US Pharm. 2017;42(2):5-7.
Heart disease (HD) is the leading cause of death in the United States and is responsible for claiming five times as many women as breast cancer over a lifetime.1,2 In particular, acute myocardial infarction (MI), or heart attack, is an acute obstruction of a coronary artery resulting in necrosis of the myocardial muscle. While symptoms include chest pain or discomfort with or without dyspnea, nausea, and diaphoresis, pharmacists should be aware that 20% of acute MIs are silent; women and patients who have diabetes are more likely to pre-sent with atypical symptoms, such as shortness of breath, pressure or pain in the lower chest or upper abdomen, dizziness, light-headedness or fainting, upper back pressure, or extreme fatigue.3,4
While positive outcomes with drugs and treatments for acute MI require prompt intervention—ideally at the first sign of distress—according to the Women’s Heart Foundation (WHF) about one-third of women do not experience chest pain when having a heart attack.2 Furthermore, 71% of women report flu-like symptoms for about 2 weeks to 1 month prior to experiencing more acute chest discomfort or severe shortness of breath.2
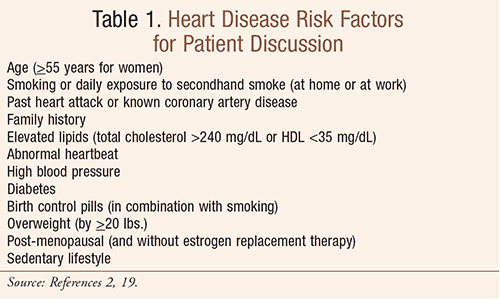
A lack of public awareness may contribute to the fact that the milder symptoms of an MI experienced by some women are underreported to staff in emergency departments. Pharmacists can certainly assist in educating women by helping them to become familiar with the risk factors for heart disease (TABLE 1) and the warning signs of a heart attack (TABLE 2), while encouraging and empowering them with the knowledge and confidence that seeking emergency treatment is critical for the effectiveness of lifesaving drugs and treatments. This article provides an overview of MI treatment and outcomes to assist in that process.
Gender, Care, and Outcomes
Men and women have differences in the mechanisms and pathophysiology of HD.5 There are a significant number of women who have normal arteries upon angiogram but actually show biochemical or imaging evidence of MI.6 More than one--third of women with MI, despite having no demonstrable coronary artery disease, show plaque rupture and ulceration upon examination with intravascular ultrasound.7
Research has shown that female patients who present with MI are, on average, older than male patients and have more comorbidities (e.g., smoking, obesity, hypertension, diabetes, poor mental health) and lower income.8,9 One study found a pathophysiological difference involving women and men regarding pulmonary capillary wedge pressure that was independent of age, hypertension status, or infarct size, suggesting that it is largely gender-dependent.10 Some pathophysiological differences may be associated with differences in MI symptomology and options available for revascularization.11,12
Women are more likely than men to experience delays between the onset of symptoms and arrival at the hospital; there are also gender differences in the delays between onset of symptoms and the initiation of guideline-based treatment and the use of various surgical (e.g., revascularization) and pharmacologic treatments.5 Of note, despite variations in healthcare and culture outside the U.S., outcomes are similar for women internationally.5
Research presented at the 2015 annual meeting of the American Heart Association indicated that women are less likely than men to get the recommended treatments for MI survivors.13 Researchers found that women were 8% less likely to be on an optimal regimen when discharged; suboptimal post-MI care accounts for the gender gap in MI patients’ long-term survival.
Women, on average, have worse outcomes than men following MI, with more complications, higher mortality rates, and poorer recovery.5 In a recent peer-reviewed report from the Aetna Foundation and the University of Connecticut School of Medicine regarding current trends and outcomes, Graham indicated that disparities exist and persist in the cardiovascular care of women.5 This has proven to be the case even when categories of income, educational level, and site of care are taken into consideration, and despite recent general improvements in healthcare.1,14 Gender differences have been observed regarding MI, including risk assessment, disease awareness, comorbidities, presentation, treatment, and outcomes.5 Graham concludes that because women differ in MI presentation symptoms and physiology, avenues for both diagnosing and treating MI must be developed in a gender-dependent fashion.5
Reinforcing Emergency Status
Women are more likely than men to experience delays between the onset of MI symptoms and arrival at the hospital.5 Pharmacists have an opportunity to guide their patients, family members, friends, colleagues, and other healthcare professionals about the dos and don’ts of seeking care for a heart attack. Ultimately, it’s about stressing the patient’s emergency status and not delaying getting emergency care. And while this may seem fundamental, women often underestimate the situation when they experience milder symptoms of a heart attack.
According to the WHF, if a woman even suspects she is having a heart attack, she should:
• Call 911
• State “I am having a heart attack”
• Chew an uncoated aspirin immediately to reduce heart-muscle damage
• Be taken by EMTs to the nearest medical facility that has 24-hour emergency cardiac care. (She should not drive herself). Even if she is not sure that the pain is serious, it is recommended to go to the emergency room to find out
• Get treatment quickly. Do not wait, since clot-buster medicine and coronary angioplasty work best when provided after the first signs of distress
• Understand that every minute counts, so get to the emergency room without delay.
When possible, after calling 911, individuals can prepare for the paramedics’ arrival by15:
• Staying on the line
• Unlocking the front door
• Containing pets in a different room
• Sitting or lying down and loosening any restrictive clothing
• Having a cell phone with emergency contacts at hand
• Informing paramedics whom to contact if a family member or caregiver is not aware of the situation.
What to Expect in the ER
Upon presentation, all patients are given aspirin 160 mg to 325 mg (not enteric-coated) if not contraindicated.3 Diagnosis is by ECG and cardiac markers (i.e., serum markers of myocardial cell necrosis) including cardiac enzymes (e.g., creatine kinase-MB) and cell contents (e.g., troponin I, troponin T, myoglobin); the markers appear at different times following injury, and levels decrease at varying rates.16
Coronary angiography most often combines diagnosis with percutaneous coronary intervention (PCI)—which includes angioplasty and stent placement.16 Emergency coronary angiography and PCI are done as soon as possible after the onset of acute MI. These procedures have significantly lowered morbidity and mortality and improved long-term outcomes; often, the MI is aborted when the time from pain to PCI is less than 3 to 4 hours.16
Medications discussed below are employed in patients with acute MI unless contraindicated.3 Antiplatelet drugs used include aspirin, clopidogrel, or both (prasugrel and ticagrelor are used as alternatives to clopidogrel). Anticoagulants are given to patients with unstable angina. Heparin may be given (unfractionated or low-molecular-weight heparin); in patients with a known or suspected history of heparin-induced thrombocytopenia, bivalirudin is recommended. Beta-blockers, ACE inhibitors, and statins are considered standard therapy for all patients with unstable angina. High-risk patients may require glycoprotein IIb/IIIa inhibitor therapy (e.g., abciximab, tirofiban, eptifibatide). Chest pain can be treated with nitroglycerin (sublingually, then by continuous IV drip if necessary) or morphine (IV every 15 minutes as needed); elevation of the lower extremities can combat morphine-induced hypotension and bradycardia. For a summarized overview of reperfusion therapy in acute MI, see Reference 3.
Following recovery, it is imperative that the following medications be initiated or continued, in most cases, unless contraindicated: aspirin and other antiplatelet drugs, beta-blockers, ACE inhibitors, and statins.16 Rehabilitation and post-discharge treatment (TABLE 3) also include a functional evaluation and changes in lifestyle that incorporate regular exercise, diet modification, weight loss, and smoking cessation.3,13

Conclusion
While symptoms of acute MI include chest pain or discomfort with or without dyspnea, nausea, and diaphoresis, women are more likely to present with atypical MI symptoms and are overall less likely to present with chest pain.5 It has recently been suggested that educational approaches specifically tailored to women may assist in reducing the incidence of MI, as well as improving post-hospitalization outcomes; furthermore, in order to observe continued improvement, gender-specific consideration may be required.5
REFERENCES
1. CDC. National Center for Health Statistics. Leading causes of death. October 7, 2015. www.cdc.gov/nchs/fastats/leading-causes-of-death.htm. Updated October 7, 2016. Accessed January 20, 2017.
2. Women’s Heart Foundation. Heart attack symptoms: an action plan for women. A healthy hearts guide. www.womensheart.org/content/HeartAttack/heart_attack_symptoms_risks.asp. Accessed January 6, 2017.
3. MerckManuals.com. Acute myocardial infarction (MI). Revised September 2016. www.merckmanuals.com/professional/cardiovascular-disorders/coronary-artery-disease/acute-myocardial-infarction-mi. Accessed January 10, 2016.
4. American Heart Association. Heart attack symptoms in women. Updated January 10, 2017. www.heart.org/HEARTORG/Conditions/HeartAttack/WarningSignsofaHeartAttack/Heart-Attack-Symptoms-in-Women_UCM_436448_Article.jsp. Accessed January 17, 2017.
5. Graham G. Acute coronary syndromes in women: recent treatment trends and outcomes. Clin Med Insights Cardiol. 2016;10:1-10.
6. Cenko E, Bugiardini R. Vasotonic angina as a cause of myocardial ischemia in women. Cardiovasc Drugs Ther. 2015;29(4):339-345.
7. Reynolds HR, Srichai MB, Iqbal SN, et al. Mechanisms of myocardial infarction in women without angiographically obstructive coronary artery disease. Circulation. 2011;124(13):1414-1425.
8. Yu J, Mehran R, Grinfeld L, et al. Sex--based differences in bleeding and long term adverse events after percutaneous coronary intervention for acute myocardial infarction: three year results from the HORIZONS-AMI trial. Catheter Cardiovasc Interv. 2015;85(3):359-368.
9. Pelletier R, Humphries KH, Shimony A, et al. GENESIS-PRAXY Investigators. Sex--related differences in access to care among patients with premature acute coronary syndrome. CMAJ. 2014;186(7):497-504.
10. Dreyer RP, Beltrame JF, Neil C, et al. Cardiac hemodynamics in men versus women during acute ST--segment elevation myocardial infarction. Am J Cardiol. 2013;112(2):143-149.
11. De Ferrari GM, Fox KA, White JA, et al. Outcomes among non--ST--segment elevation acute coronary syndromes patients with no angiographically obstructive coronary artery disease: observations from 37,101 patients. Eur Heart J Acute Cardiovasc Care. 2014;3(1):37-45.
12. Patel MR, Chen AY, Peterson ED, et al. Prevalence, predictors, and outcomes of patients with non--ST--segment elevation myocardial infarction and insignificant coronary artery disease: results from the Can Rapid risk stratification of Unstable Angina patients Suppress ADverse outcomes with Early implementation of the ACC/AHA Guidelines (CRUSADE) initiative. Am Heart J. 2006;152(4):641-647.
13. AHA: women more often receive suboptimal post-MI care. HealthDay News. November 10, 2015. www.merckmanuals.com/professional/news/external/2015/11/10/17/54/aha-women-more-often-receive-suboptimal-post-mi-care. Accessed January 9, 2017.
14. Cook NR, Paynter NP, Eaton CB, et al. Comparison of the Framingham and Reynolds risk scores for global cardiovascular risk prediction in the multiethnic Women’s Health Initiative. Circulation. 2012;125(14):S1711-1741.
15. Cobb C. Have an exit plan. In: Detz J. 10 ways to live longer. Family Circle. February 2017. www.familycircle.com/health/concerns/heart/10-ways-to-live-longer/?page=3. Accessed January 20, 2017.
16. MerckManuals.com. Overview of acute coronary syndromes (ACS). Revised September 2016. www.merckmanuals.com/professional/cardiovascular-disorders/coronary-artery-disease/overview-of-acute-coronary-syndromes-acs#true. Accessed January 16, 2017.
17. Boudi B. Risk factors for coronary artery disease. Medscape.com. Updated: November 27, 2016. http://emedicine.medscape.com/article/164163-overview. Accessed January 9, 2017.
18. Sousa C, Rocha A, Rangel I, et al. Functional capacity benefits of cardiac rehabilitation after acute coronary syndrome are sustained in time and independent of left ventricle systolic function. Eur Heart J. http://eurheartj.oxfordjournals.org/content/34/suppl_1/P5795. Accessed January 17, 2017. E-pub Aug. 1 2013.
19. National Heart, Lung, and Blood Institute. What are the risk factors for heart disease? Updated July 10. 2014. www.nhlbi.nih.gov/health/educational/hearttruth/lower-risk/risk-factors.htm. Accessed January 31, 2017.
To comment on this article, contact rdavidson@uspharmacist.com.






