US Pharm. 2022;47(8):18-20.
ABSTRACT: Type 1 diabetes mellitus (T1DM), an autoimmune disease that causes insulin deficiency, accounts for about 80% of new DM diagnoses in patients aged 19 years and younger. The most common cause of elevated ketones in pediatric patients with DM is insulin deficiency. Elevated ketones can be a precursor to diabetic ketoacidosis (DKA), a medical emergency that is more common in T1DM than in type 2 DM. DKA treatment includes the ABCs for general resuscitation, fluid resuscitation, electrolyte replacement, and insulin infusion. Pharmacists in any practice setting can play a vital role in helping prevent future episodes of DKA in pediatric patients.
Type 1 diabetes mellitus (T1DM) is an autoimmune disease that destroys the pancreatic beta cells, which produce insulin. T1DM often presents in childhood, but it can be diagnosed at any age.1 T1DM accounts for approximately 80% of new DM diagnoses in patients aged 19 years and younger in the United States. The exact etiology of T1DM remains unknown.2,3
T1DM Pathophysiology
Insulin is an anabolic hormone that helps glucose enter adipose and muscle cells, stimulates the liver to store glucose as glycogen and synthesize fatty acids, enables the uptake of amino acids, inhibits fat breakdown in adipose tissue, and triggers potassium uptake into cells. Lifelong insulin replacement therapy is necessary in T1DM patients.4 Pediatric patients with T1DM typically present in a hyperglycemic state with polydipsia, polyuria, and polyphagia.4
Ketones
The primary fuel source in humans is glucose. Ketones are chemicals made by the liver that build up when the body starts to burn fat for energy instead of glucose. The body switches to this source only if no glucose is provided by the diet or if glucose is unable to enter the cells because of insulin deficiency. There are three types of ketones: beta-hydroxybutyrate (BHB), acetoacetate, and acetone.5,6
The most common cause of elevated ketones in pediatric patients with DM is insulin deficiency, which can be caused by medication nonadherence, insulin-pump failure, or illness. Without sufficient insulin, glucose builds up in the bloodstream and cannot enter the cells; the cells then burn fat instead of glucose. Elevated ketones can alert DM patients or their caregivers to a serious medical emergency known as diabetic ketoacidosis (DKA).7 Although pediatric patients with type 2 DM (T2DM) can develop DKA, this condition is more common in T1DM.8 DKA occurs when the body has an inadequate amount of insulin. Without enough insulin, the glucagon level increases, causing the adipose tissue to release free fatty acids and the muscle cells to release amino acids. Ketone bodies are produced by the liver and are utilized by the brain, skeletal muscle, and cardiac tissue as a fuel source when the body cannot use glucose effectively.9
When to Test Ketones
The medical team will advise the patient or caregiver regarding when testing is appropriate. Ketone monitoring is recommended if the blood glucose (i.e., blood sugar) is >250 mg/dL for 2 days in a row, if the patient has been sick or injured, if the patient wants to exercise and the blood sugar is >250 mg/dL, or if the patient is pregnant.10
Ketone monitoring is also recommended if a pediatric patient is experiencing signs or symptoms of DKA. These include dehydration, tachycardia, tachypnea, Kussmaul respiration with a smell of ketones in the breath, nausea, vomiting, abdominal pain, confusion, drowsiness, and reduced consciousness.8
Ketones can be tested via urine or blood samples. The normal range for blood ketones is <0.6 mmol/L. The presence of slightly high (0.6-1.0 mmol/L) blood ketone levels could mean that ketones have started to build up in the body. The most common reason for this in pediatric patients is a missed insulin injection, which should be taken as soon as possible. It is recommended that ketones be rechecked in a few hours. The presence of moderate-to-high (1.0-3.0 mmol/L) or very high (>3.0 mmol/L) ketone levels could signal DKA, and the patient or caregiver should call the healthcare provider (HCP) or go to the emergency department immediately.10
In urine ketone testing, the color of the dipped ketone strip is compared against a diagram on the product container. Possible results include no ketones; trace amounts of ketones; moderate amounts of ketones; and large amounts of ketones. Urine ketone levels may correlate with the level of ketones in the blood. For instance, urine showing 1+ ketones correlates to low-to-moderate blood ketone levels, whereas a result of 3+ (+++) urine ketones signifies severe blood ketone levels.9 It is suggested that urine ketones be tested when the blood sugar concentration is >250 mg/dL, and the presence of moderate-to-large ketones could indicate DKA.10,11 Blood ketone testing is a better representation of a patient’s current status, as there is a delay with urine ketone testing. Methods for lowering ketone levels include drinking extra water to flush ketones out of body, testing the blood sugar every 3 to 4 hours, and (for the combination of high blood sugar and high ketones) limiting exercise.10,11 Blood and urine ketone test kits are available for purchase OTC.
DKA Diagnosis
Diagnostic criteria for DKA include elevated blood glucose >200 mg/dL with a venous pH <7.3 and/or bicarbonate (HCO3) level <15 mmol/L. DKA may be accompanied by ketonemia, ketonuria, blood BHB >3 mmol/L, and a moderate level of urine ketones.8,9 Accurate diagnosis of DKA is necessary to rule out other potential causes, including pneumonia, meningitis, dehydration, and other conditions.8,9 TABLE 1 lists risk factors for patients with DKA.8,9
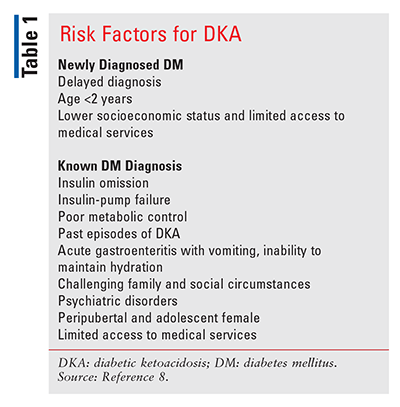
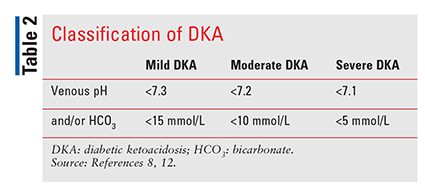
DKA is usually managed in any hospital unit or in a pediatric inpatient unit. A pediatric ICU is necessary for patients younger than age 2 years and for severe cases of DKA. During the evaluation, a thorough medical history is helpful, and a physical examination should be performed.8,9 Assessment should include the severity of dehydration, level of consciousness according to the Glasgow Coma Scale, and height and body weight, if the patient is mobile. Additional measurements include blood glucose concentration, blood BHB (not universally available for diagnosis), serum electrolytes, and renal function.8,9 The severity of DKA is categorized by the degree of acidosis; see TABLE 2 for a summary of DKA classification.8,12
DKA Treatment
Treatment for DKA involves the “ABCs” for general resuscitation and fluid resuscitation, including securing the airway with 100% oxygen, breathing, and circulation.9 It is necessary to obtain the patient’s body weight in order to make accurate calculations for various medications and fluids. Fluid therapy is initiated to restore circulating volume, replace electrolytes, and assist in clearing ketones and glucose from the blood, and the usual dosage is 0.9% normal saline and 10 mL/kg to 20 mL/kg normal saline bolus for 1 to 2 hours.8 Fluid therapy is typically planned for 48 hours but is adjusted based on clinical status. No more than 1.5 to 2 times the normal daily limit for fluid therapy should be infused. If hypokalemia is present, potassium should be replaced before insulin therapy is initiated; otherwise, potassium replacement may begin with insulin therapy. Potassium replacement should be deferred if hyperkalemia is present and until urine output is evident. Short-acting or regular insulin is administered via IV insulin infusion, with 0.06 unit/kg/hour to 0.1 unit/kg/hour initiated 1 to 2 hours after starting fluid-replacement therapy, until the pH is <7.30, HCO3 is <15 mmol/L, and BHB is <1 mmol/L.8
In treating DKA in pediatric patients, bolus dosing of insulin should be avoided because it could worsen hypokalemia or cause cerebral edema.9 Once a patient’s acidosis is improved and a diet can be implemented, the insulin may be switched to subcutaneous injections.9 Bicarbonate therapy is not usually included in DKA management, and it may cause paradoxical central nervous system acidosis.8 The cause of DKA should be discussed with the patient and caregiver, if possible, with the goal of preventing subsequent episodes.8 The patient or caregiver should work closely with the healthcare team to adjust the treatment regimen and provide necessary follow-up.
Complications Associated With DKA and Its Treatment
In the U.S., there is a reported 0.15% mortality risk with each occurrence of DKA.12 Complications include renal failure, hypokalemia, hypophosphatemia, peripheral venous thrombosis, rhabdomyolysis, acute pancreatitis, sepsis, mucormycosis, and hypoglycemia.8,9,12 Cerebral edema, a major cause of death in pediatric patients with DKA, occurs in 0.5% to 0.9% of cases.8 Risk factors for cerebral edema include being newly diagnosed and aged younger than 5 years, rapid rehydration, insulin received before or within the first hour of fluid initiation, high blood urea, hypernatremia, and pH <7.1.8 IV mannitol 0.5 g/kg to 1 g/kg over 10 to 15 minutes should be administered to treat cerebral edema, and the dose should be repeated if no response occurs in 30 minutes to 2 hours.8 An alternative to mannitol is hypertonic 3% saline 2.5 mL/kg to 5 mL/kg over 10 to 15 minutes.8 Survivors of cerebral edema are likely to have neurologic morbidities.9
The Pharmacist’s Role
Pharmacists are known to be one of the most accessible healthcare professionals and therefore have opportunities to educate patients and caregivers. Regardless of the practice setting, pharmacist participation and intervention can make an impact on patients with diabetes. Inpatient pharmacists can recognize patients at high risk for readmission and provide appropriate education. Opportunities can be identified during the transitions-of-care process. For instance, pharmacists can inform patients or caregivers who cannot afford insulin about manufacturer-based resources for reducing costs, such as copay cards, vouchers, and patient-assistance programs. Ambulatory-care and community pharmacists can identify patients at risk because of nonadherence or insulin-pump failures and can help patients navigate prescription plans. Community pharmacies can stock ketone testing supplies to increase patient access and can counsel on their use.
Patients and caregivers should receive thorough education on the DM disease process and management. Pharmacists can encourage adequate hydration, more frequent blood-sugar monitoring, alertness to the signs and symptoms of DKA, and the development of a sick-day plan in consultation with the HCP.13 Interested pharmacists can seek additional training to become a certified diabetes care and education specialist (i.e., CDCES), which will enhance their expertise in providing education on DM. In any practice setting, pharmacists can play a vital role in the care of pediatric patients with DM.
Conclusion
T1DM accounts for approximately 80% of new DM diagnoses in patients aged 19 years and younger in the U.S. DKA, a serious condition, occurs more often in T1DM patients than in those with T2DM. To reduce episodes of DKA, pediatric patients or their caregivers should be thoroughly educated on DKA and on sick-day management, including when to monitor ketones and when to seek medical attention. If DKA occurs, it should be appropriately managed in order to minimize potential complications.
REFERENCES
1. Levitsky LL, Misra M. Epidemiology, presentation, and diagnosis of type 1 diabetes mellitus in children and adolescents. UpToDate. Waltham, MA: UpToDate Inc; 2021. www.uptodate.com/contents/epidemiology-presentation-and-diagnosis-of-type-1-diabetes-mellitus-in-children-and-adolescents. Accessed May 12, 2022.
2. Mayer-Davis EJ, Lawrence JM, Dabelea D, et al. Incidence trends of type 1 and type 2 diabetes among youths, 2002-2012. N Engl J Med. 2017;376(15):1419-1429.
3. Lawrence JM, Divers J, Isom S, et al. Trends in prevalence of type 1 and type 2 diabetes in children and adolescents in the US, 2001-2017. JAMA. 2021;326(8):717-727.
4. Lucier J, Weinstock RS. Diabetes Mellitus Type 1. Treasure Island, FL: StatPearls Publishing; 2022 Jan-.
5. Laffel L. Ketone bodies: a review of physiology, pathophysiology and application of monitoring to diabetes. Diabetes Metab Res Rev. 1999;15(6):412-426.
6. Biology Dictionary. Ketone bodies. https://biologydictionary.net/ketone-bodies/. Accessed May 20, 2022.
7. CDC. Diabetic ketoacidosis. www.cdc.gov/diabetes/basics/diabetic-ketoacidosis.html. Accessed May 20, 2022.
8. Raghupathy P. Diabetic ketoacidosis in children and adolescents. Indian J Endocrinol Metab. 2015;19(suppl 1):S55-S57.
9. El-Mohandes N, Yee G, Huecker MR. Pediatric Diabetic Ketoacidosis. Treasure Island, FL: StatPearls Publishing; 2022 Jan-.
10. American Diabetes Association. Diabetes & DKA (ketoacidosis). www.diabetes.org/diabetes/dka-ketoacidosis-ketones. Accessed May 20, 2022.
11. Association of Diabetes Care & Education Specialists. Diabetes-related ketoacidosis. www.diabeteseducator.org/docs/default-source/education-and-career/dka_ketoacidosis.pdf. Accessed May 25, 2022.
12. Rosenbloom AL. The management of diabetic ketoacidosis in children. Diabetes Ther. 2010;1(2):103-120.
13. American Diabetes Association. Planning for sick days. www.diabetes.org/diabetes/treatment-care/planning-sick-days. Accessed May 30, 2022.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.






