US Pharm. 2018;43(6):6-10.
Lipomas are considered the most common soft-tissue tumors, occurring in 1% of the population.1 Because more than half of lipomas encountered by clinicians are subcutaneous in location, pharmacists may be the initial healthcare practitioner consulted by trusting patients for their opinion and advice about whether or not to seek medical attention. In this regard, pharmacists should have an awareness of and knowledge about this benign tumor of adipose tissue that is associated with a genetic predisposition and usually develops in adults aged between 40 and 60 years.2 An adult aged more than 65 years may have a lipoma that has been slow-growing for years, possibly causing physical discomfort or distress about its appearance.
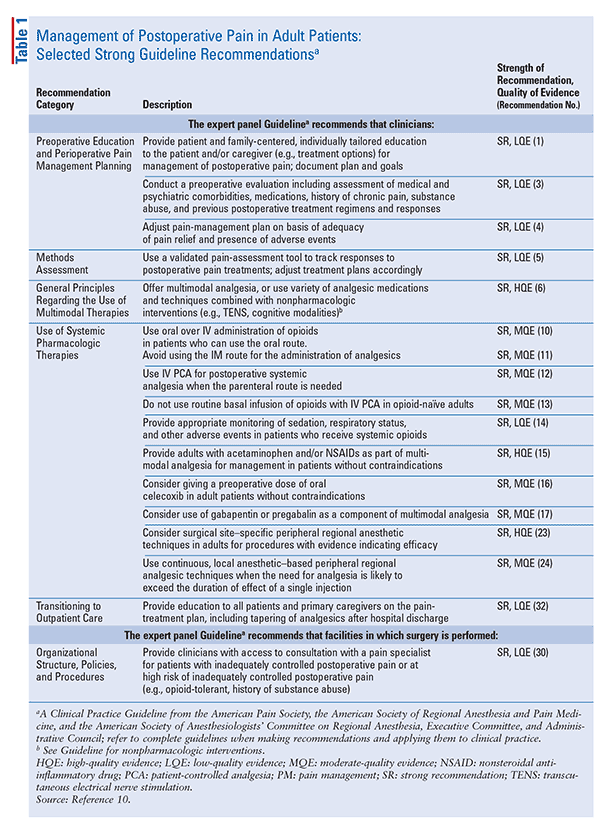
Importantly, pain associated with surgical procedures is a major concern for patients, and its management is an integral component of the increasing emphasis on clinical outcomes and quality of care.3 Furthermore, pharmacists can provide evidence-based recommendations for anticipating and treating acute postsurgical pain (APSP) associated with the removal of a subcutaneous lipoma while reducing or avoiding the use of opioids in older adults. This article outlines expert-panel guidelines, including strong recommendations for multimodal analgesia or the use of a variety of analgesic medications combined with nonpharmacologic interventions (transcutaneous electrical nerve stimulation, cognitive modalities) for the treatment of postoperative pain in adults (TABLE 1).
Clinical Presentation
Lipomas are common benign tumors that are usually located in the subcutaneous tissues. Slow-growing (i.e., over months or years), these fatty tumors develop into soft, lobulated masses that are encapsulated by thin fibrous tissue.1 Lipomas can occur almost anywhere on the body, but are typically found on the trunk, shoulders, neck, and armpits, with some people having more than one.1,4 Rarely, lipomas may develop in other locations, such as in muscles and internal organs (e.g., retroperitoneum, gastrointestinal tract, heart, and pericardium).1,4,5 To the touch, a lipoma feels doughy and typically is not tender; with slight finger pressure, it will move readily.2 In most cases, a lipoma is diagnosed with physical examination; if it is large and/or painful, other tests, including biopsy, CT scan and MRI, may be ordered to rule out malignancy.4
While most lipomas are small (i.e., usually less than 2 inches across) and removed purely for cosmetic reasons, some may reach almost 8 inches across.1,4 The type of surgery required to remove a lipoma will be determined by the location, size, and depth into the skin or extent of the tumor (e.g., superficial—between skin and muscle, attaching to muscle). Procedures to remove lipomas are usually done under local anesthesia and patients go home the same day.4 Resection of lipomas frequently requires incisions equal to the diameter of the tumor; side effects of surgery include residual hypoesthesia and chronic pain at the incision site.6 Recently, a minimally invasive technique for the removal of subcutaneous lipoma has been described by Sakamoto and colleagues, involving a small incision and the preservation of retaining ligaments, which may contain cutaneous nerves.6 Lipomas removed for cosmetic reasons usually have limited scarring; for larger lipomas, liposuction can be useful; however, the procedure is associated with a higher rate of recurrence.4
Various types of surgeons would be qualified to remove a lipoma; the best choice would probably depend on the location of the lesion. A lipoma in the head and neck area could be removed by a facial plastic surgeon, plastic surgeon, otolaryngologist, head and neck surgeon, or general surgeon; plastic surgeons are particularly well qualified in techniques to minimize scarring. A lipoma on another part of the body would likely be treated by a plastic surgeon, general surgeon, or dermatologic surgeon, depending on the above-noted determining features.
Of note, since subcutaneous lipomas are more common in patients with Wilson disease than in the general population, it has been suggested that the presence of lipomas should contribute to the differential diagnosis of Wilson disease.7 It is more probable that lipomas are at the benign end of the spectrum of tumors, which, at the malignant end, include liposarcomas.1
Cancerous tumors in fatty tissues grow rapidly, don’t move under the skin, and are usually painful. Importantly, this supports the pharmacist’s recommendation that the patient visit the primary care provider for evaluation of suspected lipoma.2
Postsurgical Pain Management
With regard to postsurgical pain management, pharmacists should be aware of risk factors to identify patients at high risk for pain (TABLE 2). Educating patients about APSP with videos or audio-accompanied slides also improves patient attitudes toward APSP.8 Furthermore, monitoring pain before and after treatment (particularly pain that occurs while the individual is in motion) is an absolute necessity for 1) identifying the effectiveness of pain treatment; 2) promoting activity after surgery; and 3) reducing complications.8 Taking a multimodal approach to managing APSP can effectively attenuate APSP and reduce patient opioid requirements.9,10 Multimodal analgesia, defined as the use of a variety of analgesic medications and techniques that target different mechanisms of action in the peripheral and/or central nervous system, may have additive or synergistic effects and more effective pain relief compared with single-modality interventions; it may also be combined with nonpharmacologic interventions.10
For a review of the anatomy of pain, presurgical pain management, and pain management during surgery, including choosing local anesthesia (e.g., less cardiotoxic anesthetics such as lidocaine and mepivacaine) for patients with high-risk cardiac disease or who are taking medications such as beta-blockers, digitalis preparations, and calcium channel blockers, consult Reference 8.
Systemic Pharmacologic Therapies
Acetaminophen and nonsteroidal anti-inflammatory drugs: Acetaminophen is the most commonly used pain medication for minor dermatologic procedures.8 Nonsteroidal anti-inflammatory drugs (NSAIDs) are also commonly recommended for mild-to-moderate pain; they are capable of reducing pain by about 50% and significantly reduce future opioid requirements.8,10 Postoperatively, acetaminophen, usually dosed at 500 to 1,000 mg by mouth every 6 hours (no clear difference between IV and oral), and NSAIDs (e.g., celecoxib 200 mg twice daily in adult patients without contraindications) are recommended as an intervention, with suggested use as a component of multimodal analgesia; this recommendation is known to reduce the use of postoperative opioids.10
Acetaminophen/NSAID contraindications and cautions: for acetaminophen, hepatotoxicity; for NSAIDs, gastrointestinal bleeding and ulceration, cardiovascular events, and renal dysfunction. Tailoring medications and dosages based on age, the current medication regimen, renal and hepatic function, and the Beers Criteria is helpful in developing a treatment plan in older adults.
While gabapentin and pregabalin may be considered opioid-sparing as a component of multimodal analgesia, these drugs were mainly studied in patients who underwent major surgery, and may be problematic at effective doses; considerations include the possibility of increased sedation at higher doses, dizziness, and the need for a reduced dose in patients with renal dysfunction (TABLE 1).10 More research is necessary regarding new or nontraditional combinations such as gabapentin and ibuprofen.3,8,9
Opioids: Minimizing the number of central nervous system (CNS)-active drugs in an older adult’s medication regimen, or preferably avoiding these drugs—including opioid-receptor agonist analgesics—is recommended to avoid drug-drug interactions involving two or more CNS-active drugs that may contribute to falls.11 While opioids are indicated for moderate-to-severe pain, in reality they are frequently used for mild-to-moderate pain as well.8 A preoperative evaluation to determine preoperative opioid use and doses should be conducted, if applicable. Opioid use is also complicated because of poor tolerance (codeine has been removed from many formulations) and because of the high risk that patients will develop opioid dependence. For these reasons, opioids should be second-line therapy in dermatologic surgery.8
When necessary, oral opioids are used as a component of multimodal analgesia, underscoring oral as the preferred route for patients who can take oral medications. Contraindications and cautions include respiratory depression, potential for addiction and abuse, sedation, nausea and vomiting, and constipation.10 Pharmacists should consult Table 4 in Reference 10 for guidelines on the management of postoperative pain in patients receiving long-term opioid therapy.
Use of Ice or Gel Cold Packs
It has been suggested, based on small studies, that ice or gel cold packs at the site during or after surgery decrease pain and/or use of opioids in the first few days after surgery; more research should be conducted regarding the use of this simple and low-cost technique for decreasing APSP.8
Conclusion
Lipomas are common benign tumors usually located in the subcutaneous tissues. Since accessible pharmacists may be consulted by patients asking if they should seek medical attention, knowledge about these adipose masses is helpful whether or not pain or discomfort is a presenting symptom. Researchers have found that combined medications, such as acetaminophen and an NSAID or opioid and nonopioid pain relievers, have shown effectiveness in pain treatment. Pharmacists can provide evidence-based recommendations for anticipating and treating acute postsurgical pain associated with the removal of a subcutaneous lipoma, while reducing or avoiding the use of opioids in older adults, if appropriate.
REFERENCES
1. Nickloes TA. Lipomas. Medscape.com. Updated June 8, 2017. https://emedicine.medscape.com/article/191233-overview. Accessed April 18, 2018.
2. Lipoma. Mayoclinic.org. April 3, 2018. www.mayoclinic.org/diseases-conditions/lipoma/diagnosis-treatment/drc-20374474. Accessed April 26, 2018.
3. Meeks NM, Glass JS, Carroll BT. Acute pain management in dermatology: mechanisms and pathways. J Am Acad Dermatol. 2015;73(4):533-540.
4. Lipomas. Clevelandclinic.org. November 27, 2017. https://my.clevelandclinic.org/health/diseases/15008-lipomas. Accessed April 26, 2018.
5. Naseerullah FS, Javaiya H, Murthy A. Cardiac lipoma: an uncharacteristically large intra-atrial mass causing symptoms. Case Rep Cardiol. 2018;2018:3531982.
6. Sakamoto A, Okamoto T, Matsuda S. Subcutaneous lipomas: a minimally invasive method for resection of subcutaneous lipomas preserving retaining ligaments. Eur J Plast Surg. 2018;41(2):173-176.
7. Schaefer M, Gotthardt DN, Didion C, et al. Increased prevalence of subcutaneous lipomas in patients with Wilson disease. J Clin Gastroenterol. 2015;49(7):e61-e63.
8. Stiles L. Guidelines for treating pain after dermatologic surgery. October 23, 2015. www.clinicalpainadvisor.com/acute-pain/guidelines-for-treating-pain-after-dermatologic-surgery/article/448974/4/. Accessed April 16, 2018.
9. Glass JS, Hardy CL, Meeks NM, et al. Acute pain management in dermatology: risk assessment and treatment. J Am Acad Dermatol. 2015;73(4):543560.
10. Guidelines on the management of postoperative pain. J Pain. 2016;17(2):131-157.
11. Reuben DB, Herr KA, Pacala JT, et al. Geriatrics at Your Fingertips: 2016. 18th ed. New York, NY: The American Geriatrics Society; 2016:21.
To comment on this article, contact rdavidson@uspharmacist.com.