US Pharm. 2021;46(2):6-12.
ABSTRACT: Lipid-lowering medications have been shown to be efficacious, but adherence can be challenging in patients who are at risk for cardiovascular disease. It is critical for pharmacists to utilize tools in their practice to help patients attain better adherence outcomes, as nonadherence to evidence-based pharmacotherapy has been associated with excess morbidity and mortality. Pharmacists can work toward a better understanding of the factors affecting treatment adherence and interact compassionately with patients to determine the reasoning behind their actions. Furthermore, the pharmacist can identify the specific cause of nonadherence, address this with effective tools and resources in collaboration with the patient and physician, and distinguish nonadherence from drug-treatment ineffectiveness.
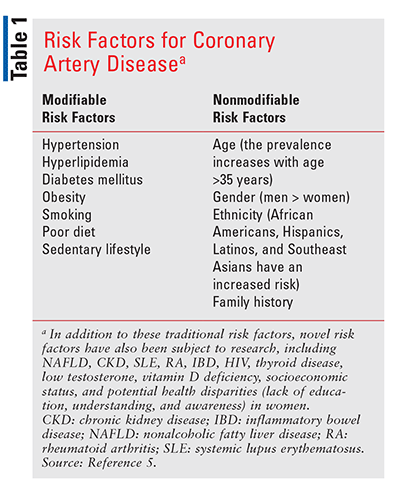
In the United States, heart disease is the leading cause of death in both men and women and in people of most racial and ethnic groups. Nonadherence to lipid-lowering medications, such as 3-hydroxy-3-methylglutaryl-coenzyme A reductase inhibitors (i.e., statins), plays a strong role in negative health outcomes in patients at risk for cardiovascular disease (CVD). Because the risk factors for coronary heart disease (TABLE 1) tend to be additive, nonadherence to medical treatment for any individual risk factor increases the level of risk. The reasons for lipid-lowering medication nonadherence are complex and may include patient, physician, and institutionalized factors. An understanding of the consequences of low adherence may spur the implementation of strategies to increase the appropriate use of statins. Systematic review has found that adherence to lipid-lowering medication improves after intensified patient care, and since pharmacists are readily accessible, they have a unique role in achieving this result. Intensified care includes drug-regimen simplification; patient education and information; patient follow-up with reminders via mail, telephone, and hand-held pill devices; complex behavioral approaches; group sessions; decision-support systems; administrative improvements; and large-scale pharmacy-led automated telephone sessions. Compared with standard care, these interventions have demonstrated significantly better adherence rates and a reduction in cholesterol levels in both the short and long term.1-5
Evidence-Based Literature on the Importance of Adherence
The importance of adherence to lipid-lowering medications in patients with dyslipidemia has been shown in a primary prevention study in which statins demonstrated a decrease in CVD morbidity and mortality.4 Patients in the treatment group with more than 75% adherence had fewer definite coronary events and lower CVD mortality. A dose-response effect was associated with better adherence, a result that argues for improving medication adherence to maximize therapeutic response. Similarly, a cohort study of patients with type 2 diabetes mellitus showed that higher refill adherence to lipid-lowering medications was associated with a lower risk of CVD in primary- and secondary-prevention patients.6 Not having medications on hand for more than 180 days was associated with a mortality risk 6% higher in primary-prevention patients and 18% higher in secondary-prevention patients, which points out another area that the pharmacist is uniquely well positioned to help improve. Furthermore, interventions conducted exclusively by pharmacists or implemented by pharmacists collaborating with physicians or nurses further support pharmacists’ key role in intervention.7,8 These interventions include patient education and counseling about medications, lifestyle, or compliance; reminder systems; measurement of CVD risk factors; medication management (medical record review or adjustment or changes in medications); feedback to physicians; and education of healthcare professionals. All interventions were associated with significant reductions in total cholesterol (nine studies including 1,121 patients; –17.4 mg/L [95% CI, –25.5 to –9.2]) and LDL cholesterol (LDL-C) (seven studies including 924 patients; –13.4 mg/L [95% CI, –23.0 to –3.8]). In order to implement these changes effectively in a pharmacy setting, pharmacists need to better understand the factors involved in, and barriers to, adherence to lipid-lowering medications.5-8
Factors Affecting Treatment Adherence
As compassionate healthcare professionals, pharmacists have a duty to understand the factors affecting treatment adherence, as this will equip them with a much better plan of action and help them avoid patient judgment. There are numerous patient-related factors not specific to the type of treatment that may affect adherence to treatment regimens.
Preconceived Notions and Motivation for Treatment: Younger patients with premature atherosclerotic CVD may believe that this is a disease of the elderly, and they may lack the necessary understanding of their disease progression to attain optimal statin adherence. This can be a challenging situation to deal with, as feeling pressured by others and feeling conflicted about change have been associated with nonadherence. Finding ways to motivate patients to embrace a commitment to positive self-related outcomes can help them sustain adherence. It is extremely important for pharmacists to be mindful of how to converse with their patients so as not to provoke fear of what may happen if they are not adherent to medication, which tends to promote initial, but not sustained, adherence.2,3,7,9
Functional Illiteracy and Effective Communication With Clinicians: Functional health illiteracy is common in some patient groups, perhaps more than is realized. In one study, 41% of patients aged 60 years and older did not understand the label instruction “Take on an empty stomach.”10 Even more alarmingly, 50% of their spouses and 25% of their children were unaware of this difficulty. The National Assessment of Adult Literacy, which provided the first measure of U.S. health literacy, found that 14% of American adults function at the below-basic level, 22% function at the basic level, 53% have an intermediate level of health literacy, and 12% have proficient health literacy.11 Interpreting medication labels requires intermediate skill. This means that 36% of adult Americans have levels of health literacy below what is required to understand typical medication information. Improved adherence often ensues when clinicians use plain terms to communicate with patients, provide precise information about the effects of treatment and potential side effects, and collaborate on a treatment plan that incorporates the patient’s values, motivations, and difficulties with treatment.10,11
Lack of Clinical Follow-Up: A lack of clinical follow-up can adversely affect patient adherence and treatment outcomes. These factors can be substantially improved by means of a case-management approach that utilizes follow-up phone calls or emails to assist the patient with adherence problems.2,3,7,9
Regimen Complexity and Past Medication Fills: Pharmacists are likely well aware that complex regimens involving medications taken at different times are associated with poor adherence. This was shown in a cohort study in which nonadherence to statins and ACE inhibitors or angiotensin receptor blockers increased with the complexity of the treatment regimen and prescription filling, as measured by the number of prescribed medications, prescribers, pharmacies, pharmacy visits, and pharmacy visits per prescription fill.12,13
Nearly one-half of new users of statins are adherent to their statin therapy in the first year of treatment initiation. A systematic review found that new statin use and factors such as age, sex, race, socioeconomic status, side effects, and comorbidities are potential reasons for nonadherence.12 Previous research indicating baseline adherence to chronic medications was a relatively strong predictor of future adherence to newly initiated statins. There is value in using records of past medication fills to identify new statin users who are likely to be nonadherent in the first year of treatment initiation. This is important to be aware of, as time and resources are limited in the pharmacy setting. The use of patient-assistance tools such as medication therapy management (to simplify regimens) or charts and pill organizers can improve adherence, as can the involvement of family members or caregivers.12
Side Effects and Possible Medication Intolerance: Although statins are first-line LDL-C–lowering medications for primary and secondary prevention of CVD, patients often report adverse effects (e.g., muscle symptoms). Pharmacists can exclude other causes of side effects and interactions and share information on long-term risk reduction and safety with patients. Additionally, there are ways to resolve these symptoms (e.g., statin holiday, switching, initiating lower dose, or combining other lipid-lowering agents).7,9
Cost and Lifestyle Barriers: One barrier for many patients is the cost of the medication. Additionally, the inconvenience of changing a daily routine to incorporate medications or the demands of maintaining a medication schedule while traveling may affect adherence. A study found that obtaining statins through a mail-order pharmacy rather than a local pharmacy was associated with improved control of LDL-C.14
Cognitive Impairment and Psychopathology: Patients, especially elderly ones, tend to have memory or concentration problems. Others may lack the capacity to understand the impact of treatment versus no treatment, and this deficit may be relatively subtle following an event such as stroke or myocardial infarction. Moreover, clinical depression, which is not uncommon in cardiac patients over the course of disease, influences a patient’s inclination to make and sustain changes, increases hopelessness, and promotes the attitude that treatment does not matter.9,10,15,16
Adherence-Enhancing Strategies Pharmacists Can Use in Practice
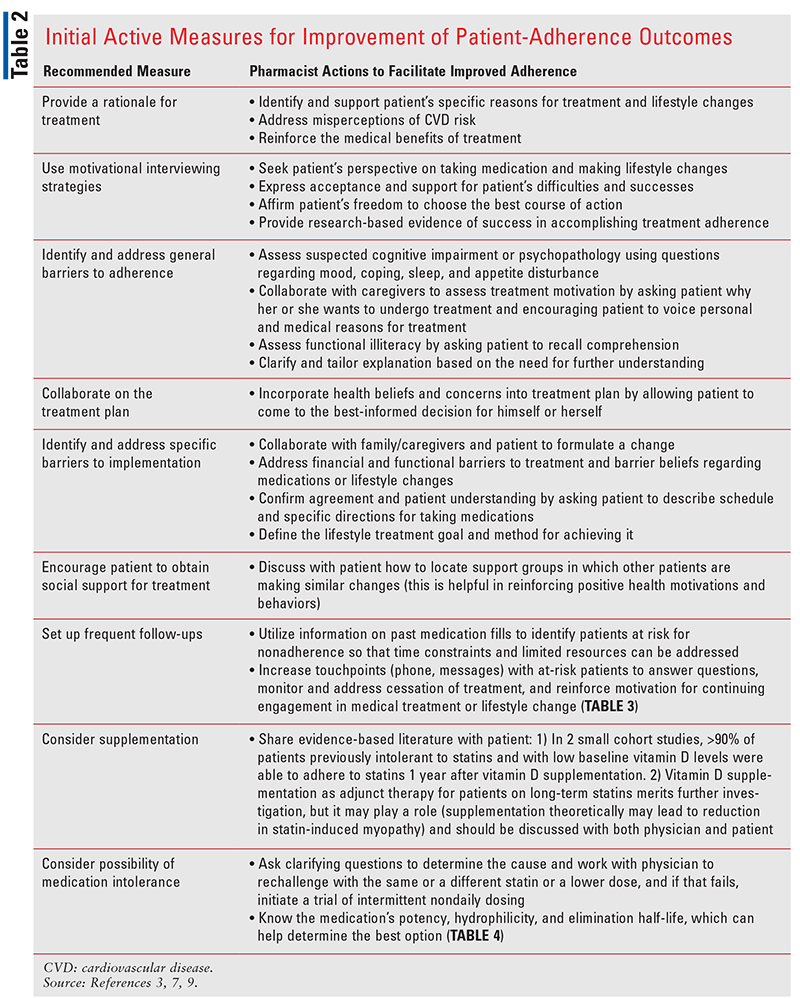
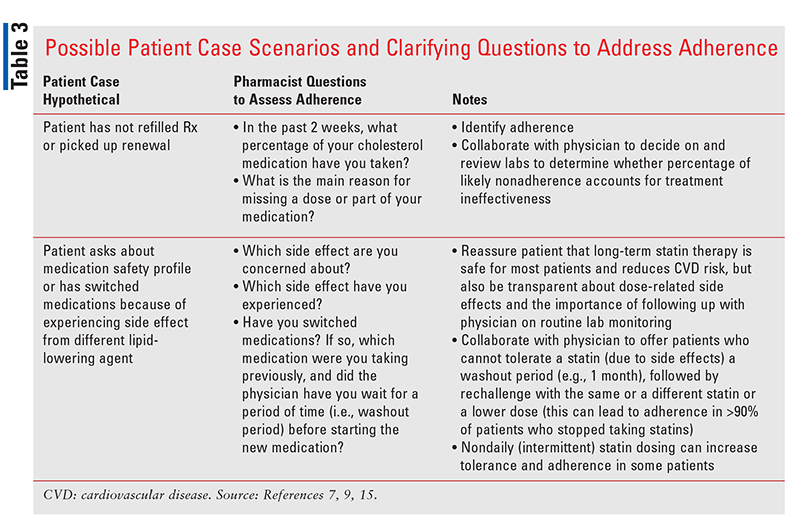
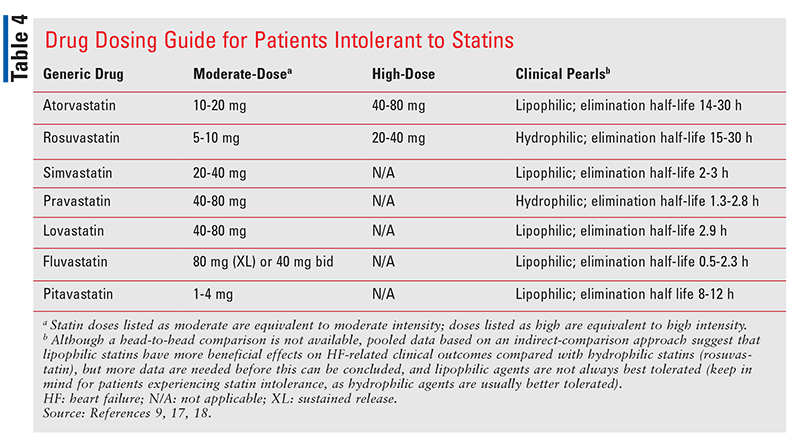
The American Heart Association Expert Panel on Compliance has reviewed existing adherence-enhancing strategies found to be effective in clinical research and has made recommendations including patient education, contracts, self-monitoring, tailoring interventions to individual needs, telephone follow-ups, and social support, all of which are tools that pharmacists can use to help improve patients’ treatment adherence (TABLE 2 and TABLE 3). Although the 2020 Veterans Affairs and Department of Defense guidelines on the management of dyslipidemia for CVD risk reduction emphasize that regular measurement of lipid levels is not required to monitor therapy effects, there are many reasons that a provider may wish to obtain these values.9 Knowing the LDL-C level may provide the pharmacist with objective data, facilitate shared decision making, and identify medication nonadherence or the possibility of intolerance (TABLE 4). This can help the provider both motivate the patient to follow the treatment regimen and individualize therapy for patients who are at high risk despite statin use. The pharmacist can also easily assess adherence indirectly via patient report and medication-refill frequency. Additionally, pharmacists can incorporate knowledge of patient-specific factors into regular patient visits (TABLE 2).2,7,9,14,15
Conclusion
Medication adherence is multifactorial and can be complex; therefore, a comprehensive and multidisciplinary approach to understanding the root cause behind patient nonadherence is critical, and pharmacist involvement is essential for optimization. To this end, the pharmacist may employ tools such as continuous check-ins, counseling, and medication therapy management with patients in their practice. Communicating effectively, offering empathetic and nonjudgmental understanding, and being willing to work with a nonadherent patient may improve future adherence or adherence with other caregivers. It is important to facilitate discussions that are sensitive to patients’ beliefs and differences. Additionally, the pharmacist should keep in mind that progress may be slow and meaningful change often takes time. Ultimately, pharmacist-delivered interventions may lead to improved patient adherence to lipid-lowering medications and positive outcomes.
REFERENCES
1. CDC WONDER [online database]. Underlying cause of death 1999-2018. https://wonder.cdc.gov/wonder/help/ucd.html. Accessed October 17, 2020.
2. Grundy SM, Stone NJ, Bailey AL, et al. 2018 AHA/ACC/AACVPR/AAPA/ABC/ACPM/ADA/AGS/APhA/ASPC/NLA/PCNA guideline on the management of blood cholesterol: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Circulation. 2019;139:e1082-e1183.
3. van Driel ML, Morledge MD, Ulep R, et al. Interventions to improve adherence to lipid-lowering medication. Cochrane Database Syst Rev. 2016;(12):CD004371.
4. Shepherd J. The West of Scotland Coronary Prevention Study (WOSCOPS): benefits of pravastatin therapy in compliant subjects. Circulation. 1996;94(suppl):1.
5. Brown JC, Gerhardt TE. Risk factors for coronary artery disease. www.statpearls.com/ArticleLibrary/viewarticle/28614. Accessed January 20, 2021.
6. Karlsson SA, Hero C, Svensson AM, et al. Association between refill adherence to lipid-lowering medications and the risk of cardiovascular disease and mortality in Swedish patients with type 2 diabetes mellitus: a nationwide cohort study. BMJ Open. 2018;8:e020309.
7. Reston JT, Buelt A, Donahue MP, et al. Interventions to improve statin tolerance and adherence in patients at risk for cardiovascular disease: a systematic review for the 2020 U.S. Department of Veterans Affairs and U.S. Department of Defense Guidelines for Management of Dyslipidemia. Ann Intern Med. 2020;173:806-812.
8. Santschi V, Chiolero A, Burnand B, et al. Impact of pharmacist care in the management of cardiovascular disease risk factors: a systematic review and meta-analysis of randomized trials. Arch Intern Med. 2011;171:1441-1453.
9. O’Malley PG, Arnold MJ, Kelley C, et al. Management of dyslipidemia for cardiovascular disease risk reduction: synopsis of the 2020 updated U.S. Department of Veterans Affairs and U.S. Department of Defense clinical practice guideline. Ann Intern Med. 2020;173:822-829.
10. Williams MV, Parker RM, Baker DW, et al. Inadequate functional health literacy among patients at two public hospitals. JAMA. 1995;274:1677-1682.
11. Agency for Healthcare Research and Quality. Strategies to improve communication between pharmacy staff and patients: training program for pharmacy staff. www.ahrq.gov/health-literacy/improve/pharmacy/guide/train2.html. Accessed November 10, 2020.
12. Yala SM, Duru OK, Ettner SL, et al. Patterns of prescription drug expenditures and medication adherence among Medicare Part D beneficiaries with and without the low-income supplement. BMC Health Serv Res. 2014;14:665.
13. Majd Z. Using medication fill records to help predict nonadherence of statins in new users. www.managedhealthcareconnect.com/content/using-medication-fill-records-help-predict-nonadherence-statins-new-users. Accessed November 10, 2020.
14. Schmittdiel JA, Karter AJ, Dyer W, et al. The comparative effectiveness of mail order pharmacy use vs. local pharmacy use on LDL-C control in new statin users. J Gen Intern Med. 2011;26:1396-1402.
15. Bailey AL, Campbell CL. The U.S. Department of Veterans Affairs and U.S. Department of Defense guideline for the management of dyslipidemia: is moderate risk reduction enough? Ann Intern Med. 2020;173:846-847.
16. Barnason S, White-Williams C, Rossi LP, et al. Evidence for therapeutic patient education interventions to promote cardiovascular patient self-management: a scientific statement for healthcare professionals from the American Heart Association. Circ Cardiovasc Qual Outcomes. 2017;10:e000025.
17. Bonsu KO, Reidpath DD, Kadirvelu A. Lipophilic statin versus rosuvastatin (hydrophilic) treatment for heart failure: a meta-analysis and adjusted indirect comparison of randomized trials. Cardiovasc Drugs Ther. 2016;30:177-188.
18. Imran T, Wong A, Schneeweiss S, Desai RJ. Statin lipophilicity and the risk of incident heart failure. Cardiology. 2020;145:375-383.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





