US Pharm. 2023;48(8):8-12.
ABSTRACT: Since pain varies in its etiology, degree of severity, and duration, its management warrants an individualized approach to treatment. Research has indicated that pain management in the pediatric patient population often presents clinicians with various challenges. Moreover, it is not always adequately assessed and treated, and this may result in long-term and short-term adverse effects, including exacerbation of pain, anxiety, and fear. Accurately assessing pain is an integral component of pain management, and clinicians should be familiar with the recommended pain-assessment tools commonly employed and be able to identify and address barriers to effective pain management. Treatment plans often warrant a multimodal approach that may include pharmacologic and nonpharmacologic measures tailored to patient needs. As members of the multidisciplinary team of clinicians involved in pain management, pharmacists can be instrumental in patient care by making clinical recommendations based on guidelines to provide safe and effective pain management, improve clinical outcomes, and diminish or prevent adverse events in pediatric patients.
The International Association for the Study of Pain (IASP) defines pain as “an unpleasant sensory and emotional experience that arises from actual or potential tissue damage.”1-3 Pain is considered one of the most common symptoms for which individuals from all age groups seek medical care; however, various studies have indicated that pain is often underestimated and not adequately managed among the pediatric patient population.2-4 According to the World Health Organization (WHO) Guidelines on the Management of Chronic Pain in Children, the management of pain in pediatric patients can be challenging and multifaceted, and there is a lack of high-quality research studies with regard to optimal treatment interventions and management approaches in this patient population.5 Pain management entails a patient-centered approach involving pharmacologic and nonpharmacologic measures tailored to patient needs.5
Incidence of Pediatric Pain
Various publications have demonstrated that pediatric pain is often undetected and not always adequately treated. Additionally, pain can be complex and affects everyone differently; however, it may be challenging to assess and manage pain in pediatric patients—especially in very young patients—since they are unable to verbalize/articulate their pain.
The exact incidence of pain among pediatric patients is unknown; however, according to the Emergency Medicine Residents’ Association, among pediatric patients, pain accounts for an estimated 78% of emergency department (ED) visits, including episodic, acute, or exacerbations of chronic pain.6 The IASP indicates that, globally, chronic pain affects approximately 20% to 35% of pediatric patients.7
A recent publication in Practical Pain Management indicated that an estimated 33% to 82% of hospitalized pediatric patients experience moderate-to-severe pain, especially post surgery, and an estimated 20% of those patients do not obtain adequate pain relief, which may result in chronic pain.8 The authors also indicated that the incidence of unreported pain remains unknown, but this may be the result of various patient and/or parent/caregiver factors, including a lack of awareness about pain-management strategies, apprehension regarding unnecessary medications and adverse effects (AEs), and fear of injectable analgesics.8
Examples of some of the most commonly cited reasons for ED visits attributed to pediatric pain include musculoskeletal injuries, abdominal pain, sore throat, otalgia, and headaches.6 Pain in pediatric patients also occurs in those who have undergone surgery, those with neuropathic pain, and those with chronic conditions such as sickle cell disease (SCD), cancer, juvenile arthritis, fibromyalgia, and inflammatory bowel disease.6,7
In a recent report in the Journal of the American College of Emergency Physicians Open, the authors noted that untreated pain may have numerous consequences, including physical, emotional, and psychological issues.4 Unmanaged pain can affect patient productivity, academic performance, day-to-day activities and social activities with others, and it may cause sleep disturbances, depending upon age.4
Multiple barriers to effective pain management in the pediatric patient population, especially in the hospital setting, have been documented in the literature, including difficulty evaluating pain in pediatric patients, inadequate or insufficient prescriber medication orders to meet the needs of pediatric patients, lack of time to administer analgesics before procedures, unawareness and/or underreporting of pain by parents/caregivers, and lack of knowledge about pain management for pediatric patients.9
The American Academy of Pediatrics (AAP) notes that examples of barriers to providing adequate pain control to pediatric patients include challenges in accurately assessing pain, particularly in patients unable to verbalize information about their pain, lack of awareness about pain-assessment tools for pediatric pain, and fear of AEs, including respiratory depression or addiction.2,3
Assessing Pain in Pediatric Patients
According to a Pain Management Best Practices Inter-Agency Task Force report, there are unique issues and challenges in managing pain in the pediatric patient population.10 Moreover, poor pain management may correlate with an expanded incidence of chronic pain and augment the risk for persistent pain and increased impairment into adulthood.10 The task force also noted that the integration of a patient-centered approach involving parents and family in the management of pain is critical since both family and parental factors can influence pain in pediatric patients, and appropriate pain management in childhood is imperative because pain experiences during childhood can affect how they perceive and handle pain in adulthood.10
According to the AAP, the underutilization of evaluation tools designed for pain assessment in pediatric patients based on the developmental stage of the patient often results in inadequate assessment of pain.11 Moreover, establishing the nature of the pain provides clinicians with valuable information that enables them to implement an optimal pain-management approach tailored to patient needs, and clinical interventions should be centered on the age and developmental stage of the patient.4
The AAP notes that, in general, the goals of assessing pain in pediatric patients include identifying the etiology of the pain; determining the degree of severity, duration, and aggravating and alleviating factors to pain; and evaluating the response to therapy once initiated. Clinicians should understand that it is critical to employ pain-assessment tools appropriate for the patient’s age to obtain the necessary information to establish the optimal pain-management plan. The AAP specifies two types of tools often employed to assess pain in pediatric patients: self-reporting and observational-behavioral scales in patients who cannot self-report their pain.2,3 Clinicians can also evaluate pain by monitoring certain biological responses such as heart rate, blood pressure, transcutaneous oxygen, sweating, and stress response.12 It is important to note that the dependability of pain assessment expands with age and the child’s cognitive ability.2,3
The AAP also notes that self-report measures are contingent upon the patient’s ability to measure and verbally describe the location and degree of pain.2,3 Literature indicates that pediatric patients aged as young as 3 years may be proficient in quantifying and interpreting pain using a visual representation.2,3,13 Globally, the Wong-Baker FACES and the Faces Pain Scale–Revised (FPS-R) are commonly employed methods for assessing pain in pediatric patients that entail the use of a visual analogue of pain scales centered upon a sequence of faces displaying an increase in distress or pain with a rating of 0 to 10, indicating zero pain to intense pain, respectively.2,3,13-15 According to the IASP, the FPS-R is an easy-to-administer tool for pediatric patients and requires no special equipment other than a copy of the scale.15 The IASP also notes that numerical self-rating scales (0-10) can be employed in pediatric patients aged older than 8 years, and behavioral-observation scales are required for those unable to provide a self-report.14,15 A depiction of the FPS-R can be found on the IASP website: www.iasp-pain.org/resources/faces-pain-scale-revised.
According to a recent publication by the AAP, examples of frequently employed and validated observational pain scales include the FLACC (Face, Legs, Activity, Cry, Consolability; or revised FLACC [FLACC-R]), Neonatal Infant Pain Scale, and CRIES (C-crying, R-requires increased oxygen, I-increased vital signs, E-expression, S-sleeplessness); see TABLE 1.2,3,16-19
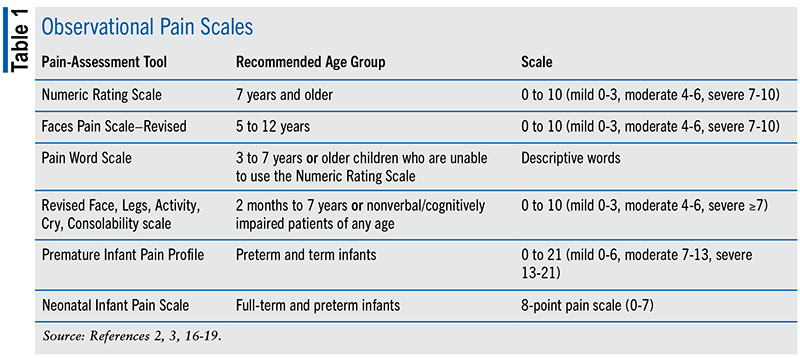
In addition to the information obtained from the use of one of the tools mentioned above, clinicians should also obtain information from the parents/caregivers, and pain should be routinely assessed.19
Guidelines for Management of Pediatric Pain
The AAP indicates that the practices for the management of pediatric pain may not be evidence-based since most pharmacologic agents are utilized off-label and depend on the extrapolation of data from studies involving adults.2,3 A summary of the recommendations from the AAP regarding the management of pediatric pain include the following:
• The AAP recommends that prescribers employ pediatric-specific, evidence-based methods whenever feasible.
• Consult pain-management experts early, especially if the use of opioids is warranted.
• For pediatric patients, nonpharmacologic measures, including relaxation and breathing exercises, guided imagery, biofeedback, massage, or distraction (e.g., art, pet, play, or music therapy), can significantly decrease the need for pharmacologic pain management.
• When feasible, employ the least painful routes of administration (e.g., oral, transdermal, topical, and intranasal routes), while avoiding IM and rectal medications.
• When devising a treatment plan, employ a stepwise approach, and when no contraindications are present, initiate therapy with nonopioid agents and increase to opioids as indicated based on the severity of the pain. Moreover, the AAP states, “Less medication is required to prevent pain than to eliminate it. Therefore, initially, use as much medication as necessary to achieve pain control, then dose as frequently as needed to maintain adequate analgesia.”
• Conduct routine pain evaluations to assess the patient’s pain and the therapeutic effects of the selected treatment.
• Remember that in patients previously treated for pain, such as those with advanced cancer or SCD, there may be a need for dose adjustments and adjunctive therapies to manage pain.
• When feasible, prescribe scheduled or long-acting medications to manage long-term pain and immediate-release analgesic formulations to manage incidental or breakthrough pain episodes.2,3
WHO Guidelines
In December 2020, the WHO issued guidelines for managing chronic pain in pediatric patients.6 The updated guidelines emphasize the significance of physical, psychological, and pharmacologic interventions for managing primary and secondary chronic pain in children aged 0 to 19 years.6 These guidelines recognize that pain is a multifaceted issue that is an intricate interaction of biological, psychological, and social factors; therefore, pain management, in turn, necessitates a multimodal, interdisciplinary approach. The guidelines address the issue of opioid abuse and provide tips that prescribers can employ to encourage appropriate opioid stewardship for pediatric patients with chronic pain, which was not included in the previous guidance.6 More information can be found at www.who.int/publications/i/item/9789240017870.
Management of Pain
A recent article in the Journal of the American College of Emergency Physicians Open indicated that due to the current opioid crisis, prescribers should be familiar with both pharmacologic and nonpharmacologic approaches for pain management and with identifying and addressing fear and anxiety in pediatric patients that could enhance clinical outcomes.4
Optimal pain management warrants an accurate assessment of pain, reviews should be conducted routinely, and changes to therapy should be implemented when necessary. It has been well established that effective pain management warrants an individualized approach that may involve the implementation of pharmacologic and nonpharmacologic measures depending on the etiology, duration, and severity of the pain. Managing pain in the pediatric patient population generally includes reducing, controlling, and preventing pain episodes while minimizing AEs.
Nonpharmacologic Measures
Examples of nonpharmacologic measures for pain management include the following:
• Physical measures: heat and cold therapy, acupuncture, massage, exercise, and physical therapy
• Behavioral measures: biofeedback, relaxation techniques, and art and play therapy tailored to the patient’s age and developmental stage
• Cognitive measures: using age-appropriate video games, virtual reality, and imagery
• Examples of other recommended nonpharmacologic measures include pacifiers and swaddle blankets for infants, providing a calm and relaxing environment, and emotional support from loved ones.2,3,12,19-21
Pharmacologic Measures
With regard to pharmacologic measures, the selection of therapy should be individualized and based on the patient’s age, and allergy, medical, and medication history. Additional factors that may be considered include the patient’s response to previous analgesics, if applicable, route of administration, frequency, and type and degree of pain. It is critical to evaluate pain routinely and modify treatment plans when warranted. When no contraindications are present, pain is frequently managed with acetaminophen and nonsteroidal anti-inflammatory drugs (NSAIDs). Clinical data show that both have demonstrated efficacy and safety and are cost-effective analgesics.12,19 Literature indicates that ibuprofen is one of the most commonly used NSAID in infants and children for pain relief.12,19 Both NSAIDs and acetaminophen have been revealed to have noninferior analgesic effects when compared with opioids for acute pain.18,22,23 Comparable findings have been demonstrated when NSAIDs were compared with opioids for managing postfracture pain in children.24 A review demonstrated that the analgesic effects of NSAIDs had equivalent efficacy to opioids when treating musculoskeletal pain.25 In addition, studies have demonstrated that NSAIDs have noninferior analgesic effects and result in better functional outcomes and fewer AEs than opioid analgesics.4,25,26 Moreover, opioids such as morphine and oxycodone, as well as topical analgesics, are often prescribed when appropriate, and adjuvant medications, such as antidepressants and anticonvulsant agents, are prescribed for persistent nerve pain.
When no contraindications are present, mild pain can generally be adequately treated with acetaminophen and NSAIDs, and moderate-to-severe pain is generally treated with opioid agents, often in combination with nonopioid analgesics.27 Literature indicates that NSAIDs may offer numerous advantages, since this class of drugs is effective in diminishing the incidence of pain and inflammation and has the potential to generate adequate pain relief while reducing overall opioid requirements and associated AEs.27,28 Clinicians should monitor patients for the adverse drug reactions commonly associated with the use of NSAIDs, including diarrhea, headache, nausea, constipation, rash, dizziness, and abdominal pain.
Patient-Controlled Analgesia
The AAP notes that patient-controlled analgesia (PCA) is the safest technique for administering IV opioids such as morphine, fentanyl, or hydromorphone.2,3 Examples of when PCA with continuous infusion is prescribed for pain management include vaso-occlusive episodes in a patient with SCD, severe postoperative pain, cancer-related pain, or when goals of care have changed to principally palliative care and routine close monitoring of patients is recommended.2,3
Recent Clinical Studies
In a recent publication in Pediatric Drugs, the authors summarized the available clinical data regarding the efficacy and safety of NSAIDs used to treat pain in infants (children aged younger than 2 years). The authors stated that initial therapy should entail using the lowest age-appropriate or weight-based dose to enhance the safety of NSAIDs in infants.29 Extent of treatment and dosage should be routinely assessed, and proper dosing and use should align with the manufacturer’s recommendations. They also stated that therapy for nonchronic pain should be as brief as possible, and patients treated for chronic pain should be routinely assessed for AEs associated with NSAIDs.29
A cross-sectional study published in BMC Pediatrics indicated that there is still a need to advance pain management in pediatric patients, and patients should be evaluated for pain while at rest and during movement to obtain a complete representation of the pain experienced.30 They also noted that response to treatment should be monitored routinely to thwart pain undertreatment, and nonpharmacologic methods are a valuable component of a pain management strategy.30
In a publication in Pediatric Blood & Cancer, researchers assessed the efficacy of nonpharmacologic measures in diminishing pain related to SCD. They discovered that nonpharmacologic measures may be effective in decreasing pain. Cognitive behavioral therapy and biofeedback meaningfully diminished the incidence and/or intensity of SCD-related pain in outpatient settings, while virtual reality and yoga significantly reduced pain in in-patient settings. Biofeedback also drastically diminished the need for analgesics.31
Conclusion
Numerous strategies are recommended for managing pain in the pediatric patient population, depending upon the type of pain, severity, and duration. Effectively assessing and managing pain in pediatric patients warrants a multidisciplinary approach involving nonpharmacologic and pharmacologic measures. Pharmacists are well poised to make clinical recommendations that address the pediatric patient’s needs by ensuring proper use of medications, including nonprescription analgesics, individualizing pain-management plans, and conducting periodic medication reviews that have the potential to optimize pain relief, improve clinical outcomes, and minimize and/or prevent AEs. Pharmacists can aid patients and parents/caregivers via pain and medication education, collaborating with other healthcare providers, screening for potential drug-drug interactions and contraindications, routinely assessing patient response, and recommending therapy modifications when warranted. Pharmacists can also direct parents/caregivers to seek medical care from their pediatricians if pain relief is not attained after using nonprescription analgesics.
REFERENCES
1. Raja SN, Carr DB, Cohen M, et al. The revised International Association for the Study of Pain definition of pain: concepts, challenges, and compromises. Pain. 2020;161(9):1976-1982.2. Kaufman D, Villacreas S. Pain management. In: Gershel JC, Rauch DA, eds. Caring for the Hospitalized Child: A Handbook of Inpatient Pediatrics. 2nd ed. American Academy of Pediatrics Section on Hospital Medicine; January 2018.
3. Dadwani A, Shanley LA. Pain management. In: Gershel JC, Rauch DA, eds. Caring for the Hospitalized Child: A Handbook of Inpatient Pediatrics. 3rd ed. American Academy of Pediatrics Section on Hospital Medicine; May 2023.4. Chumpitazi CE, Chang C, Atanelov Z, et al. Managing acute pain in children presenting to the emergency department without opioids. J Am Coll Emerg Physicians Open. 2022;3(2):e12664.
5. World Health Organization. Guidelines on the management of chronic pain in children. December 22, 2020. www.who.int/publications/i/item/9789240017870. Accessed July 10, 2023.6. Webb T, Sanders J. Pediatric pain. In: Cisewski DH, Motov SM, eds. Pain Management Guide. 1st ed. Emergency Medicine Residents’ Association; 2020.
7. International Association for the Study of Pain. Pain in children: management. July 9, 2021. www.iasp-pain.org/resources/factsheets/pain-in-children-management/. Accessed July 10, 2023.8. Abiezze C, Ranaraja A, Kilano R, et al. Pediatric pain management: a review of clinical diagnosis and management. Pract Pain Manag. 2020;20(3).
9. Czarnecki ML, Guastello A, Turner HN, et al. Barriers to pediatric pain management: a brief report of results from a multisite study. Pain Manag Nurs. 2019;20(4):305-308.10. Cheng J, Rutherford M, Singh VM. The HHS Pain Management Best Practices Inter-Agency Task Force report calls for patient-centered and individualized care. Pain Med. 2020;21(1):1-3.
11. Fein JA, Zempsky WT, Cravero JP. Relief of pain and anxiety in pediatric patients in emergency medical systems. Pediatrics. 2012;130(5):e1391-e1405.12. American Academy of Pediatric Dentistry. Pain management in infants, children, adolescents, and individuals with special health care needs. In: The Reference Manual of Pediatric Dentistry. Chicago, IL: American Academy of Pediatric Dentistry. 2022:392-400.
13. Hicks CL, von Baeyer CL, Spafford P, et al. The Faces Pain Scale—Revised: toward a common metric in pediatric pain measurement. Pain. 2001;93:173-183.14. International Association for the Study of Pain. Faces Pain Scale−Revised. www.iasp-pain.org/resources/faces-pain-scalerevised/#references. Accessed July 10, 2023.
15. Breivik H, Borchgrevink PC, Allen SM, et al. Assessment of pain. Br J Anaesth. 2008;101(1):17-24.16. Malviya S, Voepel-Lewis T, Burke C, et al. The revised FLACC observational pain tool: improved reliability and validity for pain assessment in children with cognitive impairment. Pediatr Anaesth. 2006;16(3):258-265.
17. Stevens BJ, Gibbins S, Yamada J, et al. The Premature Infant Pain Profile−Revised (PIPP-R): initial validation and feasibility. Clin J Pain. 2014;30(3):238-243.18. Hicks CL, von Baeyer CL, Spafford PA, et al. The Faces Pain Scale−Revised: toward a common metric in pediatric pain measurement. Pain. 2001;93(2):173-183.
19. Gai N, Naser B, Hanley J, et al. A practical guide to acute pain management in children. J Anesth. 2020;34(3):421-433.20. Drugs.com. Non-pharmacological pain management therapies for children. July 3, 2023. www.drugs.com/cg/non-pharmacological-pain-management-therapies-for-children.html. Accessed July 10, 2023.
21. Thrane SE, Wanless S, Cohen SM, Danford CA. The assessment and non-pharmacologic treatment of procedural pain from infancy to school age through a developmental lens: a synthesis of evidence with recommendations. J Pediatr Nurs. 2016;31(1):e23-e32.22. Kelley-Quon LI, Kirkpatrick MG, Ricca RL, et al. Guidelines for opioid prescribing in children and adolescents after surgery: an expert panel opinion. JAMA Surg. 2021;156(1):76-90.
23. Koh SWC, Li CF, Loh JSP, et al. Managing tooth pain in general practice. Singapore Med J. 2019;60(5):413.24. Stovitz SD, Johnson RJ. NSAIDs and musculoskeletal treatment: what is the clinical evidence? Phys Sportsmed. 2003;31(1):35-52.
25. Chang AK, Bijur PE, Esses D, et al. Effect of a single dose of oral opioid and nonopioid analgesics on acute extremity pain in the emergency department: a randomized clinical trial. JAMA. 2017;318(17):1661-1667.26. Le May S, Ali S, Khadra C, et al. Pain management of pediatric musculoskeletal injury in the emergency department: a systematic review. Pain Res Manag. 2016;2016:4809394.
27. Cooney MF. Pain management in children: NSAID use in the perioperative and emergency department settings. Paediatr Drugs. 2021;23(4):361-372.28. Wong I, St. John-Green C, Walker SM. Opioid-sparing effects of perioperative paracetamol and nonsteroidal anti-inflammatory drugs (NSAIDs) in children. Paediatr Anaesth. 2013;23(6):475-495.
29. Ziesenitz VC, Welzel T, van Dyk M, et al. Efficacy and safety of NSAIDs in infants: a comprehensive review of the literature of the past 20 years. Paediatr Drugs. 2022;24(6):603-655.30. Andersson V, Bergman S, Henoch I, et al. Pain and pain management in children and adolescents receiving hospital care: a cross-sectional study from Sweden. BMC Pediatr. 2022;22(1):252.
31. van Veelen S, Vuong C, Gerritsma JJ, et al. Efficacy of non-pharmacological interventions to reduce pain in children with sickle cell disease: a systematic review. Pediatr Blood Cancer. 2023;70(6):e30315.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.






