US Pharm. 2022;47(3):43-48.
Multiple sclerosis (MS) is a chronic immune-mediated, inflammatory neurologic disease affecting the brain, spinal cord, and optic nerve. It is a condition characterized by demyelination and axonal loss, resulting in interruption of nerve impulses, causing a multitude of symptoms, such as sensation loss, muscle weakness, vision loss, incoordination, cognitive impairment, fatigue, and bladder and bowel disturbances. The pathological hallmark of MS is the accumulation of demyelinating lesions found in the white and gray matter of the brain and spinal cord. It is estimated that nearly 1 million adults are living with MS in the United States. It is a very costly condition; in 2019 the total economic burden of MS was estimated to be $85.4 billion, with the majority of this attributed to direct medical costs.1-6
MS is one of the most common causes of nontraumatic disability in young adults, with incidences peaking between the ages of 20 and 40 years, with a higher prevalence in women. It is a debilitating disease that diminishes quality of life; mobility is impaired in up to 90% of patients with MS, fatigue affects up to 95% of patients, and pain is reported in up to 86% of patients. People with MS often have difficulty working, pursuing leisurely activities, and participating in overall daily activities. As MS progresses, patients experience increased disability. More than half of those who have MS will experience walking impairments within 10 years of disease onset. There is also a significant reduction in life expectancy by 7 to 14 years in patients with MS compared with the general population. Currently, there is no cure for MS, and lifelong treatment is required. Current treatment involves a multidisciplinary approach and consists of disease-modifying therapies (DMTs), symptomatic treatment, lifestyle modifications, psychological support, and rehabilitation interventions. As medication experts, pharmacists serve as a resource for patients and their caregivers, aiding in the discussion about the importance of therapy, adherence, and of proper administration techniques.2,7,8
Four Clinical Courses of MS
The clinical course of MS is defined by periods of relapse and/or disease progression. A relapse is the occurrence of new symptoms or worsening of old symptoms in the absence of fever or infection lasting more than 24 hours and separated from the previous attack by at least 30 days. Some common presentations of relapses include optic neuritis, sensory deficits, cerebellar dysfunctions, or severe fatigue. Disease progression is worsening of signs and symptoms over at least 6 months despite having periods of relapse or remissions.9
Patients with MS can be classified or grouped into four major categories based on their disease course: relapsing-remitting MS (RRMS), secondary progressive MS (SPMS), primary progressive MS (PPMS), and progressive relapsing MS (PRMS). The most common form of MS at disease onset is RRMS, composing almost 90% of cases. This disease pattern is characterized by periods of symptom flareups, or relapses, followed by periods of partial or complete remission. There is no evidence of disease progression between attacks. For some patients, relapses decrease in frequency over time and sometimes completely disappear. However, in most patients, neuronal damage becomes clinically evident, and usually within 10 to 20 years after disease onset, patients progress to SPMS. A steady worsening of neurologic deficits occurs. Periods of relapses typically lead to further progression. About 10% of patients will present with PPMS at disease onset; symptoms continue to worsen from the beginning. Patients do not experience periods of relapses or remissions but may experience occasional plateaus. The mean age of onset is about 40 years, and it seems to more frequently affect men. PRMS is rare, affecting fewer than 5% of patients. It is progressive from the beginning and is characterized by a continual decline in neurologic functioning with occurrences of superimposed relapses.3,5,9,10
Risk Factors
The exact cause of MS is still unknown, but epidemiologic data suggest environmental and genetic factors both play a role (see TABLE 1). Genetics seem to play a role in the development of MS. The recurrence rate of MS in families is about 13% to 20%, but the risk decreases with increasing genetic distance. In first-degree relatives, MS risk is 2.77%. This risk drops to 1.02% in second-degree relatives and to 0.88% in third-degree relatives. The risk in monozygotic twins is 25% to 30% compared with 3% to 5% in dizygotic twins. More than 200 genetic risk variants have been identified for MS, with the human leukocyte antigen (HLA) region representing the strongest MS susceptibility locus; the presence of the HLA-DRB1*15:01 allele increases MS risk threefold.1,3,9,10

Many environmental and lifestyle factors have been identified that may increase an individual’s risk for MS development. The timing of exposure to these risk factors may be important; migration studies have shown that key environmental exposures associated with adult-onset MS occur before age 15 years. Environmental exposure and MS risk may also depend on the genetic background of the individual. The most well-established environmental risk factors include Epstein-Barr virus (EBV), tobacco exposure, low sun exposure, low vitamin D levels, and adolescent obesity.3,9-12
Exposure to the EBV, including infectious mononucleosis, especially in adolescence, has been associated with an increased risk of MS. Almost 100% of patients with MS are positive for EBV antibodies. Smoking has consistently been shown to increase the risk of MS. The risk is dose-dependent, with both a higher amount of smoking and cumulative smoking associated with an increased risk. The age at which a person starts smoking does not seem to affect risk, but smoking cessation regardless of the cumulative dose has been correlated with a gradual decline in risk, with the risk approaching zero after 10 years of quitting. Passive exposure to smoking has been associated with an increased risk as well. Smoking has also been linked to a faster disease severity progression, increasing the risk of conversion from RRMS to SPMS and disability progression. MS appears to be more prevalent in geographical regions that are further from the equator. Sun exposure, which decreases with increasing latitude, has been inversely correlated to MS risk. Sun exposure is also a major determinant of vitamin D levels; low levels of vitamin D have been shown to increase the risk of MS and disease activity. Vitamin D supplementation may lower the risk of MS in susceptible individuals. Adolescent obesity doubles the risk of developing MS—especially in females—and has been correlated with an earlier age at the onset of MS.9-12
Clinical Presentation
Symptoms of MS are not unique to the disease itself; almost any neurologic sign or symptom can result from MS. The clinical presentation of MS varies widely and is dependent on where the demyelination occurs. Some patients will present with cognitive changes, while others may experience prominent ataxia, hemiparesis or paraparesis, depression, or visual symptoms. In most patients, disease onset involves a clinically isolated syndrome consisting of an unpredictable neurologic dysfunction due to demyelinating lesions occurring either in the optic nerve, brainstem, or cerebellum, or the cerebral hemisphere. The initial attack is generally mild and self-limiting and is usually recognized as the initial presentation in retrospect once a diagnosis of MS has been determined.10,13
Visual impairment due to optic neuritis is a common initial symptom. Optic neuritis is the first neurologic episode in almost 25% of patients. This is characterized by partial or total vision loss in one eye with a blind spot in the visual field, color vision deficiency, and orbital pain that is worsened by eye movement. Sensory symptoms including paresthesia, Lhermitte sign (sensations of electric shocks radiating down the spine on neck flexion), and decreased pain and light touch perception are experienced by up to 43% of patients initially presenting with MS. Motor manifestations—characterized by pyramidal signs that include spasticity, weakness, Babinski sign, paresis, and hyperreflexia—are the initial presenting symptoms in up to 40% of patients and will affect almost everyone during the course of the disease. Brainstem and cerebellar symptoms affect almost 70% of MS patients. These symptoms include ocular movement impairments, diplopia, ataxia and gait imbalance, slurred speech, and dysphagia. Sphincter and sexual dysfunctions are dependent upon the degree of lower extremity impairment and will eventually affect all patients with MS. Other symptoms include cognitive impairment, fatigue, affective disturbances, and depression.10,13
Management
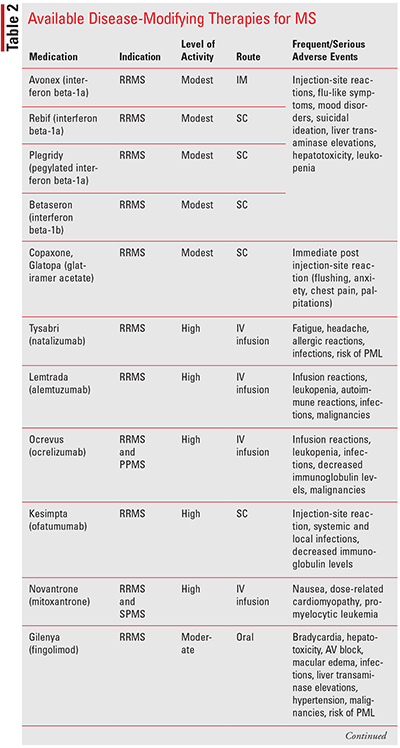
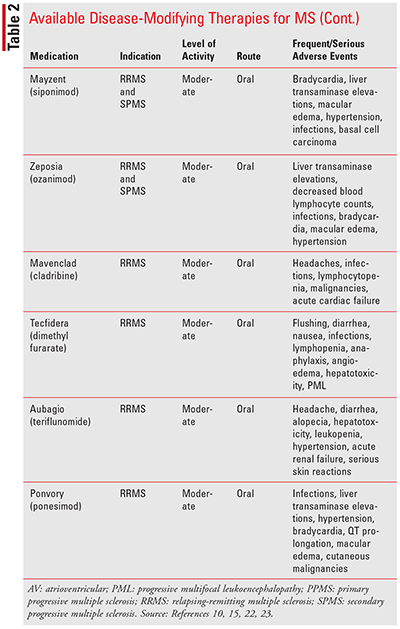
Currently, there is no curative treatment for MS. Treatment is focused on treating relapses, modifying or slowing disease progression, providing symptomatic relief, and maintaining an acceptable quality of life. Acute relapses are commonly managed with a short course of corticosteroids, such as methylprednisolone or dexamethasone administered IV or orally. Disease-modifying therapies (DMTs) have been shown to reduce the frequency and severity of relapses, and reduce the accumulation of lesions, and they can stabilize, delay, or modestly improve disability. Treatment with DMTs should be initiated as early as possible, ideally within 5 years of clinical symptom onset to reduce the risk of disease progression. Currently, there are several injectable, infusion, and oral DMTs available for the treatment of MS (see TABLE 2). These agents have immunosuppressive and immunomodulatory effects targeting lymphocyte number, proliferation, trafficking, and cytokine production, reducing central nervous system inflammation, and preventing disease progression. They have all been found to be effective in RRMS only, except for ocrelizumab, which is the only agent indicated for the management of PPMS as well. They are categorized as moderately effective or highly effective based on their impact on relapses. The selection of the most appropriate DMT for a patient can be challenging and is based on a multitude of factors, including clinical symptoms, MRI activity, agent efficacy, side-effect profile, and patient considerations, which include convenience, cost, and preference. Currently, the dominant treatment strategy used is the escalation regimen. Therapy is started with a less-effective agent and is switched to another lower efficacy agent if the patient experiences intolerable side effects and to a higher-efficacy DMT when disease activity worsens. Common management of MS symptoms, including spasticity, pain, fatigue, cognitive impairment, walking impairment, and bladder and bowel issues, should include a combination of pharmacologic and nonpharmacologic agents. The management of these symptoms is important to improving the quality of life in MS patients and requires a multidisciplinary approach.5,10,13-18
Role of the Pharmacist
An important role of the pharmacist in the management of MS is medication safety, identifying any contraindications to therapy and adverse event risks, and providing patient education about MS and its management. Many agents will require complete blood counts and liver function tests. Other agents will require yearly skin exams to detect malignancies, such as melanoma. Many monitoring parameters are outlined by regulatory agencies, and pharmacists can ensure that the recommended and required monitoring parameters are completed at baseline and before refill authorizations. Before initiating a DMT, a patient’s comorbid conditions should be taken into consideration. For example, interferons should be avoided in patients with a history of depression, and fingolimod should be used with caution or avoided in patients with cardiac complications. By completing a comprehensive medication review for all patients, pharmacists can help identify such conditions that may worsen with the addition of specific DMTs. A comprehensive review also provides the pharmacist an opportunity to speak with the patient one-on-one about MS, the importance of early treatment, and adhering to their regimen. Once therapy has been initiated, pharmacists play an important role in counseling the patient on the appropriate use and adverse effects of the medication.19,20
Pharmacists may also help the healthcare team understand more about the patient’s needs, assess potential drug interactions, and identify potential barriers to adherence. One factor that can affect treatment adherence is cost. MS therapies are very costly, with annual expenses anywhere from $90,000 to $195,000. Many insurance providers require prior authorizations for these products, which can delay treatment start. Most manufacturers provide financial assistance through copay assistance programs to help with out-of-pocket expenses but require submission of documentation. Pharmacists are in a unique position to help patients navigate this very confusing process by assisting them in selecting the most cost-effective option based on the patient’s insurance coverage and financial needs and serving as an advocate for patients to obtain their medications promptly.19-21
Conclusion
MS is a chronic progressive disease with no cure. Management is focused on delaying the disease process. The use of DMTs is the cornerstone of treatment, and pharmacists can be an invaluable resource to both the patient and the interdisciplinary healthcare team. Pharmacists can help patients manage their disease state more effectively by providing education about their therapy, help patients and their caregivers understand the risks and benefits of DMTs and the possible adverse effects, and assist patients in navigating the confusing landscape of insurance prior authorizations and copay assistance programs to obtain their medications in a timely manner.

What Are the Symptoms of MS?
This condition can cause many symptoms, depending on where the nerve damage is. Symptoms may differ greatly from person to person. Common symptoms include numbness, tingling, and feeling of pins and needles; muscle weakness or spasms; vision problems such as double vision, blurriness, partial color blindness, and eye pain; fatigue; trouble with coordination and balance; trouble walking or speaking; trouble thinking clearly; sensitivity to heat; trouble controlling your bowels or bladder; vaginal dryness in women and erectile dysfunction in men; and electric shock sensations when you move your head a certain way.
What Causes MS?
We do not know the exact cause of MS, but it is likely due to genetic and environmental factors. Women are more likely to be affected than men. If one of your parents or siblings has MS, you may be at greater risk. Certain viral infections, such as Epstein-Barr, can trigger the condition. MS is more common in areas that are farther away from the equator. Having low levels of vitamin D and low exposure to sunlight can increase your risk. Smokers are also at higher risk for MS than nonsmokers.
How is MS Treated?
There is currently no cure for MS. Different medicines can be given at different times to help with symptoms. Corticosteroids, such as methylprednisolone, are often used to help manage relapses. To help manage other symptoms such as muscle spasms, urinary problems, pain, depression, and constipation, medicines that are normally taken to help with these conditions are utilized.
The main class of medicines used works at slowing down the disease process. This class of medications is known as disease-modifying therapies. If you have MS, you want to start these medications as soon as possible to prevent further progression and help prevent disability. Many of these medications have significant health risks associated with their use. It is very important that you speak with your healthcare team, including your pharmacist, about the associated risks, adverse effects, and monitoring needs.
Where Can I Go for More Information?
You can contact the following organizations for additional support and resources:
Multiple Sclerosis Foundation (MSF): https://msfocus.org/ or 888-MSFOCUS.
National Multiple Sclerosis Society (NMSS): https://www.nationalmssociety.org/ or 800-344-4867.
Multiple Sclerosis Association of America (MSAA): https://mymsaa.org/ or 800-532-7667.
REFERENCES
1. Reich DS, Lucchinetti CF, Calabresi PA. Multiple sclerosis. N Engl J Med. 2018;378(2):169-180. 2. McGinley MP, Goldschmidt CH, Rae-Grant AD. Diagnosis and treatment of multiple sclerosis: a review. JAMA. 2021;325(8):765-779.
3. Segal BM. Multiple Sclerosis. In: Rich RR, Fleisher TA, Shearer WT, et al, eds. Clinical Immunology (Fifth Edition). Elsevier; 2019:891-902.e1.
4. Wallin MT, Culpepper WJ, Campbell JD, et al. The prevalence of MS in the United States: a population-based estimate using health claims data. Neurology. 2019;92(10):e1029-e1040.
5. Leary S, Porter B, Thompson A. Multiple sclerosis: diagnosis and the management of acute relapses. Postgrad Med J. 2005;81(955):302-308.
6. Wexler M. Economic burden of MS in US exceeded $85B in 2019. ECTRIMS2021. www.multiplesclerosisnewstoday.com/news-posts/2021/10/18/ectrims2021-economic-burden-ms-us-exceeded-85b-2019/. Accessed January 26, 2022.
7. Zwibel HL, Smrtka J. Improving quality of life in multiple sclerosis: an unmet need. Am J Manag Care. 2011;17:S139-S145.
8. Motl RW, Goldman MD, Benedict RH. Walking impairment in patients with multiple sclerosis: exercise training as a treatment option. Neuropsychiatr Dis Treat. 2010;6:767-774.
9. Kamm CP, Uitdehaag BM, Polman CH. Multiple sclerosis: current knowledge and future outlook. Eur Neurol. 2014;72(3-4):132-141.
10. Filippi M, Bar-Or A, Piehl F, et al. Multiple sclerosis. Nat Rev Dis Primers. 2018;4(1):43.
11. Waubant E, Lucas R, Mowry E, et al. Environmental and genetic risk factors for MS: an integrated review. Ann Clin Transl Neurol. 2019;6(9):1905-1922.
12. Jakimovski D, Guan Y, Ramanathan M, et al. Lifestyle-based modifiable risk factors in multiple sclerosis: review of experimental and clinical findings. Neurodegener Dis Manag. 2019;9(3):149-172.
13. Saguil A, Kane SF, Edwin A. Farnell IV. Multiple sclerosis: a primary care perspective. Am Fam Physician. 2014;90(9):644-652.
14. Ross AP. Management of multiple sclerosis. Am J Manag Care. 2013;19(16):S301-S306. www.ajmc.com/view/ace014_nov13_ms-ce_ross. Accessed January 29, 2022.
15. Hauser SL, Cree BAC. Treatment of multiple sclerosis: a review. Am J Med. 2020;133(12):1380-1390.e2.
16. Rae-Grant A, Day GS, Marrie RA, et al. Practice guideline recommendations summary: disease-modifying therapies for adults with multiple sclerosis: report of the Guideline Development, Dissemination, and Implementation Subcommittee of the American Academy of Neurology. Neurology. 2018;90(17):777-788.
17. DeAngelis F, John NA, Brownlee WJ. Disease-modifying therapies for multiple sclerosis. BMJ. 2018;363:k4674.
18. Samjoo IA, Worthington E, Drudge C, et al. Efficacy classification of modern therapies in multiple sclerosis. J Comp Eff Res.2021;10:495-507.
19. Schultz J, Weber C, Kamholz J. Letter to the editor: the emerging role of pharmacists in the multidisciplinary care of patients with multiple sclerosis. Int J MS Care. 2016;18(5):219-220.
20. Habibi M, Kuttab HM. Management of multiple sclerosis and the integration of related specialty pharmacy programs within health systems. Am J Health-Syst Pharm. 2016;73(11):811-819.
21. Kaltwasser J. MS spending spiked over the past decade as costly DMTs emerged, reports at ISPOR show. www.ajmc.com/view/ms-spending-spiked-over-the-past-decade-as-costly-dmts-emerged-reports-at-ispor-show. Accessed February 3, 2022.
22. Ponesimod (Ponvory) for multiple sclerosis. The Medical Letter, Inc. August 9, 2021. www.secure.medicalletter.org/article-share?a=1630c&p=tml&title=Ponesimod%20(Ponvory)%20for%20Multiple%20Sclerosis&cannotaccesstitle=1. Accessed February 3, 2022.
23. Drugs for Multiple Sclerosis. The Medical Letter, Inc. March 22, 2021. www.secure.medicalletter.org/article-share?a=1620b&p=tml&title=Drugs%20for%20Multiple%20Sclerosis&cannotaccesstitle=1. Accessed February 3, 2022.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





