US Pharm. 2013;38(4):38-43.
ABSTRACT: Many vaccines, particularly live vaccines, are labeled with warnings against use in patients who may have compromised immune function due to a medical condition or certain medications. However, there is uncertainty about which drugs cause a significant enough immunosuppressant effect that they could decrease vaccine efficacy or increase risks with vaccination. This article presents current literature on the use of influenza, pneumococcal, and herpes zoster vaccines in adults taking disease-modifying antirheumatic drugs (DMARDs) such as glucocorticoids, methotrexate, and biologics.
When considering vaccines for adults, a patient’s immune status is a critical component to both sides of the risk-benefit equation that pharmacists and patients weigh together when discussing treatment and prevention options. The immunosuppressed patient may be at an increased risk for vaccine-preventable diseases, negative consequences of vaccination with live vaccines, and reduced vaccine response.1 Pharmacists are uniquely positioned as adult immunizers who also understand the immunosuppressant effects of different drugs and medication regimens.
A great deal of what is known about vaccine efficacy is based on antibody titers or other surrogate immunologic markers instead of relevant clinical outcomes, like reduction and prevention of disease morbidity and mortality.2 The relatively short duration and frequent use of surrogate endpoints in vaccine studies limit the accuracy of projections that can be made. The outbreak of pertussis in the states of California in 2010 and Washington and many other states in 2012 predominantly among fully vaccinated children (with DTaP) demonstrate the shortcomings of some vaccine studies.3,4 Many of these vaccines have not been extensively studied in the immunosuppressed, who are generally at increased risk for infection.5 Nevertheless, recommendations can still be made to try to prevent vaccine-preventable diseases in these patients.
VACCINATE FIRST!
The most important and applicable consideration is whether an immunocompromised state can be anticipated. If it can be anticipated, it is best to vaccinate before inducing this state. For example, it would be advisable to provide vaccines to a person on an organ transplant waiting list or to someone being evaluated for chemotherapy or radiation therapy for cancer. There are at least three good reasons to consider vaccinating first:
1) There are ample data suggesting that patients with impaired immune systems demonstrate reduced vaccine response. If the immunosuppressed state can be anticipated, vaccinating first is the best opportunity for a positive immunologic response.2,5-7
2) The risk for certain types of invasive infections goes up significantly in the immunocompromised state5; vaccinating first may help reduce this risk.
3) Many live vaccines are contraindicated in immunosuppressed states because of both reduced immunologic response and the potential for contracting an infection from the vaccine.8,9
The family members and other direct contacts of the immunosuppressed person should also be considered. If any direct contacts of the soon-to-be immunosuppressed person are going to need live vaccines, recommend these before inducing the immunosuppressed state because live vaccines contain warnings against direct contact with immunosuppressed patients following vaccination.8
PATIENTS AT RISK
Patients Taking Glucocorticoids
The increased risk for infection with glucocorticoid use is significant and highly dose dependent. One study identified minimal thresholds for a daily dose and total exposure dose at which prednisone apparently increases the risk for infection.10 In the 71 clinical trials pooled together in this meta-analysis, when the total cumulative dose was <700 mg (21 of 71) or with daily doses <10 mg (5 of 71), there was no statistically significant increased risk for infection detected with prednisone compared to the control group. Sixteen out of 47 trials with prednisone doses exceeding these thresholds demonstrated an increased risk of infection in the prednisone group compared to the control group. The increased risk of infection was particularly high in patients with neurologic diseases (relative risk [RR] 2.8; 95% CI, 1.9-4.3; P <.001).10 When looking at the daily dose only, a glucocorticoid dose ≥20 mg/day (prednisone equivalents) is a universally recognized point at which the risk for infections increases.10,11
Likewise, a daily prednisone dose ≥20 mg is commonly considered the cutoff at which vaccine efficacy is substantially lost. Short durations of glucocorticoid therapy (<2 weeks) and lower doses (<10-20 mg/day of prednisone equivalents) do not usually contraindicate vaccination, even with live-virus vaccines. On the other hand, live vaccines may be ineffective (or even dangerous) and are contraindicated in patients on higher doses and longer durations of glucocorticoids.11 When a patient has been on high-dose prednisone at doses >10 to 20 mg per day for longer durations, there should be a waiting period of up to 3 months after discontinuation of higher-dose therapy before administering a live-virus vaccine.11 If a vaccine is administered during high-dose glucocorticoid use, patients should be considered unvaccinated and be revaccinated if and when they achieve immunocompetence.11
Patients Taking Disease-Modifying Antirheumatic Drugs (DMARDs)
Many patients with immune-mediated diseases, like rheumatoid arthritis, already have a baseline risk for infections independent of drug therapy.10 Most of the scientific literature aimed at determining the risk of infections with the antirheumatic drugs compares the various drugs against other drugs in this group, and not against placebo. Some of the more useful comparisons available are when drugs that may be immunosuppressive (e.g., methotrexate, leflunomide, tumor necrosis factor [TNF]-alpha inhibitors, and other biologics) are compared against agents unlikely to have immunosuppressive effects (e.g., anti-inflammatory drugs like sulfasalazine.)12
Methotrexate (MTX): This drug may increase infection risk and impair response to vaccines, especially at chemotherapy doses. There is also some concern in the medical community about the risk for varicella zoster (VZ) and herpes zoster (HZ) infections in patients on lower doses as used in immunologic conditions like rheumatoid arthritis. However, a recent analysis detailed three studies in particular that failed to discover a link between MTX use (vs. other DMARD therapy) and these infections.13
TNF-alpha Inhibitors: The TNF-alpha inhibitors (infliximab [Remicade], etanercept [Enbrel], adalimumab [Humira], golimumab [Simponi], certolizumab pegol [Cimzia]) contain numerous warnings in their prescribing information, medication guides, Web sites, and various advertisements regarding the risk of infections. A black box warning assigned to the labeling of all of these products contains multiple warnings about infection risk.14 Infliximab may be associated with the greatest risk for infection, as it has been associated with a statistically significant increase in serious infections (especially pneumonia and soft-tissue infections) compared to etanercept and adalimumab.15
It is less clear how TNF-alpha inhibitors affect immunization considerations. There is incomplete or conflicting information as to whether TNF-alpha therapy (or other DMARDs for that matter) poses an increased risk for infection with vaccine-preventable diseases and/or vaccine failure. When TNF-alpha antagonists, MTX, glucocorticoids, and other DMARDs are compared, only glucocorticoid use (baseline and initiation) stands out for association with a dose-dependent increase in serious infections and herpes zoster.15
IMMUNIZATIONS
The Influenza Vaccine
While prevention of influenza is critical in the immunosuppressed, there is evidence of diminished immunogenicity in these patients. General evidence-based, guideline-based, or simple common sense recommendations include:
1. Provide annual vaccination in patients on long-term immunosuppressant therapy.
2. If the current or upcoming year’s flu vaccine is available and the patient has not yet started immunosuppressant therapy, elect to vaccinate before initiating immunosuppressant therapy.
3. Since both a live (intranasal) and an inactivated (for injection) influenza vaccine is available, recommend only the inactivated vaccine in those already immunosuppressed.16
4. In patients receiving bone marrow or solid organ transplant (SOT), the flu vaccine is recommended after the first 6 months. Some clinicians and researchers hypothesize that giving a vaccine may increase the risk for transplant rejection in the first few months after therapy, but most do not agree. The primary reason for waiting 6 months is to maximize vaccine efficacy. Some evidence suggests that the first vaccination in bone marrow transplant recipients is unlikely to be effective. A small study had striking results: 0% had serologic response when vaccinated within 6 months of the transplant, and 13% had it within 7 to 24 months (but 64%-71% had vaccine response 2 years after the procedure).2
5. Because of the high morbidity and mortality in immunosuppressed patients, the use of an antiviral medication like oseltamivir is prudent during local outbreaks, especially after confirmed influenza exposures.2
It is not known whether the strategies addressed in the following questions might help increase the immunogenicity of influenza vaccination:
1. Would the high-dose flu vaccine (four times the antigen content), currently approved only for those over the age of 65 years, provide more efficacy than the standard vaccine in patients on potentially immunosuppressant drug therapy?
2. In the years when the vaccine composition (influenza strains) changes from the previous year’s or when an immunosuppressed patient has missed the previous year’s dose, should the patient receive two doses of flu vaccine prior to the next flu season?
Until these questions have been answered, it is best to continue with standard annual influenza vaccination in most patients.
Zoster Vaccine Live
The likelihood that an HZ vaccination will be effective in preventing infection in an at-risk individual decreases with increasing age. Contrariwise, since the occurrence of HZ and postherpetic neuralgia increases exponentially with increasing age,8 the importance of immunization actually increases greatly with age. The HZ vaccine is now FDA approved for adults aged 50 years and above; however, the Advisory Committee on Immunization Practices (ACIP) still only routinely recommends vaccination for adults aged 60 years and older.17 Several years ago, the ACIP cited vaccine supply as a major factor in not expanding the recommended age for HZ vaccination to 50 years and older; it is possible the recommendation may change, as vaccine is now readily available.18,19
As with the other vaccines discussed in this article, but particularly because the HZ vaccination is a live vaccine, its use should be considered before a planned immunosuppressed state. Because of this unique consideration (being a live vaccine), a large portion of this article has been devoted to it. However, it is important to not misinterpret this as a recommendation that the HZ vaccine is the most important vaccine in this population.
The live HZ vaccine (Zostavax) is considered contraindicated in patients receiving immunosuppressant medications. The HZ vaccine prescribing information (PI) warns against vaccinating immunosuppressed or immunodeficient patients due to the risk for disseminated disease.8 The PI specifically rules out various immunologic conditions that preclude use of the vaccine but warns only very broadly against use in patients on immuno-suppressive therapy. Specifics are likely absent because it is very challenging to clearly define “immunosuppressive therapy.”8
In the two drug-approval trials (Zostavax Efficacy and Safety Trial [ZEST] and Shingles Prevention Study [SPS]), subjects were monitored for injection-site reactions and non-injection-site zoster- or varicella-like rashes for 42 days postvaccination.8 These studies, as well as a recent cohort study, showed that adverse health outcomes in the first 42 days after vaccination resulting in HZ- or VZ-like rash, hospitalizations, or emergency room visits were very low and were not increased by the vaccine.8,18
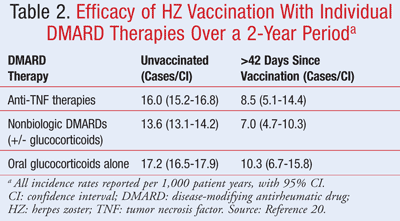
An article published in 2012 retrospectively looked at the association between HZ vaccination and the risk for HZ infection in older patients (≥60 years) with immune-mediated diseases.20 The authors analyzed both acute-onset HZ episodes after vaccination (for safety, possibly vaccine-induced) and HZ episodes over the long term for a median of 2 years (efficacy). The analysis included 463,541 Medicare beneficiaries with one of the following immune-mediated diseases: rheumatoid arthritis, psoriasis, psoriatic arthritis, ankylosing spondylitis, or inflammatory bowel disease. Medications included in this portion of the analysis included all immune-modulating biologic agents (anti-TNF and non-TNF biologics), MTX (>0.4 mg/kg/wk), and non-MTX, nonbiologic DMARDs. None of these mutually exclusive medication groups were associated with a statistically significant increased HZ risk in unvaccinated patients. On the other hand, the addition of a glucocorticoid (prednisone equivalents >20 mg/day) independently increased the incidence rate of HZ across these medication groups (1.2- to 2.0-fold). The pooled data on prednisone increasing HZ vaccination risk were statistically significant, and statistical significance was maintained on the smaller scale for most drugs when individually analyzed. But most important, across all of these groups it was shown to be beneficial and not risky to administer the HZ vaccine to prevent HZ in these patients (TABLES 1 and 2).20
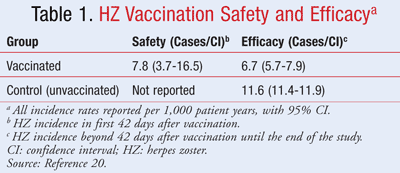
As indicated in the tables, the safety analysis identified only 7.8 cases per 1,000 patient-years in patients on DMARDS who received the HZ vaccination compared to rates of 11.6 cases per 1,000 patient-years in the unvaccinated group over the 2-year follow-up (the difference was not statistically significant).20 Furthermore, no cases of varicella or HZ occurred within 42 days in those exposed to biologics (95% CI, 0-4.7 per 1,000 biologics users; 0-5.4 per 1,000 specifically in the anti-TNF users). Among the only 633 (out of 7,780 vaccinated) patients exposed to biologic DMARDs (including 551 patients exposed to anti-TNF biologics) no cases of varicella or HZ were reported within 42 days following vaccination.12 As with a group of healthy patients at risk for HZ, there appears to be risk reduction long-term with vaccination similar to patients not on DMARD therapy. Vaccination against HZ conferred a statistically significant adjusted hazard ratio of 0.61 (95% CI, 0.52-0.71) overall for contracting HZ (or a slightly more modest 0.67 [95% CI, 0.59-0.75] if pharmacy claims data for HZ reporting were not included) during the “efficacy” follow-up period.
These data may warrant clarification in the PI about which therapies that should (or should not) be considered “immunosuppressive” and allow for greater patient inclusion for the vaccine; at the very least, a new prospective study is warranted. Authors of a recently published study that showed a lack of association between the initiation of anti-TNF therapy and the risk for HZ also believe that a trial to evaluate HZ vaccination among current anti-TNF users is warranted.21 Current data should be interpreted carefully, as this study only applies to patients on DMARDs. Also, this study was retrospective, not prospective, and therefore has some potential confounders. It is still unknown as to whether the risk for acute adverse reactions and reduced HZ vaccination immunogenicity may be greater in patients on other immunosuppressant drugs (e.g., organ transplant anti-rejection regimens) or with other immunologic or hematologic conditions (e.g., cancer patients).
Pneumonia Vaccine
Pneumococcal disease is one of the greatest concerns in the immunosuppressed, particularly in organ transplant recipients.1 There are now two vaccines available for prevention of pneumococcal disease in adults, the 23-valent pneumococcal polysaccharide vaccine (PPSV23) and the newly approved 13-valent pneumococcal conjugate vaccine (PCV13). In immunosuppressed patients, 50% of invasive pneumococcal diseases (IPDs) are caused by serotypes contained in PCV13; an additional 21% of serotypes causing IPD are contained in PPSV23. The PPSV23 vaccine is routinely recommended for adults over 65 years and high-risk adults aged 18 to 64 years. Most of the information for PPSV23 in immunosuppressed patients comes from use in HIV-infected patients, and data regarding efficacy are conflicting. The ACIP recommends the PCV13 and PPSV23 vaccines for the same indications in immunocompromised persons.22
A prospective study examined pneumococcal vaccine (PPSV23) response in patients on immunosuppressant drugs used for inflammatory bowel disease (Crohn’s disease and ulcerative colitis). The results are summarized in TABLE 3.7
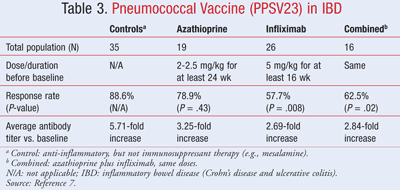
Drug information references state that pneumococcal vaccine should be given at least 2 weeks before an anticipated immunosuppressed state, including medications (organ transplant antirejection drugs, immunosuppressant therapy, or chemotherapy) or elective splenectomy.23 Low-dose prednisolone might not affect vaccine response (17.5 mg per week), but the supportive data are questionable.6
Other Vaccines to Consider
The pertussis (Tdap) and meningococcal vaccines warrant a brief discussion.
Tdap: To protect against tetanus, the tetanus-diphtheria (Td) vaccine should be administered at least every 10 years during adult life. Current recommendations for pertussis prevention state that a single dose of Tdap—instead of standard Td (diphtheria-pertussis)—should be administered during adult life. This is usually provided in the third decade of life, particularly to expecting parents. Recent concerns about the duration of protection of the acellular pertussis vaccine may prompt changes in the adult vaccine schedule.3,4 Until then, it is preferable to administer the Tdap vaccine to eligible adults soon (for next Td booster), especially if they are in direct contact with infants and children. Given the emerging poor efficacy data on the acellular version of this vaccine, as with other vaccines, it should be given before an immuno-suppressed state develops, if possible, to maximize the benefits this vaccine may provide.
Meningococcal Vaccine: The CDC’s Vaccine Information Statement for the meningococcal vaccine does not contain detailed information on whether there is increased risk of adverse reactions in immunosuppressed patients.24 This vaccine is routinely administered (2 doses) to adolescents between ages 11 and 18 years and is not a routine adult vaccine. Nevertheless, certain immunosuppressed patients have been identified at increased risk for meningococcal disease, and the following may be candidates for the vaccine24:
- "Anyone who has a damaged spleen, or whose spleen has been removed.
- Anyone who has persistent complement component deficiency (an immune system disorder).”
ROLE OF THE PHARMACIST
Pharmacists should try to help patients reduce long-term systemic glucocorticoid use as much as possible due to many detrimental adverse effects, in particular the dose-dependent increased risk of infection. Pharmacists are in an excellent position to identify patients eligible for adult vaccines, encourage their use, and, when applicable, prescribe and administer (or at least recommend) indicated vaccines. When possible, pharmacists should advise the administration of indicated vaccines prior to the induction of an immunosuppressed state. Pharmacists need cognizance of the important but imperfect disease prevention imparted by vaccines in healthy adults as well as the potentially diminished efficacy in those taking immunosuppressant medications, and should help foster healthy expectations of vaccine efficacy. Pharmacists should discuss the risk of infection with patients receiving immunosuppressant therapy and help monitor for signs and symptoms of infection.
REFERENCES
1. McAdam AJ, Sharpe AH. Infectious diseases: infections in immuno-suppressed hosts. In: Kumar K, Abbas A, Aster AC, Fausto N. Robbins and Cotran Pathologic Basis of Disease. 8th ed. Philadelphia, PA: Saunders Elsevier; 2009.
2. Kunisaki KM, Janoff EN. Influenza in immunosuppressed
populations: a review of infection frequency, morbidity, mortality, and
vaccine responses. Lancet Infect Dis. 2009;9:493-504.
3. Klein NP, Bartlett J, Rowhanie-Rahbar A, et al. Waning
protection after fifth dose of acellular pertussis vaccine in children. N Engl J Med. 2012;367:1012-1019.
4. CDC. Pertussis epidemic–Washington 2012. MMWR Morb Mortal Wkly Rep. 2012;61:517-522.
5. Dummer JS, Singh N. Infections in solid organ transplant recipients. In: Mandell GL, Bennett JE, Dolin R. Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases. 7th ed. Philadelphia, PA: Churchill Livingstone Elsevier; 2010:3839-3850.
6. Influence of methotrexate, TNF blockers and
prednisolone on antibody responses to pneumococcal polysaccharide
vaccine in patients with rheumatoid arthritis. Rheumatology. 2006;45:106-111.
7. Fiorino G, Peyrin-Biroulet L, Naccarato P, et al.
Effects of immunosuppression on immune response to pneumococcal vaccine
in inflammatory bowel disease: a prospective study. Inflamm Bowel Dis. 2012;18:1042-1047.
8. Zostavax (zoster vaccine live) package insert. Whitehouse Station, NJ: Merck & Co., Inc; 2011.
9. Vaccine information statement: typhoid vaccines. CDC.
May 29, 2012. www.cdc.gov/vaccines/pubs/vis/downloads/vis-typhoid.pdf.
Accessed October 31, 2012.
10. Stuck AE, Minder CE, Frey FJ. Risk of infectious complications in patients taking glucocorticosteroids. Rev Infect Dis. 1989;11:954-963.
11. Prednisone. Drugs. MD Consult [subscription required]. www.mdconsult.com. Accessed October 25, 2012.
12. Zhang N, Wilkinson S, Riaz M, et al. Does methotrexate
increase the risk of varicella or herpes zoster infection in patients
with rheumatoid arthritis? A systematic literature review. Clin Exp Rheumatol. 2012;30:962-971.
13. Remicade (infliximab) package insert. Horsham, PA: Janssen Biotech, Inc; 2011.
14. Grijalva CG, Kaltenbach L, Arbogast PG, et al.
Initiation of rheumatoid arthritis treatments and the risk of serious
infections. Rheumatology. 2012;49:82-90.
15. Grijalva CG, Chen L, Delzell E, et al. Initiation of
tumor necrosis factor-alpha antagonists and the risk of hospitalization
for infection in patients with autoimmune diseases. JAMA. 2011;306:2331-2339.
16. Vaccine information statement: influenza vaccine,
2012-13. CDC. July 2, 2012.
www.cdc.gov/vaccines/pubs/vis/downloads/vis-flu.pdf. Accessed October
31, 2012.
17. CDC. Update on herpes zoster vaccine: licensure for persons aged 50 through 59 years. MMWR Morb Mortal Wkly Rep. 2011;60:1528.
18. Baxter R, Tran TN, Hansen J. Safety of Zostavax—a cohort study in a managed care organization. Vaccine. 2012;30:6636-6641.
19. Merck vaccines: supply status. Merck & Co., Inc.
www.merckvaccines.com/Order-Vaccines/Pages/supply-status.aspx. Accessed
October 31, 2012.
20. Zhang J, Xie F, Delzell E. Association between
vaccination for herpes zoster and risk of herpes zoster infection among
older patients with selected immune-mediated diseases. JAMA. 2012;308:43-49.
21. Winthrop KL, Baddley JW, Chen L, et al. Association
between the initiation of anti-tumor necrosis factor therapy and risk of
herpes zoster. JAMA. 2013;309:887-895.
22. Use of 13-valent pneumococcal conjugate vaccine and
23-valent pneumococcal polysaccharide vaccine for adults with
immunocompromising conditions: recommendations of the Advisory Committee
on Immunization Practices (ACIP). MMWR Morb Mortal Wkly Rep. 2012;61:816-819.
23. Pneumococcal vaccine, polyvalent. Drugs. MD Consult [subscription required]. www.mdconsult.com. Accessed October 31, 2012.
24. Vaccine information statement: mennigococcal vaccine.
CDC. October 2011.
www.cdc.gov/vaccines/pubs/vis/downloads/vis-mening.pdf. Accessed October
31, 2012.
To comment on this article, contact rdavidson@uspharmacist.com.





