US Pharm. 2021;46(2):14.
In 2017, according to the CDC, 11.5%, 9.5%, 7.4%, and 6.4% of white, black, Hispanic, and Asian adults, respectively, experienced heart attacks. Heart disease is the leading cause of death in the United States, and high total cholesterol is one of the four clinical risk factors for heart disease. The National Health and Nutrition Examination Survey (NHANES) reported that 44.9% of adults were treated for hypercholesterolemia from 2013 to 2016, and the Healthy People 2030 goal is to increase the number of patients receiving treatment in order to reduce the mean total-cholesterol level to 186.4 mg/dL.
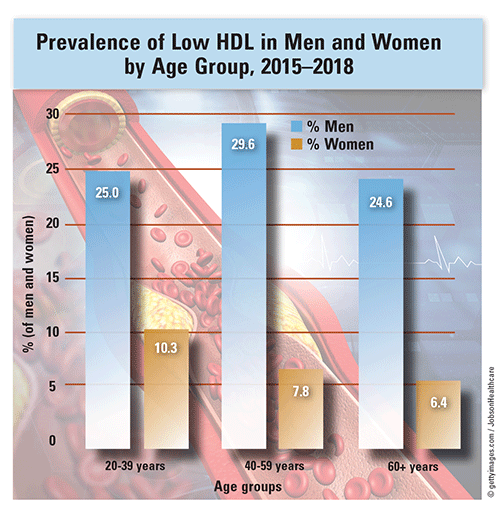
Prevalence: The prevalence of hypercholesterolemia increased 17.6% between the time periods 1999–2002 (25%) and 2013–2016 (29.4%). In the time period 2015–2016, the prevalence of hypercholesterolemia was 12.2%, after decreasing since 2010 at an average annual rate of 0.3%. During 2015–2016, 12.4% of adults had high total cholesterol and 18.4% had low HDL cholesterol. During 2013–2016, 11.8% of adults had high serum total-cholesterol levels, with a mean of 191 mg/dL.
Demographics: In the time period 2013–2016, 27.1% of adults had hypercholesterolemia, with a notably higher proportion of males (29.1%) than females (25.3%); the same trend was observed across all ethnic groups. Non-Hispanic white patients had the highest prevalence of hypercholesterolemia (28%), followed by Asian (25.7%), Hispanic (24.8%), and black patients (24.2%). The greatest discrepancy occurred among Hispanic patients, with 17.5% more males (26.8%) than females (22.8%) having hypercholesterolemia. For white patients, 14.9% more males (30%) than females (26.1%) had hypercholesterolemia; among Asian patients, the rate was 11.9% higher in males (27.3%) than in females (24.4%), and among black patients, 5.5% more males (25%) than females (23.7%) had hypercholesterolemia. Non-Hispanic white, Hispanic, non-Hispanic Asian, and non-Hispanic black adults were equally likely to have high cholesterol (12.6%, 11.2%, 10.7%, and 10.2%, respectively).
Diagnosis and Medication Use: Annually, 8.7 office visits per 100 persons were to a cardiologist. The primary diagnosis in 1.2% of visits was coronary atherosclerosis and other ischemic heart disease. Male patients outnumbered female patients by 9.1%. Of laboratory tests ordered during office visits, 12.2% were for lipids or cholesterol, and 10% more male (9.6%) than female patients (8.8%) were tested. Between the time periods 1998–1994 and 2007–2010, the use of cholesterol-lowering drugs increased 6.7-fold (1.6%-10.7%) in persons aged 18 to 64 years and 8-fold (5.9%-46.7%) in those aged 65 years and older, according to NHANES data. In 2016, during office visits for cardiovascular-disease treatment, an average of 5.1 prescriptions for cardiovascular drugs were written per visit, constituting three refills for every two new prescriptions.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





