US Pharm. 2018;44(4):20-23.
ABSTRACT: Annually, more than 200,000 medication errors are reported to U.S. poison-control centers. Approximately 30% of these errors involve children. Dosing errors are the most common medication error. It is crucial for healthcare providers to ensure that the appropriate drug and dose are prescribed to children, especially neonates, because of their differences in response to drugs compared with adults. Understanding pediatric pharmacokinetics and stages of development can help providers more accurately prescribe medications for children and minimize dosing errors. Pharmacists can help prevent medication errors by checking dosing calculations, screening for drug-drug interactions, and counseling caregivers on proper administration and medication-storage safety tips.
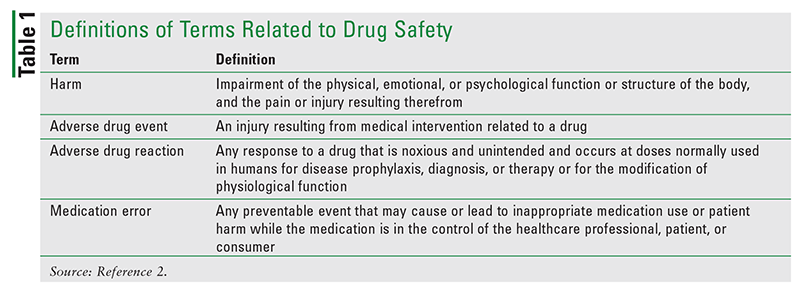
Drug safety is paramount in pediatric patients, owing to an alarming number of adverse events caused by medications. U.S. poison-control centers handle more than 200,000 cases of out-of-hospital medication errors annually, and children under 6 years old constitute approximately 30% of these cases.1 To clarify the differences between adverse events, adverse drug reactions, and medication errors, the National Coordinating Council for Medication Error Reporting and Prevention, the Institute of Medicine, and the World Health Organization have provided definitions of these drug-safety terms (see TABLE 1). Adverse drug reactions and adverse drug events occur once patient harm from a drug has occurred. All adverse drug reactions are adverse drug events; however, not all adverse drug events are caused by an error.2
Pediatric Pharmacokinetics and Developmental Stages
The process of drug absorption, distribution, metabolism, and elimination is referred to as pharmacokinetics.3 It is important to recognize differences in the factors that affect drug disposition in children. To help differentiate stages of development, pediatric patients are grouped according to age, as shown in TABLE 2.4 Depending on the patient’s stage of development, there are important age-related variations in pharmacokinetics.4 It is crucial that healthcare providers take particular care to ensure that the appropriate drug and dose are prescribed to children, especially neonates, because of the differences in their response to drugs compared with adults.

Absorption: Several factors affect the absorption of drugs from the gastrointestinal tract, such as gastric-acid secretion, bowel length and absorptive surface, gastric emptying time, bile-acid formation, and microbial flora. The bioavailability of acid-labile drugs such as penicillin increases and the bioavailability of weakly acidic drugs such as phenobarbital decreases owing to reduced gastric-acid secretion. The bioavailability of lipophilic drugs such as diazepam lessens because of reduced bile-salt formation.3 The time a drug takes to reach therapeutic concentrations is increased in young infants due to prolonged gastric-emptying time. Alterations in intestinal flora that facilitate metabolism may affect absorption in the gut.3 Neonates and young infants have a thinner stratum corneum, and the ratio of surface area to weight is greater than in older children and adults; therefore, transdermal absorption may be enhanced.3,5
Distribution: The proportions of body water, fat, and muscle in pediatric patients differ throughout the stages of development. Therefore, providers must consider these differences because they can impact the dosing of drugs.4 Neonates and premature infants have a higher amount of water composition than adults, which affects the dosing of water-soluble drugs. On a milligram-per-kilogram basis, neonates require higher doses of water-soluble drugs compared with adults.4,5 As children grow older, lower doses are needed to avoid toxicity because there is a decline in water as a percentage of body weight.3
When drugs bind to proteins such as albumin, lipoprotein, and alpha-1 acid glycoprotein, the distribution of free drug throughout the body is limited. Neonates have decreased protein binding due to competitive binding by bilirubin and free fatty acids, which circulate in higher concentrations in neonates and infants. This may result in increased free drug concentrations, which can contribute to a higher frequency of adverse effects at lower drug concentrations.3
Metabolism: The most important system for drug metabolism is the CYP450 enzyme system in the liver and small bowel.3 Enzyme systems mature at different stages of development, and they may be absent at birth or exist at fairly reduced levels.5 Because the increase in metabolic rate in children is often greater than that in adults, children may require higher doses on a milligram-per-kilogram basis or more frequent dosing compared to adults.5
Elimination: The liver and kidney are the main organs that break down and eliminate drugs from the body. These organs mature with age. Therefore, drugs in neonates and infants are broken down and eliminated more slowly than in older children and adults.3 The bile and the kidney eliminate drug metabolites. Renal elimination of drugs depends on the glomerular filtration rate, renal blood flow, plasma protein binding, and tubular secretion.4 In the first 2 years of life, these factors are altered. At birth, renal plasma flow is low and reaches adult levels by the age of 1 year. The glomerular filtration rate is low at birth and increases to an adult level when the infant reaches age 3 to 5 months.3
Potential Causes of Medication Errors
There are a host of factors from which medication errors can derive. Illegible prescriptions, abbreviations in prescriptions, language barriers, lack of communication skills, tiredness, and multiple drug combinations are some of the major factors leading to medication errors. Children with multiple prescriptions are at risk for preventable adverse drug events. Dosing errors, such as incorrect dosage or frequency of administration and either underdosing or overdosing, are common medication errors. Other errors include inappropriate medication selection for the indication, incorrect route of administration, failure to screen drug interactions or monitor side effects, and lack of communication between members of the healthcare team.6
The Pharmacist’s Role
Pharmacists are able to intercept and prevent medication errors by checking the dosing to ensure the accuracy of a prescription. Pharmacists can provide medication counseling to caregivers regarding the medication’s use, proper administration, potential side effects, and adverse effects; they can also provide general medication-safety tips. Studies have shown that in low-income populations, medication errors are more prevalent because potentially inadequate or marginal literacy can lead to the misunderstanding of medication-dosing instructions.6
Pharmacists and pharmacy technicians should obtain a patient’s age and weight at every visit. Children’s weight frequently changes, and drug doses are calculated based on milligram per kilogram. It should be noted that even in very large children, the highest dose should not exceed the maximum adult dose.4 Healthcare providers should consult pediatric references such as LexiComp, Micromedex, Harriet Lane, and NeoFax. In reference to children with renal failure, a good source of renal dosing is Drug Prescribing in Renal Failure. Also, for pregnant and lactating mothers, Drugs in Pregnancy and Lactation—a reference guide to fetal and neonatal risk—should be consulted.
Pharmacists should keep in mind the following counseling and medication-safety points7-11:
• When dispensing medications for pediatric patients, always include any appropriate auxiliary labels. Common labels such as Shake well, Refrigerate, Take with food, Avoid sunlight, and Wear sunscreen serve as reminders to caregivers.
• Check the expiration dates on medications. Expired medications may lose potency and become harmful. Encourage patients to properly dispose of medications that are no longer being used. For example, fentanyl patches are highly potent opioids, and a small amount left on a patch can cause respiratory depression, hypotension, or death in a small child exposed to it. Proper disposal of these patches is to adhere the sticky sides together and then flush the patch down the toilet.7
• A common error resulting in approximately 60,000 emergency department visits each year occurs when children access medications when parents or other caregivers are not looking.8 Always dispense medications with childproof caps. Counsel caregivers to keep the childproof caps on medication bottles when not in use.
• Secure both OTC and prescription medications out of reach of children. A locked dresser drawer and a high closet shelf are some good storage places.
• Discourage patients from removing medications from blister packs in advance of taking them or removing them all at once to store them in an unmarked container. For example, iron tablets are toxic to a toddler, but the child may think it is candy and eat it because the tablets are sugar-coated.
• Explain to caregivers that they should never tell children that their medication is candy in order to get them to take it; instead, they should explain what the medication is used for.8
• When administering medications, it is best not to mix drugs with food or liquid unless specifically instructed to do so because this can interfere with the medication’s effectiveness or dilute the dose.9
• Always counsel caregivers on how to properly measure liquid medications with a syringe. Household spoons and tablespoons are inaccurate and should not be used to administer liquid medications.10,11 It has been found that medication errors are more common when caregivers use dosing cups instead of syringes.
Conclusion
Medication errors in pediatric patients can lead to unwanted adverse events and reactions. It is important for physicians, pharmacists, and other healthcare providers to be aware that children need special dosing considerations and careful monitoring because their bodies are in different stages of development compared with adults. Pharmacists are in the position to counsel parents and caretakers about proper medication administration and storage. Communication between all persons involved in the care of pediatric patients will yield a better outcome.
REFERENCES
1. American Academy of Pediatrics. Every 8 minutes a child experiences an out-of-hospital medication error. www.aap.org/en-us/about-the-aap/aap-press-room/Pages/Every-8-Minutes-a-Child-Experiences-an-.aspx. Accessed January 5, 2019.
2. National Coordinating Council for Medication Error Reporting and Prevention. Contemporary view of medication-related harm. A new paradigm. www.nccmerp.org/sites/default/files/nccmerp_fact_sheet_2015-02-v91.pdf. Accessed January 5, 2019.
3. Jones BL. Pharmacokinetics in children. www.merckmanuals.com/professional/pediatrics/principles-of-drug-treatment-in-children/pharmacokinetics-in-children. Accessed January 5, 2019.
4. Technician tutorial: dispensing drugs for pediatric patients. Pharmacist’s Letter/Pharmacy Technician’s Letter. July 2018.
5. Henderson R. Prescribing for children. https://patient.info/doctor/prescribing-for-children. Accessed January 5, 2019.
6. Bailey SC, Pandit AU, Yin S, et al. Predictors of misunderstanding pediatric liquid medication instructions. Fam Med. 2009;41(10):715-721.
7. Technician tutorial: keeping kids safe from medications. Pharmacist’s Letter/Pharmacy Technician’s Letter. January 2016.
8. Consumer Healthcare Products Association. Safe storage. www.chpa.org/SafeStorage.aspx. Accessed January 5, 2019.
9. HealthyChildren.org. Medication safety tips. www.healthychildren.org/English/safety-prevention/at-home/medication-safety/Pages/Medication-Safety-Tips.aspx. Accessed January 5, 2019.
10. Mehndiratta S. Strategies to reduce medication errors in pediatric ambulatory settings. J Postgrad Med. 2012;58(1):47-53.
11. ConsumerMedSafety.org. Tips for measuring liquid medicines safely. www.consumermedsafety.org/tools-and-resources/medication-safety-tools-and-resources/taking-your-medicine-safely/measure-liquid-medications. Accessed January 5, 2019.
To comment on this article, contact rdavidson@uspharmacist.com.





