US Pharm. 2015;40(10):52-56.
ABSTRACT: Eating disorders are less likely to be diagnosed in men than in women. Male eating disorders are not limited to a specific age group or subset of the population, although certain groups may be at greater risk. To date, the most commonly studied demographics include adolescent males, undergraduate college-age males, and athletes. Other subsets of the population requiring additional study include homosexual males and men aged older than their 20s. Treatment of patients with eating disorders includes both behavioral and pharmacologic options. Currently, the most studied medications include antidepressants and antipsychotics. More research is required to accurately diagnose and treat eating disorders in the male population.
A substantial amount of research has been completed addressing eating disorders in females, but relatively small amounts in males. Although the incidence of eating disorders is not as high in men as in women, studies suggest ratios as high as 1:4 in the general population and 1:2 in athletes.1
Since the early 2000s, researchers have placed a greater focus on the assessment of eating disorders in males, particularly adolescents.2,3 Findings from these studies have elucidated a greater prevalence of disordered eating behavior in males than previously thought. It has also been shown that male athletes are at a greater risk for disordered eating behavior than males who are not athletes; specifically, those who participate in sports where weight goals (e.g., wrestling) are of significant importance.2 Among heterosexual men, body fat dissatisfaction was found to be an important aspect of male body image, and may be uniquely related to psychological distress compared to muscle dissatisfaction.3 To date, no studies have examined the potential increased risk of eating disorders among homosexual athletes.
According to a recently published study in the Journal of the American Medical Association (JAMA), body dissatisfaction does not motivate adolescents to adopt healthy habits, but instead is associated with unhealthy eating behaviors.4 A response to the article urged a greater focus on eating disorders in the homosexual male population, stating that “men who have sex with men often have perceptions of body type that differ substantially from heterosexual males.”5 Homosexual men are more likely than heterosexuals to address their physique dissatisfaction through restrictive dieting, rather than by engaging in compulsive exercise.6
Diagnostic Criteria
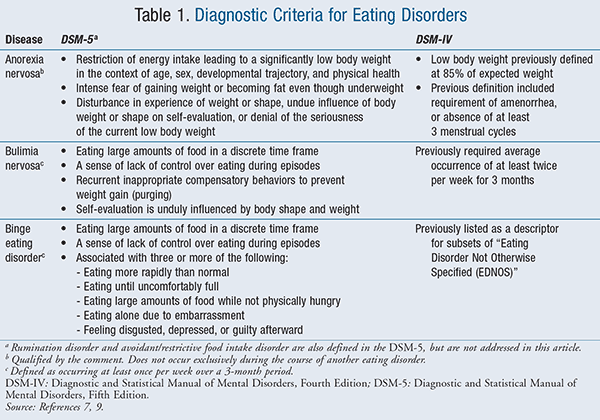
The Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition (DSM-IV) outlined three types of eating disorders—anorexia nervosa (AN), bulimia nervosa (BN), and binge eating disorder (BED).7 In 1996, the American Psychiatric Association (APA) published its Diagnostic and Statistical Manual of Mental Disorders: Primary Care Version, Fourth Edition (DSM-IV-PC), which accounted for disordered eating behaviors not previously outlined in the DSM-IV.8 This included dieting and body image behaviors and binge-purge eating behaviors. These additions to the description of disordered eating behaviors outlined a continuum of behaviors, rather than distinctive illnesses. The Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5), published in 2013, further clarified this potential spectrum by outlining more disordered eating behaviors than previously published.9 These additions include pica, rumination disorder, avoidant/restrictive food intake disorder, other specified feeding or eating disorder, and unspecified feeding or eating disorder. Description of DSM-5 diagnostic criteria, with comparison to DSM-IV criteria, are outlined in TABLE 1.9
Eating Disorders in Adolescent Males
In a 2006 review by Muise et al pertaining to adolescent and young adult males, it was estimated that 5% to 15% of cases of AN and BN and 40% of cases of BED occur in boys and men.10 Traditionally, the prevalence of AN in males as compared to females was thought to be 10:1, but when utilizing the diagnosis of a partial syndrome (as newly outlined in the DSM-5 ) prevalence increased to 2:1. Significant variance is noted throughout the literature due to many complications with diagnosis. This includes a lack of screening by primary care providers, lack of reporting by patients because of fear or social stigma, and a lack of diagnostic criteria for males that are traditionally used in females.
Previously, the diagnostic criteria for AN included the requirement of amenorrhea (absence of three menstrual cycles).8 This criterion has been removed in the DSM-5 due to inability to apply to prepubescent women, men, and postmenopausal women. Criteria reviewed in screening should include body mass index (BMI), height, weight, upper arm circumference, and skinfold thickness of the triceps and subscapula.10 Males with BN are noted to have higher rates of comorbid psychiatric disorders, particularly substance abuse, than females. Subclinical disordered eating is a widespread problem in the adolescent population, and it leads many researchers to suggest the development of eating disorders on a spectrum, rather than using a list of finite diagnoses.10
Many males also have behaviors geared toward increasing muscle size or tone, rather than weight loss. Additionally, homosexual male adolescents are more than three times as likely as heterosexual males to report unhealthy weight-control behaviors, such as attempting to lose weight through fasting, taking diet pills or powders without a physician’s advice, vomiting, or using laxatives.11 This leads to behaviors that vary significantly from the typical AN, BN, or BED symptoms, and include risks such as using protein powders, creatine, or steroids.12
Eating Disorders in Male Athletes
Adolescents feel pressure from their peers as well as the media to have the perfect body. This pressure can be rooted very early as boys play with GI Joes and other action figures that have become unrealistically muscular.13 Since the 1980s, the United States has seen an increase in large, lean, muscular male models presented in ever more revealing stages of undress.12 On top of intensifying media focus, males who participate in sports receive added body image pressure. If an athlete does not fit the ideal body form for a given sport, he is at an increased risk for body image dissatisfaction.13 A study on muscle dysmorphia in male weight lifters referred to this as “reverse anorexia nervosa” because the goal for large muscles in males shares many similarities with the drive to be thin in females.13
Athletes must possess certain characteristics, such as determination, perfectionism, obsessive behavior, and competitive drive, to be successful in sports. Unfortunately, these are also the same factors that increase the risk of developing disordered eating behaviors.1 For this reason, it is important for coaches to take responsibility and pay close attention to weight fluctuations and unhealthy eating habits, so that issues can be caught early and further complications prevented. According to Goltz et al, there is a tendency for athletes to underreport their symptoms to protect either their athletic department or themselves or possibly as a result of denial.1
Eating Disorders in Homosexual Males
One subset of the male population that requires attention specifically in regard to diagnosis is homosexual males. Heterosexual males and females with prior same-sex partners, homosexual males, and bisexual females were all more likely to misperceive themselves as being overweight relative to their same-sex, exclusively heterosexual peers.11 Due to the constant perception of being overweight, homosexual men are more likely than heterosexual men to experience poor body image and related eating disorder symptomatology.6 In addition to perceiving themselves as overweight, homosexual men have significantly lighter perceived ideal body weights and have higher body fat dissatisfaction than their heterosexual counterparts.3,6,14 Homosexual men were also found to have a higher likelihood of eating disorders with or without the presence of body dysmorphic disorder.3,6,11,14,15 This type of body dissatisfaction is not only predictive of the potential for eating disorders, but also increases the risk of psychological distress, lower self-esteem, and worsening depression.15
Recently, there has been increased research focused on the impact of body image on eating disorders and subsequent high-risk behavior in homosexual males.2,11,14 One area overlooked in all this new information is the lack of data on homosexual men after their early-to-mid 20s. Currently, there are only two easily accessible studies on homosexual men with eating disorders and exercise patterns whose average age is >30 years.
It has been noted that a man’s preferred body image is muscular, as this is seen as a sign of health by society as a whole.1 Within the homosexual community, muscularity may be a significant signal of health, which may be especially important as the community deals with the impact of the HIV/AIDS epidemic.15 This propensity for increased muscularity comes as a revelation, as initially homosexual males were thought to desire being thinner, much like females.3 Contrary to preconceived notions, homosexual men are at particular risk for body dissatisfaction, and the nature of that dissatisfaction for most appears to be concerns about muscularity rather than thinness.15
Steroid Use
Individuals who experience body image dissatisfaction are at higher risk for using anabolic-androgenic steroids in an attempt to increase muscle mass and strength. Such individuals are also at a greater risk of low self-esteem.16 It has also been found that males who have experienced muscle dysmorphia have higher rates of mood and anxiety disorders as compared to those who have not.17
Project EAT (Eating Among Teens) was an analysis of approximately 500 high school–aged teenagers that aimed to explore the prevalence of steroid use among adolescent males and females for the purpose of gaining muscle.2 The study found several correlations related to steroid use in adolescents, including higher risks for suicide attempts, illicit drug use, binge eating, and eating disorder diagnosis.2 Additionally, researchers found that steroid use is more likely in adolescents who participate in a sport where specific weight requirements affect class or performance and in those whose parents are concerned about weight or body image. Over the 5-year follow-up, Project EAT found that steroid use decreased in adolescent boys and girls as they aged; that the peak age of use was in middle school (7th and 8th grade); and that use declined significantly in high school (9th through 12th grade).18
Treatment Options
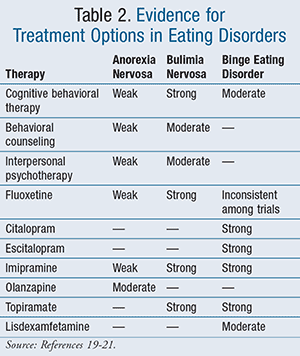
Approach to treatment varies based on the type of disorder. Treatment information is outlined in TABLE 2.19-21 AN patients derive the most benefit from psychosocial therapy alone.19,22 Pharmacologic options for patients with AN include both antipsychotics and antidepressants. When examining the antipsychotics, olanzapine appears to have the best supporting evidence for helping patients to gain weight. The use of antidepressants in AN, in particular the selective serotonin reuptake inhibitors (SSRIs), tended not to provide significant weight gain. Combination therapy consisting of both psychosocial therapy and antidepressants did not yield significantly better results than psychosocial therapy alone.19,22
Patients with BN also responded well to cognitive behavioral therapy (CBT).19,22 Pharmacologic treatment of patients with BN includes tricyclic antidepressants (TCAs), SSRIs such as fluoxetine, and anticonvulsants such as topiramate. Currently, treatment of patients with BN using a combination of medications and CBT is ongoing, with previous studies indicating little to no improvement over CBT alone.19,22
For patients with BED, formerly known as eating disorder not otherwise specified (EDNOS), CBT has demonstrated positive outcomes.19,22 Pharmacologic options for BED now include a new indication for lisdexamfetamine (Vyvanse), making it the first drug FDA-approved to treat this specific condition.21 Other treatment options include antidepressants (citalopram, escitalopram, imipramine, sertraline) and the anticonvulsant topiramate.19,22 Previous studies looking at CBT combined with drug therapy did not yield a significant effect on a reduction in binge-eating days per week when compared with medication alone.19,22 Since publication of the APA guidelines, lisdexamfetamine has demonstrated a reduction in binge-eating days per week; however, no studies have been found comparing lisdexamfetamine to CBT.21
Conclusion
The incidence of eating disorders in the male population, though less than in women, is likely higher than reported. The disease often presents differently in men than in women. Certain groups, such as adolescents, homosexual males, and athletes are at a greater risk of developing an eating disorder. These at-risk populations would benefit from early detection and increased screening. Additional research is needed to better understand disordered eating behaviors in men and to help healthcare providers develop more appropriate treatment plans.
REFERENCES
1. Goltz FR, Stenzel LM, Schneider CD. Disordered eating behaviors and body image in male athletes. Rev Bras Psiquiatr. 2013;35(3):237-242.
2. Irving LM, Wall M, Neumark-Sztainer D, Story M. Steroid use among adolescents: findings from Project EAT. J Adolesc Health. 2002;30(4):243-252.
3. Blashill AJ. Elements of male body image: prediction of depression, eating pathology and social sensitivity among gay men. Body Image. 2010;7(4):310-316.
4. Neumark-Sztainer D, Eisenberg ME. Body image concerns, muscle-enhancing behaviors, and eating disorders in males. JAMA. 2014;312(20):2156-2157.
5. Nguyen GT, Margo KL. Male body image and weight-related disorders [letter to the editor]. JAMA. 2015;313(8):856.
6. Kaminski PL, Chapman BP, Haynes SD, Own L. Body image, eating behaviors, and attitudes toward exercise among gay and straight men. Eat Behav. 2005;6(3):179-187.
7. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition (DSM-IV). Washington, DC: American Psychiatric Association; 1994.
8. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders: Primary Care Version, Fourth Edition (DSM-IV-PC). Washington, DC: American Psychiatric Association; 1996.
9. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5). Arlington, VA: American Psychiatric Press; 2013.
10. Muise AM, Stein DG, Arbess G. Eating disorders in adolescent boys: a review of the adolescent and young adult literature. J Adolesc Health. 2003;33(6):427-435.
11. Hadland SE, Austin SB, Goodenow CS, Calzo JP. Weight misperception and unhealthy weight control behaviors among sexual minorities in the general adolescent population. J Adolesc Health. 2014;54(3):296-303.
12. Eisenberg ME, Wall M, Neumark-Sztainer D. Muscle-enhancing behaviors among adolescent girls and boys. Pediatrics. 2012;130(6):1019-1026.
13. Olivardia R, Pope HG Jr, Hudson JI. Muscle dysmorphia in male weightlifters: a case-control study. Am J Psychiatry. 2000;157(8):1291-1296.
14. Mor Z, Parfionov K, Davidovitch N, Grotto I. Gym exercising patterns, lifestyle and high-risk sexual behaviour in men who have sex with men and in heterosexual men. BMJ Open. 2014;4(11):e005205.
15. Levesque MJ, Vichesky DR. Raising the bar on the body beautiful: an analysis of the body image concerns of homosexual men. Body Image. 2006;3(1):45-55.
16. Cafri G, Thompson JK, Ricciardelli L, et al. Pursuit of the muscular ideal: physical and psychological consequences and putative risk factors. Clin Psychol Rev. 2005;25(2):215-239.
17. Cafri G, Olivardia R, Thompson JK. Symptom characteristics and psychiatric comorbidity among males with muscle dysmorphia. Compr Psychiatry. 2008;49(4):374-379.
18. VandenBerg P, Neumark-Sztainer D, Cafri G, Wall M. Steroid use among adolescents: longitudinal findings from Project EAT. Pediatrics. 2007;119(3):476-486.
19. American Psychiatric Association. Guideline Watch: Practice Guideline for the Treatment of Patients with Eating Disorders. 3rd ed. Washington, DC: APA; August 2012. http://psychiatryonline.org/pb/assets/raw/sitewide/practice_guidelines/guidelines/eatingdisorders-watch.pdf. Accessed July 15, 2015.
20. Treasure J, Claudino AM, Zucker N. Eating disorders. Lancet. 2010;375:583-593.
21. McElroy SL, Hudson JI, Mitchell JE, et al. Efficacy and safety of lisdexamfetamine for treatment of adults with moderate to severe binge-eating disorder; a randomized clinical trial. JAMA Psychiatry. 2015;72(3):235-246.
22. American Psychiatric Association. Practice Guideline for the Treatment of Patients with Eating Disorders. 3rd ed. Washington, DC: APA; June 2006. http://psychiatryonline.org/pb/assets/raw/sitewide/practice_guidelines/guidelines/eatingdisorders.pdf. Accessed July 15, 2015.
To comment on this article, contact rdavidson@uspharmacist.com.





