US Pharm. 2021;46(5):23-27.
ABSTRACT: Anxiety disorders, which are the most common psychiatric illnesses, often go undiagnosed or undertreated. Social anxiety disorder (SAD) involves the persistent, intense fear of being observed or judged in social situations, such as public speaking or interactive settings, and affects a person’s quality of life by impacting relationships, work or school, and social activities. Common comorbidities in patients with SAD include cardiovascular, neurologic, gastrointestinal, respiratory, autoimmune, and endocrine disorders. Psychological and pharmacologic approaches are used to treat SAD. It is important to consider treatment guidelines and patient-related factors in choosing the best therapy for a patient with SAD, and pharmacists’ comprehensive knowledge of drugs and ability to evaluate drug therapy are essential in treatment management.
Anxiety disorders are the most common psychiatric illnesses, with up to 33.7% of the population experiencing an anxiety disorder during the lifetime, but they often go undiagnosed or undertreated.1 In persons aged 18 years and older, the 1-year prevalence rate for anxiety disorders is 21.3%, and that for social anxiety disorder (SAD) is 8.0%.2 SAD, which affects more women than men, typically begins in childhood or adolescence but occasionally develops later in life.3 SAD involves the persistent, intense fear of being observed in social situations, such as performance or interactive settings.4 A typical example is public speaking, which often provokes fear of scrutiny or judgment by others.2 SAD affects a person’s quality of life by impacting social activities, relationships, work, or academic studies.5 There is no definitive cause for SAD, but researchers believe that a genetic component—with several plausible candidate genes—may be responsible.2
Several self-screening instruments are used as diagnostic aids, along with the criteria listed in the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5).6 The previous edition (DSM-IV) replaced the term “social phobia” with “social anxiety disorder” to differentiate SAD from other specific phobias, and SAD became the primary term when DSM-5 was published in 2013.6-8 DSM-5 also included a “performance-only” specifier instead of the “generalized” specifier in DSM-IV.7,8 This change has helped clarify diagnosis because performance-only SAD has distinct symptoms.7,9 Additionally, for clinical diagnosis of SAD, the patient must have experienced persistent fear (lasting at least 6 months) in one or more social or performance situations (i.e., activity leads to intense fear of humiliating oneself in public).10 However, before a diagnosis is made, the healthcare professional should conduct a differential diagnosis to rule out mental or somatic symptom disorders and certain physical illnesses.11 Various therapeutic options are available for anxiety disorders, including psychotherapy and pharmacotherapy.11
Pathophysiology
The limbic-paralimbic system in the brain contains several structures, including the amygdala, locus coeruleus, hippocampus, and hypothalamus, that are responsible for emotional processing and play a pivotal role in anxiety disorders.12-14 Heightened activity in these structures alters their functions.15 The role of the amygdala is to assess fearful or threatening stimuli, whereas the locus coeruleus signals the neurotransmitter norepinephrine, leading to release of the hormone.14 When the norepinephrine is released, critical parts of the autonomic nervous system are activated, leading to mood, cognition, and sleep adjustments as well as elevated heart rate and other hyperarousal symptoms.12,15 Traumatic memories and fear conditioning are housed in the hippocampus, and the hypothalamus mediates stressful occurrences.12,14 Neurotransmitters such as norepinephrine, dopamine, and serotonin are vital to the pathophysiology of anxiety.12,15 Patients who have SAD are likely to present with decreased serotonin, decreased dopamine, and increased glutamate.13,14 Pharmacologic agents used to treat SAD have mechanisms that act to regulate these neurotransmitters.12
Treatment
According to the National Institute of Health and Clinical Excellence (NICE) guidelines for SAD, treatment includes psychological and pharmacologic options.6 The psychological intervention termed cognitive-behavioral therapy (CBT) is used to help patients face barriers directly through exposure techniques, relaxation techniques, and training in social and conversational skills. It is recommended that CBT be implemented ahead of pharmacologic therapy; however, some patients may decline it based on personal preference.6 Patients who manage their symptoms with psychological and pharmacologic treatments are more likely to achieve continued symptom-improvement benefits.3
Before pharmacologic agents are initiated, treatment options, expected outcomes, and possible adverse effects (AEs) of medications should be discussed with the patient.6 Following initiation, it is necessary to monitor treatment frequently in order to assess efficacy.6 Once the patient attains the desired therapeutic response, the medication should be continued for at least 12 months in order to prevent relapse.11 Selective serotonin reuptake inhibitors (SSRIs), serotonin-norepinephrine reuptake inhibitors (SNRIs), monoamine oxidase inhibitors (MAOIs), gamma-aminobutyric acid (GABA)ergic drugs, benzodiazepines (BZDs), beta-blockers, and other anxiolytics are the standard drug classes used to treat SAD (TABLES 1 and 2).1
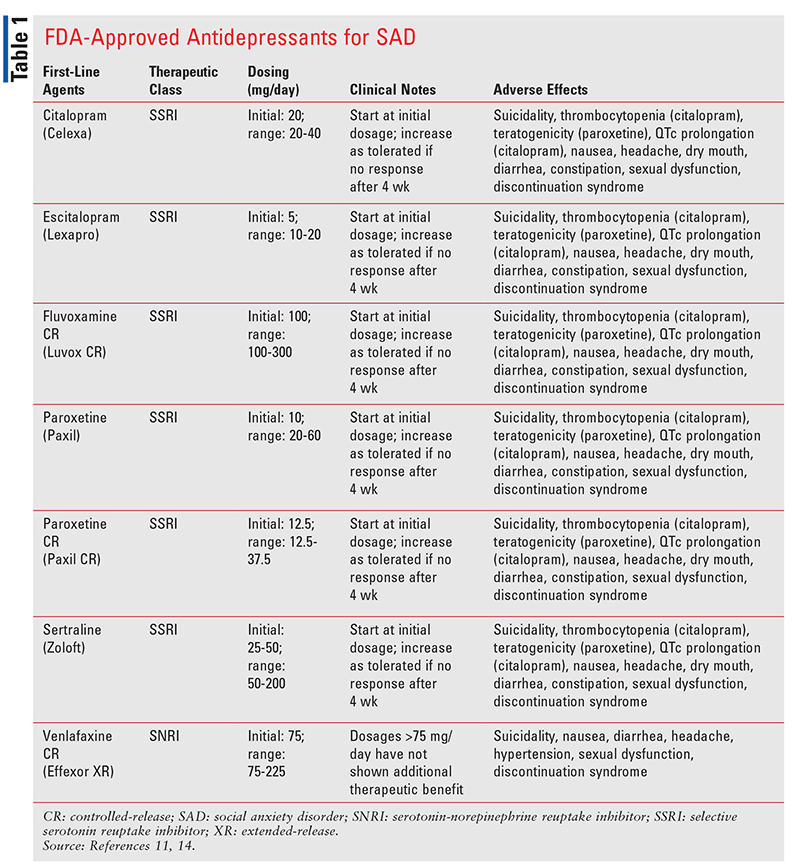
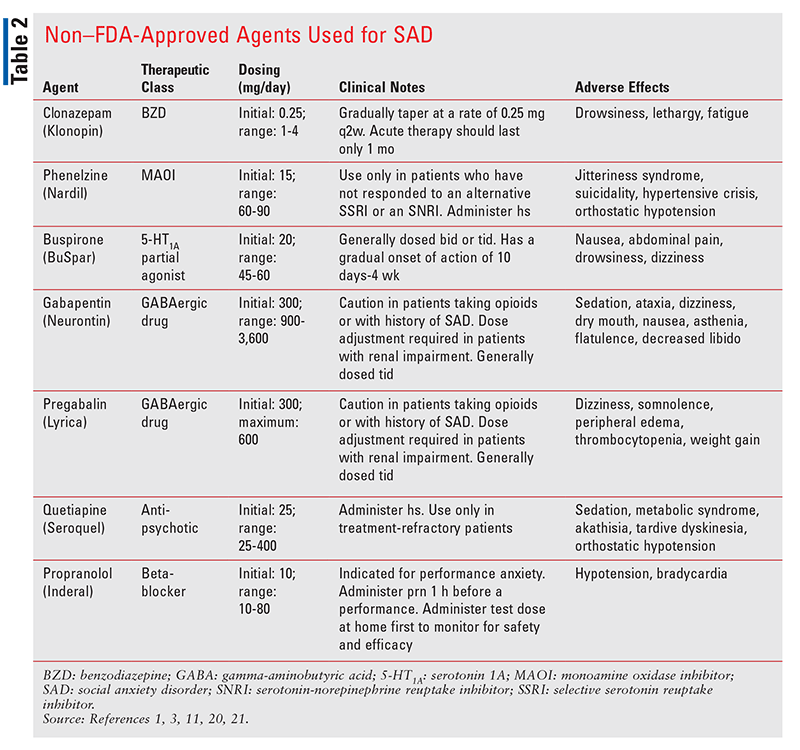
SSRIs: SSRIs, which are first-line agents for SAD treatment, work by elevating the patient’s serotonin level, ultimately leading to regulated mood and improved mental well-being.1,3,16 Sertraline, paroxetine, and fluvoxamine are the FDA-approved SSRIs for SAD, and fluoxetine, citalopram, and escitalopram have been used off-label.1,17 Research has found no superior agent among SSRIs; however, paroxetine and sertraline effectively prevented relapse compared with placebo.1,18 Furthermore, paroxetine and fluvoxamine were superior to placebo for long-term treatment (24 months or longer).18 It may take up to 6 weeks to see symptom improvement with SSRIs.11 Some patients may experience increased anxiety or jitteriness during the first 2 weeks of therapy.1,11 Historically, SSRIs are the most widely used antidepressant class owing to more tolerable and shorter-lasting AEs than other classes.1 To prevent withdrawal symptoms, an SSRI should not be discontinued abruptly; instead, the dosage should be slowly decreased on a monthly basis once it has been decided to discontinue the agent.11,14
SNRIs: Venlafaxine is an SNRI approved for first-line treatment of SAD.17 SNRIs work similarly to SSRIs; however, with SNRIs, concentrations of both serotonin and norepinephrine are increased.19 In studies, venlafaxine was superior to placebo in reducing total SAD symptom severity.18 Head-to-head trials have not found one agent to be more effective than another.20 One trial investigating the efficacy of venlafaxine and paroxetine concluded that these agents had similar response rates and were significantly superior to placebo.5 Venlafaxine also has a latency period for its anxiolytic effect.11
BZDs: BZDs are frequently prescribed for SAD and other anxiety disorders in the United States.11 These agents work by enhancing affinity to GABA type A receptors, which produces a calming effect in the brain.21 Unlike SSRIs and SNRIs, the anxiolytic effect of BZDs begins shortly after administration.11 Although BZDs have a quick onset of action, long-term treatment is not recommended because of the potential for abuse.14 Research has demonstrated that BZDs are effective for reducing symptoms of SAD.18 Additionally, a Cochrane review concluded that clonazepam and bromazepam were superior to placebo in lessening associated disability on the work and social adjustment subscale.18 According to the NICE guidelines, BZDs are not recommended as first-line therapy for SAD; however, they can be used in combination with an SSRI or SNRI during the latency period for the latter agents’ anxiolytic effect.6,11 To prevent dependency, BZDs should be avoided in patients with a history of substance abuse.11,21 It is extremely important to avoid abrupt cessation of these agents based on their potential to cause discontinuation syndrome; instead, their use should be gradually tapered.14 In patients receiving BZD therapy for more than 8 weeks, a 25% weekly dose decrease is an adequate taper regimen.14
GABAergics: Pregabalin and gabapentin are GABAergic drugs proven beneficial for treating SAD.1,18 These agents have similar pharmacologic profiles, working as calcium modulators to inhibit excitatory neurotransmitter release.22 Pregabalin has a quicker onset of action than FDA-approved antidepressants.11 Despite this, GABAergics are reserved for augmentation therapy if first-line agents are not effective; this is due to their abuse potential and risk of withdrawal effects.1,23 In randomized, controlled trials, pregabalin dosages of 450 mg or 600 mg per day and gabapentin dosages of 600 mg to 2,400 mg per day were efficacious.1 Given their abuse potential, these agents must be tapered when the decision is made to discontinue therapy, and during therapy the patient should be monitored frequently for any signs or symptoms of abuse.1 Patients with a history of substance (especially opioid) abuse should avoid GABAergic drugs.1
Beta-Blockers: This drug class is widely used for cardiac conditions, and beta-blockers are also helpful for managing somatic anxiety symptoms.14,24 Owing to their potent anxiolytic effect and ability to reduce tremors, beta-blockers have been used to treat performance anxiety.24 However, little evidence exists to support benefits from beta-blocker use, especially atenolol.3,18,25 Propranolol is frequently prescribed for performance anxiety, and older studies concluded that administration approximately 1 hour before the performance anxiety–provoking situation could be helpful.1,3,20 Additionally, a trial dose may help determine tolerability before drug adminstration at the event itself.20
MAOIs: These antidepressants work by inhibiting the breakdown of mood neurotransmitters.3 MAOIs are typically reserved as a last-line option because of their AEs and drug-food interactions, which is why they are no longer frequently prescribed.3,21 Phenelzine is the preferred MAOI for SAD, although it should not be attempted until the patient has failed treatment with an SSRI or SNRI.3,6 Phenelzine was found to be superior to placebo in acute and long-term treatment of SAD in several clinical trials.18 However, this agent has been associated with postural hypotension and significant bradycardia.3
Other Agents: Buspirone and quetiapine are alternative agents that may be used in patients with an inadequate response to initial SAD treatment.14,26 Buspirone, a drug of the azapirone class, is believed to possess anxiolytic properties as a partial serotonin agonist.14,27 Quetiapine, on the other hand, is a second-generation antipsychotic.1 Both of these agents demonstrate efficacy for generalized anxiety disorder rather than for SAD.14,26 However, buspirone showed some benefit when used as an augmentation agent for SSRIs.28
Comorbidities
Other diseases may present concomitantly in patients with SAD.29 These comorbidities are extremely common and play a prominent role in SAD treatment.14,29 Obsessive-compulsive disorder, posttraumatic stress disorder, and eating disorders are the most frequent psychiatric comorbidities, and patients with SAD are at increased risk for major depression, alcoholism, and suicide.29 Additionally, anxiety symptoms are sometimes misinterpreted in patients with chronic conditions.14 However, adequate treatment should eradicate any anxiety symptoms. Patients who present with cardiovascular, endocrine, gastrointestinal, neurologic, respiratory, or autoimmune disease should be assessed thoroughly because these disease states are typically associated with anxiety symptoms.14
The Pharmacist’s Role
Pharmacists have an essential role in managing treatment in patients with SAD.14 Their comprehensive drug knowledge is invaluable in joint practice with other healthcare professionals.30 In the outpatient setting, pharmacists interact with patients by performing drug evaluations to determine adherence and AEs.31 These assessments are crucial for making any needed improvements to a standing regimen, so they should be discussed with the prescriber as needed.31 Finally, the accessibility of pharmacists validates their importance in providing patient care.30
REFERENCES
1. Garakani A, Murrough JW, Freire RC, et al. Pharmacotherapy of anxiety disorders: current and emerging treatment options. Front Psychiatry. 2020;11:595584.
2. Stein MB, Stein DJ. Social anxiety disorder. Lancet. 2008;371(9618):1115-1125.
3. National Collaborating Centre for Mental Health (UK). Social Anxiety Disorder: Recognition, Assessment and Treatment. NICE Clinical Guidelines, No. 159. Leicester, UK: British Psychological Society; 2013.
4. Craske MG, Stein MB. Anxiety. Lancet. 2016;388(10063):3048-3059.
5. Liebowitz MR, Gelenberg AJ, Munjack D. Venlafaxine extended release vs placebo and paroxetine in social anxiety disorder. Arch Gen Psychiatry. 2005;62(2):190-198.
6. National Institute for Health and Care Excellence. Social anxiety disorder: recognition, assessment and treatment. Clinical guideline [CG159]. www.nice.org.uk/guidance/cg159. Accessed April 19, 2021.
7. American Psychiatric Association. DSM history. www.psychiatry.org/psychiatrists/practice/dsm/history-of-the-dsm. Accessed February 24, 2021.
8. Substance Abuse and Mental Health Services Administration. DSM-5 changes: implications for child serious emotional disturbance (2016). Table 16, DSM-IV to DSM-5 social phobia/social anxiety disorder comparison. www.ncbi.nlm.nih.gov/books/NBK519712/table/ch3.t12/. Accessed April 21, 2021.
9. Boyers GB, Broman-Fulks JJ, Valentiner DP, et al. The latent structure of social anxiety disorder and the performance only specifier: a taxometric analysis. Cogn Behav Ther. 2017;46(6):507-521.
10. Buckley L. Case-based learning: anxiety disorders. Pharmaceutical J. 2020;304(7937):20207899.
11. Bandelow B, Michaelis S, Wedekind D. Treatment of anxiety disorders. Dialogues Clin Neurosci. 2017;19(2):93-107.
12. Sobnosky JL. Overview and management of anxiety disorders. US Pharm. 2014;39(11):56-62.
13. Martin EI, Ressler KJ, Binder E, Nemeroff CB. The neurobiology of anxiety disorders: brain imaging, genetics, and psychoneuroendocrinology. Psychiatr Clin North Am. 2009;32(3):549-575.
14. Melton ST, Kirkwood CK. Anxiety disorders: generalized anxiety, panic, and social anxiety disorders. In: DiPiro JT, Yee GC, Posey L, et al, eds. Pharmacotherapy: A Pathophysiologic Approach. 11th ed. New York, NY: McGraw-Hill; 2020.
15. Marazziti D, Abelli M, Baroni S, et al. Recent findings on the pathophysiology of social anxiety disorder. Clin Neuropsychiatry. 2014;11(2):91-100.
16. Hormone Health Network. What is serotonin? www.hormone.org/your-health-and-hormones/glands-and-hormones-a-to-z/hormones/serotonin. Accessed April 19, 2021.
17. Sartori SB, Singewald N. Novel pharmacological targets in drug development for the treatment of anxiety and anxiety-related disorders. Pharmacol Ther. 2019;204:107402.
18. Williams T, Hattingh CJ, Kariuki CM, et al. Pharmacotherapy for social anxiety disorder (SAnD). Cochrane Database Syst Rev. 2017;(10):CD001206.
19. GoodTherapy. SNRIs (serotonin norepinephrine reuptake inhibitors). www.goodtherapy.org/drugs/antidepressants-snris.html. Accessed April 19, 2021.
20. Schneier FR. Clinical practice. Social anxiety disorder. N Engl J Med. 2006;355(10):1029-1036.
21. Griffin CE III, Kaye AM, Rivera Bueno F, Kaye AD. Benzodiazepine pharmacology and central nervous system-mediated effects. Ochsner J. 2013;13(2):214-223.
22. Sills GJ. The mechanisms of action of gabapentin and pregabalin. Curr Opin Pharmacol. 2006;6(1):108-113.
23. Baldwin DS, Anderson IM, Nutt DJ, et al. Evidence-based pharmacological treatment of anxiety disorders, post-traumatic stress disorder and obsessive-compulsive disorder: a revision of the 2005 guidelines from the British Association for Psychopharmacology. J Psychopharmacol. 2014;28(5):403-439.
24. Farzam K, Jan A. Beta blockers. In: StatPearls [Internet]. Treasure Island, FL: StatPearls Publishing; January 2020. www.ncbi.nlm.nih.gov/books/NBK532906/. Accessed April 19, 2021.
25. Steenen SA, van Wijk AJ, van der Heijden GJ, et al. Propranolol for the treatment of anxiety disorders: systematic review and meta-analysis. J Psychopharmacol. 2016;30(2):128-139.
26. Vaishnavi S, Alamy S, Zhang W, et al. Quetiapine as monotherapy for social anxiety disorder: a placebo-controlled study. Prog Neuropsychopharmacol Biol Psychiatry. 2007;31(7):1464-1469.
27. Blanco C, Antia SX, Liebowitz MR. Pharmacotherapy of social anxiety disorder. Biol Psychiatry. 2002;51(1):109-120.
28. Van Ameringen M, Mancini C, Wilson C. Buspirone augmentation of selective serotonin reuptake inhibitors (SSRIs) in social phobia. J Affect Disord. 1996;39(2):115-121.
29. Koyuncu A, Ince E, Ertekin E, Tükel R. Comorbidity in social anxiety disorder: diagnostic and therapeutic challenges. Drugs Context. 2019;8:212573.
30. Frick A, Osae L, Ngo S, et al. Establishing the role of the pharmacist in mental health: implementing Mental Health First Aid into the doctor of pharmacy core curriculum. Curr Pharm Teach Learn. 2021;13(6):608-615.
31. Eaves S, Gonzalvo J, Hamm JA, et al. The evolving role of the pharmacist for individuals with serious mental illness. J Am Pharm Assoc (2003). 2020;60(5s):S11-S14.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





