An estimated 500,000 people in the United States have herpes simplex virus (HSV) ocular disease.1 Each year about 50,000 new and recurring cases are diagnosed, with their treatment costing the nation approximately $17.7 million annually.1-4 Ocular HSV is considered the most common cause of infectious corneal blindness in the U.S.2
Many patients are often unsure as to whether or not to seek medical attention for an eye condition they experience as uncomfortable and distressing, but often consider unworthy of their doctor’s time and the expense of a consultation. Furthermore, ocular HSV is frequently misdiagnosed.5 In light of these issues, this article will address HSV keratitis and highlight the need to treat the condition and prevent recurrences, as well as the need for pharmacists to guide patients regarding these concerns. TABLE 1 provides details on signs and symptoms as well as treatment of the conditions discussed below.
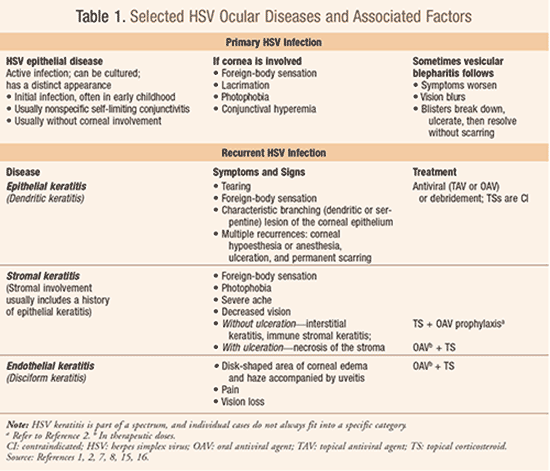
Ocular HSV can cause disease in any layer of the eye; most cases have been attributed to HSV-1.1,2 Common manifestations include follicular conjunctivitis, blepharitis, keratitis, and uveitis.2 HSV epithelial (dendritic) keratitis involves inflammation of the cornea with a characteristic dendritic (branched like a tree) ulceration. When the matrix or supporting tissue of the eye becomes involved, the condition is referred to as stromal keratitis; HSV stromal keratitis accounts for considerable visual morbidity, medical expense, and lost productivity among otherwise healthy individuals. Endothelial (disciform) keratitis is a deeper, disk-shaped area of secondary corneal edema and haze accompanied by anterior uveitis, causing pain and vision loss. A concern in the developed world is that a changing HSV seroprevalence may be contributing to a rising incidence of HSV keratitis, which may be in part counteracting the benefit of improved treatment.1
Ocular HSV Infection and Recurrence
HSV travels retrograde along the ophthalmic division of the fifth cranial nerve after ocular infection, or via other routes (e.g., oral route) after extraocular infection, to develop latency in trigeminal ganglia; it also may develop latency locally in the cornea.1 After an initial episode, the recurrence rate of ocular HSV is approximately 27% at 1 year, 50% at 5 years, and 63% at 20 years; risk increases with the number of recurrences.6 HSV keratitis is typically a recurrence of primary HSV ocular infection that was a nonspecific, self-limiting conjunctivitis.7 Often, follicular conjunctivitis is assumed to be pinkeye conjunctivitis. Pharmacists should note that typical conjunctivitis is caused by viruses such as adenovirus and is almost always bilateral, while HSV conjunctivitis is almost always unilateral.2 It has been recommended that if a patient presents with unilateral follicular conjunctivitis, a culture be performed to definitively rule out HSV.2
Recurrence and Risk of Vision Loss
The global incidence of HSV keratitis is roughly 1.5 million, including 40,000 new cases of severe monocular visual impairment or blindness, per year.1 HSV keratitis is believed to be an important cause of infectious blindness, with stromal opacification believed to be the main cause.1 Proven triggers for recurrence include ultraviolet (UV) light, fever, and refractive surgery.2
Clinical Presentation and Diagnosis
Symptoms of HSV keratitis include pain in and around the eye, redness, sensation of a foreign body in the eye, blurred vision, light sensitivity, and watery discharge.8 Characteristic signs include a dendritic corneal lesion (i.e., indicating dendritic keratitis) or disk-shaped, localized corneal edema and haze plus anterior uveitis (i.e., indicating endothelial, or disciform, keratitis).7 Diagnosis of HSV keratitis is confirmed by finding a dendritic ulcer via slit-lamp examination using fluorescein dye; if not conclusive, viral culture of the lesion can confirm the diagnosis.7,9,10
Preventing Recurrence of HSV Keratitis
While there are no proven methods for preventing HSV keratitis, there are steps that can be taken to assist in controlling its recurrences. Patients should be instructed to8,11
• Avoid touching the eyes or area around the eyes unless hands have been properly washed, particularly when a herpes infection (e.g., cold sore) is present.
• Refrain from using eye drops unless they have been prescribed or recommended by an ophthalmologist or other provider.
Habits, supplies, and techniques matter considerably when it comes to the health of the eyes while wearing contact lenses. Tips found in the Resource section can help pharmacists guide patients in the prevention of HSV recurrence by instructing those who wear contact lenses in the proper habits with regard to storage solution, cleaning technique, and replacement of lenses and storage cases.
Treatment
While there may be an increasing incidence of ocular HSV in the developed world, improved access to antiviral treatment may cause the overall visual burden of the disease to remain stable or decrease.1 The caveat, according to Farooq and Shukla, is that primary exposure to HSV is not easily prevented; thus, developing improved treatments and a vaccine to prevent HSV keratitis are important.1
Treatment of HSV keratitis requires antiviral therapy with topical or oral agents. Antiviral resistance appears to remain low in immunocompetent individuals, most likely because the immune system drives the virus into a latent state; resistance is much higher in the immunocompromised.12 Experts indicate that this factor should be considered as a cause of treatment failure, so that alternative treatments can be used, even though cross-resistance may also occur.13
Although most patients who have HSV keratitis are managed by an ophthalmologist, referral to one becomes obligatory if stromal or uveal involvement is present, owing to the necessity of more involved treatment.7 TABLE 1 indicates the type of agent used for selected diagnostic HSV categories. It is important to recognize that HSV keratitis is part of a spectrum, and an individual case may not fit into a specific category.2 Particular agents, including dosing recommendations and specific geriatric considerations, are discussed below. Medication changes are often necessary during a course of treatment, and close monitoring is required to maintain the delicate balance involved in clearing the virus, preventing reactivation, and controlling inflammation.2
Unless otherwise directed by a doctor, patients should not wear contact lenses while using medication. Debridement by gentle swabbing with a cotton-tipped applicator before beginning drug therapy may speed healing if the epithelium surrounding the dendrite is loose and edematous. If vision problems occur owing to scarring secondary to HSV keratitis, surgery may be considered, although it is rarely necessary.8
Topical antiviral therapy is usually effective and includes2,7,14,15
• Ganciclovir 0.15% gel applied every 3 hours while awake (5 times/day) until ulcer heals, then 3 times daily for 7 days, or
• Trifluridine 1% solution, 1 drop every 2 hours while awake (e.g., 9 times/day) until reepithelization, then 1 drop every 4 hours while awake, for 7 days.
The patient’s and caregiver’s ability to safely administer the correct dose of ophthalmic medication should be assessed, particularly in older adults.
Oral or IV antiviral therapy may be indicated2,7,14-16
• Acyclovir 400 mg orally 5 times/day (or 3 times/day for recurrent HSV keratitis) or
• Valacyclovir or famciclovir may simplify regimens
• Immunocompromised patients may require IV antivirals (e.g., acyclovir 5 mg/kg IV every 8 hours for 7 days).
In the geriatric patient, dosage adjustment may be necessary depending on creatinine clearance.14,15
In addition to antiviral agents, topical corticosteroids are used to control inflammation and minimize damage to the eye in cases of stromal involvement or uveitis.2,7 These agents are contraindicated when active viral replication is occurring on the ocular surface, as in acute epithelial keratitis (dendritic keratitis), but may be effective when used with an antiviral to manage later-stage stromal involvement (stromal keratitis) or uveitis.2,7
For example, prednisolone acetate 1% suspension or prednisolone sodium phosphate 1% is instilled every 2 hours initially (e.g., in the first 24-48 hours), then the interval is widened to every 4 to 8 hours as symptoms improve; many patients do not require a topical steroid more than four times a day to get stromal disease under control.2,7,14 A gradual taper to discontinuation is recommended.
Agents to relieve photophobia may be necessary, as is the case with uveitis: atropine 1% solution, 1-2 drops instilled 1 to 4 times daily with compression of the lacrimal sac for 2 to 3 minutes after drops are administered; or atropine 1% ointment applied in conjunctival sac 1 to 3 times daily. The peak (30 to 40 minutes) and duration (7 to 12 days) of mydriasis should be considered. Geriatric patients may not tolerate the anticholinergic effects of atropine and may be particularly at risk for cardiovascular and central nervous system adverse events.7,14
Conclusion
There are many challenges associated with HSV ocular disease, of which HSV keratitis causes considerable visual morbidity, medical expense, and loss of productivity. Understanding the role of recurrence prevention and appropriate treatment will assist pharmacists in caring for patients with this important cause of infectious blindness.
REFERENCES
1. Farooq AV, Shukla D. Herpes simplex epithelial and stromal keratitis: an epidemiologic update. Surv Ophthalmol. 2012;57:448-462.
2. Weiner G. Demystifying the ocular herpes simplex virus. American Academy of Ophthalmology. January 2013. www.aao.org/publications/eyenet/201301/feature.cfm. Accessed March 7, 2015.
3. Lairson DR, Begley CE, Reynolds TF, et al. Prevention of herpes simplex virus eye disease: a cost-effectiveness analysis. Arch Ophthalmol. 2003;121:108-112.
4. Liesegang TJ, Melton LJ, Daly PJ, et al. Epidemiology of ocular herpes simplex: incidence in Rochester, Minn, 1950 through 1982. Arch Ophthalmol. 1989;107:1155-1159.
5. National Institutes of Health. National Eye Institute. Facts about the cornea and corneal disease. Last reviewed May 2013. www.nei.nih.gov/health/cornealdisease/#k. Accessed March 6, 2015.
6. Young RC, Hodge DO, Liesegang TJ, Baratz KH. Arch Ophthalmol. 2010;128:1178-1183.
7. MerckManuals.com. Herpes simplex keratitis. October 2014. www.merckmanuals.com/professional/eye_disorders/corneal_disorders/herpes_simplex_keratitis.html. Accessed March 6, 2015.
8. Centers for Disease Control and Prevention. Basics of HSV (herpes simplex virus) keratitis. January 27, 2015. www.cdc.gov/contactlenses/viral-keratitis.html. Accessed March 6, 2015.
9. WebMD.com. Herpes and the eye. July 15, 2014. www.webmd.com/genital-herpes/guide/eye-herpes. Accessed March 18, 2015.
10. MedlinePlus Medical Encyclopedia. Fluorescein eye stain. March 16, 2015. www.nlm.nih.gov/medlineplus/ency/article/003845.htm. Accessed March 18, 2015.
11. Mayo Clinic. Diseases and conditions. Keratitis. September 20, 2012. www.mayoclinic.org/diseases-conditions/keratitis/basics/causes/con-20035288. Accessed March 25, 2015.
12. Bacon TH, Levin MJ, Leary JJ, et al. Herpes simplex virus resistance to acyclovir and penciclovir after two decades of antiviral therapy. Clin Microbiol Rev. 2003;16:114-128.
13. Morfin F, Thouvenot D. Herpes simplex virus resistance to antiviral drugs. J Clin Virol. 2003;26:29-37.
14. Epocrates Rx Pro. Version 15.2.1. Updated March 16, 2015.
15. Semla TP, Beizer JL, Higbee MD. Geriatric Dosage Handbook. 19th ed. Hudson, OH: Lexicomp; 2014.
16. Wang JC, Ritterband DC. Herpes simplex keratitis treatment and management. Medscape.com. Updated February 20, 2014. http://emedicine.medscape.com/article/1194268. Accessed March 30, 2015.
To comment on this article contact rdavidson@uspharmacist.com.






