US Pharm. 2019;44(3):HS2-HS8.
ABSTRACT: Over the past decade, rates of opioid abuse and overdose have increased dramatically and have received significant national attention. Owing to their knowledge of pharmacokinetics and pharmacology, pharmacists play a vital role in identifying and managing opioid overdose in the hospital setting. Pharmacists should possess sufficient knowledge to recommend nonpharmacologic and pharmacologic patient-specific treatment regimens for opioid overdose in the hospital setting, in addition to identifying and managing acute withdrawal signs and symptoms. In addition, it is critical to account for toxicology and pharmacotherapy alterations in certain populations—such as elderly persons, children, pregnant women, and opioid-dependent patients—during opioid toxicity.
Opioid abuse and overdose have received significant national attention over the past decade and were proclaimed an epidemic by President Donald Trump in September 2018.1 Between 1999 and 2014, prescription opioid sales in the United States quadrupled and drug-overdose deaths tripled; 60% of these deaths were attributed to opioids.2,3 The staggering 15.6% increase in opioid-related deaths that occurred between 2014 and 2015 is attributed to a rise in the use of illicitly manufactured synthetic opioids.2
Pharmacology and Pharmacokinetics
Opioids bind to and activate opioid receptors (mu, kappa, and delta) throughout the body, modulating pain signaling, respiratory rate, and gastrointestinal (GI) motility.4,5 The mu receptor is associated with analgesia, euphoria, respiratory depression, and miosis. The kappa receptor is linked to analgesia, respiratory depression, miosis, and sedation. Delta receptors are involved with euphoria, analgesia, and seizures.4
Opioids typically undergo first-order elimination pharmacokinetics, meaning that a constant fraction of drug is converted over time.4,6 During an overdose, this mechanism is overwhelmed, leading to saturation in which first-order elimination is converted to zero-order elimination. In zero-order elimination, small increases in the dose of a medication lead to disproportionate increases in plasma concentrations, and a constant amount of drug—rather than a constant fraction—is eliminated over time. These characteristics of zero-order elimination pharmacokinetics lead to the toxicokinetic effects that occur with opioid toxicity and render the traditionally recognized pharmacokinetic properties of various opioid formulations largely irrelevant during overdose. Additionally, patient-specific factors may alternatively affect opioid absorption, distribution, metabolism, and elimination during overdose. For example, a large-ingestion-quantity overdose may lead to erratic absorption because of bezoar formation and slowed GI motility (which prolongs drug absorption), and drug misuse (e.g., heating analgesic patches, applying multiple analgesic patches, crushing extended-release tablets, injecting crushed oral dosage forms) may increase the rate of drug absorption and distribution.
Clinical Presentation
Respiratory depression (i.e., respiratory rate <12 breaths/minute or apnea in the absence of physiological sleep) and oxygen saturation <90% on room air are suggestive of opioid toxicity, particularly when they occur in conjunction with stupor and/or miosis.4,6 Decreased peristalsis following opioid-receptor activation in the gut may lead to hypoactive or absent bowel sounds. Less commonly, patients in a prolonged motionless state may present with rhabdomyolysis and subsequent myoglobinuric renal failure or with compartment syndrome caused by compressed fascia-bound muscle groups. If the patient’s stupor has left him or her exposed to the environment, hypothermia may be present as well. The onset of such signs and symptoms may be delayed if the patient has ingested or applied long-acting opioid formulations. The patient should be promptly undressed and searched for fentanyl patches to ensure that further intoxication ceases upon removal.
Polysubstance intoxications are frequent and may influence the presence of typical opioid-toxicity signs and symptoms. Either mydriasis or normoreactive pupils and seizures may occur with concomitant meperidine and tramadol intoxication.4 Concomitant intoxication with antipsychotics, ethanol, anticonvulsants, and sedative hypnotics may further exaggerate the respiratory depression associated with opioid overdose.
Owing to the availability of combination opioid-nonopioid formulations (e.g., acetaminophen and hydrocodone), it is wise to assess the patient for toxicity of potential nonopioid products.4 Acetaminophen overdose or ethanol intoxication may present with elevated aminotransferases or hepatic failure. It is important to remember that early acetaminophen toxicity is frequently undetectable and that subsequent testing of serum acetaminophen levels may be warranted.
Goals of Care
Initial management of opioid toxicity involves maintaining adequate oxygenation through ventilation (respiratory rate >12 breaths per minute and oxygen saturation >90%).6 Subsequent care focuses on identifying and treating coingestants, treating withdrawal symptoms, and performing psychosocial interventions to treat opioid addiction and cope with withdrawal.
Acute Management
Nonpharmacologic Management: Initial management of an opioid overdose should encompass support for the patient’s airway, breathing, and circulation.4 In patients with apnea or a respiratory rate <12 breaths per minute, the airway should be opened via the jaw-thrust or chin-lift technique, followed by oxygenation and ventilation with a bag-valve mask or endotracheal intubation, if needed.7 If breathing and mental status do not improve, naloxone should be administered by any appropriate route available.6,8
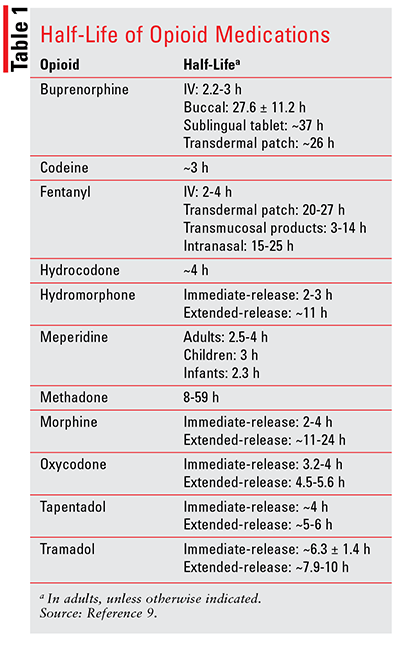
Naloxone: Naloxone is a competitive, short-acting opioid receptor antagonist used for the reversal of opioid overdose.9 This agent is considered first-line treatment for opioid overdose and is indicated for complete or partial reversal of opioid effects induced by natural or synthetic opioids, including respiratory depression.7,9 Naloxone may be administered via the intravenous (IV), intramuscular (IM), subcutaneous (SC), intranasal, endotracheal, or pulmonary route. Orally administered naloxone undergoes significant first-pass metabolism that results in minimal effectiveness; therefore, its use is not recommended during overdose.10 The onset of action for naloxone administered via the endotracheal, IM, and SC routes is 2 to 5 minutes versus approximately 2 minutes, 8 to 13 minutes, and 5 minutes for IV, intranasal, and pulmonary administration, respectively.9 Depending on the route of administration, naloxone’s duration of action ranges from 30 to 120 minutes, a time frame shorter than that for most opioids.4,9 These disparities in duration of action may require the administration of multiple doses of naloxone in order to achieve adequate reversal of opioid overdose. Half-lives of opioid analgesics are presented in TABLE 1.6,9
The specific dose of naloxone required for opioid reversal depends on the amount of opioid ingested, the opioid’s affinity for opioid receptors, and the patient’s weight.9 Unfortunately, most of this information is unknown upon presentation, making empiric dosing necessary. Initial dosing of naloxone in adults is 0.4 mg to 2 mg. If no response is evoked, the dose should be increased every 2 to 3 minutes, to a maximum of 10 mg (TABLE 2).4,6,7,9 If there is no change in respiratory rate after 10 mg of naloxone, other etiologies of respiratory depression must be considered.

The reversal of overdose symptoms after one dose of naloxone is typically transient. Once ventilation is restored, repeated doses of naloxone may be required to maintain an adequate respiratory rate. The presence of recurrent respiratory depression is an indication for continuous naloxone infusion (off-label use).4,9 For naloxone infusion, two-thirds of the total initial dose required to restore breathing every hour should be delivered.9,11 The care of patients who are intoxicated with long-acting or extended-release opioids, have recurrent respiratory depression, or require a naloxone infusion should be managed in the ICU for close monitoring.
Acute Withdrawal Symptoms
Following an opioid-dependent patient’s return to a conscious state, withdrawal symptoms may occur if an opioid is discontinued or dramatically dose-reduced. Furthermore, although naloxone-induced reversal is associated with very few serious side effects, this agent induces signs and symptoms associated with opioid withdrawal.4 These signs and symptoms are unpleasant, but not life-threatening.5,12 Tachycardia, hypertension, hyperventilation, agitation, anxiety, mydriasis, piloerection, and diaphoresis are withdrawal symptoms resulting from a noradrenergic catecholamine surge previously depressed by occupancy of the mu-opioid receptors. Nausea, vomiting, abdominal cramping, and diarrhea may also occur owing to decreased occupancy of mu-opioid receptors in the gut, leading to increased peristalsis. Symptoms typically present within 12 hours of discontinuation of short-acting opioids (e.g., oxycodone, hydrocodone) and resolve within 3 to 5 days.13 Patients dependent on long-acting opioids (e.g., methadone) will demonstrate withdrawal symptoms 30 hours after drug discontinuation, and symptoms will resolve within 10 days.
Multiple symptom-driven opioid-withdrawal scales, such as the Clinical Opiate Withdrawal Scale, have been developed to guide management of withdrawal symptoms based on subjective and objective information in both inpatient and outpatient settings.12,13 Clinicians who employ gradual opioid-agonist tapering or alpha2-adrenergic agonists with nonopioid medications for symptom-specific management can use such scales to assess the effectiveness of opioid-withdrawal symptom management.
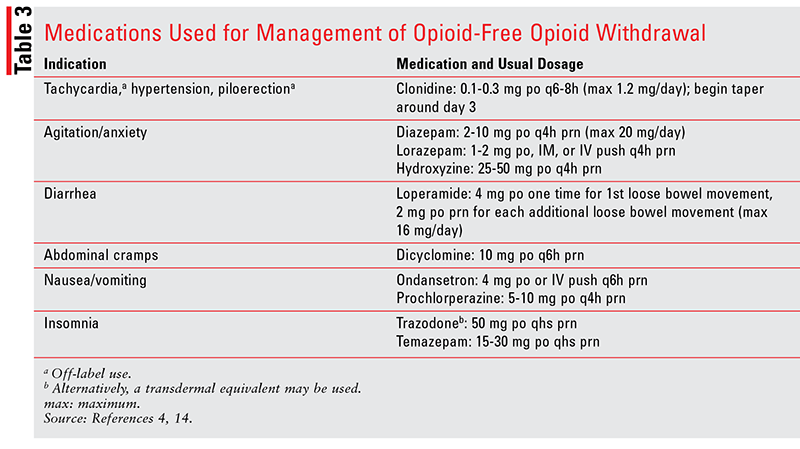
Gradual opioid-agonist tapering is typically attained with methadone or buprenorphine prescribed by specially licensed practitioners.13 Symptom-specific management is achieved with drug classes that target the opposite physiological effects of those that occur when opioids are being used. For example, an alpha2-adrenergic agonist such as clonidine may be used to reduce noradrenergic stimulation of the brain, with use limiting the effects of hypotension.14 Other common nonopioid drugs or classes used in symptom-specific management include benzodiazepines and hydroxyzine for anxiety, loperamide for diarrhea, dicyclomine for abdominal cramping, acetaminophen or other nonopioid analgesics for pain, ondansetron for nausea, and sleep aids (e.g., trazodone) for insomnia (TABLE 3).4,14
Special Populations
Elderly: Elderly patients often present with exaggerated and prolonged effects of opioid toxicity that depend on the comorbid disease state.4 Patients who have an underlying respiratory disorder (e.g., chronic obstructive pulmonary disease, sleep apnea) may experience heightened respiratory depression. Those with renal or cardiac dysfunction may experience drug accumulation or impaired metabolism owing to decreased renal clearance and hepatic metabolism, respectively. Not uncommonly, elderly patients receive higher doses of naloxone than their younger counterparts who ingest the same quantity of opioids, based on these changes in pharmacokinetic and pharmacodynamic parameters.
Children: Compared with adults, children often require a larger naloxone dose for opioid reversal, as they typically ingest a greater opioid dose per kilogram of body weight.4 A bigger dose may also be required in children presenting with profound respiratory depression from tramadol and codeine due to ultrarapid metabolism to their active forms.15 The initial starting dosage of naloxone in children aged younger than 5 years or weighing 20 kg is 0.1 mg/kg/dose IV (preferred route) repeated every 2 to 3 minutes as needed (maximum 2 mg per dose).9 Children aged 5 years and older who weigh >20 kg should receive naloxone 2 mg IV per dose, repeated every 2 to 3 minutes as needed.
Pregnant Patients: Pregnant patients who are experiencing opioid toxicity should be treated with naloxone.16 Naloxone should be administered to reverse maternal opioid overdoses despite the potential of withdrawal induction to contribute to fetal stress.
Opioid-Dependent Patients: Naloxone may be safely administered to patients with opioid dependence. Opioid-dependent patients typically need higher doses of opioids to achieve the same effect, but they require lower doses of naloxone for opioid reversal in order to prevent the development of acute opioid withdrawal (TABLE 2).4,6,7,9 With chronic opioid use, tolerance to analgesic properties develops more quickly than respiratory depression does, thereby increasing the risk of respiratory depression in this patient population despite a perceived lack of analgesic effect.4,7,17
The Pharmacist’s Role
There are numerous crucial roles pharmacists can play in the appropriate care of patients with opioid toxicity in the hospital setting. Pharmacists should recognize that the typical pharmacokinetic properties of various opioid formulations are largely irrelevant during opioid overdose because of changes in variable patient-specific factors affecting absorption, distribution, metabolism, and elimination.4 Pharmacists should employ this knowledge and their understanding of opioids and other potential coingestant mechanisms of action to help determine appropriate diagnostic tests, as well as reversal and treatment methods. Following stabilization of ventilation, pharmacists’ critical function is to recommend appropriate withdrawal treatment with a gradual opioid-agonist taper or nonopioid symptom-specific treatment with medications.
REFERENCES
1. Trump DJ. Presidential proclamation on prescription opioid and heroin epidemic awareness week, 2018. www.whitehouse.gov/presidential-actions/presidential-proclamation-prescription-opioid-heroin-epidemic-awareness-week-2018. Accessed December 15, 2018.
2. Rudd RA, Seth P, David F, Scholl L. Increases in drug and opioid-involved overdose deaths—United States, 2010–2015. MMWR Morb Mortal Wkly Rep. 2016;65(50-51):1445-1452.
3. Burton BN, Lin TC, Said ET, Gabriel RA. National trends and factors associated with inpatient mortality in adult patients with opioid overdose. Anesth Analg. 2019;128(1):152-160.
4. Boyer EW. Management of opioid analgesic overdose. N Engl J Med. 2012;367(2):146-155.
5. McDonald J, Lambert DG. Opioid receptors. Continuing Education Anaesth Crit Care Pain. 2005;5:22-25.
6. Parthvi R, Agrawal A, Khanijo S, et al. Acute opiate overdose: an update on management strategies in emergency department and critical care unit. Am J Ther. 2017 Sept 13 [Epub ahead of print].
7. Cumpston KL, Wiggins JC, Mlodzinski S, et al. Update on current treatment of acute opioid overdose. Curr Treat Options Psychiatry. 2018;5(3):301-312.
8. Mills CA, Flacke JW, Flacke WE, et al. Narcotic reversal in hypercapnic dogs: comparison of naloxone and nalbuphine. Can J Anaesth. 1990;37(2):238-244.
9. Lexi-Drugs [online database]. Riverwoods, IL: Lexi-Comp, Inc. http://online.lexi.com. Accessed December 7, 2018.
10. Rzasa Lynn R, Galinkin JL. Naloxone dosage for opioid reversal: current evidence and clinical implications. Ther Adv Drug Saf. 2018;9(1):63-88.
11. Goldfrank L, Weisman RS, Errick JK, Lo MW. A dosing nomogram for continuous infusion intravenous naloxone. Ann Emerg Med. 1986;15(5):566-570.
12. Wesson DR, Ling W. The clinical opiate withdrawal scale (COWS). J Psychoactive Drugs. 2003;35(2):253-259.
13. Kampman K, Jarvis M. American Society of Addiction Medicine (ASAM) national practice guideline for the use of medications in the treatment of addiction involving opioid use. J Addict Med. 2015;9(5):358-367.
14. Gowing L, Farrell M, Ali R, White JM. Alpha2-adrenergic agonists for the management of opioid withdrawal. Cochrane Database Syst Rev. 2016;3(5):CD002024.
15. FDA. FDA Drug Safety Communication: FDA restricts use of prescription codeine pain and cough medicines and tramadol pain medicines in children; recommends against use in breastfeeding women. www.fda.gov/Drugs/DrugSafety/ucm549679.htm. Accessed January 23, 2019.
16. American College of Obstetricians and Gynecologists. ACOG committee opinion no. 711: opioid use and opioid use disorder in pregnancy. Washington, DC: American College of Obstetricians and Gynecologists; August 2017.
17. White JM, Irvine RJ. Mechanism of fatal opioid overdose. Addiction. 1999;94(7):961-972.
To comment on this article, contact rdavidson@uspharmacist.com.






