US Pharm.
2007;1:56-61.
Normal
pressure hydrocephalus (NPH) is a neurologic condition that is considered
vastly underdiagnosed, as it typically induces symptoms similar to those seen
in other forms of dementia. Some key symptoms associated with NPH also exist
in other neurologic diseases, including Alzheimer's disease (AD), Parkinson's
disease (PD), and vascular dementia. In fact, it has been estimated that
375,000 Americans who suffer from NPH have been misdiagnosed with dementia or
PD.1 Additionally, some experts believe that between 1% and 10% of
elderly persons living in the community and as many as 6% of nursing home
residents have NPH; this is much higher than the number of persons actually
diagnosed.2 Because NPH is treatable and considered a reversible
form of dementia, early and appropriate diagnosis and treatment are essential
for optimal clinical outcomes. Pharmacists working with the elderly both in
nursing homes and the community should be aware of NPH, its signs and
symptoms, and the impact of the disease on those who suffer from it.
NPH was first described in
1965 by Adams et al. as a condition that involved various neurologic symptoms,
ventricular enlargement, and what appears to be "normal" cerebrospinal fluid
(CSF) pressure upon lumbar puncture.2 The cardinal symptoms of NPH
are known as the Adams triad: gait disturbance, dementia, and urinary
difficulties.3 The classic theory is that the CSF pressure does not
increase in NPH because the ventricles expand to accommodate the increased CSF
volume; therefore, the pressure appears normal. Another theory is that the
pressure temporarily increases when the ventricles are inflating but
normalizes after they equilibrate. This is similar to inflating a balloon:
Increased pressure is required to inflate the balloon, but at maximum size,
the pressure is maintained at a reduced or seemingly normal pressure. By the
time clinical symptoms develop, the ventricles will have already enlarged, and
the pressure might have already normalized. Thus, checking the CSF pressure
will not aid in confirming a diagnosis. The lack of elevated CSF pressure, as
seen in other forms of hydrocephalus, lends to the difficulty in diagnosing
NPH.
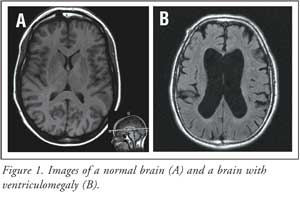
The resulting ventriculomegaly
is thought to cause the triad of symptoms by compressing or stretching nerves
in various areas of the brain, thus leading to improper neuronal signaling.
Figure 1 illustrates both a brain with normal-sized ventricles and one
with ventriculomegaly.
Pathophysiology
When the brain
functions properly, CSF is produced by the choroid plexus at a rate of 20 to
25 mL per hour. The CSF then circulates from the lateral ventricles through
the midline third ventricle and finally into the fourth ventricle found within
the posterior fossa of the brain. From the fourth ventricle, CSF exits the
ventricular system and enters the subarachnoid space surrounding the brain and
spinal cord, where it acts as a cushion to help prevent brain injury. The CSF
is normally reabsorbed by the arachnoid villi and passed into the venous
sinuses at the same rate of CSF production to maintain consistent circulation
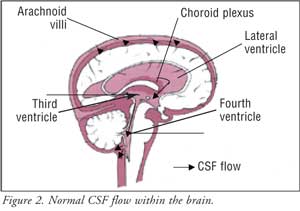
and pressure.3 Figure 2 illustrates the normal flow of CSF
in the brain. In patients with NPH, however, CSF is not adequately reabsorbed,
causing excessive accumulation of fluid in the brain and leading to the triad
of symptoms.
The excessive CSF within the brain
can result from either idiopathic changes or trauma, with about 50% of
patients in each category.2 Although the disrupted reabsorption of
CSF by the arachnoid villi is not fully understood, some theories have
implicated the accumulation of scar tissue. It is believed that scar tissue
either decreases the ability of CSF to be absorbed properly through the
arachnoid villi, or that scar tissue surrounding the venous sinuses in the
brain impedes CSF from entering the bloodstream. Head or brain surgery,
intracranial hemorrhage, and meningitis have been associated with NPH.3
Unfortunately, the progression of NPH is often slow, obscuring an exact
etiopathology.
Clinical Presentation
NPH can occur at
any age; however, it is typically more common among the elderly, most
frequently in the sixth or seventh decade of life.4 Although
symptoms of the Adams triad are strongly linked to advanced NPH, they may not
all be present in early stages of the disease in these patients.5
One of the earliest symptoms is gait abnormalities, which are generally
described as either shuffling (short strides), magnetic (difficulty raising
legs), or broad based (legs far apart for stability).2 Regardless
of which gait abnormality is present, patients with NPH tend to fall backward
when walking without support.
Impaired gait can further
contribute to urinary problems such as incontinence, when worsening of
mobility increases the walking time to the bathroom. Urinary problems can
present as increased urinary frequency, urgency, or incontinence, depending on
level of disease.2
Cognitive decline, unlike gait
and urinary symptoms, tends to be gradual in patients with NPH. Symptoms
typically include psychomotor slowing, verbal difficulties, and deficits in
executive function.2 Hypersomnia can be present in up to 40% of NPH
patients.2 Behavioral disturbances such as depression and agitation
can also occur but are infrequent.
Differential Diagnosis
The nonspecific
symptoms associated with NPH require careful evaluation to avoid misdiagnosing
NPH as a neurologic disorder such as AD, PD, or vascular dementia. Since the
onset and severity of symptoms among the various forms of dementia vary
widely, making a diagnosis requires the ability of a skilled diagnostician. In
patients with NPH, changes in gait, urinary difficulty, and cognitive decline
are not always present initially. An abnormal gait can occur both in NPH and
PD; however, the stance of patients with PD is typically narrow, whereas the
stance of patients with NPH is wider. NPH patients often lack cogwheel
rigidity, lack a resting tremor, and do not respond to levodopa therapy.2
The onset and character of gait disturbances in patients with NPH also differ
from those seen in patients with AD. Gait disturbances in patients with AD do
not precede cognitive decline as they do in patients with NPH. In addition,
NPH patients usually lack the apraxia typically seen in AD patients.
Urinary disturbances are
exacerbated by the gait changes with NPH; however, urinary incontinence may
result from a variety of other complications unrelated to dementing illness.
People with NPH can have bladder control difficulties that range from
increased urgency or increased frequency to incontinence. The bladder-related
issues observed in NPH are similar to those seen in AD, PD, and vascular
dementia but might not be directly related to these conditions. Thus, patients
presenting with urinary symptoms should always be evaluated for infection,
prostate disease (in men), or stress incontinence before a neurologic cause is
suspected.
Although cognitive impairment
in AD, PD, vascular dementia, and NPH overlap, the characteristics of each
disorder are distinct. Cognitive impairment associated with NPH is typically
characterized by decreased verbalization, planning skills, and initiative,
2 whereas behavioral issues, such as agitation, aggressiveness,
delusions, and hallucinations, are rarely linked to NPH. However, these
symptoms are more commonly seen in PD, AD, and vascular dementia. Cognitive
impairment among AD patients is usually characterized by agnosia and aphasia,
which are not normally associated with NPH patients. Cognitive impairment
associated with vascular dementia typically occurs in a stepwise fashion as a
result of stroke. With each stroke, a person's cognitive impairment worsens,
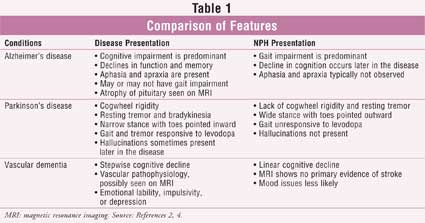
whereas in NPH, this decline tends to be more linear. Table 1 provides
a comparison of features seen with NPH and other common forms of dementia.
Diagnostic Tests
Both computed tomography (CT) scans
and magnetic resonance imaging can be used to diagnose NPH; however, there are
no reliable criteria for confirming a diagnosis with either method.2
Some elderly patients experience normal enlargement of the ventricles that is
independent of NPH; thus, the ventricles might seem enlarged only because the
brain has atrophied or shrunk. In such cases, the pressure and the flow
pattern of the CSF will be normal.2 The radiologist can, however,
rule out NPH by confirming an increased Evans ratio (i.e., the ratio of the
frontal horns compared with the width of the skull as measured from the inner
calvarial table). Non-NPH dementias with ventriculomegaly are usually
associated with an increase in the Evans ratio. Radiologists should examine
the hippocampus for atrophy or confirm an increase in CSF volume.
Cisternography, one of the
main tests used to diagnose NPH, relies on CT monitoring of radionucleotides
injected into the subarachnoid space via spinal tap. The ventricular reflux of
radionucleotides is monitored with CT intermittently over a four-day period.
2,4 Owing to the poor reabsorption of CSF in NPH patients, it is thought
that the radionucleotide dye will not be readily absorbed as it would in
non-NPH patients.2 For those in whom a diagnosis of NPH remains
possible, a lumbar puncture should also be performed. There are two options: a
one-time lumbar puncture or a continuous lumbar drainage. Before the lumbar
puncture is performed, a gait test is administered, during which the patient
walks 50 feet while being videotaped. Then, at least 30 mL of CSF is removed,
and the gait is reevaluated. After the lumbar puncture, an immediate
improvement is usually seen in patients with true NPH; however, in some cases,
a few days may be required before an improvement occurs.2 With
continuous lumbar drainage, the CSF is allowed to drain for two to three days,
during which the patient is periodically assessed for clinical improvement.
This is believed to be a more reliable method of confirming a diagnosis of NPH.
2
Treatment Options
Acetazolamide is a possible
pharmacologic treatment option for NPH because it can help to reduce CSF
secretion. Although some reports indicate it is an effective treatment for
NPH, clinical results have not been encouraging.6 The most
effective treatment for NPH is CSF shunting. Lumbar peritoneal,
ventriculopleural, ventriculoatrial, and ventriculoperitoneal (VP) shunts are
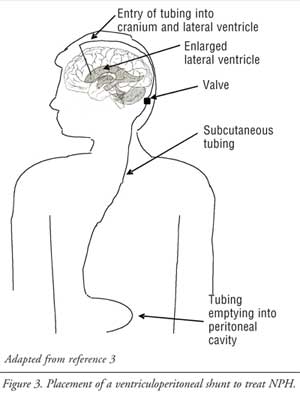
available; however, the VP shunt is the most commonly used.6 The VP
shunt requires placing a catheter within the ventricles and attaching it to a
valve just under the scalp. Another catheter, tunneled subcutaneously, leads
from the valve to the peritoneal cavity, where the CSF drains and is readily
absorbed (Figure 3).3 In addition to multiple types of
shunts, there are two valve options: the fixed valve and the programmable
valve. The traditional fixed valve has multiple settings, but after
implantation, adjustment of the valve speed requires surgery and valve
replacement. The newer programmable valve allows for modifications without
invasive surgery to adjust the amount of CSF drained.6 This newer
valve technique allows for adjustments based on clinical benefit. Shunt
placement involves several risks, including shunt malfunction (20%), subdural
hematoma (2% to 17%), seizures (3% to 11%), infection (3% to 6%), and
intracerebral hematoma (3%).5,6
Summary
NPH is a neurologic syndrome
associated with the Adams triad: abnormal gait, urinary difficulty, and
symptoms of dementia. The symptoms of NPH are often similar to those seen in
various forms of dementia, including AD, PD, or vascular dementia. Unlike
other forms of dementia, NPH is reversible if treated early and appropriately.
The timely implantation of a VP shunt to divert CSF from the brain has been
shown to reverse the dementia and other symptoms associated with NPH, provided
it is performed before damage from the enlarging ventricles has occurred.
Because NPH is a reversible disease that is often mistaken for other
nonreversible neurologic disorders, it is important that pharmacists and other
members of the health care team become familiar with this condition and that
they learn to distinguish it from other dementing illnesses.
REFERENCES
1. Boschert S. Excess CSF can mimic Parkinson's disease, dementia: normal pressure hydrocephalus, typically undiagnosed, can be treated with a shunt. Intern Med News. 2004;37(14):1-2.
2. Bejjani GK, Hammer MD. Normal-pressure hydrocephalus: another treatable "dementia": part I. Contemp Neurosurg. 2005;27(16):1-6.
3. Byrd C. Normal pressure hydrocephalus: dementia's hidden cause. Nurse Pract. 2006;31:28-29, 31-35.
4. Factora R. When do common symptoms indicate normal pressure hydrocephalus? Cleve Clin J Med. 2006;73:447-450, 452, 455-456 passim.
5. Gallia GL, Rigamonti D, Williams MA. The diagnosis and treatment of idiopathic normal pressure hydrocephalus. Nat Clin Pract Neurol. 2006;2:375-381.
6. Bejjani GK, Hammer MD.
Normal-pressure hydrocephalus another treatable "dementia": part II.
Contemp Neurosurg. 2005;27(17):1-6.
To comment on this article, contact
editor@uspharmacist.com.





