US Pharm. 2011;36(9):HS4-HS7.
According to the Centers for Disease Control and Prevention (CDC), hysterectomy, the surgical removal of the uterus, is the second most frequent major surgical procedure among reproductive-age women.1 Whiteman et al reported that the incidence of hysterectomies performed in the United States was 600,000 yearly (2000-2004).2 Rates vary per age group, with the highest incidence in 45- to 60-year-olds (based on short-stay, nonfederal 1990-2007 discharge data).3 The incidence in all age groups has declined since 1990, likely due to new techniques such as endometrial ablation and uterine fibroid embolization, which are less invasive for conditions previously only treated by hysterectomy.4,5
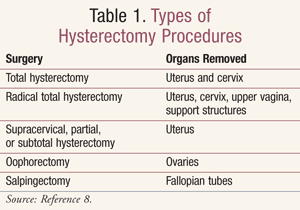
Although the incidence is declining, over a half million hysterectomies are still being performed in the U.S. annually,1 and pharmacists need to be informed so that they can educate patients and answer their questions. Knowing the different indications, the types of procedures (TABLE 1), the necessary pre- and postoperative care, and alternatives allows pharmacists to provide better care to female patients.
Since the evidence to support the use of hysterectomy in many disease states is limited, a woman and her physician should discuss alternatives, risks, and need, using as much information as possible. Issues to consider include the woman’s childbearing plans, functional impairment, response to medical treatment, and overall health condition, as well as alternatives to hysterectomy. Often there is not much evidence to support or detract from the choice of hysterectomy, so informed consent is important.
Indications for Hysterectomy
Hysterectomy may be performed to reduce or eradicate malignant or premalignant disease. Electively, the procedure can be used to remove benign lesions of the uterus, such as uterine fibroids or leiomyomas (fibroid tumors) or correct pelvic support problems (e.g., uterine prolapse). Abnormal or excessive uterine bleeding, chronic pelvic pain, or gynecologic infections (e.g., endometriosis, pelvic inflammatory disease) refractory to common medical therapies may also lead to hysterectomy. During urgent conditions such as uterine rupture, there may be no time to assess alternatives.6,7
Less extreme alternatives to hysterectomy exist for a variety of underlying disorders. For nonmalignant symptomatic leiomyoma, uterine artery embolization or myomectomy may be more appropriate. Nonsurgical therapies, such as pelvic floor exercises or a pessary (a medical device placed into the vagina to support the uterus), can be effective for some uterine or bladder prolapses. More extensive investigations into the causes for excessive uterine bleeding, endometrial hyperplasia, or pelvic pain, and then the use of targeted appropriate medical or ablative therapies, are often effective in preventing hysterectomy.7
Types and Anatomy of Hysterectomy
Total hysterectomy includes the removal of the uterus and cervix (TABLE 1). If additional structures are related to the symptoms or disease state, a radical total hysterectomy would also include removal of the upper vagina and the support structures. Removal of the ovaries is called oophorectomy, and of the fallopian tubes, salpingectomy. Supracervical, partial, or subtotal hysterectomy removes the uterine body above the cervix. Cytologic screening following a supracervical hysterectomy is still recommended. Patients who have had previous cervical malignancy should continue screening even after cervical removal.8,9 Patients who have had their cervix removed for a benign condition do not need to continue to have Pap smears.10 Long-term complications of supracervical hysterectomies include cyclical vaginal bleeding in 11% to 17% of women and the development of benign or neoplastic conditions that may require the future removal of the cervical stump.11
Methods of Hysterectomy
Depending on the patient, indications, and extent of surgery, there are various surgical methods that can be employed. These methods have been compared in the literature to determine safety and efficacy. Vaginal hysterectomy, where the uterus and other structures are removed via the vagina and no incisions are made through the abdomen, is recommended for benign conditions when possible and indicated. The recommendation is based on a shorter operating time, less anesthesia, shorter hospital stay, faster return to daily activities, and fewer complications than abdominal or laparoscopic techniques.7 Abdominal hysterectomy may be chosen for patients with large leiomyomas, previous surgical adhesions, or malignancy. A hysterectomy may be guided by laparoscope in which multiple small incisions are made in the abdomen and a camera is introduced into the cavity. The surgeon is able to remove the uterus and other organ structures via the abdominal incision or release structures from adhesions for removal through the vagina. Robotic assistance with laparoscopic surgery is a recent innovation to this technique.12,13
Perioperative Management
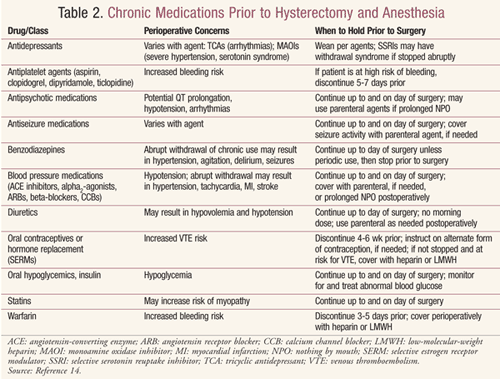
Counseling the patient prior to hysterectomy about home medications, including herbal and other dietary supplements, would be done as in any major surgical procedure. Chronic home medications often do not need to be discontinued prior to surgery. In some cases, this practice of discontinuance may cause harm that is unintended (TABLE 2).14 Many herbal dietary supplements should be held for 1 to 2 weeks prior to scheduled surgery to avoid increased bleeding risk or potential interactions with anesthetic agents.15
Unless there is extensive endometriosis or other potentially complicating structural abnormalities, no bowel preparation regimen is routine. The patient will be asked not to eat or drink for 12 hours or more prior to surgery to reduce aspiration risk. An antibiotic that will cover vaginal and skin organisms (e.g., first-generation cephalosporin [Cefazolin 1 g]) will be given just before surgery to reduce postoperative infection complications.16,17 Deep venous thrombosis (DVT) prophylaxis, either compression stockings, heparin, low-molecular-weight heparin (LMWH), or a combination of therapies, is recommended for moderate- to high-risk patients. Patients at increased risk include those who smoke, obese individuals, persons over 40 years of age, or those with a history of malignancy.18,19
Management of Postoperative Nausea and Vomiting
Postoperative nausea and vomiting (PONV) is a concern of many patients undergoing surgery. It is estimated that PONV occurs in more than 30% of surgeries and may be as high as 70% to 80% in certain high-risk populations that do not receive prophylaxis.20 Patient-related factors that increase the risk of PONV include female gender, nonsmoker, and history of PONV or motion sickness. The most well-established, surgery-related risk for PONV is the duration of surgery, with longer durations having a higher risk. Certain types of surgery are also considered possible risk factors. Intra-abdominal, laparoscopic, and major gynecologic surgeries are included among those that may increase the risk of PONV. Anesthesia-related risk factors include the use of general anesthesia with volatile anesthetics, nitrous oxide, or postoperative opioids.21-23
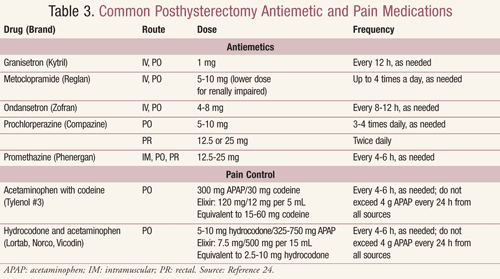
Women undergoing hysterectomy should be considered for prophylaxis of PONV (antiemetics are summarized in TABLE 3).24 A systematic review found that droperidol, metoclopramide, ondansetron, tropisetron, dolesetron, dexamethasone, cyclizine, and granisetron reliably prevented PONV and that no one drug was better than another. Drug efficacy was not affected by the patient’s age, the type of surgery, or the time the drug was given.22 While 5-hydroxytryptamine-3 (5-HT3) antagonists (e.g., granisetron, ondansetron) are effective choices, consideration should be given to side effects, drug interactions, and cost. Combination therapy is generally recommended for patients considered at moderate risk for PONV, while a multimodal approach (combination therapy with other pharmacologic and nonpharmacologic techniques) can be considered for those at high risk for PONV.20 If nausea or vomiting occurs despite prophylaxis, a rescue antiemetic from a different pharmacologic class should be used. If no prophylaxis was given, a 5-HT3 antagonist can be used.20
Pain After Hysterectomy
The type of hysterectomy performed may affect the amount of acute pain postoperatively. Patients undergoing laparoscopic hysterectomy have been shown to have lower pain scores and require less opiate use compared to patients undergoing abdominal hysterectomy.7 Laparoscopic hysterectomy also has lower pain scores on day 0 after surgery than vaginal hysterectomy. However, patients used more oral pain medications on postoperative day 0.7
While many health care providers focus on controlling the acute pain immediately after hysterectomy, it is important to be aware of the risk of chronic pain and be proactive in pain management (pain medications are summarized in Table 3).24 Brandsborg et al found that 60% to 100% of women reported pain prior to hysterectomy, and this pain is often a reason for the surgery to be performed.25 At 1 to 2 years after hysterectomy, pain prevalence varied from 4.7% to 31.9%, indicating that hysterectomy did provide pain control in many patients. However, pain as a new symptom or increased pain was reported in 1% to 14.9% and 2.9% to 5% of women, respectively. No differences in pain prevalence or frequency were noted between women who had abdominal hysterectomies and those who had vaginal hysterectomies.25 Risk factors for chronic pain include women with preoperative pelvic pain, previous cesarean delivery, pain as an indication for hysterectomy, pain problems elsewhere, preoperative depression, two or more pregnancies, and economic disadvantages.25,26
Chronic pain after hysterectomy can be due to abdominal/pelvic masses, endometriosis, spinal radiculopathy, or other pathology that is independent of the hysterectomy. Once these have been ruled out, a neuroma should be suspected when patients present with pain lasting more than 6 months that is not relieved with standard medical therapy. Neuromas can form when a peripheral nerve is damaged or becomes engulfed in scar tissue. Patients with neuromas after gynecologic surgery generally present with numbness at or below the incision site, pain and burning along the incision site, or referred pain in the pelvic region or groin with absence of gynecologic or other pathology (e.g., hernia).17,27
Postoperative Quality of Life and Sexual Function
Since most hysterectomies are performed for benign rather than life-threatening conditions, it is important to examine quality of life (QOL), including sexual function, after hysterectomy. Thakar et al conducted a prospective, randomized, double-blind study comparing total versus subtotal hysterectomy in 279 women undergoing hysterectomy for benign conditions.28 QOL was assessed using the Short-Form-36 (SF-36) before the hysterectomy and 6 and 12 months later. The SF-36 is a self-administered questionnaire that measures health in eight dimensions: health perception, mental health, energy, physical function, role limitations due to physical factors, role limitations due to emotional factors, social function, and pain. Nearly all subscales of the SF-36 were improved after hysterectomy. In addition, psychological outcomes were assessed using the General Health Questionnaire-28 (QHQ-28), which measures four elements of distress: depression, anxiety, social dysfunction, and somatic symptoms. All elements were improved in women after hysterectomy.28
Several studies examining sexual function after hysterectomy are conflicting. Previous, uncontrolled, retrospective studies suggested a decline in sexual libido after hysterectomy. However, later prospective studies report either an increase or no change in sexual desire.29 Similar findings have been reported for the frequency of intercourse after hysterectomy.29 Although overall sexual functioning is difficult to quantify, the more recent longitudinal studies suggest hysterectomy improves the sexual function of most women. There is, however, a subgroup of women (10%-25%) who may develop a sexual problem after hysterectomy.29 A systematic review of multiple posthysterectomy outcomes concluded that regardless of whether the cervix is removed, women undergoing hysterectomy generally experience improved QOL and sexual function.30
Conclusion
Patients awaiting surgical procedures often ask pharmacists about what can be expected before and after their operation. The pharmacist should be ready to answer questions about chronic medication management perioperatively, the potential outcomes, and the treatment of possible complications of gynecologic surgery. To best help our patients, the pharmacist should understand the use of antiemetics and pain control medications after hysterectomy. Most patients undergoing hysterectomy for benign conditions will experience relief of symptoms and a better QOL after surgery.
REFERENCES
1. Centers for Disease Control and Prevention. Women’s reproductive health: hysterectomy. Updated 2009. www.cdc.gov/
2. Whiteman MK, Hillis SD, Jamieson DJ, et al. Inpatient hysterectomy surveillance in the United States, 2000-2004. Am J Obstet Gynecol. 2008;198:34.e1-34.e7.
3. National Center for Health Statistics. Health, United States, 2010: With Special Feature on Death and Dying. Hyattsville, MD: National Center for Health Statistics; 2011:340-341. www.cdc.gov/nchs/data/hus/
4. Lethaby A, Hickey M, Garry R, Penninx J. Endometrial resection/ablation techniques for heavy menstrual bleeding. Cochrane Database Syst Rev. 2009;(4):CD001501.
5. Gupta JK, Sinha AS, Lumsden MA, Hickey M. Uterine artery embolization for symptomatic uterine fibroids. Cochrane Database Syst Rev. 2006;(1):CD005073.
6. American College of Obstetricians and Gynecologists. ACOG Committee opinion no. 444: choosing the route of hysterectomy for benign disease. Obstet Gynecol. 2009;114:1156-1158.
7. Nieboer TE, Johnson N, Lethaby A, et al. Surgical approach to hysterectomy for benign gynaecological disease. Cochrane Database Syst Rev. 2009;(3):CD003677.
8. Kives S, Lefebvre G, Wolfman W, et al. Supracervical hysterectomy. J Obstet Gynaecol Can. 2010;32:62-68.
9. ACOG Committee on Practice Bulletins–Gynecology. ACOG Practice Bulletin no. 109: cervical cytology screening. Obstet Gynecol. 2009;114:1409-1420.
10. Sirovich BE, Welch HG. Cervical cancer screening among women without a cervix. JAMA. 2004;291:2990-2993.
11. American College of Obstetricians and Gynecologists. ACOG Committee opinion no. 388, November 2007: supracervical hysterectomy. Obstet Gynecol. 2007;110:1215-1217.
12. Sarlos D, Kots L, Stevanovic N, Schaer G. Robotic hysterectomy versus conventional laparoscopic hysterectomy: outcome and cost analyses of a matched case-control study. Eur J Obstet Gynecol Reprod Biol. 2010;150:92-96.
13. Robotic-assisted laparoscopic surgery. Med Lett Drugs Ther. 2010;52:45-46.
14. Whinney C. Perioperative medication management: general principles and practical applications. Cleve Clin J Med. 2009;76(suppl 4):S126-S132.
15. Ang-Lee MK, Moss J, Yuan CS. Herbal medicines and perioperative care. JAMA. 2001;286:208-216.
16. Lazenby GB, Soper DE. Prevention, diagnosis, and treatment of gynecologic surgical site infections. Obstet Gynecol Clin North Am. 2010;37:379-386.
17. Stany MP, Farley JH. Complications of gynecologic surgery. Surg Clin North Am. 2008;88:343-359.
18. Geerts WH, Bergqvist D, Pineo GF, et al. Prevention of venous thromboembolism: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines (8th Edition). Chest. 2008;133(suppl 6):381S-453S.
19. ACOG Committee on Practice Bulletins–Gynecology. ACOG Practice Bulletin no. 84: prevention of deep vein thrombosis and pulmonary embolism. Obstet Gynecol. 2007;110:429-440.
20. Le TP, Gan TJ. Update on the management of postoperative nausea and vomiting and postdischarge nausea and vomiting in ambulatory surgery. Anesthesiol Clin. 2010;28:225-249.
21. Gan TJ. Risk factors for postoperative nausea and vomiting. Anesth Analg. 2006;102:1884-1898.
22. Carlisle JB, Stevenson CA. Drugs for preventing postoperative nausea and vomiting. Cochrane Database Syst Rev. 2006;(3):CD004125.
23. Ignoffo RJ. Current research on PONV/PDNV: practical implications for today’s pharmacist. Am J Health Syst Pharm. 2009;66(suppl 1):S19-S24.
24. Lacy CF, Armstrong LL, Goldman MP, eds. Lexi-Comp’s Drug Information Handbook 2010-11. 19th ed. Hudson, OH: Lexi-Comp, Inc; 2010.
25. Brandsborg B, Nikolajsen L, Kehlet H, Jensen TS. Chronic pain after hysterectomy. Acta Anaesthesiol Scand. 2008;52:327-331.
26. Brandsborg B, Nikolajsen L, Hansen CT, et al. Risk factors for chronic pain after hysterectomy: a nationwide questionnaire and database study. Anesthesiology. 2007;106:1003-1012.
27. Ducic I, Moxley M, Al-Attar A. Algorithm for treatment of postoperative incisional groin pain after cesarean delivery or hysterectomy. Obstet Gynecol. 2006;108:27-31.
28. Thakar R, Ayers S, Georgakapolou A, et al. Hysterectomy improves quality of life and decreases psychiatric symptoms: a prospective and randomised comparison of total versus subtotal hysterectomy. BJOG. 2004;111:1115-1120.
29. Flory N, Bissonnette F, Binik YM. Psychosocial effects of hysterectomy: literature review. J Psychosom Res. 2005;59:117-129.
30. Lethaby A, Ivanova V, Johnson NP. Total versus subtotal hysterectomy for benign gynaecological conditions. Cochrane Database Syst Rev. 2006;(2):CD004993.
To comment on this article, contact rdavidson@uspharmacist.com.





