US Pharm. 2020;44(3):24-28
ABSTRACT: There is mounting interest among patients and healthcare professionals about the clinical benefits of medical cannabis for various ailments, most commonly for pain relief. Some studies have concluded that medical cannabis may be an alternative for opioids in certain patient populations, while other studies concluded there is insufficient evidence. Medical cannabis is believed to be useful for treating several medical conditions and symptoms, and there is great debate about the safety and efficacy of cannabis for medicinal purposes. It is estimated that 2.1 million Americans use medical cannabis. The legalization and expansion of medical cannabis have created a great debate within the medical community. As the majority of states now allow medical cannabis use, pharmacists must be prepared to provide pharmaceutical care for patients who use medical cannabis, while practicing within the boundaries of the law.
According to a 2018 publication from the CDC, chronic pain has been cited as the most common reason adults in the United States seek medical care.1 The reports states that in 2016, an estimated 20.4%—representing approximately 50 million U.S. adults—had chronic pain, and 8% had high-impact chronic pain that restricted or hindered at least one major life activity.1 Chronic pain is common, expensive, and challenging to treat. Many individuals with chronic pain have turned to cannabis as an alternative form of pain management.2 Moreover, interest in the use of cannabis and cannabinoids to treat chronic noncancer pain is escalating because of their potential to diminish opioid dose requirements.3 For some, the augmented curiosity is due to their greater safety compared with opioids and the possibility that their use can decrease opioid dose requirements via an opioid-sparing effect.3 Both factors have been proposed to contribute to fewer opioid-related deaths.3
According to the National Institutes of Health’s National Center for Complementary and Integrative Health, medical marijuana, also known as cannabis, has been used in medical treatment for more than 3,000 years for a plethora of conditions, including pain relief, digestive issues, and psychological disorders.4 While medical cannabis is thought to be useful for treating several medical conditions and symptoms, there is still great debate about the safety and efficacy of using cannabis for medicinal purposes.5 Current U.S. medical usage is most commonly for pain, although it is also used for anorexia, nausea, glaucoma, and seizures.5 In light of the ongoing opioid epidemic, many of those who suffer with chronic pain are looking for alternatives for analgesia. Results from a recent study revealed that more than 62% of individuals who use medical cannabis do so to treat chronic pain.6 It is estimated that 2.1 million Americans use medical cannabis.6 The World Health Organization reports that an estimated 2.5% of the global population uses cannabis annually, making it the most frequently used drug worldwide.7 The discussion about medical cannabis continues for both prescribers and patients, and clearly, more research is warranted.
What Is Medical Cannabis?
For many patients and prescribers, there is increasing interest in the use of cannabis-based medicines, and researchers are exploring the benefits versus risks.8 Cannabis-based medicines contain cannabinoids derived from the cannabis plant, including delta-9-tetrahydrocannabinol (THC), cannabidiol (CBD), or a combination of THC and CBD.9 There is, however, ambiguity and disagreement regarding the use of cannabis-based medicines for the management of chronic pain.9 The expanding interest about medical cannabis is believed to be related to growing concerns of addressing the ongoing opioid-abuse epidemic.10 Some preliminary evidence suggests that patients who use cannabis may reduce their opioid use, but more research is needed.11,12
Cannabis is made up of multiple types of phytocannabinoid components, the two most studied being THC and CBD.13 In traditional cannabis sativa plants (sometimes called medical or recreational cannabis), THC and CBD are the two most abundant cannabinoid receptors.13 To date, 568 unique molecules have been identified in cannabis; of these, more than 60 are cannabinoids—compounds that act on receptors in the body’s endocannabinoid system (ECS).14 This system plays a key role in endogenous pain control.14-17 Two of the cannabinoids found in cannabis, THC and CBD, along with other cannabinoids, terpenes, and flavonoid compounds, are thought to exhibit synergistic effects that promote pain relief.16,17
THC is the most psychoactive cannabinoid found in cannabis and is principally responsible for the high associated with cannabis.17 It can also diminish nausea and increase appetite. CBD does not provide the euphoria associated with THC and is associated with reduced pain and inflammation.17 Two of the most commonly utilized cannabinoid receptors are CB1 (primarily in the brain and peripheral tissue) and CB2 (primarily in the immune and hematopoietic systems).18 Because CBD acts on the CB2 receptors, it does not cause the significant psychoactive effects that THC does (THC acts primarily on the CB1 receptors).19
State Legalization of Medical Cannabis
Despite the ever-expanding number of statutes approved by state legislatures, cannabis, whether used for medicinal or recreational purposes, remains illegal under federal law via the Controlled Substances Act.20 As the majority of states now permit medical cannabis use, pharmacists must be prepared to provide pharmaceutical care for patients who use these therapies while practicing within the limits of the law.20 Pharmacists should be aware of medical cannabis’ historical events, legislative timeline, legal considerations, professional dilemmas, and future implications so that they can effectively counsel patients about these issues.20
The legalization and expansion of medical cannabis have created ongoing debate within the medical community, with input from the pharmacy profession being mostly left out of legislative discussions, and the construction of regulations linked to medical cannabis.21 This is concerning given the variety of clinical issues that result from the use of medical cannabis, including an understanding of the disease states for which use is considered potentially beneficial.21 Moreover, clinicians should consider that the possibility of drug-drug interactions is a significant concern that needs to be evaluated before patients begin using medical cannabis.21
Due to their pharmacology expertise, pharmacists are an ideal asset to prescribers considering the use of medical cannabis for their patients since pharmacists can screen for potential contraindications and drug-drug interactions. Furthermore, pharmacists should become knowledgeable about the use of cannabis because some states require pharmacist involvement in the legal distribution of medical cannabis.21 According to the American Association of Colleges of Pharmacy, many states, as well as the District of Columbia, Guam, and Puerto Rico, have legalized medical cannabis.22 Three states are already requiring that pharmacists be part of the dispensing process, according to the National Community Pharmacists Association.22 For example, New York State requires a pharmacist to be on the premises and supervising the activities within a cannabis-dispensing facility.22
While medical cannabis presents many possibilities, the plant itself is extremely controversial, with questions over its legality, overall addictiveness, and effectiveness.22 Surveys report that an estimated 85% of Americans support legalizing medical cannabis.22 As of April 2019, medical cannabis was legal in 34 states, many of which necessitate patient registry or identification cards for the purchase and use of the substance for specific, diagnosed medical conditions.16 These conditions differ by state and continue to change. At the federal level, marijuana is classified as a Schedule I substance under the Controlled Substances Act, and there are no recognized medical uses.
In many of the states with legalized cannabis, some type of product testing is required; however, testing varies by state and may be limited to contamination tests or may include quantification of CBD and THC levels.16,23 California, for example, requires dispensaries to sell only cannabis that has been tested for pesticides, contaminants, and microbial impurities.16,23 Starting in July 2018, California also began to require testing to ascertain plant potency (i.e., levels of THC and CBD). This information is included on the product label.16,23 In addition, 12 states have enacted legislation allowing for limited use of medical cannabis (i.e., low CBD:THC ratios). These states, as of spring 2019, included Alabama, Georgia, Indiana, Kentucky, Mississippi, North Carolina, South Carolina, Tennessee, Texas, Virginia, Wisconsin, and Wyoming. It is important to know that consistency and quality of the product received may differ from dispensary to dispensary and from state to state.23
The majority of states with medical cannabis laws restrict its use to patients diagnosed with a predefined set of qualifying conditions, such as cancer, HIV/AIDS, multiple sclerosis, cachexia or wasting syndrome, glaucoma, amyotrophic lateral sclerosis, Crohn’s disease, and seizures.24 More states are beginning to include pain, posttraumatic stress disorder, and problems with sleep. Some are less explicit—the District of Columbia and California both allow cannabis use for any condition that cannot be effectively treated by other means and that limits a patient’s ability to perform activities of daily living.24
The evidence for cannabis’ treatment efficacy across different conditions fluctuates extensively, and comprehensive data on the conditions for which individuals use cannabis are deficient.25 In a recent publication, Boehnke et al analyzed state-registry data to provide nationwide estimates characterizing the qualifying conditions for which patients are licensed to use cannabis medically.25 They found that chronic pain is currently and historically the most common qualifying condition reported by medical cannabis patients (67.5% in 2016).25 An estimated 85.5% of patient-reported qualifying conditions had either substantial or conclusive evidence of therapeutic efficacy.25
Regulation of Cannabis and Cannabis-Derived Products
To date, the FDA has not approved a marketing application for cannabis for the treatment of any disease or condition.26 However, the FDA has approved one cannabis-derived and three cannabis-related drug products.26 These approved products are only available with a prescription from a licensed healthcare provider. The FDA has approved Epidiolex, which contains a purified form of the drug substance CBD for the treatment of seizures associated with Lennox-Gastaut syndrome or Dravet syndrome in patients aged 2 years and older.26 The agency has also approved Marinol and Syndros for therapeutic uses in the U.S., including for the treatment of anorexia associated with weight loss in AIDS patients.26 Marinol and Syndros include the active ingredient dronabinol, a synthetic THC, which is considered the psychoactive component of cannabis.26 Another FDA-approved drug, Cesamet, contains the active ingredient nabilone, which has a chemical structure comparable to THC and is synthetically derived.26
Treating Chronic Pain
Cannabis has been employed to treat pain based on its action on both CB1 and CB2 receptors.27 CB receptor agonists have been revealed to cause antinociceptive and antihyperalgesic effects by regulating neuronal and non–nervous system inflammatory activity.27 One theory proposes that activation of CB1 receptors in mast cells elevates cyclic adenosine monophosphate and suppresses degranulation.27Analgesia may also result from CB1 receptor activation, causing negative modulation of the P2X3 receptor in primary afferent neurons.28 Activation of CB2 receptors can hinder the release of proinflammatory factors, causing suppression of nerve growth factor–induced mast-cell degranulation and neutrophil accumulation.27,28
A growing body of clinical research and a history of anecdotal evidence support the use of cannabis for the relief of some types of chronic pain, including neuropathic pain, and spasticity associated with multiple sclerosis.14,29 In a recent comprehensive review of current data on the health effects of cannabis and cannabinoids, the National Academies of Sciences determined that adult patients with chronic pain who were treated with cannabis/cannabinoids were more likely to experience a clinically noteworthy reduction in pain symptoms.29 They rated these effects as “modest.”14,29 Studies also imply some efficacy for cancer-related pain, migraines, fibromyalgia, and other pain conditions.14,30 It has been suggested that these compounds may be valuable in other conditions, including rheumatoid arthritis, osteoarthritis, and various other types of acute and chronic musculoskeletal pain.31,32 However, how different cannabis species, routes of administration, and doses differ in their effect is less clear, and more research is required.14
Chronic pain relief is by far the most common condition cited by patients using cannabis for medical purposes. Studies and observational reports have demonstrated that more than 80% of patients enrolled in clinical trials and/or with a medical cannabis card indicate “severe pain” as the reason for use.29 In addition, evidence proposes that some individuals with chronic pain are substituting the use of opiates with cannabis.29 Data from a survey directed by a Michigan medical cannabis dispensary claimed that use of medical cannabis was associated with a 64% decrease in use of opioids.33 In addition, a recent analysis of prescription data from Medicare Part D enrollees in states with medical access to cannabis suggested a substantial reduction in prescriptions for conventional pain medications, principally opioids.34
Clinical Study Results
A number of research studies examined the efficacy of medical cannabis on treating chronic pain and other conditions. For example, the findings from a 2019 study published in the Journal of Psychoactive Drugs, which evaluated data from 1,000 individuals taking legalized cannabis in one state, found that among the 65% of individuals taking cannabis for pain, 80% found it was very or tremendously helpful.36 This led to 82% of these individuals being able to reduce, or halt, taking OTC pain medications and 88% being able to halt taking opioids.35
In addition, results reported at the American Academy of Neurology 2019 Annual Meeting revealed that in a preliminary study, investigators at the Dent Neurologic Institute in Buffalo, New York, found that the cannabis provided elderly patients with relief from chronic pain, sleep disorders, and anxiety related to diseases such as amyotrophic lateral sclerosis, Parkinson disease, neuropathy, spinal cord damage, and multiple sclerosis.6 Their findings show that medical cannabis is well tolerated in people aged 75 years and older and may improve symptoms such as chronic pain and anxiety.6
Finally, some evidence suggests cannabinoids may diminish opioid requirements for analgesia, although this finding is not conclusive.36 In a systematic review, Nielsen et al evaluated the effect of cannabinoids to reduce opioid requirements for analgesia and found some lower quality studies suggesting a reduction in opioid requirements during coadministration with cannabinoids. Higher quality studies, however, failed to confirm an opioid-sparing effect.36
The Role of the Pharmacist
As the interest in using medical cannabis for pain relief continues, it is important that pharmacists are aware of the pros and cons of using medical cannabis. There is ongoing research about the ECS and the role of cannabinoid compounds in various medical conditions. As knowledge expands, it is critical that pharmacists are prepared to answer the questions and concerns of healthcare professionals and patients alike. While there are numerous areas of potential therapeutic development of products acting on the ECS intended to treat pain- and non–pain-related conditions, it is vital to recognize that the overall place in therapy for almost all of these products (pharmaceutical, botanical, or otherwise) is still widely unknown, and there is a growing need for more clinical safety and efficacy data since comprehensive information in these areas is still deficient.13
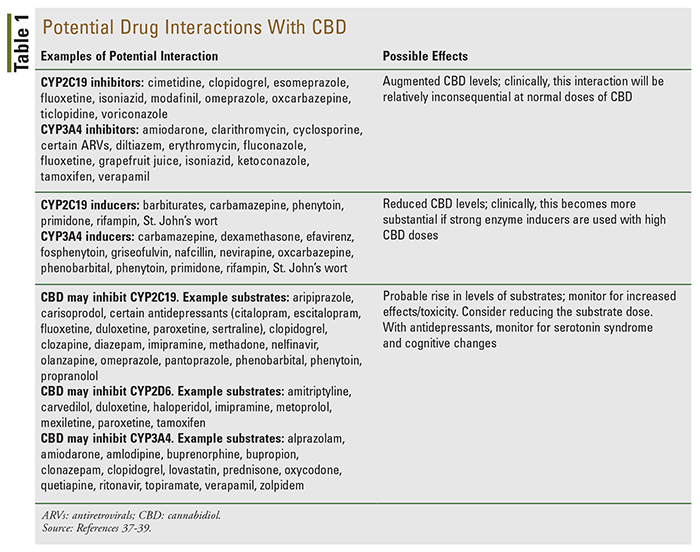
Similarly, it is also crucial to consider that the majority of these products (especially those acting on CB1 and CB2 receptors) may be associated with cognitive dysfunction and increases in psychoactive behavior. It is imperative, therefore, that patients are advised to use these products with caution and to discuss their use with their primary healthcare provider. There is also a potential for drug-drug interactions (TABLE 1).
Conclusion
Clearly, the debate regarding the pros and cons associated with the use of medical cannabis will persist due to continuing legalization and research efforts. Therefore, it is imperative that pharmacists are knowledgeable about this issue and are prepared to answer clinician and patient questions. As one of the most accessible healthcare providers, pharmacists have a pivotal role in educating patients and prescribers about medical cannabis, including the current regulations and clinical studies exploring the potential uses of medical cannabis in chronic pain. There is ongoing research about the ECS and the role of cannabinoid compounds in various medical conditions. While various clinical studies have been conducted regarding the clinical benefits of medical cannabis, more research is required to better understand effective pain-management regimens for medical cannabis users.
REFERENCES
1. Dahlhamer J, Lucas J, Zelaya, C, et al. Prevalence of chronic pain and high-impact chronic pain among adults–United States, 2016. MMWR Morb Mortal Wkly Rep. 2018;67:1001-1006.
2. Boehnke KF, Scott JR, Litinas E, et al. Pills to pot: observational analyses of cannabis substitution among medical cannabis users with chronic pain. J Pain. 2019;20(7):830-841.
3. Campbell G, Hall WD, Peacock A, et al. Effect of cannabis use in people with chronic non-cancer pain prescribed opioids: findings from a 4-year prospective cohort study. Lancet Public Health. 2018;3(7):e341-e350.
4. Medical marijuana. NIH National Center for Complementary and Integrative Health. https://nccih.nih.gov/health/marijuana. Accessed January 13, 2020.
5. Carr D, Schatman M. Cannabis for chronic pain: not ready for prime time. Am J Public Health. 2019;109(1):50-51.
6. Cassels C. Medical cannabis safe, effective in the elderly. Medscape. www.medscape.com/viewarticle/912624. May 6, 2019. Accessed January 13, 2020.
7. Cannabis. World Health Organization. www.who.int/substance_abuse/facts/cannabis/en. December 7, 2010. Accessed January 13, 2020.
8. Banerjee S, McCormack S. Medical cannabis for the treatment of chronic pain: a review of clinical effectiveness and guidelines. Ottawa (ON): Canadian Agency for Drugs and Technologies in Health. 2019. www.ncbi.nlm.nih.gov/books/NBK546424.
9. Freeman TP, Hindocha C, Green SF, Bloomfield MAP. Medicinal use of cannabis-based products and cannabinoids. BMJ. 2019;365:l1141.
10. Hauser W, Finn DP, Kalso E, et al. European Pain Federation (EFIC) position paper on appropriate use of cannabis-based medicines and medical cannabis for chronic pain management. Eur J Pain. 2018;22(9):1547-1564.
11. Vigil JM, Stith SS, Adams IM, Reeve AP. Associations between medical cannabis and prescription opioid use in chronic pain patients: a preliminary cohort study. PLoS One. 2017;12(11):e0187795.
12. Piper BJ, DeKeuster RM, Beals ML, et al. Substitution of medical cannabis for pharmaceutical agents for pain, anxiety, and sleep. J Psychopharmacol. 2017;31(5):569-575.
13. Bettinger JJ, Chu R. The potential of the endocannabinoid system. Practical pain management. www.practicalpainmanagement.com/treatments/pharmacological/analgesics-future-potential-endocannabinoid-system. Updated May 9, 2019. Accessed January 15, 2020.
14. Wachter K. Navigating cannabis options for chronic pain. Practical pain management. www.practicalpainmanagement.com/patient/treatments/marijuana-cannabis/navigating-cannabis-options-chronic-pain. Accessed January 15, 2020.
15. Lewis MM, Yang Y, Wasilewski E, et al. Chemical profiling of medical cannabis extracts. ACS Omega. 2017;2:6091-6103.
16. Russo EB. Taming THC: potential cannabis synergy and phytocannabinoid-terpenoid entourage effects. Br J Pharmacol. 2011;163:1344-1364.
17. Aliana S. The medical marijuana issue. Practical pain management. www.practicalpainmanagement.com/treatments/pharmacological/medical-marijuana-issue. Updated December 3, 2019. Accessed January 16, 2020.
18. Jensen B, Chen J, Furnish T, Wallace M. Medical marijuana and chronic pain: a review of basic science and clinical evidence. Curr Pain Headache Rep. 2015;19(10):50.
19. Pertwee RG, Howlett AC, Abood ME, et al.
20. Wheeler JS, Hagemann TM. Medical marijuana in the United States: historical perspectives, legal considerations, and professional obligations of the pharmacist. J Am Coll Clin Pharm. 2018;1:e9-e16.
21. Nichols J. Medical cannabis: A new frontier for pharmacists. Pharm Today. 2019;25(10):42-53.
22. Cantlupe J. Medical marijuana goes mainstream. AACP. www.aacp.org/article/medical-marijuana-goes-mainstream. Accessed January 13, 2020.
23. State Medical Marijuana Laws. National Conference of State Legislatures, June 27, 2018. www.ncsl.org/research/health/state-medical-marijuana-laws.aspx.
24. Balick R. Pharmacists tread carefully into the world of medical cannabis. Pharm Today. 2018;24(1):28-31.
25. Boehnke KF, Gangopadhyay S, Clauw DJ, Haffajee RL. Qualifying conditions of medical cannabis license holders in the United States. Health Aff. 2019;38(2):295-302.
26. FDA Regulation of Cannabis and Cannabis-Derived Products: Q&A. U.S. Food and Drug Administration. www.fda.gov/news-events/public-health-focus/fda-regulation-cannabis-and-cannabis-derived-products-including-cannabidiol-cbd#whatare. Accessed January 15, 2020.
27. Manzanares J, Julian M, Carrascosa A. Role of the cannabinoid system in pain control and therapeutic implications for the management of acute and chronic pain episodes. Curr Neuropharmacol. 2006;4(3):239-257.
28. Oliviera-Fusaro MCG, Zanoni CIS, Dos Santos GG, et al. Antihyperalgesic effect of CB1 receptor activation involves modulation of P2X3 receptor in the primary afferent neuron. Eur J Pharmacol. 2017;798:113-121.
29. National Academies of Sciences, Engineering, and Medicine. Evidence and Recommendations for Research. Washington, DC: The National Academies Press; 2017.
30. Fine PG, Rosenfeld MJ. The endocannabinoid system, cannabinoids, and pain. Rambam Maimonides Med J. 2013;4:e0022.
31. Ciccone CO. Medical marijuana: just the beginning of a long, strange trip? Phys Ther. 2017;97(2):239-248.
32. Savage SR, Romero-Sandoval A, Schatman M, et al. Cannabis in pain treatment: clinical and research considerations. J Pain. 2016;17:654-668.
33. Boehnke KF, Litinas E, Clauw DJ. Medical cannabis use is associated with decreased opiate medication use in a retrospective cross-sectional survey of patients with chronic pain. J Pain. 2016;17:739-744.
34. Bradford AC, Bradford WD. Medical marijuana laws reduce prescription medication use in Medicare Part D. Health Aff (Millwood). 2016;35:1230-1236.
35. Bachhuber M, Arnsten JH, Wurm G. Use of cannabis to relieve pain and promote sleep by customers at an adult use dispensary. J Psychoactive Drugs. 2019;51:400-404.
36. Nielsen S, Sabioni P, Trigo JM, et al. Opioid-sparing effect of cannabinoids: a systematic review and meta-analysis. Neuropsychopharmacology. 2017;42(9):1752-1765.
37. Gaston TE, Bebin EM, Cutter GR, et al. Interactions between cannabidiol and commonly used antiepileptic drugs. Epilepsia. 2017;58:1586-1592.
38. Epidiolex (cannabidiol) Prescribing Information. Carlsbad, CA: Greenwich Biosciences, Inc; 2018.
39. Medical Cannabis: Adverse Effects and Drug Interactions. Department of Health, Washington, DC. https://doh.dc.gov/sites/default/files/dc/sites/doh/publication/attachments/Medical%20Cannabis%20Adverse%20Effects%20and%20Drug%20Interactions_0.pdf.
To comment on this article, contact rdavidson@uspharmacist.com.





