US Pharm. 2020;45(11):24-30.
ABSTRACT: Hypoglycemia, which is a major barrier to the optimal management of diabetes, is associated with significant morbidity and mortality. Educating patients with diabetes about the prevention, early identification, and appropriate treatment of hypoglycemia is a critically important component of individualized diabetes care. Hypoglycemia prevention involves an understanding of the impact of diet, exercise, and medications on hypoglycemia risk. Treatment of hypoglycemia includes administration of oral carbohydrates for the patient who is conscious and administration of glucagon in the setting of severe hypoglycemia. Advances in glucose monitoring and the availability of newer glucagon formulations provide additional intervention options for the management of hypoglycemia.
Despite many recent therapeutic and technological advances, hypoglycemia remains a significant barrier to treatment intensification and the achievement of individualized glycemic goals in diabetes patients.1 The individualization of treatment goals for diabetes is critical for preventing overtreatment in clinically complex patients at risk for severe hypoglycemia.1,2 According to the CDC, 235,000 emergency-department visits for hypoglycemia were made in the United States in 2016.3 Recurrent severe hypoglycemia is associated with an increased risk of cardiovascular events and all-cause mortality.4 Accordingly, current recommendations published by organizations such as the American Diabetes Association (ADA), the American Association of Clinical Endocrinologists, and the American College of Endocrinology emphasize the importance of minimizing hypoglycemia risk when a patient-centered treatment plan is being developed.1,5 This article will provide a brief review of hypoglycemia classification and discuss approaches to the prevention and treatment of this condition in the ambulatory care setting.
CLASSIFICATION
The ADA categorizes hypoglycemia into three levels: Level 1 hypoglycemia is defined as a blood-glucose value between 54 mg/dL and 70 mg/dL; level 2 is a blood-glucose value less than 54 mg/dL; and level 3 denotes severe hypoglycemic events characterized by altered mental and/or physical status that require assistance for resolution.1 While this classification is useful in characterizing the severity of hypoglycemic events, any blood-glucose value below 70 mg/dL is considered clinically important.1 Therefore, from a practical standpoint, hypoglycemia may be broadly defined as any blood-glucose value below 70 mg/dL. The ADA recommends that, at each clinical encounter, patients with diabetes be asked about the occurrence of both symptomatic and asymptomatic hypoglycemia.1
SIGNS AND SYMPTOMS
The signs and symptoms of hypoglycemia vary depending on the severity of the event and can also differ between patients. Symptoms may be generally categorized as autonomic or neuroglycopenic.6 Autonomic symptoms comprise both adrenergic (catecholamine-mediated) symptoms and cholinergic (acetylcholine-mediated) symptoms. Examples of adrenergic symptoms include tremor, palpitations, tachycardia, and anxiety; some cholinergic symptoms are sweating, hunger, and paresthesias.6 The adrenergic symptoms of hypoglycemia may be masked in patients taking beta-adrenergic blockers, so patients using these agents should be counseled about how to recognize cholinergic and neuroglycopenic symptoms. Importantly, the blood-glucose threshold at which an individual patient will experience hypoglycemic symptoms depends on the degree of diabetes management. That is, the threshold for hypoglycemia will be higher in patients with consistently elevated blood-glucose levels; conversely the threshold tends to be lower in those who experience frequent hypoglycemia. Neuroglycopenic symptoms result from a lack of glucose in the central nervous system and may include dizziness, weakness, drowsiness, delirium, confusion, seizure, and (potentially) coma.6
TREATMENT-ASSOCIATED HYPOGLYCEMIA
A variety of factors have been associated with an increased risk of treatment-associated hypoglycemia, such as use of insulin and/or insulin secretagogues, impaired renal or hepatic function, older age, longer duration of diabetes, cognitive impairment, hypoglycemia unawareness, alcohol use, polypharmacy, and presence of a physical or intellectual disability that may impair the patient’s response to hypoglycemia.1 The ADA recommends that these factors be considered when individualized treatment goals are being developed. For diabetes patients who meet one or more of these criteria, individualized treatment plans should consider risks of treatment intensification versus potential benefits.
PREVENTION STRATEGIES
Educating patients about strategies for hypoglycemia prevention is an important aspect of diabetes care. The following sections discuss considerations for hypoglycemia prevention, including medication, diet and physical activity, use of glucose monitoring, and screening and management of hypoglycemia unawareness.
MEDICATION-RELATED CONSIDERATIONS
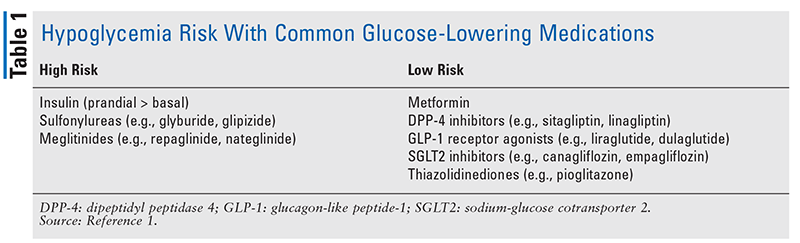
Patients whose diabetes is managed with insulin and/or insulin secretagogues (i.e., sulfonylureas and meglitinides) have the highest risk of experiencing hypoglycemia. TABLE 1 summarizes the associated hypoglycemia risk of common glucose-lowering medications.1,7 Although many classes of glucose-lowering medications are considered low-risk, it should be noted that the risk of hypoglycemia increases when these medications are added to background insulin and/or insulin secretagogues. If a patient is struggling with severe or recurrent hypoglycemia, it is important for the clinician to critically evaluate the appropriateness of the continued use of high-risk medications.1
Dietary Considerations
It is important for patients who are taking insulin and/or insulin secretagogues to understand that fasting or delaying meals can increase the risk of hypoglycemia. Patients should also be counseled that alcohol consumption can increase the risk of hypoglycemia, particularly if they use insulin and/or insulin secretagogues.8 Some key counseling points related to alcohol-associated hypoglycemia include the following1,8:
• Moderate consumption of alcohol is recommended (<1 drink per day for women, <2 drinks per day for men).
• Consume alcohol with food to reduce the risk of nocturnal hypoglycemia.
• Increase the frequency of glucose monitoring after drinking alcohol in order to identify and treat hypoglycemia early.
• Alcohol-induced hypoglycemia is often delayed and may present many hours after consumption of alcohol.
• Hypoglycemia symptoms or awareness may be lessened by the cerebral effects of alcohol.
Physical Activity
Although physical activity has many health benefits and should be encouraged in patients with diabetes, it can contribute to hypoglycemia in at-risk individuals; therefore, caution is warranted and individualized strategies for hypoglycemia prevention should be developed. The effect of exercise on glucose levels will vary depending on the timing of physical activity relative to meals and medication administration as well as the duration and intensity of physical activity. Although the approach to avoiding hypoglycemia with physical activity should be individualized, it has been suggested that a patient eat additional carbohydrates before exercise if pre-exercise blood glucose is lower than 90 mg/dL and that a patient using insulin should reduce the pre-exercise mealtime insulin dose and/or reduce the basal insulin dose during exercise.9
Glucose Monitoring
Monitoring via finger-stick glucose readings and a glucose meter or a continuous glucose monitor (CGM) is essential for the detection and avoidance of hypoglycemia.1 CGMs can be particularly useful for patients with intensive insulin regimens and in those with hypoglycemia unawareness. Patients at risk for hypoglycemia should be counseled to check their blood glucose before engaging in potentially dangerous activities (e.g., driving) in order to avoid accidents.
Hypoglycemia Unawareness
As noted previously, the threshold for experiencing hypoglycemia is often lower in patients who have frequent hypoglycemic events. If a patient has level 2 hypoglycemia (glucose <54 mg/dL) without experiencing hypoglycemia symptoms, he or she likely has hypoglycemia unawareness.1 Patients with hypoglycemia unawareness have diminished autonomic responses and deficient counterregulatory hormone responses to hypoglycemia.1 Hypoglycemia unawareness impairs patient safety, and its presence should trigger reevaluation of the medication regimen and current glycemic goals. The ADA also recommends that insulin-treated patients with hypoglycemia unawareness be advised to raise their glycemic target to strictly avoid hypoglycemia for at least several weeks in order to partially reverse hypoglycemia unawareness and reduce the risk of future episodes.1
TREATMENT
While implementation of strategies to prevent hypoglycemia is critical, diabetes patients at risk for hypoglycemia (e.g., those treated with insulin and/or insulin secretagogues) should be counseled about the appropriate treatment of hypoglycemia should it occur. Hypoglycemia treatment involves two main strategies: 1) administration of oral carbohydrates and 2) administration of glucagon in the setting of severe hypoglycemia.
Oral Glucose
When the blood-glucose level goes below 70 mg/dL, it is important that the patient treat the hypoglycemia immediately to avoid worsening of the event. The preferred treatment for hypoglycemia in conscious patients is glucose, but any readily available form of carbohydrate that contains glucose may be used.1 The Rule of 15 (TABLE 2) should be used to guide treatment.

The Rule of 15 both facilitates the appropriate resolution of hypoglycemia and prevents overtreatment of the hypoglycemic event in order to minimize rebound hyperglycemia. Carbohydrate sources high in protein should be avoided, as protein will delay carbohydrate absorption and resolution of hypoglycemia. It may be helpful to provide patients with examples of carbohydrate sources that contain approximately 15 grams of carbohydrate, such as glucose tablets or gel (carbohydrate content may vary), five or six Life Savers candies, 4 oz of juice or soda (regular, not diet), and 8 oz of skim milk.11
Glucagon for Hypoglycemic Emergencies
In situations where the patient is unconscious or otherwise unable to ingest oral carbohydrates, the administration of exogenous glucagon is indicated.1 The ADA recommends that patients at increased risk for level 2 hypoglycemia be given a prescription for glucagon.1 It is also recommended that all caregivers, family members, and (when applicable) school personnel know where the glucagon is stored and receive education on when and how to administer it. After administration, emergency medical services (EMS) should be contacted and the patient should be turned on his or her side to prevent choking and/or aspiration if vomiting occurs.12,13 Before EMS arrives, a second dose of glucagon may be administered if the hypoglycemic event has not resolved by 15 minutes following the initial administration of glucagon.12,13
Lyophilized glucagon has been available commercially for several decades. Traditional glucagon kits, however, can be difficult for nonmedical providers to prepare and appropriately administer because of difficulties surrounding glucagon reconstitution and/or injection.14,15
Newer Glucagon Formulations: The limitations of traditional lyophilized glucagon kits have led to the development of two new glucagon formulations that address barriers to use and appropriate administration. The following paragraphs give a brief overview of the Baqsimi and Gvoke glucagon products (see also TABLE 3).12,13
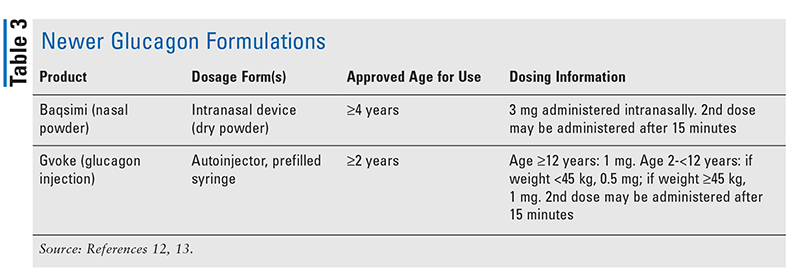
Baqsimi (glucagon nasal powder)—This product is a dry glucagon powder administered intranasally via a prefilled device.12 Baqsimi provides an alternative delivery option for caregivers or family members who are reluctant to administer glucagon via injection. Intranasal glucagon has been shown to be comparable to traditional glucagon emergency kits in terms of hypoglycemia resolution. While all glucagon formulations can lead to adverse effects such as nausea, vomiting, and headache, intranasal glucagon can also cause rhinorrhea, nasal congestion or discomfort, and epistaxis.12 Notably, in a study involving caregivers and untrained persons, participants were able to appropriately administer a full dose of intranasal glucagon more than 90% of the time versus 13% of the time for a traditional glucagon emergency kit.16 Additionally, the time required to prepare and administer a dose of glucagon was less than 30 seconds versus several minutes for the intranasal and the traditional product, respectively.
The Baqsimi nasal device comes in a yellow tube enclosed in shrink wrap.12 Prior to administration, the shrink wrap is removed and the tube is opened to retrieve the device. The device is gently inserted into one nostril, and the plunger is then firmly depressed all the way in to administer the full dose. Because this formulation is a nasal powder, it may be stored at temperatures up to 86°F; however, it should not be stored in moist or humid conditions, as moisture may render the drug ineffective.
Gvoke (glucagon injection)—This new glucagon solution, which is administered via injection, does not require reconstitution.13 It is available in both prefilled syringes and prefilled autoinjectors.13 Like Baqsimi, Gvoke has been shown to be comparable to traditional glucagon emergency kits in terms of efficacy and tolerability.16 In studies, Gvoke was demonstrated to have faster and increased rates of successful administration; compared with traditional glucagon emergency kits; this was attributed to the facts that Gvoke does not require reconstitution and is available as an autoinjector.16 This alternative injectable glucagon option may be simpler and quicker for nonmedical personnel to administer in the setting of a severe hypoglycemic event.
CONCLUSION
Hypoglycemia remains a significant barrier in the optimal management of diabetes. Pharmacists can play a critical role in educating diabetes patients about the prevention, recognition, and appropriate treatment of hypoglycemia in the ambulatory care setting. The widespread availability of CGM systems and newer, easier-to-use glucagon formulations provides opportunities for pharmacists to educate patients about these treatment options if they are struggling with recurrent hypoglycemic events.
REFERENCES
1. American Diabetes Association. Standards of Medical Care in Diabetes—2020. Diabetes Care. 2020;43(suppl 1):S1-S212.2. McCoy RG, Lipska KJ, Yao X, et al. Intensive treatment and severe hypoglycemia among adults with type 2 diabetes. JAMA Intern Med. 2016;176(7):969-978.
3. CDC. National Diabetes Statistics Report, 2020. Atlanta, GA: CDC; 2020.4. Agiostratidou G, Anhalt H, Ball D, et al. Standardizing clinically meaningful outcome measures beyond HbA1c for type 1 diabetes: a consensus report of the American Association of Clinical Endocrinologists, the American Association of Diabetes Educators, the American Diabetes Association, the Endocrine Society, JDRF International, The Leona M. and Harry B. Helmsley Charitable Trust, the Pediatric Endocrine Society, and the T1D Exchange. Diabetes Care. 2017;40(12):1622-1630.
5. Garber AJ, Handelsman Y, Grunberger G, et al. Consensus statement by the American Association of Clinical Endocrinologists and American College of Endocrinology on the comprehensive type 2 diabetes management algorithm—2020 Executive Summary. Endocr Pract. 2020;26(1):107-139.6. Cryer PE. Hypoglycemia in adults with diabetes mellitus. UpToDate. Waltham, MA: UpToDate; 2020.
7. Sircar M, Bhatia A, Munshi M. Review of hypoglycemia in the older adult: clinical implications and management. Can J Diabetes. 2016;40(1):66-72.8. Evert AB, Dennison M, Gardner CD, et al. Nutrition therapy for adults with diabetes or prediabetes: a consensus report. Diabetes Care. 2019;42(5):731-754.
9. Colberg SR, Sigal RJ, Yardley JE, et al. Physical activity/exercise and diabetes: a position statement of the American Diabetes Association. Diabetes Care. 2016;39(11):2065-2079.10. American Diabetes Association. Practical Insulin. 5th ed. Alexandria, VA: American Diabetes Association; 2019:43-47.
11. Hypoglycemia? Low blood glucose? Low blood sugar? Clin Diabetes. 2012;30(1):38.12. Baqsimi (glucagon) package insert. Indianapolis, IN: Eli Lilly and Co; July 2019.
13. Gvoke (glucagon) package insert. Chicago, IL: Xeris Pharmaceuticals, Inc; September 2019.14. Fendrick AM, He X, Liu D, et al. Glucagon prescriptions for diabetes patients after emergency department visits for hypoglycemia. Endocr Pract. 2018;24(10):861-866.
15. Haymond MW, Liu J, Bispham J, et al. Use of glucagon in patients with type 1 diabetes. Clin Diabetes. 2019;37(2):162-166.16. Thieu VT, Mitchell BD, Varnado OJ, Frier BM. Treatment and prevention of severe hypoglycaemia in people with diabetes: current and new formulations of glucagon. Diabetes Obes Metab. 2020;22(4):469-479.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





