US Pharm. 2013;38(7):43-46.
ABSTRACT: Chronic obstructive pulmonary disease (COPD) is currently the third leading cause of death in the United States and is a major cause of disability. The recently updated Global Initiative for Chronic Obstructive Lung Disease (GOLD) guidelines address the management of stable COPD. Management of symptoms can decrease exacerbation risk and limit emergency room and hospital visits. As part of the multidisciplinary team, pharmacists can be an invaluable resource in educating patients about the disease and the proper administration of medications. Pharmacists can also have an active role in nonpharmacologic treatments such as smoking cessation and vaccine administration.
Chronic obstructive pulmonary disease (COPD) is a very common disease, with approximately 12 million people diagnosed in the United States.1,2 COPD has been associated with increased mortality, and many people remain undiagnosed. It is currently the third leading cause of death in the U.S. and is a major cause of disability.1 In 2005, more than 3 million people died as a result of COPD. Within the next 10 years, the total number of deaths from COPD is projected to increase by more than 30%.3 Previously, men were six times more likely to die from COPD than women; however, new data suggest that this trend has reversed.1
In 1998, a multidisciplinary team of physicians, health providers, and scientists across the world came together to form the Global Initiative for Chronic Obstructive Lung Disease (GOLD) to increase the awareness of COPD. The GOLD committee developed a consensus report known as the Global Strategy for the Diagnosis, Management, and Prevention of COPD that was last revised in 2011 and most recently updated in February 2013.4 This article will review updates to current guidelines for the management of stable COPD.
Pathophysiology
COPD is a preventable and progressive disease that is characterized by an increased chronic inflammatory response resulting in persistent airflow limitation.5 When exposed to noxious particles like tobacco smoke, an inflammatory response is initiated to release neutrophils and macrophages into the lungs and airways. This results in the release of chemical mediators like tumor necrosis factor alpha, interleukin 8, and leuko-triene B4. This inflammatory response is comple-mentary and leads to damage to the airways, pulmonary vasculature, and lung parenchyma.2 This state of chronic inflammation causes fibrosis due to constant repair, resulting in airflow limitation. Other processes like oxidative stress and imbalances of proteases and antiproteases may also play a role.
Combined Assessment
COPD is diagnosed by spirometric results that guide therapy. In the updated GOLD guidelines, the severity of COPD has become more multifactorial based on patient symptoms, degree of spirometric abnormality, exacerbation risk, and presence of comorbidities.4 Physicians should perform individual assessments of patients to determine the classification of disease severity.
It is often recognized that patients with COPD have multiple comorbidities that can have a major impact on quality of life and survival. These comorbidities can include cardiovascular disease, skeletal muscle dysfunction, metabolic syndrome, osteoporosis, depression, and lung cancer. It is recommended that these be identified and treated appropriately to reduce the exacerbation risk.4
The exposure to risk factors greatly impacts patients and their likelihood of developing COPD. Common risk factors include male gender, age >40 years, low socioeconomic status, occupational dusts, indoor/outdoor air pollution, respiratory infections, and genetic predisposition. The most common worldwide risk factor for COPD is cigarette smoking.3
Symptoms commonly associated with COPD include chronic cough, sputum production, and dyspnea. Frequently, questionnaires are utilized to assess the severity of individual symptoms. The Modified British Medical Research Council (mMRC) questionnaire is used to determine the health status of a patient by assessing physical limitations due to shortness of breath. The COPD Assessment Test (CAT) questionnaire is utilized to assess a patient’s quality of life with COPD. Furthermore, the Clinical COPD Questionnaire (CCQ) measures clinical control in patients. Current guidelines recommend the mMRC or CAT questionnaire as a tool to assess symptoms.4
In order to clinically diagnose COPD, spirometry is required after administration of a short-acting inhaled bronchodilator. An FEV1/FVC ratio (forced expiratory volume in 1 second/forced vital capacity) of <0.70 confirms airflow limitation.4 TABLE 1 shows the classification of airflow limitation and its correlation to disease severity, commonly referred to as COPD stage.4 There are few data to suggest that spirometric evaluation alone will adequately assess the health status of the patient. It is recommended that spirometry be used in combination with assessment of symptoms and exacerbation risk.

An exacerbation is defined as an acute event that is associated with worsening of any symptom (cough, sputum production, or dyspnea) beyond normal day-to-day functioning. COPD exacerbations can result in visits to the physician’s office, emergency room, and/or hospital. Frequent exacerbations have a high correlation with increased hospitalizations and an increased risk of mortality. Patients can be deemed to have a high exacerbation risk if they are categorized as GOLD 3 or 4 or if they have a history of two or more exacerbations in the past year.4
From the latest GOLD updates, it is now recommended to classify patients into groups (A, B, C, or D) based on the criteria seen in FIGURE 1.4 Utilize the example in the following paragraph to determine how to use this chart.
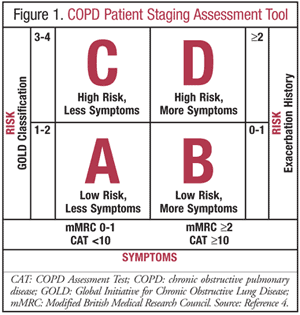
A 55-year-old patient presents with an mMRC score of 2 and a CAT score of 12. Spirometry readings showed an FEV1 of 70% of predicted and four COPD exacerbations within the past year. When assessing a patient, start with determining his or her symptoms as represented by the CAT and/or mMRC questionnaires. In this example, the patient would be classified as either Group B or D because the questionnaire results correlate with more symptoms. Next, look at the patient’s risk by comparing spirometry readings and exacerbation history. When the spirometry results are evaluated, the patient would be described as moderate disease (GOLD 2), which correlates with low risk, or Group B. When the patient’s exacerbation history is looked at, he or she would be classified as high risk, or Group D. It is recommended that the highest risk parameter be utilized to yield a more accurate reflection of the patient’s current COPD status. Therefore, this patient would be classified as Group D based on the high severity of risk associated with the history of exacerbations.
Treatment Options for Stable COPD
COPD is a progressive disease that worsens with time, and available treatment options will not eradicate the disease. Treatment goals include reducing current symptoms and future exacerbation risk.4 Effective management depends on the patient’s past medical history, current symptoms, tolerance to therapy, and accessibility to medications. Each patient should be educated about the disease state, decreasing exposure to common risk factors, proper inhaler technique, and exacerbation risk. Studies have shown that patients who are more knowledgeable about their disease are more likely to have increased medication adherence.6 Pharmacists are in the optimal setting to provide this fundamental education.
Nonpharmacologic Treatment Options
Smoking Cessation: Regardless of COPD severity, smoking cessation is considered the most important intervention for individuals who smoke.4 Pharmacists play an integral role in assisting patients in identifying nicotine replacement therapy options (e.g., nicotine inhalers, nasal sprays, OTC nicotine gum, transdermal patches, lozenges, or electronic cigarettes) to meet their specific needs and in providing counseling on appropriate usage. Additionally, health professionals, including pharmacists who provide smoking cessation counseling, have been shown to increase quit rates among patients compared to self-initiated attempts.7
Pulmonary Rehabilitation: Health care providers offer a variety of services to patients including exercise and strength training, nutrition counseling, and breathing techniques to improve the level of physical activity. It has been shown that patients who are able to maintain physical activity develop an increased exercise tolerance and are less likely to experience dyspnea and fatigue. Exercise training has also been shown to decrease the risk of mortality.8
Immunizations: Since they are at an increased risk of lower respiratory tract infections, patients with COPD should receive the pneumococcal and annual influenza vaccinations. It has been shown that patients with COPD who have received both vaccinations are at a decreased risk of acquiring pneumonia or influenza compared to patients who are not vaccinated.9 The role of pharmacists in providing services like immunizations has expanded significantly. Depending on state laws, these vaccinations can be offered conveniently in many community pharmacy settings.
Pharmacologic Treatment Options
Current treatment options aid in improving symptoms and decreasing the risk of exacerbations. Pharmacologic agents are selected depending on the patient’s individual response, tolerability, and availability. TABLE 2 lists drugs commonly used in the treatment of COPD and their adverse effects.4,10
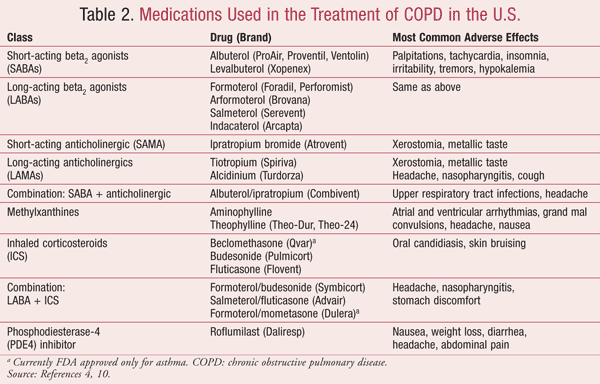
Treatment is not solely dependent on a patient’s spirometry readings. The GOLD guidelines provide a stepwise approach for treatment recommendations based on COPD patient staging (TABLE 3).4 Available treatment options can be categorized as bronchodilators or anti-inflammatory agents.

Bronchodilator Therapy: Bronchodilators are the mainstay of treatment for COPD; they include short- or long-acting anticholinergics (SAMAs or LAMAs) and short- or long-acting beta2 agonists (SABAs or LABAs). Beta2 agonists relax smooth muscle in the airways by stimulating beta2 receptors to increase production of cyclic adenosine monophosphate (cAMP) to promote bronchodilation.10 LABAs and anticholinergics (muscarinic antagonists) are preferred over short-acting formulations.4 Depending on disease severity and patient symptoms, medications may be utilized daily or as needed. Long-acting inhaled bronchodilators reduce the number of exacerbations and related hospitalizations. Most of the treatment options for COPD can be used in combination therapy. If symptoms persist, it is plausible to combine SABAs and LABAs with anticholinergics if symptoms are not controlled by monotherapy.
In 2002, it was estimated that the economic burden of COPD was $32.1 billion.11 A study showed that when treatment followed GOLD guidelines using a combination therapy of a LABA, a long-acting anticholinergic, or inhaled corticosteroids (ICS) to treat moderate-to-severe disease, the cost of COPD management decreased.11 Methylxanthines like theophylline are not recommended due to their adverse-effect profile and narrow therapeutic index, unless bronchodilators are not available or affordable for the patient.
Many patients with COPD also have a concurrent diagnosis of asthma. LABA monotherapy in COPD has not been found to increase respiratory mortality. While there are no restrictions on LABA use in COPD, there is controversy with LABAs as sole therapy for asthma, since concerns have been raised suggesting that its use could lead to an increased risk of respiratory death in asthma patients.12 Based on these findings, it is not recommended to manage patients with COPD and asthma with LABAs alone.
Every patient should ensure that they have quick and easy access to short-acting bronchodilators at all times. These agents have the quickest onset of action and work to improve respiratory symptoms within 15 minutes. Side effects may include increased heart rate, throat irritation, or cough.10 Caution should be advised with regard to storing the medication in a vehicle, especially during warmer months, as some canisters may be pressurized.
Anti-inflammatory Therapy: ICS are used in combination with a long-acting bronchodilator in the management of COPD. There is controversy about the efficacy of ICS in the treatment of COPD, because it is thought that the chronic inflammation is not reversible as compared to asthma. Additionally, the use of ICS has been associated with adverse effects including an increased risk of pneumonia in elderly patients with COPD.13 Oral corticosteroids are often prescribed for COPD exacerbations to shorten recovery time, improve lung function (FEV1) and arterial hypoxemia (PaO2), and reduce the length of hospital stay, the risk of early relapse, and the risk of treatment failure.4 The typical duration of systemic corticosteroid use for acute COPD exacerbations ranges from 10 to 14 days, but new studies have shown that 5 days of treatment may be noninferior to the standard length of therapy.14 Corticosteroids are associated with adverse effects such as glucose intolerance (hyperglycemia), fluid retention, and increased appetite.10
Roflumilast, a phosphodiesterase-4 (PDE4) inhibitor, is an oral medication that inhibits the breakdown of intracellular cAMP to suppress inflammatory activity.10 Roflumilast may be used to decrease exacerbations in patients with chronic bronchitis and severe/very severe COPD.15 It is indicated as adjunct therapy to a long-acting bronchodilator. A medication guide is required to be dispensed with the prescription due to its potential adverse effects including mood disturbances, weight loss, and suicidal ideation.15
Conclusion and Role of the Pharmacist
There are a variety of treatment options available for COPD based on the clinical judgment of the provider to improve symptoms and daily quality of life for each patient. Pharmacists play an important role in educating patients about common adverse effects associated with medication therapy, as well as in providing smoking cessation counseling and vaccine administration. Furthermore, pharmacists can render assistance on proper inhaler technique to promote medication adherence.
REFERENCES
1. Chronic obstructive pulmonary disease (COPD). National
Institutes of Health. 2010.
http://report.nih.gov/nihfactsheets/Pdfs/ChronicObstructivePulmonaryDisease(NHLBI).pdf.
Accessed February 21, 2013.
2. Williams DM, Bourdet SV. Chapter 34. Chronic
obstructive pulmonary disease. In: Talbert RL, DiPiro JT, Matzke GR, et
al, eds. Pharmacotherapy: A Pathophysiologic Approach. 8th ed. New York, NY: McGraw-Hill; 2011. www.accesspharmacy.com/content.aspx?aID=7975888. Accessed March 1, 2013.
3. Chronic obstructive pulmonary disease fact sheet. World
Health Organization. 2012.
www.who.int/mediacentre/factsheets/fs315/en/. Accessed February 20,
2013.
4. Global Initiative for Chronic Obstructive Lung Disease
(GOLD). Global strategy for the diagnosis, management, and prevention of
chronic obstructive pulmonary disease. Updated February 2013.
www.goldcopd.org. Accessed
February 20, 2013.
5. Tuder RM, Petrache I. Pathogenesis of chronic obstructive pulmonary disease. J Clin Invest. 2012;122:2749-2755.
6. Khdour MR, Hawwa AF, Kidney JC, et al. Potential risk
factors for medication non-adherence in patients with chronic
obstructive pulmonary disease (COPD). Eur J Clin Pharmacol. 2012;68:1365-1373.
7. Baillie AJ, Mattick RP, Hall W, Webster P. Meta-analytic review of the efficacy of smoking cessation interventions. Drug Alcohol Rev. 1994;13:157-170.
8. Reid WD, Yamabayashi C, Goodridge D, et al. Exercise
prescription for hospitalized people with chronic obstructive pulmonary
disease and comorbidities: a synthesis of systematic reviews. Int J Chron Obstruc Pulmon Dis. 2012;7:297-320.
9. Sehatzadeh S. Influenza and pneumococcal vaccinations for patients with chronic obstructive pulmonary disease (COPD). Ont Health Technol Assess Ser. 2012;12:1-64.
10. Lexi-Comp. Lexi-Comp Database. http://online.lexi.com/crlsql/servlet/crlonline. Accessed March 14, 2013.
11. Asche CV, Leader S, Plauschinat C, et al. Adherence to
current guidelines for chronic obstructive pulmonary disease (COPD)
among patients treated with combination of long-acting bronchodilators
or inhaled corticosteroids. Int J Chron Obstruct Pulmon Dis. 2012;7:201-209.
12. Tashkin DP, Fabbri LM. Long-acting beta-agonists in
the management of chronic obstructive pulmonary disease: current and
future agents. Medscape. www.medscape.com/viewarticle/732393_1. Accessed June 11, 2013.
13. Thornton Snider J, Lunda Y, Wong KS, et al. Inhaled
corticosteroids and the risk of pneumonia in Medicare patients with
COPD. Curr Med Res Opin. 2012;28:1959-1967.
14. Leuppi JD Schuetz P, Bingisser R, et al. Short-term vs
conventional gluco-corticoid therapy in acute exacerbations of chronic
obstructive pulmonary disease: the REDUCE randomized clinical trial. JAMA. 2013;309:2223-2231.
15. Reid DJ, Pham NT. Roflumilast: a novel treatment for chronic obstructive pulmonary disease. Ann Pharmacother. 2012;46:521-529.
To comment on this article, contact rdavidson@uspharmacist.com.






