cause of anaphylaxis in admitted patients.2 Such reported data further validate the importance of pharmacists and their role in the prevention and management of hospitalized-induced anaphylaxis. With the lack of research on anaphylaxis that originates in a hospital setting, all health care providers must work together to ensure the safety of their patients.
REFERENCES
1. Pastorello EA, Rivolta F, Bianchi M, et al. Incidence
of anaphylaxis in the emergency department of a general hospital in
Milan. J Chromatogr B Biomed Sci Appl. 2001;756:11-17.
2. Tejedor Alonso MA, Moro MM, Hernandez JE, et al. Incidence of anaphylaxis in hospitalized patients. Int Arch Allergy Immunol. 2011;156:212-220.
3. The International Collaborative Study of Severe
Anaphylaxis. An epidemiologic study of severe anaphylactic and
anaphylactoid reactions among hospital patients: methods and overall
risks. Epidemiology. 1998;9:141-146.
4. Lieberman P, Camargo CA, Bohlke K, et al. Epidemiology
of anaphylaxis: findings of the American College of Allergy, Asthma, and
Immunology Epidemiology of Anaphylaxis Working Group. Ann Allergy Asthma Immunol. 2006;97:596-602.
5. Simmons FE, Ardusso LR, Bio MB, et al. World Allergy
Organization guidelines for the assessment and management of
anaphylaxis. J Allergy Clin Immunol. 2011;593:1-22
6. Cianferoni A, Novembre E, Mugnaini L, et al. Clinical
features of acute anaphylaxis in patients admitted to a university
hospital: an 11-year retro-spective review (1985-1996). Ann Allergy Asthma Immunol. 2001;87:27-32.
7. Moneret-Vautrin DA, Morisset M, et al. Epidemiology of life-threatening and lethal anaphylaxis: a review. Allergy. 2005;60:443-451.
8. Khan BQ, Kemp SF. Pathophysiology of anaphylaxis. Curr Opin Allergy Clin Immunol. 2011;11:319-325.
9. Demoly P, Bousquet J. Epidemiology of drug allergy. Curr Opin Allergy Clin Immunol. 2001;1:305-310.
10. Peavy RD, Metcalfe DD. Understanding the mechanisms of anaphylaxis. Curr Opin Allergy Clin Immunol. 2008;8:310-315.
11. van der Klauw MM, Wilson JH, Stricker BH.
Drug-associated anaphylaxis: 20 years of reporting in the Netherlands
(1974-1994) and review of the literature. Clin Exper Allergy. 1996;26:1355-1363.
12. Bock SA, Muñoz-Furlong A, Sampson HA. Fatalities due to anaphylactic reactions to foods. J Allergy Clin Immunol. 2001;107:191-193.
13. Kim H, Fischer D. Anaphylaxis. Allergy Asthma Clin Immunol. 2011;7:1-7.
14. Waserman S, Chad Z, Francoeur MJ, et al. Management of
anaphylaxis in primary care: Canadian expert consensus recommendations.
Allergy. 2010;65:1082-1092.
15. Webb LM, Lieberman P. Anaphylaxis: a review of 601 cases. Ann Allergy Asthma Immunol. 2006;97:39-43.
16. The International Collaborative Study of Severe
Anaphylaxis. Risk of anaphylaxis in a hospital population in relation to
the use of various drugs. Pharmacoepidemiol Drug Saf. 2003;12:195-202.
17. Katayama H, Yamaguchi K, Kozuka T, et al. Adverse
reactions to ionic and nonionic contrast media: a report from the
Japanese Committee on the Safety of Contrast Media. Radiology. 1990;175:621-628.
18. Shehadi WH, Toniolo G. Adverse reactions to contrast media. Radiology. 1980;137:299-302.
19. Palmer FG. The RACR survey of intravenous contrast media reactions: final report. Australas Radiol. 1988;32:426-428.
20. Chong YY, Caballero MR, Lukawska J, et al. Anaphylaxis
during general anaesthesia: one-year survey from a British allergy
clinic. Singapore Med J. 2008;49:483-487.
21. Laxenaire MC. Epidemiology of anesthetic anaphylactoid reactions. Fourth multicenter survey. Ann Fr Anesth Reanim. 1999;18:796-809.
22. Mertes PM, Laxenaire MC. Allergy and anaphylaxis in anaesthesia. Minerva Anestesiol. 2004;70:285-291.
23. Ghazavi MK, Johnston GA. Insulin allergy. Clin Dermatol. 2011;29:300-305.
24. Ness P, Creer M, Rodgers GM, et al. Building an
immune-mediated coagulopathy consensus: early recognition and evaluation
to enhance post-surgical patient safety. Patient Saf Surg. 2009;3:8.
25. Harada A, Tatsuno K, Kikuchi T, et al. Use of bovine
lung heparin to obviate anaphylactic shock caused by porcine gut
heparin. Ann Thorac Surg. 1990;49:826-827.
26. Garabrant DH, Roth HD, Parsad R, et al. Latex sensitization in health care workers and in the US general population. Am J Epidemiol. 2001;150:515-522.
27. Thong BY, Yeow-Chan. Anaphylaxis during surgical and interventional procedures. Ann Allergy Asthma Immunol. 2004;92:619-628.
28. Yunginger JW. Latex associated anaphylaxis. Immunol Allergy Clin North Am. 2001;21:669-677.
29. Ownby DR, Tomlanovich M, Sammons N, et al. Anaphylaxis associated with latex allergy during barium enema examinations. AJR Am J Roentgenol. 1991;156:903-908.
30. Hompes S, Köhli A, Nemat K, et al. Provoking allergens
and treatment of anaphylaxis in children and adolescents—data from the
anaphylaxis registry of German-speaking countries. Pediatr Allergy Immunol. 2011;22:568-574.
31. Sampson HA. Anaphylaxis and emergency treatment. Pediatrics. 2003;111:1601-1608.
32. McLean-Tooke A, Bethune CA, Fay AC, Spickett GP. Adrenaline in the treatment of anaphylaxis: what is the evidence? BMJ. 2003;327:1332-1335.
33. Sampson HA, Muñoz-Furlong A, Campbell RL, et al.
Second symposium on the definition and management of anaphylaxis:
summary report—Second National Institute of Allergy and Infectious
Disease/Food Allergy and Anaphylaxis Network symposium. J Allergy Clin Immunol. 2006;117:391-397.
34. Technician training tutorial: drug allergies. Pharm Lett/Prescr Lett. 2010;26:260601.
35. Thong BY, Leong K, Tang C, et al. Drug allergy in a general hospital. Ann Allergy Asthma Immunol. 2003;90:342-347.
36. Gavalas M, Sadana A, Metcalf S. Guidelines for the management of anaphylaxis in the emergency department. J Accid Emerg Med. 1998;15:96-98.
To comment on this article, contact rdavidson@uspharmacist.com.






