US Pharm. 2017;42(2):27-31.
ABSTRACT: Coronary artery disease (CAD) is the most common type of heart disease and the leading cause of death worldwide. Angina pectoris, a clinical syndrome characterized by discomfort typically located in the chest, neck, or left arm, is one of several clinical manifestations of CAD. The gold standard for diagnosing and evaluating CAD is coronary angiography. The goals of treatment are to maximize quality of life and minimize the risk of death through the modification of risk factors such as diabetes, hypertension, and hyperlipidemia and the management of acute ischemic symptoms. Some frequently used pharmacotherapeutic options include beta-blockers, calcium channel blockers, nitrates, ACE inhibitors, statins, and antiplatelet agents.
Coronary artery disease (CAD), also known as coronary heart disease, coronary artery atherosclerosis, or stable ischemic heart disease (SIHD), occurs when there is an inadequate blood supply to the myocardium. This is usually caused by atherosclerotic buildup in the coronary arteries. CAD is the leading cause of death worldwide.1
Angina pectoris, a clinical syndrome characterized by discomfort typically located in the chest, neck, or left arm, is one of several possible clinical manifestations of coronary heart disease.2 Chronic stable angina pectoris is a common manifestation of CAD. An estimated 15.5 million American adults have chronic CAD, and more than seven million have angina. Angina is the initial manifestation in approximately one-half of all patients who present with CAD. The presence of chronic angina approximately doubles the risk of major cardiovascular events (CVEs).1
Chest pain that can be characterized as chronic stable angina typically is produced with physical exertion and is relieved by rest and/or nitroglycerin. In contrast, chest pain that occurs at rest usually is indicative of unstable disease such as acute coronary syndromes (ACS).2 Many patients, however, describe angina not as frank pain but as tightness, pressure, or discomfort. Women and the elderly, in particular, may present with atypical symptoms such as nausea, vomiting, mid-epigastric discomfort, or sharp (atypical) chest pain. Anginal pain caused by cardiac ischemia typically lasts minutes. The location is usually substernal, and pain can radiate to the neck, jaw, epigastrium, or arms. Pain above the mandible, below the epigastrium, or localized to a small area over the left lateral chest wall is rarely angina. Angina is often precipitated by exertion or emotional stress and relieved by rest. Sublingual nitroglycerin usually relieves angina within 30 seconds to several minutes.3
Diagnosis
The evaluation of patients with SIHD includes coronary angiography, which is considered the gold standard for CAD diagnosis.4 Coronary angiography uses a contrast material and x-rays to show how blood flows through the coronary arteries.5 Patients in whom SIHD is suspected who have unacceptable ischemic symptoms and who, despite guideline-directed medication therapy, still have persistent ischemic symptoms may benefit from coronary angiography. Coronary angiography may be able to define the extent and severity of CAD in patients in whom SIHD is suspected. These patients must be amenable to and qualify for coronary revascularization and have undergone noninvasive testing, excluding stress tests indicating a high likelihood of severe IHD. Coronary angiography may also be beneficial in patients who cannot undergo stress testing or have an indeterminate or nondiagnostic stress test when there is a high likelihood that findings may result in changes to therapy. Additionally, coronary angiography may be considered in patients with acceptable stress-test results not suggestive of the presence of CAD when clinical suspicion of CAD remains high and the likelihood is great that findings may result in changes to therapy.5
Guideline-Directed Therapy
The goals of treating patients with SIHD are to maximize quality of life and minimize the risk of death. Guidelines for the management of SIHD state that the following fundamental strategies, when combined, can help achieve these goals4:
1. Patient education on the causes, clinical presentation, treatment options, and prognosis of the disease, in order to encourage active participation in treatment decisions
2. Identification and treatment of conditions that can contribute to or worsen the disease
3. Modification of risk factors through both pharmacologic and nonpharmacologic strategies
4. Use of pharmacologic treatments to improve quality of life and/or survival, with particular attention to side effects and drug interactions
5. Use of cardiac revascularization, when appropriate, to optimize overall health status and improve survival
It is important to remember that not all strategies with evidence of mortality benefit will offer patients improved quality of life. Additionally, some treatments that potentially have no effect on survival are implemented in order to improve symptoms and quality of life.4
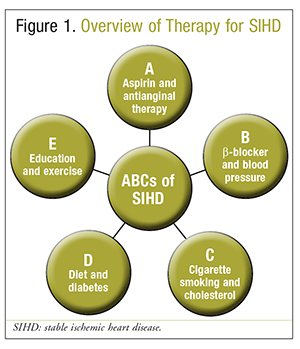
It is crucial for the patient to have a personalized education plan to optimize care and promote wellness. The education plan must include essential components such as (but not limited to) the importance of medication adherence; a comprehensive review of all therapeutic options; exercise education; self-monitoring skills; and how to recognize an exacerbation.4 See FIGURE 1.
Lifestyle modification includes daily physical activity, weight management, and dietary restrictions, such as reduction of saturated fats (<7% of total calories), trans-fatty acids (<1% of total calories), and cholesterol (<200 mg/day). In addition, a moderate-dose or high-dose statin should be prescribed in the absence of contraindications or documented adverse effects. Alternatively, bile acid sequestrants could be used.4
All patients should be counseled on the need for weight control, increased physical activity, alcohol moderation, and sodium reduction. Increased consumption of low-fat dairy products and fresh fruits and vegetables should be emphasized. In addition to or after a trial of the above lifestyle modification, if the patient’s blood pressure (BP) remains >140/90 mmHg, antihypertensive therapy should be initiated. Recommendations include ACE inhibitors and/or beta-blockers; possible additions include thiazide diuretics or calcium channel blockers, if needed, to achieve a goal BP <140/90 mmHg. Additionally, in patients who consume alcohol, a reasonable quantity of alcohol is one drink (4 oz wine, 12 oz beer, or 1 oz spirits) per day for nonpregnant women and one or two drinks per day for men, unless alcohol is contraindicated (e.g., patients with a history of alcohol abuse/dependence or liver disease).4
In patients with a short duration of diabetes mellitus and a long life expectancy, a goal glycosylated hemoglobin (HbA1c) of ≤7% is reasonable. The goal may be adjusted to 7% to 9% depending on age, history of hypoglycemia, presence of microvascular or macrovascular complications, or presence of coexisting medical conditions. Initiation of pharmacologic interventions may be warranted to achieve goal HbA1c, but rosiglitazone, which is associated with an increased risk of cardiovascular complications, should not be initiated in patients with SIHD. Patients who are already receiving this agent and whose blood glucose is well controlled should be counseled about the potential hazards, and a switch to a different agent should be strongly considered.4
Physical activity is an integral component of a comprehensive coronary risk-factor modification strategy for patients with SIHD. Clinicians should encourage 30 to 60 minutes of moderate-intensity aerobic activity, such as brisk walking, at least 5 days and preferably 7 days per week, supplemented by an increase in daily lifestyle activities (e.g., walking breaks at work, gardening, household work) to improve cardiorespiratory fitness. Complementary resistance training twice weekly is also a reasonable addition. Goals should be a BMI of 18.5 to 24.9 kg/m2 and a waist circumference <102 cm (40 in.) in men and <88 cm (35 in.) in women (less for certain ethnic groups). The initial goal of weight-loss therapy should be to reduce body weight by approximately 5% to 10% from baseline. When the initial goal is met, further weight loss may be attempted.4
Observational studies over the past four decades have furnished incontestable evidence that smoking increases the risk of cardiovascular disease; therefore, smoking cessation and avoidance of exposure to environmental tobacco smoke is of paramount importance for SIHD patients. Referral to an appropriate smoking-cessation program and initiation of pharmacotherapy are recommended as a stepwise approach to smoking cessation.6
The World Health Organization and the American Heart Association/American College of Cardiology Foundation recommend annual IM administration of the inactivated influenza vaccine to prevent all-cause mortality and morbidity in patients with underlying cardiovascular conditions. Influenza contributes to a higher risk of mortality and hospitalization in patients with chronic medical conditions such as cardiovascular disease, and it exacerbates underlying medical conditions.6
Medications to Prevent Myocardial Infarction and Death
Antiplatelet Therapy: Platelets and their byproducts play an important role in the incidence of occlusive vascular events, including myocardial infarction (MI). When these platelet-rich atherosclerotic plaques become disrupted, platelet aggregation ensues and ultimately leads to formation of a thrombus, which may precipitate a CVE.7
Aspirin is an antiplatelet agent that works through irreversible inhibition of cyclooxygenase, leading to decreased formation of the prostaglandin derivative thromboxane A2 and to inhibited platelet aggregation. Aspirin has been associated with a 37% reduction in the risk of serious CVEs, as well as a 46% decrease in the risk of unstable angina and a 53% decrease in the need for coronary angioplasty.7 Therefore, it is important that the patient be treated with aspirin 75 to 162 mg daily unless a contraindication exists. Doses of 75 to 162 mg are comparable to doses of 325 mg, but are associated with a lower risk of bleeding.
Clopidogrel (Plavix) is considered an acceptable alternative for patients who cannot tolerate aspirin. Clopidogrel is a thienopyridine derivative that inhibits platelet aggregation through selective and irreversible inhibition of the adenosine diphosphate P2Y12 receptor. In one study, clopidogrel 75 mg daily demonstrated superiority over aspirin 325 mg daily, although the degree of clinical benefit was small.8 Because no other studies have been conducted comparing the two agents in this patient population, clopidogrel is considered an alternative to aspirin.
Prasugrel (Effient), another thienopyridine antiplatelet agent, has more potent antiplatelet effects and less interpatient variability in response compared with clopidogrel, but it has an increased risk of bleeding in patients undergoing percutaneous coronary intervention (PCI). Prasugrel is not currently indicated for patients with SIHD without ACS.9 The newest P2Y12 inhibitor, ticagrelor (Brilinta), is also indicated only for patients with ACS.10
Dipyramidole, which is commonly prescribed in combination with aspirin (as Aggrenox) in patients with ischemic stroke, also possesses antiplatelet effects, but it does not have an established role in patients with SIHD. Moreover, because dipyridamole vasodilates coronary resistance vessels and can provoke exercise-induced myocardial ischemia, it is not recommended for secondary prevention in patients with SIHD.6
Dual antiplatelet therapy (DAPT) with aspirin and clopidogrel can provide additional benefits and may reduce CVEs and mortality in certain high-risk SIHD patients. It is well established that patients with a recent MI who have undergone PCI with stent placement require DAPT for up to 1 year. DAPT is not recommended in patients with SIHD without prior stent implantation and no history of ACS or MI.11 Decisions about treatment with, and duration of, DAPT in SIHD patients who have a history of MI or coronary stent implantation require a careful assessment of the benefits versus risks and a consideration of patient preference.
Beta-Blockers
Beta-blockers reduce myocardial oxygen consumption through a decrease in heart rate and myocardial contractility. This reduction in heart rate allows for greater time spent in diastole, thereby promoting greater coronary perfusion and myocardial oxygen supply. This medication class is recommended to be initiated and continued for 3 years in patients with normal left ventricular function after an MI. For patients with left ventricular dysfunction, beta-blocker therapy should be continued indefinitely. Particular attention should be paid to the beta-blocker used in this patient population. Carvedilol, metoprolol succinate, and bisoprolol have been shown to reduce the risk of death in patients with chronic systolic heart failure (HF). This survival benefit does not extend to patients with chronic stable angina in the absence of MI or HF. However, beta-blockers should be used as first-line therapy with the goals of reducing the frequency and severity of angina and improving exercise capacity and quality of life.6
ACE Inhibitors and Angiotensin Receptor Blockers (ARBs): A body of evidence suggests that ACE inhibitors, in addition to their established efficacy in the management of hypertension, have benefits extending beyond their BP-lowering effects. The main mechanism by which ACE inhibitors work is a reduction of angiotensin II and an increase in bradykinin. Angiotensin II causes vasoconstrictive effects that increase oxidative stress, promote inflammation and thrombosis, damage the endothelium, and worsen atherosclerosis. Bradykinin promotes vasodilation, which counteracts the harmful effects of angiotensin II.12
Clinical trials have consistently shown that ACE inhibitors reduce the risk of morbidity and mortality from HF, stroke, MI, diabetes, and renal impairment. ACE inhibitors may also offer a protective effect for patients with SIHD. A clinical trial conducted in SIHD patients with no clinical evidence of HF showed a reduction in the composite endpoint of cardiovascular death.13 Therefore, it is recommended that all patients with SIHD who also have one or more risk factors, such as hypertension, diabetes, HF, or chronic kidney disease, be prescribed an ACE inhibitor. ARBs are recommended as an alternative for patients who cannot tolerate ACE inhibitors.
Medications to Relieve Symptoms (Anti-Ischemics)
Beta-Blockers: As stated above, beta-blockers are considered first-line therapy for management of SIHD symptoms, particularly exercise-induced angina. Because beta-blockers reduce BP and heart rate during exercise, the onset of angina or ischemic threshold is delayed or avoided altogether.6 Any beta-blocker may be used for treatment, although it is important to consider the beta-blocker’s selectivity, dosing requirements, and cost. Selective beta-blockers such as metoprolol and atenolol are commonly used. If a beta-blocker is being considered in a patient with vasospastic or variant (Prinzmetal’s) angina, one with alpha-blocking properties, such as carvedilol or labetalol, should be used because unopposed alpha blockade in these patients can potentially induce coronary vasospasm. The beta-blocker dose should be adjusted to limit the resting heart rate to about 55 bpm because higher resting heart rates have been associated with higher rates of mortality.6
Adherence to beta-blocker therapy may be limited by adverse effects. Although the majority of patients tolerate beta-blockers, some patients may experience fatigue, sexual dysfunction, lethargy, or sleep disturbances. If a patient is unable to tolerate beta-blocker therapy, the next option would be a calcium channel blocker or a long-acting nitrate for relief of symptoms.6
Calcium Channel Blockers: Calcium channel blockers are generally added to beta-blocker therapy when initial treatment with a beta-blocker does not adequately improve symptoms; they are also used as an alternative when beta-blocker use is contraindicated. However, beta-blockers have been shown to more effectively alleviate anginal symptoms and improve exercise tolerance, and they have an added survival benefit in patients who have HF or have had an MI.6
Dihydropyridine (e.g., nifedipine, amlodipine) and nondihydropyridine (e.g., verapamil, diltiazem) calcium channel blockers produce coronary vasodilation, a reduction in myocardial contractility, and a decrease in myocardial oxygen demand. Both classes are effective in managing anginal symptoms, so decisions about which one to use should be made on a case-by-case basis, with particular attention paid to drug interactions, adverse effects, and other patient-specific factors. Calcium channel blockers are the drugs of choice for patients with Prinzmetal’s angina, along with nitrates used alone or in combination.6
Nondihydropyridines depress cardiac pacemaker rates and slow conduction, which can lead to sinus bradycardia; therefore, dihydropyridines are preferred in patients with cardiac-conduction defects such as sick sinus syndrome and sinus bradycardia. Combining diltiazem or verapamil with beta-blockers generally should be avoided because of enhanced effects on slowed heart rate and contractility, unless combination therapy is needed to achieve heart-rate control, particularly in patients with atrial fibrillation.6
Major adverse effects of dihydropyridines include headache, palpitations, flushing, and peripheral edema due to excessive arterial vasodilation. Verapamil can cause significant constipation, especially in elderly patients.6
Nitrates: Nitrates, which are effective at managing all forms of angina, are first-line therapy for the management of acute anginal symptoms. They relax vascular smooth muscle and reduce myocardial oxygen demand by inducing systemic vasodilation. By dilating veins, nitrates reduce the pressure of the blood returning to the heart (preload), and by dilating arteries, they reduce the pressure against which the heart has to pump (afterload). Both of these effects lead to a decrease in oxygen demand.14
Long-acting nitrates, such as isosorbide dinitrate, isosorbide mononitrate, and nitroglycerin, are recommended when beta-blockers or calcium channel blockers are not tolerated or are contraindicated, or when additional therapy is needed to achieve symptom control.6 Despite differences in dosing and formulation, all nitrates seem to be roughly equivalent. Nitrates should be dosed and titrated using the lowest dose possible to alleviate symptoms and reduce the incidence of adverse effects such as headache, flushing, and tolerance. Nitrate tolerance is defined by the loss of antianginal effects after repeated dosing, necessitating increasingly higher doses to achieve a clinical effect. Therefore, a nitrate-free interval of 10 to 14 hours must be maintained to avoid tolerance. The use of long-acting nitrates does not lead to tolerance to sublingual products.6
All patients with SIHD should be prescribed sublingual nitroglycerin tablets or spray for acute episodes of angina. Most patients respond within 5 minutes of taking these products, but if relief does not occur, the patient should be advised to seek medical attention immediately. These products also may be used for prevention of exercise-induced angina; their effect lasts 30 to 40 minutes.6
Ranolazine: Ranolazine (Ranexa) is another therapy for chronic angina. It works by inhibiting the late inward sodium current in heart muscle and reducing sodium-dependent calcium levels, leading to a reduction in heart-wall tension and a decrease in oxygen consumption. Because ranolazine does not cause significant changes in heart rate or BP, it is an attractive alternative for patients with bradycardia or hypotension.15 It can be used in combination with beta-blockers when relief of symptoms has not been successful, or as an alternative therapy if beta-blockers are contraindicated.6
Ranolazine prolongs the QTc interval in a dose-dependent manner; however, there is little experience with coadministration of other QT-prolonging agents. Of note, studies have shown a lower incidence of arrhythmias such as ventricular tachycardia, bradycardia, and atrial fibrillation with ranolazine compared with placebo. Ranolazine also may lower HbA1c in patients with diabetes. Its use is contraindicated in patients with clinically significant hepatic impairment. The most common adverse effects are constipation, dizziness, headache, and nausea.15
Revascularization
Revascularization refers to procedures that are performed to restore blood flow to the tissues.16 Coronary artery bypass graft (CABG) and PCI are revascularization procedures performed in patients to address SIHD. These procedures may be performed either for symptomatic relief or to improve survival. The Heart Team approach (i.e., multidisciplinary care) is recommended in patients with diabetes mellitus and complex multivessel disease. In this subset of patients, CABG is preferred to PCI to improve survival.4
Conclusion
The primary goals of treatment for patients with SIHD are to maximize quality of life and minimize the risk of death. Risk-factor reduction can be achieved through the optimal management of diabetes, hypertension, and hyperlipidemia. Additional therapies known to reduce the incidence of cardiac events, such as aspirin, weight loss, smoking cessation, and exercise, should be implemented to manage symptoms. Beta-blockers are the preferred initial agents; however, calcium channel blockers, ranolazine, and nitrates may be used to relieve symptoms when initial beta-blocker treatment is unsuccessful or if beta-blockers are contraindicated or cause intolerable adverse effects. Understanding the role of these medications, as well as keeping abreast of the evidence supporting their use, is crucial in reducing morbidity and mortality in patients with SIHD.
REFERENCES
1. Go AS, Mozaffarian D, Roger VL, et al; American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Heart disease and stroke statistics—2014 update: a report from the American Heart Association. Circulation. 2014;129:e28-e292.
2. Trujillo TC, Dobesh PP. Traditional management of chronic stable angina. Pharmacotherapy. 2007;27:1677-1692.
3. Ohman EM. Chronic stable angina. N Engl J Med. 2016;374:1167-1176.
4. Fihn SD, Blankenship JC, Alexander KP, et al. 2014 ACC/AHA/AATS/PCNA/SCAI/STS focused update of the guideline for the diagnosis and management of patients with stable ischemic heart disease: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines, and the American Association for Thoracic Surgery, Preventive Cardiovascular Nurses Association, Society for Cardiovascular Angiography and Interventions, and Society of Thoracic Surgeons. J Am Coll Cardiol. 2014;64:1929-1949.
5. MedlinePlus. Coronary angiography. https://medlineplus.gov/ency/article/003876.htm. Accessed November 17, 2016.
6. Fihn SD, Gardin JM, Abrams J, et al. 2012 ACCF/AHA/ACP/AATS/PCNA/SCAI/STS guideline for the diagnosis and management of patients with stable ischemic heart disease: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines, and the American College of Physicians, American Association for Thoracic Surgery, Preventive Cardiovascular Nurses Association, Society for Cardiovascular Angiography and Interventions, and Society of Thoracic Surgeons. J Am Coll Cardiol. 2012;60:e44-e164.
7. Antithrombotic Trialists’ Collaboration. Collaborative meta-analysis of randomised trials of antiplatelet therapy for prevention of death, myocardial infarction, and stroke in high risk patients. BMJ. 2002;324:71-86.
8. CAPRIE Steering Committee. A randomised, blinded, trial of clopidogrel versus aspirin in patients at risk of ischaemic events (CAPRIE). Lancet. 1996;348:1329-1339.
9. Wiviott SD, Braunwald E, McCabe CH, et al. Prasugrel versus clopidogrel in patients with acute coronary syndromes. N Engl J Med. 2007;357:2001-2015.
10. Wallentin L, Becker RC, Budaj A, et al. Ticagrelor versus clopidogrel in patients with acute coronary syndromes. N Engl J Med. 2009;36:1045-1057.
11. Levine GN, Bates ER, Bittl JA, et al. 2016 ACC/AHA guideline focused update on duration of dual antiplatelet therapy in patients with coronary artery disease: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. J Am Coll Cardiol. 2016;68:1082-1115.
12. Dzau VJ, Bernstein K, Celermajer D, et al. The relevance of tissue angiotensin-converting enzyme: manifestations in mechanistic and endpoint data. Am J Cardiol. 2001;88:1L-20L.
13. Fox KM; EURopean trial On reduction of cardiac events with Perindopril in stable coronary Artery disease investigators. Efficacy of perindopril in reduction of cardiovascular events among patients with stable coronary artery disease: randomised, double-blind, placebo-controlled, multicentre trial (the EUROPA study). Lancet. 2003;362:782-788.
14. Klabunde RE. Nitrodilators. Cardiovascular Pharmacology Concepts. http://cvpharmacology.com/vasodilator/nitro. Accessed November 20, 2016.
15. Ranexa (ranolazine) package insert. Foster City, CA: Gilead Sciences, Inc; January 2016.
16. Texas Heart Institute. Cardiovascular glossary. www.texasheart.org/HIC/Gloss/#r. Accessed November 17, 2016.
To comment on this article, contact rdavidson@uspharmacist.com.





