US Pharm. 2011;36(2):HS-2-HS-8.
Torsades de pointes (TdP) is an ECG manifestation characterized by a form of ventricular tachycardia with a spiral appearance and complexes that first look positive and then negative. Drug-induced QT prolongation acts as a marker for risk of progression to TdP. However, drug-induced QT-interval prolongation does not always progress to TdP.1
The QT interval represents the time required for ventricular tissue repolarization after ventricular depolarization. Medications may alter the QT interval, increasing the duration of repolarization and reducing the amplitude of the T wave, a state known as T-wave flattening.1 To compensate for the importance of pulse in the QT interval, a heart rate–corrected QT interval (QTc) may be calculated using Bazett’s formula: QTc = QT/ÖRR.2 A QTc interval greater than 500 msec is considered to be prolonged and increases a patient’s risk for TdP.1
BACKGROUND
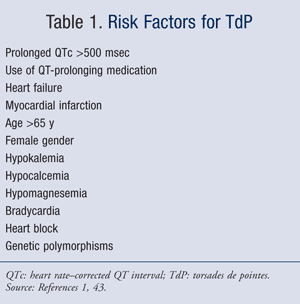
TdP is uncommon, but the prevalence varies according to many patient-specific factors, including electrolyte disturbances (specifically, potassium, magnesium, and calcium); genetics (polymorphisms increase TdP risk); and drug therapy (QT-prolonging medications). Other notable risk factors (TABLE 1) include female gender, which confers a twofold increase in risk, and age greater than 65 years.1 The presence of multiple risk factors additively increases a patient’s risk of TdP.1
TdP that is not adequately managed can progress to ventricular fibrillation (VF) or sudden cardiac death (SCD). VF is a potentially fatal arrhythmia that presents primarily in patients with ischemic or structural heart disease. On an ECG, VF shows varying QRS complexes from beat to beat.3 In the absence of medical intervention, VF could lead to SCD, which is “a natural death due to cardiac causes, involving sudden loss of consciousness and within one hour after symptoms appear.”4 Multiple studies show that QTc-prolonging medications increase the risk of SCD two- to eightfold.5,6
Medication-induced QT prolongation commonly occurs through alterations of intracellular ion channels. Prolonged depolarization is associated with increased function of inward sodium channels (INa).7 More often, medications reduce repolarization by inhibiting the outward potassium channels (IKr). Potassium and magnesium electrolyte abnormalities alter the function of IKr, increasing the risk of arrhythmias or QT prolongation and TdP.8-10
The liver and kidneys eliminate many drugs associated with QTc prolongation. When either pathway is impaired, patients may accumulate the drug, thus increasing their risk for QTc prolongation and TdP. Administration factors also must be taken into account with QT-prolonging medications. Based on animal studies, rapid infusion of QT-prolonging drugs may be associated with a higher incidence of TdP.11 The administration of IV drugs is associated with increased QT prolongation, in comparison with oral formulations.12
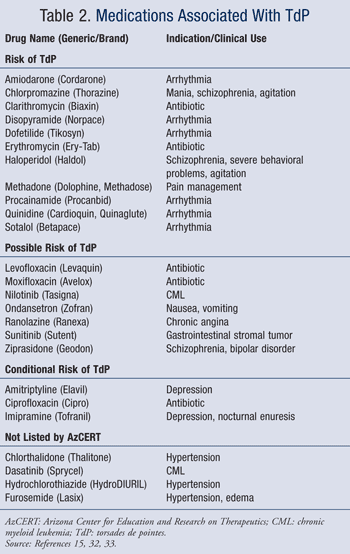
Many drugs are associated with QT prolongation. The University of Arizona Center for Education and Research on Therapeutics ( www.azcert.org) has compiled an extensive database of medications that prolong the QT interval, including those with a risk of TdP, those with a possible risk, and those with a conditional risk.13 The site also contains links to PubMed searches for expanded literature regarding QT prolongation and the medication of interest. This site is an invaluable resource for pharmacists who need to assess the QT-prolongation risk of medications. The following section gives a detailed discussion of medications that are commonly used or that carry a high risk of QT prolongation (TABLE 2).
DRUGS WHOSE MECHANISM OF ACTION CAUSES QT PROLONGATION
Antiarrhythmics
Class I: Quinidine, a class IA antiarrhythmic agent, reduces the depolarization rate and prolongs the refractory period by blocking potassium channels at low concentrations and blocking sodium channels at higher concentrations.14 This causes TdP to occur in approximately 4% to 8% of patients treated with quinidine.4
Procainamide is another class IA antiarrhythmic agent. To become active, procainamide is converted to N-acetylprocainamide.15 Toxic levels of this metabolite can increase the risk of QTc prolongation and TdP.16
Class III: Amiodarone works by blocking beta-adrenergic receptors and sodium, potassium, and calcium channels. Amiodarone has a low incidence of proarrhythmia (new arrhythmia or worsening of existing arrhythmia) and TdP compared with other antiarrhythmics because it utilizes several different mechanisms of action.17 The incidence of TdP may increase with long-term therapy, electrolyte disturbances, and combination with other medications that may prolong the QTc interval.18
Sotalol, another class III antiarrhythmic, blocks beta receptors and inhibits potassium repolarization. Sotalol is eliminated by the kidneys; therefore, dosage adjustments based on creatinine clearance (CrCl) help prevent toxicity and QTc prolongation. Because QTc prolongation may be experienced at therapeutic dosages, this medication should be started while the patient is hospitalized.19 The reported incidence of these proarrhythmic effects is around 5% to 6%, with 1% to 2% of these being TdP.20
Dofetilide is a selective potassium channel blocker. Dofetilide prolongs the refractory period without causing any changes in conduction or contractility. The QTc-interval changes and the incidence of TdP are directly related to the plasma concentration of dofetilide.21 Most reported instances of TdP occurred within the first few days of therapy. It is recommended to obtain a preliminary ECG, to dose based on CrCl, and to monitor by ECG for any QTc prolongation.22
MEDICATIONS WHOSE QT PROLONGATION IS AN ADVERSE DRUG REACTION
Antipsychotics
First Generation: Haloperidol is used to treat schizophrenia and severe agitation. Both the oral and the IV formulations block potassium channels and are associated with TdP.23 Haloperidol prolongs the QTc interval by 15 msec to 30 msec, which may be amplified when the drug is combined with other medications that prolong the QTc interval.
Chlorpromazine is an antipsychotic with some antiemetic properties. It also suppresses potassium channels, creating the potential for QTc prolongation.24 Very few reports exist documenting the incidence of TdP with chlorpromazine.
Second Generation: Ziprasidone blocks dopamine and serotonin. It can increase repolarization time by suppressing potassium currents. The QT interval is prolonged in a dose-dependent fashion up to 20 msec.25 In one case study, a patient presented with QTc prolongation greater than 500 msec that possibly was due to ziprasidone. The patient was taking other medications that may have contributed to the occurrence of TdP, so other causes could not be ruled out.26
Antidepressants
Tricyclic Antidepressants (TCAs): TCAs have activity with both sodium and potassium channels. The prolonged depolarization with sodium channels constitutes the major mechanism of QT prolongation. The combination of TCAs and drugs with increased effects on potassium channels may confer a greater risk of TdP and QT prolongation. TCAs noted for their ability to prolong QT include amitriptyline, doxepin, desipramine, and clomipramine.27
Antibiotics
Fluoroquinolones: Fluoroquinolones have variable effects on QT prolongation. Sparfloxacin- and grepafloxacin-related QT prolongation have caused discontinuation in preliminary drug development, whereas other fluoroquinolones are unlikely to cause QT changes. It is unclear whether fluoroquinolone QT prolongation occurs as a class effect or is associated with individual agents. In a comparison of ciprofloxacin, levofloxacin, and moxifloxacin, moxifloxacin was shown to cause the most pronounced QT prolongation through interactions with potassium channels.28
Macrolides: QT prolongation with macrolide antibiotics occurs because of potassium-channel suppression or drug–drug interactions. Clarithromycin, roxithromycin, and erythromycin are believed to have the greatest ability to reduce repolarization through potassium channels, giving them the largest theoretical effect on QT interval. Macrolide antibiotics have varied ability to inhibit CYP3A4 activity, increasing the risk of QT prolongation with other drugs.29
Tyrosine Kinase Inhibitors
Newer tyrosine kinase inhibitors used in the treatment of various cancers have been noted to cause significant QT prolongation. Sunitinib, nilotinib, and dasatinib have been associated with varied amounts of QT prolongation at 10 msec, 5 to 15 msec, and 3.3 msec, respectively.30-32 Depending on the indication, dasatinib may be a favorable alternative owing to the lesser likelihood of QT prolongation.
Diuretics
Diuretics may indirectly increase the risk of TdP by causing the excretion of potassium and magnesium. If untreated, these electrolyte disturbances can increase patient risks. Effects of other drugs that prolong the QT interval are exacerbated by hypokalemia and hypomagnesemia.33
Methadone
Methadone is used to treat chronic pain and opiate addiction. Levacetylmethadol, a drug similar to methadone, was removed from European markets because of the increased risk of TdP.34 Two studies have found that methadone causes a significant increase in QTc prolongation and dispersion from baseline ECG values. Higher doses were associated with an increased risk of TdP.35
Ranolazine
Ranolazine, an agent used to treat chronic angina, inhibits the sodium–calcium exchange to reduce the amount of intracellular calcium. This results in decreased myocardial oxygen demand.36 At higher doses, ranolazine blocks the outward movement of potassium, causing potential prolongation. Because of this, it has been speculated that ranolazine may increase the risk of TdP.37 Trials found that ranolazine could potentially prolong the QTc interval by 2 msec to 6 msec; however, evidence was limited that QTc prolongation caused TdP.38
Ondansetron
Ondansetron is a 5-HT3 antagonist used to prevent nausea and vomiting associated with cancer treatment and postoperative procedures.39 A study of postoperative nausea and vomiting found that postanesthesia patients possessed longer QTc intervals. When given either droperidol or ondansetron, these patients experienced a QTc interval greater than 500 msec, resulting in the recommendation that these agents be used with caution postsurgery owing to the risk of TdP.40
TREATMENT
The treatment of TdP is crucial for preventing progression to VF or SCD. Recommended therapies include correcting electrolytes such as magnesium and potassium, discontinuing the offending agents, avoiding medications that could prolong the QTc interval, and cardioversion. Magnesium supplementation is the first-line treatment for TdP. In one study, a bolus of 2 g magnesium sulfate eradicated TdP in nine of 12 patients; an additional bolus of 5 g resolved the abnormal rhythm in the remaining three patients.41 Potassium supplementation is recommended in hypokalemic patients. The administration of potassium creates an increased efflux of potassium, which shortens the QTc interval. Because electrolyte imbalances are common in hospitalized patients, it is important to monitor these values and determine whether supplementation is needed.42
ROLE OF THE PHARMACIST
Pharmacists can help reduce TdP occurrence through clinical interventions and monitoring and can aid in the therapeutic substitution of drugs with a more favorable proarrhythmic profile. Classes such as chemotherapeutic agents or fluoroquinolones have differing levels of QT prolongation. If indicated, the pharmacist may suggest conversion to an agent with less QT prolongation.
Electrolyte monitoring and necessary supplementation alter controllable risk factors for progression to TdP. Hospitalized patients taking diuretics who are already at risk for electrolyte abnormalities or TdP are a high-risk group easily monitored by pharmacists on a daily basis.
Pharmacists must be vigilant about monitoring patients for drug–drug interactions that may increase their risk of QT prolongation and, potentially, TdP. By paying attention to patient medication lists, pharmacists may identify patients at risk for QT prolongation and progression to TdP. Patients receiving one or more QT-prolonging therapies are at increased risk and should be monitored for changes in QT interval. If QT prolongation occurs, removal or substitution of current agents should be considered. Pharmacists must also take note of the clearance of QT-prolonging medications. Decreased hepatic and renal function may increase the patient’s exposure to QT-prolonging medications, thereby increasing risk. The use of drugs that alter renal and hepatic function, such as enzyme inducers or inhibitors and P-glycoprotein inhibitors, may alter serum concentrations and decrease the therapeutic benefit or put patients at risk for prolonged drug exposure.
CONCLUSION
QT prolongation and TdP present a clinically dangerous situation that may be minimized by pharmacist intervention. Resources are available to pharmacists to help identify medications that prolong the QT interval. Through a variety of clinical interventions, pharmacists may reduce the occurrence of this potentially fatal condition and improve overall patient care.
REFERENCES
1. Li EC, Esterly JS, Pohl S, et al. Drug-induced QT-interval prolongation: considerations for clinicians. Pharmacotherapy. 2010;30:684-701.
2. Bazett HC. An analysis of the time-relations of electrocardiograms. Heart. 1920;7:353-370.
3. Koplan BA, Stevenson WG. Ventricular tachycardia and sudden cardiac death. Mayo Clin Proc.
4. DiPiro JT, Matzke GR, Posey LM, et al, eds. Pharmacotherapy: A Pathophysiological Approach. 6th ed. New York, NY: McGraw-Hill Medical; 2005:347.
5. Straus SM, Kors JA, De Bruin ML, et al. Prolonged QTc interval and risk of sudden cardiac death in a population of older adults. J Am Coll Cardiol. 2006;47:362-367.
6. Straus SM, Sturkenboom MC, Bleumink GS, et al. Non-cardiac QTc-prolonging drugs and the risk of sudden cardiac death. Eur Heart J. 2005;26:2007-2012.
7. Roden DM, Balser JR, George AL Jr, Anderson ME. Cardiac ion channels. Annu Rev Physiol.
8. Yang T, Snyders DJ, Roden DM. Rapid inactivation determines the rectification and [K+]o dependence of the rapid component of the delayed rectifier K+ current in cardiac cells. Circ Res. 1997;80:782-789.
9. Zhang S, Sawanobori T, Adaniya H, et al. Dual effects of external magnesium on action potential duration in guinea pig ventricular myocytes. Am J Physiol. 1995;268:H2321-H2328.
10. Yang T, Roden DM. Extracellular potassium modulation of drug block of IKr. Implications for torsade de pointes and reverse use-dependence. Circulation. 1996;93:407-411.
11. Klotz U. Antiarrhythmics: elimination and dosage considerations in hepatic impairment. Clin Pharmacokinet. 2007;46:985-996.
12. Lexicomp Online. Sotalol.
http://online.lexi.com/crlsql/ 2009;84:289-297. 2002;64:431-475.
13. Carlsson L, Abrahamsson C, Andersson B, et al. Proarrhythmic effects of the class III agent almokalant: importance of infusion rate, QT dispersion, and early afterdepolarisations. Cardiovasc Res. 1993;27:2186-2193.
14. Siu CW, Au WY, Yung C, et al. Effects of oral arsenic trioxide therapy on QT intervals in patients with acute promyeloctyic leukemia: implications for long-term cardiac safety. Blood. 2006;108:103-106.
15. Arizona CERT. Drugs that prolong the QT interval and/or induce torsades de pointes ventricular arrhythmia.
www.azcert.org/medical-pros/
16. Wyse K, Ye V, Campbell T. Action potential prolongation exhibits simple dose-dependence for sotalol, but reverse dose-dependence for quinidine and disopyramide: implications for proarrhythmia due to triggered activity. J Cardiovasc Pharmacol. 1993;21:316-322.
17. Chow MJ, Piergies AA, Bowsher DJ, et al. Torsade de pointes induced by N-acetylprocainamide. J Am Coll Cardiol. 1984;4:621-624.
18. Lazzara R. Amiodarone and torsade de pointes. Ann Intern Med. 1989;111:549-551.
19. Lim HE, Pak H, Ahn JC, et al. Torsade de pointes induced by short-term oral amiodarone therapy. Europace. 2006;8:1051-1053.
20. D’Aloia A, Faggiano P, Brentana L, et al. Sustained torsade de pointes occurring early during oral sotalol therapy for atrial fibrillation recurrence prophylaxis in a patient without heart disease. Int J Cardiol. 2005;105:337-339.
21. Allen MJ, Nichols DJ, Oliver SD. The pharmacokinetics and pharmacodynamics of oral dofetilide after twice daily and three times daily dosing. Br J Clin Pharmacol. 2000;50:247-253.
22. Tikosyn (dofetilide) package insert. New York, NY: Pfizer Inc; November 2006.
23. Glassman AH, Bigger JT. Antipsychotic drugs: prolonged QTc interval, torsade de pointes, and sudden death. Am J Psychiatry. 2001;158:1774-1782.
24. Lexicomp Online. Chlorpromazine.
http://online.lexi.com/crlsql/
25. Ray WA, Chung CP, Murray KT, et al. Atypical antipsychotic drugs and the risk of sudden cardiac death. N Engl J Med. 2009;360:225-235.
26. Heinrich TW, Biblo LA, Schneider J. Torsades de pointes associated with ziprasidone. Psychosomatics. 2006;47:264-268.
27. Vieweg WV, Wood MA. Tricyclic antidepressants, QT interval prolongation, and torsade de pointes. Psychosomatics. 2004;45:371-377.
28. Tsikouris JP, Peeters MJ, Cox CD, et al. Effects of three fluoroquinolones on QT analysis after standard treatment courses. Ann Noninvasive Electrocardiol. 2006;11:52-56.
29. Volberg WA, Koci BJ, Su W, et al. Blockade of human cardiac potassium channel human ether-a-go-go-related gene (HERG) by macrolide antibiotics. J Pharmacol Exp Ther. 2002;302:320-327.
30. Bello CL, Mulay M, Huang X, et al. Electrocardiographic characterization of the QTc interval in patients with advanced solid tumors: pharmacokinetic-
31. Deremer DL, Ustun C, Natarajan K. Nilotinib: a second-generation tyrosine kinase inhibitor for the treatment of chronic myelogenous leukemia. Clin Ther. 2008;30:1956-1975.
32. Johnson FM, Agrawal S, Burris H, et al. Phase 1 pharmacokinetic and drug-interaction study of dasatinib in patients with advanced solid tumors. Cancer. 2010;116:1582-1591.
33. Singh BN, Hollenberg NK, Poole-Wilson PA, Robertson JI. Diuretic-induced potassium and magnesium deficiency: relation to drug-induced QT prolongation, cardiac arrhythmias and sudden death. J Hypertens. 1992;10:301-316.
34. Krantz MJ, Lowery CM, Martell BA, et al. Effects of methadone on QT-interval dispersion. Pharmacotherapy. 2005;25:1523-1529.
35. Krantz MJ, Lewkowiez L, Hays H, et al. Torsade de pointes associated with very-high-dose methadone. Ann Intern Med. 2002;137:501-504.
36. Lexicomp Online. Ranolazine.
http://online.lexi.com/crlsql/
37. Wu L, Shryock JC, Song Y, et al. Antiarrhythmic effects of ranolazine in a guinea pig in vitro model of long-QT syndrome. J Pharmacol Exp Ther. 2004;310:599-605.
38. Kumar K, Nearing B, Bartoli C, et al. Effect of ranolazine on ventricular vulnerability and defibrillation threshold in the intact porcine heart. J Cardiovasc Electrophysiol. 2008;19:1073-1079.
39. Lexicomp Online. Ondansetron.
http://online.lexi.com/crlsql/
40. Charbit B, Albaladejo P, Funck-Brentano C, et al. Prolongation of QTc interval after postoperative nausea and vomiting treatment by droperidol or ondansetron. Anesthesiology. 2005;102:1094-1100.
41. Tzivoni D, Keren A, Cohen AM, et al. Magnesium therapy for torsades de pointes. Am J Cardiol.
42. Viskin S. Torsades de pointes. Curr Treat Options Cardiovasc Med. 1999;1:187-195.
43. Drew BJ, Ackerman MJ, Funk M, et al. Prevention of torsade de pointes in hospital settings: a scientific statement from the American Heart Association and the American College of Cardiology Foundation. J Am Coll Cardiol. 2010;55:934-947. 1984;53:528-530.
To comment on this article, contact rdavidson@uspharmacist.com.





