US Pharm. 2013;38(6):43-48.
ABSTRACT: Oral sores can occur anywhere in the oral cavity and oropharyngeal region. Since not all oral sores are benign, a careful differential diagnosis is important. The two most common types are canker sores (recurrent aphthous stomatitis) and cold sores (herpetic lesions). Early intervention is important with both. The pharmacist will most likely be the primary source for recommending medications (e.g., topical corticosteroids, oral and topical antivirals) for the treatment of these conditions.
Oral sores can occur anywhere in the oral cavity and oropharyngeal region, including the lips, oral mucosa (movable tissue inside the lips, vestibule, and cheeks), gingivae or gums (nonmovable tissue immediately surrounding the teeth), tongue, soft and hard palate, and throat. Most oral sores are painful and annoying and, in severe cases, can cause significant morbidity. The two most common oral sores are canker sores and cold sores. The pharmacist will most likely be the primary source for recommending medications for the treatment of these conditions.
Canker Sores
Canker sores, also known as recurrent aphthous stomatitis (RAS) or recurrent aphthous ulcers (RAU), are one of the most common oral ulcer conditions, affecting up to 66% of the population at some point in their lifetime.1,2 About 1% of children from higher socioeconomic backgrounds in developed countries are affected by canker sores.1 RAS usually occurs in an otherwise healthy individual.
The key distinguishing presentation of RAS is that it appears on movable oral mucosa as opposed to keratinized, nonmovable tissue. Slightly more females than males experience RAS.3 The rate of recurrence of RAS is up to 25%, with a 3-month recurrence rate as high as 50%.4 Most people develop one to three ulcers at a time and may have a recurrence from immediately after an old ulcer heals to up to twice a year.
Clinical Presentation: Diagnosis of RAS is based on history and clinical appearance of the lesions. Canker sores usually first appear in the mouth as single or multiple small, red, round or ovoid spots with a prodromal symptom of tingling or burning that can occur 1 to 2 days before the appearance of the ulcer. Then an ulcer appears that is clearly defined, shallow, round, or oval with a red halo and a yellowish-gray center. Pain usually dissipates after 3 to 4 days and the lesion turns gray, at which point epithelialization occurs.1,4 RAS ulcers are extremely painful and may interfere with talking and eating.
There are three classifications of RAS, which are differentiated according to the size of the lesion2,4,5:
• Minor RAS, the most common type, appears as small ulcers of 5 to 10 mm. Healing occurs in about 7 to 10 days. Minor RAS is frequently seen on the floor of the mouth, inside of the cheek, and on the ventral and lateral board of the tongue. There is no residual scarring.
• Major RAS (Sutton’s disease) is larger ulcers (>10 mm) that are usually associated with medical comorbidities. Healing is slow, over 10 to 40 days. Major RAS usually appears on the lips, soft palate, and throat and tends to heal with scarring.
• Herpetiform ulcers, the uncommon RAS, are <5 mm in size. These painful lesions are initially multiple pinpoint sores and usually occur in older individuals. Healing takes about 7 to 10 days.
Pathophysiology: Despite the high prevalence of RAS, evidence is uncertain regarding the etiology. Genetics may play a role, with an immunologic proclivity in 33% to 42% of cases.4,6 There is a strong immunologic association with genotypes of interleukin (IL)-1 beta and IL-6 in individuals with RAS. Research has failed to find a pathogenic microorganism. Since there is no microorganism associated with RAS, it is not infectious, contagious, or sexually transmitted.1,4
In about 80% of people, RAS initially occurs in childhood or adolescence and gradually decreases in frequency and severity over time, resolving by 40 years of age.4,7 There are many risk factors associated with the development of RAS (TABLE 1).1,4,7-9 When onset occurs in an older individual, the cause is often associated with a systemic condition such as Behçet’s syndrome, autoimmune disease (e.g., HIV/AIDS), or a gastrointestinal condition. Oral lesions that are seen in systemic conditions are quite similar in appearance to RAS and are referred to as aphthous-like lesions.1,7,8 These cases may present as major aphthous ulcers. Certain drugs, including nonsteroidal anti-inflammatory drugs (NSAIDs) and nicorandil (a potassium channel blocker), cause RAS-like lesions.9,10 Illicit use of cocaine (e.g., smoking crack) may cause aphthous-like lesions on the palate.11

Management: The clinician must first properly diagnose a person with RAS by ruling out any associated systemic conditions that present with aphthous-like lesions.7 If a predisposing factor can be identified, it should be eliminated or reduced.
It is important to remember that RAS is benign and neither contagious nor infectious and will heal spontaneously in 7 to 10 days. There are no definitive guidelines for the treatment of RAS. Therefore, palliative treatment is recommended in patients who cannot tolerate the pain. If the ulcer is present for more than 2 to 3 weeks, the pharmacist should advise the individual to see a dentist.7

Treatment, for the most part, is empirical and nonspecific (TABLE 2).1,4,8,9 A selection of topical agents has been used for palliation to control the condition (i.e., reduce the healing time) and for an analgesic effect (TABLE 3).1,2 For minor RAS, palliative medication may not be necessary. However, if needed, topical agents, OTC analgesics, and prescription corticosteroids to reduce inflammation are probably sufficient for the course of the disease. Topical corticosteroids do not reduce the recurrence of the lesions or result in permanent remission, but if initiated at the time of the prodromal stage, may help abort the attack and reduce pain.1,4 Oral candidiasis and systemic absorption of the steroid through the ulcerated mucosa are of concern.
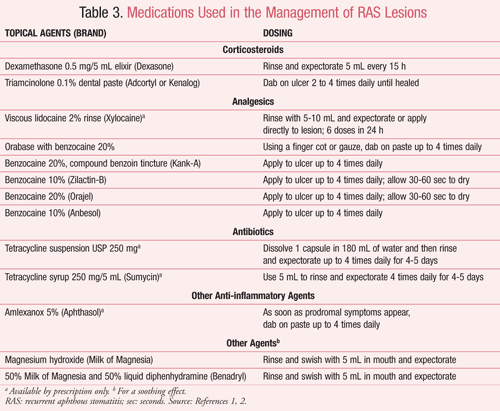
A topical paste such as amlexanox 5% (Aphthasol), which reduces healing time, accelerates pain resolution, and prevents recurrences, is recommended if there is only one lesion. A mouth rinse is indicated if there are several lesions in the mouth. Topical pastes, liquids, or gels have lidocaine or benzocaine as the active analgesic ingredient. Kank-A Mouth Pain Liquid contains compound benzoin tincture as an oral mucosal protectant. A specific preparation containing Orabase paste (carboxymethylcellulose) is indicated for intraoral use. This agent is compounded with either benzocaine (OTC) for an analgesic effect or triamcinolone for anti-inflammatory effect. When using this product, the patient is instructed to use a finger cot and to dab rather than rub the product on the lesion to allow it to adhere to the ulcer.12
Rinsing with a mouthwash (e.g., chlorhexidine gluconate) or water and salt twice a day for 6 weeks is also helpful. Although a bacterial etiology is not recognized as of yet, oral suspensions of tetracycline or doxycycline may be useful in speeding up healing time.5 Chlorhexidine mouth rinse is preferred over tetracycline for refractory cases because tetracyclines cause enamel discoloration when taken by children under 8 years of age and by pregnant women. Additionally, there is an increased risk of developing oral candidiasis.13
Adjunctive dietary and lifestyle management is important. For example, spicy and hot foods, smoking, alcohol, and citrus fruit drinks should be avoided. Since many patients are deficient in vitamin B12, zinc, or folic acid, a supplement can be recommended; however, this association is still unclear and is not advised as first-line treatment.2,14 Silver nitrate cautery may result in local necrosis and delayed healing.5,15
Major RAS and herpetiform ulcers that do not respond to topical agents will most likely require systemic drugs. Those who have them should be referred to a medical or dental specialist. Systemic immunomodulatory agents including prednisolone, methotrexate, colchicine, dapsone, pentoxifylline, thalidomide, interferon alfa, and tumor necrosis factor (TNF) antagonists have been used in resistant cases of major RAS or aphthous ulcers with systemic involvement.2,16,17
Herpetic Lesions
Herpes simplex virus type 1 (HSV-1) is a nongenital infection usually transmitted during childhood through nongenital contact. HSV-1 can occur as either a primary or recurrent infection. HSV-1 lesions usually occur on the oral mucosa, lips, and hard palate. Other nonoral HSV-1 infections include herpetic keratitis, herpetic whitlow, herpes gladiatorum, and herpetic sycosis of the beard.18
Primary herpes infection occurs with the first exposure to HSV-1. This infection is referred to as primary herpetic gingivostomatitis (PHGS) and usually occurs in infants and children (between 2 and 3 years of age) by nonsexual contact, but can occur in adults through sexual contact. After primary exposure, herpes simplex virus may persist in a latent state in the trigeminal ganglion until it is reactivated in adulthood.19
All herpes infections, whether type 1 or genital type 2, are transmissible from person to person. An important part of the transmission is intimate contact between an infected shedding person (the host) and a susceptible person. Common stimuli that disturb the host’s immune system include trauma to the oral area, fever, menstruation, exposure to sunlight, or prolonged use of corticosteroids. By adulthood, up to 90% of people will have antibodies to HSV-1.20
Pathophysiology (PHGS): The initial or primary transmission of HSV-1 is via contact with an infected person’s saliva through kissing or sharing food utensils or hand towels. The virus travels from the skin during contact and invades and replicates in neurons and skin cells. It is highly contagious and typically affects children but is also seen in adults.21 The virus remains dormant in the trigeminal sensory ganglia until a stimulus reactivates it. This results in the development of recurrent herpetic infections, which appear on the mucosa of the lips, on the face, and on the oropharyngeal and ocular mucosa.22
Clinical Features (PHGS): In children and young adults, PHGS is characterized by a high fever, malaise, fatigue, nausea and vomiting, and oral ulcers.18 Adults may have less typical clinical features, making a diagnosis more difficult.
Painful intraoral vesicles appear on the oral mucosa (e.g., lips, gingiva, hard palate, tongue), which rapidly rupture, forming small ulcers with red halos. Usually the child refuses to eat or drink because of the severe pain. Lesions first appear 12 to 36 hours after the initial symptoms. Lesions are self-limiting and will usually resolve within 10 to 14 days.23 There is also a generalized severe gingivitis, and submandibular and cervical lymphadenopathy may be present.
Diagnosis and Management: The clinical appearance of HSV-1 is usually diagnostic, but viral DNA testing can be done to confirm the diagnosis, if necessary.18 Since the infection is self-limiting but severely painful, treatment is palliative, including fluids and analgesics or antipyretics such as acetaminophen. Aspirin is contraindicated in children under 19 years of age with a viral illness due to the risk of Reye syndrome.24 Acyclovir (Zovirax) oral suspension (15 mg/kg 5 times a day for 7 days) is highly recommended.25 Early treatment with acyclovir or famciclovir may significantly shorten the duration of clinical manifestations and infectivity of affected children.
Recurrent Herpetic Infections (Cold Sores)
Once the dormant herpes virus is reactivated, it becomes recurrent herpes. Usually outbreaks occur on the lips, a condition referred to as herpes labialis (also known as cold sores or fever blisters). There is typically a prodromal burning or itching at the site 12 to 36 hours preceding the eruption.18 Clinically, a small, well-circumscribed cluster of small vesicles (blisters) appears on heavily keratinized oral mucosa, including the vermillion border of the lips, and the gingivae, hard palate, and tongue. These vesicles subsequently rupture, ulcerate, and crust within 24 to 48 hours. If left untreated, lesions may last past 14 days.19
Other nongenital manifestations of recurrent herpes include keratoconjunctivitis and herpetic whitlow of the finger. Typically, recurrent infections are not as severe as primary infections. Recurrence of herpetic lesions occurs due to stress, sunlight, immunosuppression, trauma (e.g., after a dental procedure), or other irritants.18
Management: Oral and topical medications are used to treat the herpetic lesions, as well as to prevent recurrences (TABLE 4).18,23 Antiviral drugs inhibit viral DNA synthesis, which may reduce healing time, viral shedding, and frequency of recurrences, but do not cure the condition.

Prescription drugs are effective when applied early and can reduce healing time by 1 to 2 days.26 However, these prescription medications are also expensive and have adverse effects.27 Penciclovir 1% cream (Denavir) is recommended in nonimmunocompromised individuals and should be applied during the prodromal stage.28 Acyclovir (systemic, topical) is prescribed for immuno-compromised and immunocompetent patients. Adverse effects of oral acyclovir include malaise, nausea, vomiting, diarrhea, and headaches. Topical acyclovir can cause mild pain, burning, or stinging.29
OTC Abreva (docosanol 10% cream) is applied at the first sign of a cold sore until the infection is healed.27 It works by inhibiting the fusion of the virus with the human cell membrane, thereby blocking entry and subsequent viral replication. Abreva has similar efficacy to prescription topical antiviral agents.30 Caution should be used when recommending Abreva to pregnant and nursing women and should not be used in children under 12 years of age. Headache is the most common adverse effect.30
Viroxyn Professional Use (benzalkonium chloride 0.13% with 7.5% benzocaine) was FDA approved in 2012. It is a nonprescription product available through dental professionals only. In a retrospective study, it was shown to be significantly more effective than Abreva. Viroxyn reduces the discomfort of a cold sore and is applied in a single application.27
Other OTC products available for palliative or symptomatic relief include petrolatum and cocoa butter to keep lesions moist and prevent cracking, which would make them more susceptible to secondary infection. If it is too late after the first symptoms appear to apply an antiviral agent, then a topical anesthetic such as Orabase-B (20% benzocaine) may help reduce the pain, burning, and itching. Individuals allergic to para-aminobenzoic acid (PABA) or sulfonamides may also be allergic to benzocaine. Products containing camphor (not >3%) and menthol (not >1%) act as an analgesic to relieve pain and itching. Natural products such as bioflavonoids or acidophilus are not FDA approved and have not demonstrated efficacy in controlled clinical trials.31
Conclusion
Since not all oral sores are benign, a careful differential diagnosis is important. There are many conditions that mimic and some drugs that produce classic aphthous ulcers. Most lesions can be diagnosed based on clinical appearance and history. However, if an oral sore does not heal within a certain time frame, a biopsy may be required.
Early intervention is important with both RAS and herpetic lesions. A properly diagnosed RAS responds well to topical corticosteroids. Herpes labialis responds well to oral and topical antiviral agents.
REFERENCES
1. Scully C. Aphthous ulcers. Medscape Reference. http://emedicine.medscape.com/article/867080-overview. Accessed March 5, 2013.
2. McBride DR. Management of aphthous ulcers. Am Fam Physician. 2000;62:149-154.
3. Scully C, Gorsky M, Lozada F. The diagnosis and management of recurrent aphthous stomatitis. A consensus approach. J Am Dental Assoc. 2003;134:200-207.
4. Barrons RW. Treatment strategies for recurrent oral aphthous ulcers. Am J Health Syst Pharm. 2001;58:41-50.
5. Preeti L, Magesh Rajkumar K, Karthik R. Recurrent aphthous stomatitis. J Oral Maxillofac Pathol. 2011;15:252-256.
6. Jurge S, Kuffer R, Scully C, Porter SR. Mucosal disease series. Number VI. Recurrent aphthous stomatitis. Oral Dis. 2006;12:1-21.
7. Rogers RS III. Recurrent aphthous stomatitis: clinical characteristics and associated systemic disorders. Semin Cutan Med Surg. 1997;16:278-283.
8. Messadi DV, Younai F. Aphthous ulcers. Dermatol Ther. 2010;23:281-290.
9. Shotts RH, Scully C, Avery CM, Porter SR. Nicorandil-induced severe oral ulceration: a newly recognized drug reaction. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1999;87:706-707.
10. Healy CM, Thornhill MH. An association between recurrent orogenital ulceration and nonsteroidal anti-inflammatory drugs. J Oral Pathol Med. 1995;24:46-48.
11. Leao JC, Gomes VB, Porter S. Ulcerative lesions of the mouth: an update for the general practitioner. Clinics. 2007;62:769-780.
12. Aphthasol, Kank-A, Orabase with benzocaine. www.drugs.com. Accessed
May 14, 2013.
13. Weinberg MA, Froum J. The Dentist’s Drug and Prescription Guide. Ames, IA: Wiley-Blackwell; 2012:55-56.
14. Volkov I, Rudoy I, Freud T, et al. Effectiveness of
vitamin B12 in treating recurrent aphthous stomatitis: a randomized,
double-blind, placebo-controlled trial. J Am Board Fam Med. 2009;22:9-16.
15. Altenburg A, Zouboulis CC. Current concepts in the treatment of recurrent aphthous stomatitis. Skin Therapy Lett. 2008;13:1-4.
16. Eisen D, Lynch DP. Selecting topical and systemic agents for recurrent aphthous stomatitis. Cutis. 2001;68:201-206.
17. Altenburg A, Abdel-Naser MB, Seeber H, et al. Practical aspects of management of recurrent aphthous stomatitis. J Eur Acad Dermatol Venereol. 2007;21:1019-1026.
18. Usatine RP, Tinitigan R. Nongenital herpes simplex virus. Am Fam Physician. 2010;82:1075-1082.
19. Gonsalves WC, Chi AC, Neville BW. Common oral lesions: Part I. Superficial mucosal lesions. Am Fam Physician. 2007;75:501-506.
20. Gilbert S, Corey L, Cunningham A, et al. An update on
short-course intermittent and prevention therapies for herpes labialis. Herpes. 2007;14(suppl 1):13A-18A.
21. Nasser M, Fedorowicz Z, Khoshnevisan MH, Shahiri TM. Acyclovir for treating primary herpetic gingivostomatitis. Cochrane Database Syst Rev. 2008;(4):CD006700.
22. Blevins JY. Primary herpetic gingivostomatitis in young children. Pediatr Nurs. 2003;29:199-202.
23. Cernik C, Gallina K, Brodell RT. The treatment of herpes simplex infections: an evidence-based review. Arch Intern Med. 2008;168:1137-1144.
24. Orlowski JP, Hanhan UA, Fiallos MR. Is aspirin a cause of Reye’s syndrome? A case against. Drug Saf. 2002;25:225-231.
25. Faden H. Management of primary herpetic gingivostomatitis in young children. Pediatr Emerg Care. 2006;22:268-269.
26. Esmann J. The many challenges of facial herpes simplex virus infection. J Antimicrob Chemother. 2001;47:17-27.
27. McCarthy JP, Brownling WD, Teerlink C, Veit G.
Treatment of herpes labialis: comparison of two OTC drugs and untreated
controls. J Esthet Restor Dent. 2012;24:103-109.
28. Denavir (penciclovir cream 1%). www.rxlist.com. Accessed May 14, 2013.
29. Zovirax (acyclovir ointment 10%). www.rxlist.com. Accessed May 14, 2013.
30. Treister NS, Woo SB. Topical n-docosanol for management of recurrent herpes labialis. Expert Opin Pharmacother. 2010;11:853-860.
31. Leung DT, Sacks SL. Docosan: a topical antiviral for herpes labialis. Expert Opin Pharmacother. 2004;5:2567-2571.
To comment on this article, contact rdavidson@uspharmacist.com.





