US Pharm. 2022;47(10):24-30.
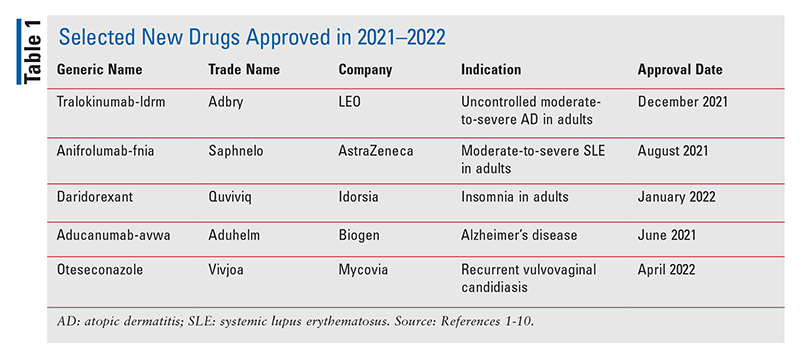
New molecular entities (NMEs), as defined by the FDA, are new drug products containing as their active ingredient a chemical substance marketed for the first time in the United States. The following descriptions of NMEs approved in 2021–2022 (TABLE 1) detail the basic clinical and pharmacologic profiles of each new drug, as well as key precautions and warnings. Also included is a brief summary of selected pharmacokinetic, adverse-reaction, drug-interaction, and dosing data submitted to the FDA in support of the manufacturer’s New Drug Application. This review is intended to be objective rather than evaluative in content. The information for each NME was obtained primarily from sources published prior to FDA approval. Experience clearly demonstrates that many aspects of an NME’s therapeutic profile are not detected in premarketing clinical studies and emerge after the drug is used in the broader population. For example, previously unreported adverse reactions become apparent for some NMEs within several years of their marketing. Some NMEs may eventually acquire at least one black box warning for serious adverse drug reactions or are withdrawn from the market for safety reasons that were not recognized at the time of approval. Therefore, while this review offers an introduction to some new drugs, it is essential that practitioners be aware of changes in their therapeutic profiles as reported in the pharmaceutical literature and by patients.
Tralokinumab-ldrm (Adbry, LEO)
Indication and Clinical Profile1,2: The FDA approved tralokinumab-ldrm for the treatment of moderate-to-severe atopic dermatitis (AD) in adults whose disease is not well controlled with topical medications or when those therapies are not advisable. AD, also known as atopic eczema, is a chronic relapsing inflammatory skin condition characterized by dry skin, itching (especially at night), and red to brownish-gray patches on various portions of the body. The incidence of AD has increased nearly threefold in industrialized nations, impacting approximately 15% to 20% of children and 1% to 3% of adults worldwide. Tralokinumab-ldrm, the first biological agent approved for the management of AD, functions by inhibiting interleukin (IL)-13, a key inflammatory mediator in this disease. Tralokinumab-ldrm may be used with or without topical corticosteroids.
Approval of this drug was based on efficacy and safety results from three double-blind, placebo-controlled, multinational phase III trials (ECZTRA 1, ECZTRA 2, and ECZTRA 3) that included more than 1,500 adult patients. Patients received injections of tralokinumab-ldrm 300 mg every other week, alone or with topical corticosteroids. The primary endpoints were an Investigator’s Global Assessment score of 0 or 1 (IGA 0/1) at week 16, and ³75% improvement in Eczema Area and Severity Index (EASI 75) at week 16. Patients achieving IGA 0/1 and/or EASI 75 with tralokinumab-ldrm at week 16 were re-randomized to tralokinumab-ldrm every 2 or 4 weeks or placebo for up to 36 weeks. At week 16, more tralokinumab-ldrm patients than placebo patients achieved IGA 0/1 (38.9% vs. 26.2%) and EASI 75 (56.0% vs. 35.7%). Of week 16 responders, 89.6% and 92.5% of those who were treated with tralokinumab-ldrm every 2 weeks and 77.6% and 90.8% of those who were treated with tralokinumab-ldrm every 4 weeks, respectively, maintained IGA 0/1 and EASI 75 at week 32. Among patients who did not achieve IGA 0/1 and EASI 75 with tralokinumab-ldrm at 16 weeks, 30.5% and 55.8%, respectively, achieved these endpoints at week 32.
Pharmacology and Pharmacokinetics1,2: Tralokinumab-ldrm is a human immunoglobulin (Ig) G4 monoclonal antibody that specifically binds to human IL-13 and inhibits its interaction with the alpha-1 and alpha-2 subunits of this receptor. IL-13, a cytokine typically produced by a type 2 immune response, promotes the release of proinflammatory cytokines, chemokines, and IgE implicated in AD.
The absolute bioavailability of tralokinumab-ldrm is estimated to be 76%, with a time to maximum plasma concentration (Tmax) of 5 to 8 days post administration. The volume of distribution is estimated to be 4.2 L. Tralokinumab-ldrm appears to undergo peptide metabolism. It has a half-life of 3 weeks, and systemic clearance is estimated to be 0.149 L/day.
Adverse Reactions and Drug Interactions1,2: Common adverse events reported with tralokinumab-ldrm during clinical trials included eosinophilia, eye and eyelid inflammation, upper respiratory tract infections, and injection-site reactions. Patients are advised to report new-onset or worsening eye symptoms, such as conjunctivitis or keratitis, to their healthcare provider. Serious hypersensitivity reactions—including anaphylaxis—and angioedema have occurred, requiring drug discontinuation. Tralokinumab-ldrm can compromise the efficacy of antihelminth therapies; therefore it should not be initiated or continued in patients with preexisting helminth infection or those who become infected during treatment. The use of live vaccines should be avoided during tralokinumab-ldrm therapy.
In terms of drug interactions, a small clinical trial evaluating tralokinumab-ldrm’s effects on the pharmacokinetics of midazolam (CYP3A4 substrate), warfarin (CYP2C9 substrate), omeprazole (CYP2C19 substrate), metoprolol (CYP2D6 substrate), and caffeine (CYP1A2 substrate) observed no significant changes in exposure (AUC or Cmax) of the CYP450 substrates after multiple tralokinumab administrations compared with tralokinumab-ldrm administered alone.
Dosage and Administration1,2: Tralokinumab-ldrm is available in a 150-mg/mL prefilled syringe for SC injection. The recommended dosage is an initial dose of 600 mg (four 150-mg injections), followed by 300 mg (two 150-mg injections) administered every other week. After 16 weeks of treatment, a dosage of 300 mg every 4 weeks may be considered in patients with body weight <100 kg who achieve clear or almost-clear skin. All age-appropriate vaccinations, as recommended by current immunization guidelines, should be completed prior to treatment initiation.
Anifrolumab-fnia (Saphnelo, AstraZeneca)
Indication and Clinical Profile3,4: Anifrolumab-fnia is a type I interferon (IFN) receptor antagonist approved for the treatment of moderate-to-severe systemic lupus erythematosus (SLE) in adults receiving standard therapy. The safety and efficacy of anifrolumab-fnia were established in three multinational, placebo-controlled clinical trials: MUSE, TULIP-1, and TULIP-2. MUSE was a phase II study whose primary endpoints included assessment of the SLE Responder Index (SRI-4) and sustained reduction in oral corticosteroids (OCS) measured at week 24. A total of 305 patients were randomized 1:1:1 to receive anifrolumab-fnia 300 mg, anifrolumab-fnia 1,000 mg, or placebo. The phase III TULIP-1 and TULIP-2 studies had a primary outcome of improvement in disease activity evaluated at 52 weeks, measured by SRI-4 in TULIP-1 and by the British Isles Lupus Assessment Group based Composite Lupus Assessment (BICLA) in TULIP-2. Secondary outcomes of TULIP-1 and TULIP-2 included maintenance of OCS reduction, improvement in cutaneous SLE activity, and flare rate.
BICLA response rates at week 52 were reported in all three trials but were primary endpoints only in TULIP-2. The difference in response rates was 28.8% for MUSE, 17% for TULIP-1, and 16.3% for TULIP-2. SRI-4 response rates at week 52 were 24% for MUSE, 6% for TULIP-1, and 18.2% for TULIP-2. Anifrolumab-fnia did not demonstrate a statistically significant difference in response rates in TULIP-1.
Pharmacology and Pharmacokinetics3,4: Anifrolumab-fnia is an immunoglobulin (Ig) G1-kappa monoclonal antibody that binds to subunit 1 of the type I IFN receptor (IFNAR1), inhibiting its activity. Reduction in the activity of type I IFNs reduces its role in the pathogenesis of SLE. Anifrolumab-fnia also acts to internalize IFNAR1, reducing available receptors. These mechanisms of action result in a reduction of the inflammation and immunologic processes that contribute to the pathology of SLE.
Anifrolumab-fnia exhibits nonlinear pharmacokinetics over the dose range of 100 mg to 1,000 mg every 4 weeks, resulting in greater AUC exposure as the dose increases. The volume of distribution in the typical SLE patient (69.1 kg) is estimated to be 6.23 L. Based on standard dosing, the clearance of anifrolumab-fnia 300 mg IV every 4 weeks was estimated to be 0.193 L/day.
Adverse Reactions and Drug Interactions3,4: The most common (>10%) adverse reactions with anifrolumab-fnia were infections (70% of patients), including influenza, urinary tract infection, tuberculosis, bronchitis, and (34% incidence) upper respiratory tract infections (i.e., nasopharyngitis, pharyngitis, and sinusitis). The incidence of serious infections during treatment was 5%. At present, data on the use of anifrolumab-fnia in human pregnancy are limited and are insufficient to inform on the drug-associated risk of major birth defects, miscarriage, or adverse maternal or fetal outcome. Monoclonal IgG antibodies are known to be actively transported across the placenta as pregnancy progresses; therefore, fetal exposure to anifrolumab-fnia may be greater during the third trimester.
The only reported contraindication with anifrolumab-fnia is severe hypersensitivity (e.g., anaphylaxis) to anifrolumab or any component of its formulation. Clinically notable adverse reactions of concern are serious infections, hypersensitivity reactions including anaphylaxis, and malignancy. To date, no formal drug-interaction studies have been conducted.
Dosage and Administration3,4: Anifrolumab-fnia is supplied as a single-dose vial containing 300 mg/2 mL (150 mg/mL). The recommended dosage is 300 mg administered as an IV infusion over 30 minutes. Prior to administration, anifrolumab-fnia must be diluted with 0.9% Sodium Chloride Injection, USP, using aseptic technique. A 2-mL volume of 0.9% Sodium Chloride Injection is withdrawn from a 100-mL infusion bag, and 2 mL of anifrolumab-fnia is added with gentle mixing to equal a total volume of 100 mL. The infusion solution should be administered immediately after preparation over a 30-minute period through an infusion line containing a sterile, low-protein binding 0.2- or 0.22-micron in-line filter. After completion of the infusion, the line must be flushed with 25 mL of 0.9% Sodium Chloride Injection, USP.
Daridorexant (Quviviq, Idorsia)
Indication and Clinical Profile5,6: Daridorexant was approved for treatment of adults with insomnia characterized by difficulty with sleep onset and/or sleep maintenance. Insomnia, the most common sleep disorder (occurring in >30% of U.S. adults), is defined as difficulty obtaining sufficient sleep and dissatisfaction with sleep combined with a significant negative impact on daytime function. Chronic insomnia is considered difficulty initiating and/or maintaining sleep at least 3 nights/week for at least 3 months. Insomnia, which appears to result from overactivity of the areas of the brain that are associated with wakefulness, has significant effects on the sufferer’s mood, energy level, and ability to concentrate. Furthermore, long-term insomnia is associated with serious health conditions, such as psychiatric disorders, cardiovascular disease, type 2 diabetes, substance abuse, and dementia.
The efficacy of daridorexant was assessed in two equally randomized, multicenter, placebo-controlled trials: Study 1 and Study 2. A total of 1,854 subjects with insomnia as defined by the Diagnostic and Statistical Manual of Mental Disorders, 5th edition, received daridorexant or placebo once daily in the evening for 3 months. Study 1 assigned 930 subjects to daridorexant 25 mg, daridorexant 50 mg, or placebo; Study 2 assigned 924 subjects to daridorexant 25 mg, daridorexant 10 mg, or placebo. At the end of the 3-month treatment period, both studies included a 7-day placebo run-out period, after which subjects could enter an extension study. A total of 600 subjects were treated for at least 6 months; of these, 373 were treated for at least 12 months. Primary efficacy endpoints for both studies were the change from baseline to months 1 and 3 in latency to persistent sleep (LPS, time to sleep induction) and wake after sleep onset (WASO, sleep maintenance), measured objectively by polysomnography in a sleep laboratory. In Study 1, daridorexant 25 mg and daridorexant 50 mg showed statistically significant improvements versus placebo in LPS and WASO and in self-reported total sleep time (sTST) at month 1 and month 3. The 50-mg dose also demonstrated significant reduction in daytime sleepiness versus placebo—as measured by the sleepiness domain score from the Insomnia Daytime Symptoms and Impacts Questionnaire 7—at months 1 and 3, a key secondary endpoint. In Study 2, the 25-mg dose showed a statistically significant improvement versus placebo in WASO and sTST at months 1 and 3, but the 10-mg dose did not.
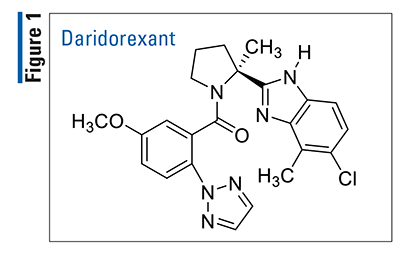
Pharmacology and Pharmacokinetics5,6: Orexin A and orexin B are neuropeptides secreted by neurons, mainly in the lateral hypothalamus. These neuropeptides elicit their effects by binding to and activating two G-protein–coupled receptors (GPCRs): orexin receptor type 1 and orexin receptor type 2 (OX1R, OX2R). Orexin receptor pathways play vital regulatory roles in many physiological processes, including the sleep-wake rhythm. Daridorexant (FIGURE 1) is benzimidazole-pyrrolidine designed to function as a dual antagonist at OX1R and OX2R, thereby suppressing the wake-promoting activity of orexin A and orexin B.
The oral bioavailability of daridorexant is 62%, and peak plasma concentrations occur within 1 to 2 hours (Tmax). Daridorexant has a volume of distribution of 31 L, and it is 99.7% bound to plasma proteins. Daridorexant undergoes extensive metabolism, primarily by CYP3A4 (89%). The primary route of excretion is via the feces (57%); a smaller fraction is excreted in the urine (28%), primarily as metabolites. The terminal half-life of daridorexant is approximately 8 hours. Daridorexant’s rapid absorption for sleep onset, as well as its clearance profile resulting in 80% elimination after a night of sleep, may minimize the residual effects.
Adverse Reactions and Drug Interactions5,6: The most common adverse reactions associated with daridorexant in clinical trials(>5%, and greater than placebo) were headache and somnolence or fatigue. The product label also includes a warning about worsening depression and suicidal thoughts as well as complex sleep behaviors including sleepwalking, sleep-driving, and engaging in other activities while not fully awake (e.g., preparing/eating food, making phone calls, having sex). Patients should contact their healthcare provider immediately if they experience any of these adverse effects. Hallucinations and sleep paralysis (temporary inability to move or talk) lasting up to several minutes may occur when the patient is falling asleep or waking. Daridorexant is contraindicated in patients with narcolepsy.
No data are available on daridorexant use in pregnant women to determine drug-associated risks of major birth defects, miscarriage, or other adverse maternal or fetal outcomes. In animal reproduction studies, daridorexant did not cause fetal toxicity at doses up to eight to 10 times the maximum recommended human dose. No data exist on the presence of daridorexant in human milk, effects on the breastfed infant, or effects on milk production, but the drug and its metabolites were detected in the milk of lactating rodents. Therefore, infants potentially exposed to daridorexant through breastmilk should be monitored for excessive sedation. Daridorexant is a federally controlled substance because it can be abused and may lead to dependence.
Dosage and Administration5,6: Daridorexant is supplied as 25-mg and 50-mg film-coated tablets for oral administration. The recommended dosage is 25 mg to 50 mg once per night, taken within 30 minutes before going to bed and with at least 7 hours remaining prior to planned awakening. The time to sleep onset may be delayed if daridorexant is taken with or soon after a meal. Daridorexant should not be taken with other central nervous system depressants or alcohol. Patients also should be advised to avoid driving, operating heavy machinery, or performing any activity that requires clear thinking while still experiencing the effects of the drug. In patients with moderate hepatic impairment, the maximum recommended dosage is 25 mg no more than once per night. Daridorexant is not recommended in patients with severe hepatic impairment. Concomitant use of daridorexant with strong inhibitors of CYP3A4 should be avoided, and the dose should limited to 25 mg in patients on concurrent therapy with moderate CYP3A4 inhibitors. The concomitant use of daridorexant with moderate-to-strong CYP3A4 inducers should also be avoided.
Aducanumab-avwa (Aduhelm, Biogen)
Indication and Clinical Profile7,8: Aducanumab-avwa is an amyloid-beta (AB)–directed antibody indicated for the treatment of Alzheimer’s disease, and it is the first new treatment for this disease since 2003. Approval was granted under the accelerated approval process used for drugs that provide a meaningful therapeutic advantage over existing treatments for a serious or life-threatening illness. Continued approval for this indication is contingent upon verification of clinical benefit in confirmatory trials. Alzheimer’s disease, an irreversible, debilitating, and progressive brain disorder affecting 6.2 million Americans, slowly erodes memory, thought, and—eventually—the ability to carry out even simple tasks. Although what specifically causes it is not fully known, Alzheimer’s disease is characterized by brain changes, including amyloid plaques and neurofibrillary (tau) tangles, that result in a loss of neurons in critical brain regions that regulate memory and thought. Currently available therapies treat only the symptoms of the disease, but aducanumab-avwa is the first agent that targets and alters the presumed process underlying Alzheimer’s disease.
Accelerated approval of aducanumab-avwa was based on results from three double-blind, placebo-controlled, dose-ranging trials that included a total of 3,482 patients with mild cognitive impairment or mild dementia stage of Alzheimer’s disease. The studies, known as EMERGE (Study 1), ENGAGE (Study 2), and PRIME (Study 3), used positron emission tomography to quantify AB plaque in brain regions implicated in Alzheimer’s disease pathology versus brain regions not involved in the disease. Patients receiving aducanumab-avwa had significant dose-dependent and time-dependent reductions in AB plaque (59%-71% across studies), whereas controls had no reduction of AB plaque. To date, there are no safety or efficacy data on initiating aducanumab-avwa treatment at earlier or later stages of Alzheimer’s disease.
Pharmacology and Pharmacokinetics7,8: Aducanumab-avwa is a human immunoglobulin-gamma (IgG) 1 monoclonal antibody that is capable of crossing the blood-brain barrier to selectively target and bind aggregated soluble oligomers and insoluble fibril conformations of AB plaques in the brain. Biochemical studies have shown that aducanumab-avwa binds selectively to a linear epitope formed by AB amino acids 3 to 7, thereby minimizing interactions with other proteins. Based on weak monovalent affinity, fast binding kinetics, and strong avidity for epitope-rich aggregates, aducanumab-avwa has been shown to discriminate between AB monomers and oligomeric or fibrillar aggregates.
Steady-state concentrations of aducanumab-avwa are reached by 16 weeks of repeated dosing with an every-4-week regimen. The peak concentration (Cmax), trough concentration (Cmin), and area under the plasma concentration versus time curve at steady state increase in a dose-proportional manner over the standard dosing range (1-10 mg/kg every 4 weeks). The estimated volume of distribution at steady state is 9.6 L. Similar to endogenous IgG, aducanumab-avwa is presumed to be hydrolyzed to small peptides, and eventually amino acids, by protein catabolic pathways. The terminal half-life of aducanumab-avwa is about 25 days. No studies evaluating pharmacokinetics in patients with renal or hepatic impairment have been reported, but the drug is not expected to undergo renal elimination or hepatic metabolism. Variations in body weight, age, sex, and race may result in altered drug exposure but were not found to significantly impact clinical response.
Adverse Reactions and Drug Interactions7,8: The most commonly reported adverse reactions with aducanumab-avwa include amyloid-related imaging abnormalities (ARIA); headache; falls; diarrhea; and confusion, disorientation, and altered mental status. The product label includes a warning for ARIA, which most commonly present as a temporary swelling of parts of the brain; this effect usually resolves over time and is not known to cause symptoms. However, some trial patients with ARIA reported headache, confusion, dizziness, vision changes, or nausea attributed to aducanumab-avwa. Rarely, the use of aducanumab-avwa has been associated with hypersensitivity reactions, including angioedema and urticaria.
Dosage and Administration7,8: Aducanumab-avwa is supplied as a preservative-free, sterile solution for IV injection in single-dose vials of 170 mg/1.7 mL (100 mg/mL) and 300 mg/3 mL (100 mg/mL). After an initial titration (over 6 weeks), the recommended dosage is 10 mg/kg as an IV infusion over approximately 1 hour every 4 weeks, at least 21 days apart. Initial titration involves administration of 1 mg/kg doses for infusions 1 and 2; 3 mg/kg doses for infusions 3 and 4; and 6 mg/kg doses for infusions 5 and 6. Dose adjustments for renal or hepatic impairment are not anticipated.
Oteseconazole (Vivjoa, Mycovia)
Indication and Clinical Profile9,10: Oteseconazole is the first and only medication indicated specifically for reducing the incidence of recurrent vulvovaginal candidiasis (RVVC) in females with a history of RVVC who are not of reproductive potential. Its use is contraindicated in pregnant and lactating women. RVVC, commonly known as chronic yeast infection, is defined as three or more symptomatic acute episodes of yeast infection within a 12-month period. Symptoms include vaginal itching, burning, irritation, and inflammation, and some patients experience abnormal vaginal discharge and painful urination or sexual intercourse. It is estimated that 75% of adult women will have at least one yeast infection in their lifetime, and approximately 50% will experience recurrence; of these women, up to 90% will develop RVVC. The FDA granted oteseconazole Fast-Track and Qualified Infectious Disease Product designations.
Oteseconazole was approved based on efficacy data from three phase III clinical trials including 875 patients from 232 sites in 11 countries. In the two global VIOLET studies, 93% to 96% of women with RVVC who received oteseconazole did not have recurrence in the 48-week maintenance period; in contrast, 57% to 61% of placebo recipients did not experience recurrence. In the U.S.-based ultraVIOLET study, 89.7% of women with RVVC who received oteseconazole cleared their initial yeast infection and had no recurrence for the 50-week maintenance period, whereas 57.1% of those who received fluconazole and placebo had no recurrence.
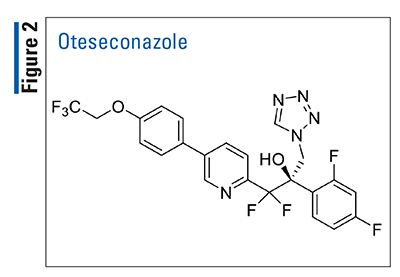
Pharmacology and Pharmacokinetics9,10: Oteseconazole (FIGURE 2) is a novel tetrazole antifungal derivative that inhibits 14-alpha-demethylase (CYP51), a fungal enzyme that catalyzes an early step in the biosynthesis of the essential fungal sterol ergosterol. Furthermore, inhibition of 14-alpha-demethylase results in the accumulation of 14-methylated sterols, which are toxic to fungi. Because of the incorporation of a tetrazole metal-binding group into its structure, oteseconazole has reduced affinity for human CYP enzymes and, presumably, better adverse-reaction and drug-interaction profiles.
Time to peak plasma concentrations of oteseconazole is in the range of 5 to 10 hours. Administration with a high-fat, high-calorie meal increased Cmax and AUC0-72h by 45% and 36%, respectively, but no significant differences were observed with a low-fat, low-calorie meal. Oteseconazole’s volume of distribution is approximately 423 L, and the drug is >99% bound to plasma proteins. Animal studies indicate that oteseconazole exposures in vaginal tissue are comparable to plasma exposures. Oteseconazole does not undergo significant metabolism. Approximately 56% of the oral dose is excreted in feces by biliary excretion, and 26% is excreted in urine. The median terminal half-life of oteseconazole is approximately 138 days.
Adverse Reactions and Drug Interactions9,10: The most frequently reported adverse reactions were headache and nausea, which occurred in 7.4% and 3.6%, respectively, of trial participants. Adverse reactions reported in <2% of patients in clinical trials included dyspepsia, hot flush, dysuria, reproductive-system disorders (menorrhagia, metrorrhagia, vulvovaginal irritation), and increased blood creatine phosphokinase. Oteseconazole was found to cause fetal harm in animal studies; therefore, it is contraindicated in females of reproductive potential as well as in pregnant and lactating women because of potential risks to a fetus or breastfed infant. Oteseconazole is also contraindicated in patients with known hypersensitivity to the drug.
Oteseconazole is a breast cancer resistance protein (BCRP) inhibitor, and concurrent use with BCRP substrates such as rosuvastatin may increase the exposure of the substrate, increasing the risk of adverse reactions associated with these agents. Therefore, it is recommended that the lowest effective initial and maintenance doses of a BCRP substrate be used if it is administered concurrently with oteseconazole, and the patient should be monitored for adverse reactions.
Dosage and Administration9,10: Oteseconazole is available as 150-mg hard gelatin capsules for oral administration. There are two recommended dosage regimens: 1) oteseconazole alone and 2) oteseconazole plus fluconazole. The product label provides detailed dosing schedules for these regimens. No dosage adjustments are recommended in patients with mild-to-moderate renal impairment or mild hepatic impairment; however, oteseconazole is not recommended in patients with severe renal impairment or end-stage renal disease (with or without dialysis) or in those with moderate or severe hepatic impairment.
REFERENCES
1. Adbry (tralokinumab-ldrm) package insert. Madison, NJ: LEO Pharma Inc; July 2022.
2. Wollenberg A, Howell MD, Guttman-Yassky E, et al. Treatment of atopic dermatitis with tralokinumab, an anti-IL-13 mAb. J Allergy Clin Immunol. 2019;143(1):135-141.
3. Saphnelo (anifrolumab-fnia) package insert. Wilmington, DE: AstraZeneca Pharmaceuticals LP; July 2022.
4. Anifrolumab: drug information. UpToDate. Waltham, MA: UpToDate; 2022. www.uptodate.com. Accessed June 28, 2022.
5. Quviviq (daridorexant) package insert. Radnor, PA: Idorsia Pharmaceuticals US Inc; April 2022.
6. Markham A. Daridorexant: first approval. Drugs. 2022;82(5):601-607.
7. Aduhelm (aducanumab-avwa) package insert. Cambridge, MA: Biogen Inc; June 2021.
8. Sevigny J, Chiao P, Williams L, et al. Aducanumab (BIIB037), an anti-amyloid beta monoclonal antibody, in patients with prodromal or mild Alzheimer’s disease: interim results of a randomized, double-blind, placebo-controlled, phase 1b study. Alz Dementia. 2015;11(7 suppl 6):P277.
9. Vivjoa (oteseconazole) package insert. Durham, NC: Mycovia Pharmaceuticals, Inc; April 2022.
10. Sobel JD, Nyirjesy P. Oteseconazole: an advance in treatment of recurrent vulvovaginal candidiasis. Future Microbiol. 2021;16(18):1453-1461.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.






