US Pharm. 2021;7(46):4-12.
ABSTRACT: Historically, the inhaled route of medication administration has been associated with the delivery of bronchodilators and/or corticosteroids to treat pulmonary conditions such as chronic obstructive pulmonary disease and asthma. However, this modality of drug delivery is increasingly being explored for use in other disease states, as drug inhalation is associated with several benefits including decreased systemic side effects, higher bioavailability, and more rapid absorption into the body. Certain inhaled medications that are used on- and off-label are encountered less frequently in daily medical practice than conventional bronchodilators. The most common on-label indications for inhaled medications include pulmonary arterial hypertension and pulmonary infections. The most reported off-label uses of inhaled medications include pulmonary infections, acute respiratory distress syndrome, pulmonary hemorrhage, and post–lung transplant.
Inhaled medications have been used to treat pulmonary conditions for over 70 years. Historically, inhaled therapies (bronchodilators, corticosteroids) were used only for obstructive lung diseases (asthma, chronic obstructive pulmonary disease [COPD]). More recently, inhaled therapies have been incorporated into the treatment of selected orphan pulmonary diseases (cystic fibrosis, pulmonary arterial hypertension) and systemic diseases (diabetes).1,2 Advantages of aerosol administration of therapies include needle-free delivery; more rapid absorption into the systemic circulation; avoidance of first-pass metabolism; lower incidence of systemic side effects; and higher bioavailability than other routes of administration.1-3 Ongoing advances in technology have resulted in smaller medication-particle size with more efficient drug delivery and a multitude of delivery devices with various advantages and disadvantages.
Clinicians are most familiar with inhaled medications for the acute and chronic treatment of asthma and COPD. Traditional bronchodilators (short-acting beta agonists, long-acting beta agonists, short-acting antimuscarinics, long-acting antimuscarinics, and inhaled corticosteroids) are endorsed as monotherapy and/or combination therapy in current evidence-based treatment guidelines for these conditions.4-6 These products are commercially available as metered-dose inhalers, soft-mist inhalers, dry-powder inhalers, and solutions for nebulization. Clinicians may be less familiar with available inhalation therapies used to treat other, less-frequently encountered pulmonary conditions and/or systemic, nonpulmonary diseases.
Here we review therapies that are approved by the FDA for inhalation, as well as therapies that may be prescribed for inhalation despite lacking specific FDA approval for inhaled administration. For each agent, a description of the inhalation therapy, delivery device, and dose will be discussed. Because the development and application of off-label inhalation therapies may be based upon case reports or small case series, information regarding stability, dosing, and the optimal inhalation delivery device is typically lacking. Therefore, we will limit our discussion of non-FDA–approved inhalation therapies to their clinical application(s).
CURRENT TREATMENTS FDA-APPROVED FOR INHALATION
Insulin
Since the introduction of SC insulin administration in the 1920s, patients have desired a safe, convenient, needle-free insulin product. More than 80 years later, in 2006, Exubera was approved to treat diabetes mellitus types 1 and 2, representing one of the first attempts to use an inhaled medication to treat a systemic disease.7 The spray-dried insulin powder in this formulation was stable at room temperature for at least 24 months. Exubera was contraindicated in smokers and those patients with poorly controlled lung disease; patients were required to have periodic pulmonary function testing (PFT) while on therapy. Because hypoglycemia was the most common side effect of Exubera, regular blood-sugar monitoring was required with therapy. While considered a breakthrough therapy when it was launched, Exubera captured less than 1% of the insulin market within its first 2 years on the market and therefore was taken off the market in October 2007 by Pfizer due to poor sales. Factors contributing to its poor uptake in practice included accelerated rate of PFT decline compared with placebo; a safety label for lung malignancies; an inconvenient inhaler design (roughly the size of a can of tennis balls); unconventional dosing (in milligrams as opposed to international units); and low bioavailability (required fivefold-higher insulin dose to achieve the same metabolic effect as injection).8-10
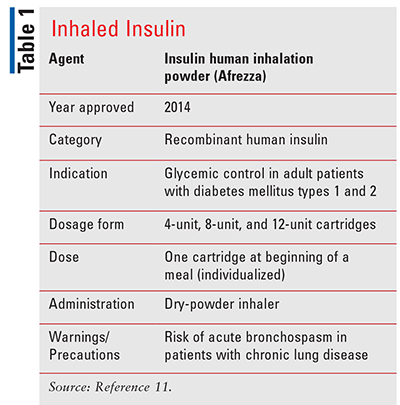
Afrezza (TABLE 1), an inhaled preparation of rapid-acting recombinant regular human insulin powder, was approved by the FDA in 2014 after it demonstrated improved glycemic control in adults with diabetes mellitus types 1 and 2.11 The Afrezza inhaler device is substantially smaller than Exubera and is dosed in IU. Afrezza is administered as a single inhalation at the beginning of a meal. The dose is individualized per patient need via single-use cartridges of 4 units, 8 units, and 12 units administered as a breath-powered inhaler. This product should not be used in smokers and carries a black box warning for acute bronchospasm in patients with chronic lung disease such as asthma or COPD. PFT should be performed before Afrezza initiation. The most common adverse effects (affecting ³2% of treated patients) include hypoglycemia, cough, and throat pain/irritation. Afrezza must be refrigerated during storage (2-8°C, 36-46°F); any unrefrigerated product must be used within 10 days. The Afrezza inhaler can be used for up to 15 days from the date of first use. After 15 days of use, the device must be discarded and replaced.11
Antimicrobial Agents
Inhaled antimicrobials are used to manage cystic fibrosis, noncystic fibrosis bronchiectasis, nontuberculous mycobacteria, and selected fungi and viruses. Antimicrobials approved by the FDA for inhalation include amikacin, aztreonam, tobramycin, pentamidine, and ribavirin.12
Amikacin liposome inhalation suspension (Arikayce; TABLE 2) is an aminoglycoside antibacterial agent solely indicated for adults who do not achieve negative sputum cultures after 6 months of oral Mycobacterium avium complex therapy.13 This product is supplied as single-dose glass vials containing 590 mg/8.4 mL and must be used with the Lamira Nebulizer System. The manufacturer recommends that the suspension should be refrigerated (2°-8°C, 36°-46°F). However, it may be kept at room temperature (<25°C; <77°F) for up to 4 weeks: thereafter, unused doses must be discarded. Adverse reactions (affecting >10% of treated patients) include dysphonia, cough, bronchospasm, hemoptysis, musculoskeletal pain, upper airway irritation, ototoxicity, fatigue/asthenia, exacerbation of underlying pulmonary disease, diarrhea, nausea, and headache. A boxed warning describes increased risk of hospitalizations for respiratory adverse reactions including hypersensitivity pneumonitis, hemoptysis, bronchospasm, and exacerbation of underlying pulmonary disease. Close monitoring of patients with neuromuscular disorders is encouraged as aminoglycosides may block the release of acetylcholine at the neuromuscular junction.13
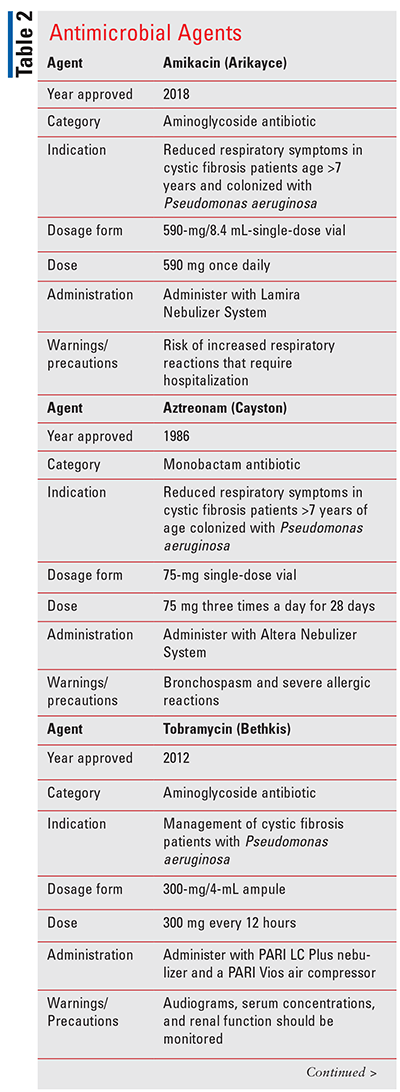
Aztreonam for inhalation solution (Cayston; TABLE 2) is a monobactam antibacterial agent used in cystic fibrosis patients to treat P aeruginosa infections.14 Doses are made from one lyophilized aztreonam vial containing 75 mg of antibiotic and one 1 mL ampule of 0.17% sodium-chloride diluent. The aztreonam vials and diluent ampules must be refrigerated (2°-8°C, 36°-46°F) for storage. They may be kept at room temperature (<25°C; <77°F) for up to 4 weeks: unused doses must be discarded after that. Dosing is one vial, nebulized three times daily for a total of 28 days via the Altera Nebulizer System, and doses should be used immediately after mixing. Common adverse reactions (>5%) include cough, nasal congestion, bronchospasm, pharyngolaryngeal pain, pyrexia, chest discomfort, abdominal pain, and vomiting. Severe allergic reactions to aztreonam inhalation have also been reported.14
Tobramycin inhalation solution (Bethkis; TABLE 2) is an aminoglycoside antibiotic used to treat P aeruginosa infections in patients with cystic fibrosis.15 This formulation is a solution in single-use 4 mL ampules containing 300 mg of tobramycin. It should be concealed from light and refrigerated (2°-8°C, 36°-46°F) during storage. Bethkis pouches may be stored at room temperature (<25°C; <77°F) for up to 28 days. Dosing is one ampule every 12 hours in 28-day cycles (i.e., 28 days on therapy, then 28 days off therapy). Inhalation solution should be administered over 15 minutes using the PARI LC Plus reusable nebulizer with a PARI Vios air compressor. Adverse reactions (>5%) include decreased forced expiratory volume, rales, red blood cell sedimentation rate increased, and dysphonia. Given that aminoglycosides can cause nephrotoxicity, ototoxicity, and worsening of neuromuscular disorders, patients should be continuously monitored for these potential complications.15
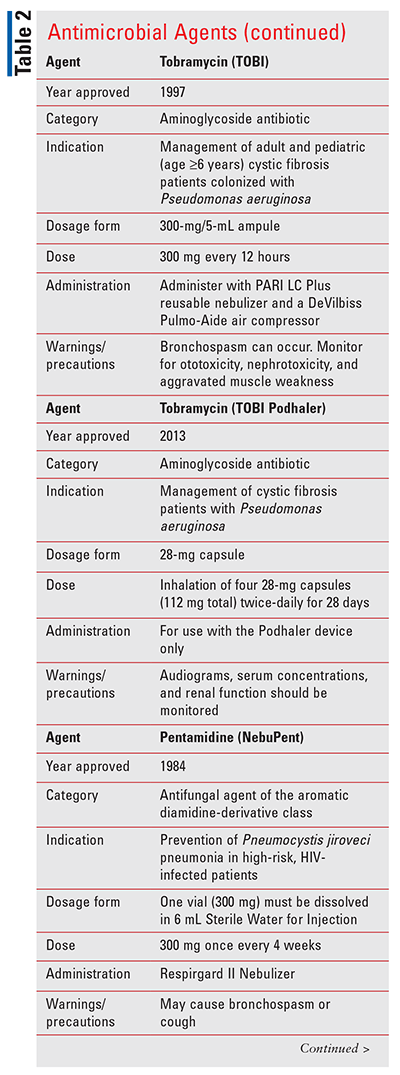
Tobramycin inhalation solution (TOBI; TABLE 2) is an aminoglycoside antibiotic used to treat P aeruginosa infections in patients with cystic fibrosis.16 This formulation is a solution with single-use 5 mL ampules containing 300 mg of tobramycin. Dosing is one ampule every 12 hours in 28-day cycles (i.e., 28 days on therapy, then 28 days off). TOBI is administered by oral inhalation over 15 minutes using a hand-held PARI LC Plus reusable nebulizer with a DeVilbiss Pulmo-Aide air compressor. TOBI should not be diluted or mixed with other medications in the nebulizer. TOBI should be refrigerated (2°-8°C, 36°-46°F) during storage. TOBI pouches (opened or unopened) may be stored at room temperature (<25°C; <77°F) for up to 28 days. The most common adverse reactions (>5%) are increased cough, pharyngitis, increased sputum, dyspnea, hemoptysis, decreased lung function, voice alteration, dysgeusia, and rash. Given that aminoglycosides can cause nephrotoxicity, ototoxicity, and worsening of neuromuscular disorders, patients should be continuously monitored for these potential complications.16
Tobramycin inhalation powder (TOBI Podhaler; (TABLE 2) is an aminoglycoside antibacterial indicated for the management of cystic fibrosis patients with P aeruginosa.17 Capsules should not be swallowed and are only used with a Podhaler device. The dose is four 28-mg capsules (112 mg total) every 12 hours in 28-day cycles (i.e., 28 days on therapy, then 28 days off). Drug capsules should be stored in the blister packs at 25°C (77°F); temperature variations from 15°-30°C (59°-86°F) are acceptable. A new Podhaler device is provided with each 7-day package of medication. Because tobramycin is an aminoglycoside, patients should be monitored for nephrotoxicity, ototoxicity, and aggravation of neuromuscular disorders. Most common adverse reactions (³10%) include cough, lung disorder, productive cough, dyspnea, pyrexia, oropharyngeal pain, dysphonia, hemoptysis, and headache.17
Pentamidine isethionate inhalant (NebuPent; TABLE 2) is an inhaled antifungal agent whose use is indicated in HIV-infected patients considered high-risk for Pneumocystis jiroveci pneumonia (PJP).18 High-risk is defined as any previous PJP infection or a serum CD4+ lymphocyte count £200/mm3. NebuPent comes in vials containing 300 mg of lyophilized antifungal product that must be stored at 20°-25°C (68°-77°F). It must be dissolved in 6 mL of sterile water prior to being administered with the Respirgard II Nebulizer. Following reconstitution, the NebuPent solution is stable for up to 48 hours if protected from light. The most common adverse reactions include cough, bronchospasm, night sweats, headache, diarrhea, nausea, respiratory tract infections, anemia, and bad taste. Other serious reactions (reported in <1% of patients) include hypotension, hypoglycemia, hyperglycemia, hyperkalemia, arrhythmia, ST segment changes on ECG, hepatic and renal dysfunction, and pancreatitis.18
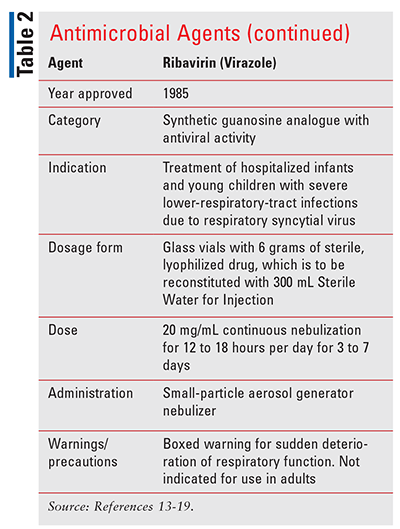
Ribavirin for inhalation solution (Virazole; TABLE 2) is used to treat respiratory syncytial virus respiratory-tract infections requiring hospital admission in infants and young children.19 Each vial of Virazole contains 6 grams of lyophilized material that should be reconstituted with 300 mL of sterile water. Lyophilized powder should be stored at room temperature (20°-25°C, 68°-77°F) with excursions acceptable from 15°-30°C (59°-86°F). After mixing the powder with sterile water, the solution should be used within 24 hours and remain at 20°-30°C, (68°-86°F). Administration requires a small-particle aerosol generator nebulizer. Recommended dosing is a continuous nebulization of 20 mg/mL for 12 to 18 hours per day for 3 to 7 days. Adverse reactions include worsening respiratory status, bronchospasm, pulmonary edema, cardiac arrest, hypotension, arrhythmias, rash, conjunctivitis, and post-treatment anemia.19
Pulmonary Arterial Hypertension Agents
Iloprost inhalation solution (Ventavis; TABLE 3) is a prostacyclin mimetic indicated for pulmonary arterial hypertension.20 Ventavis is available in 1-mL ampules in two concentrations, 10 mcg/mL and 20 mcg/mL. For each inhalation session, the entire contents of one opened ampule of Ventavis should be transferred into the I-neb AAD System’s medication chamber immediately before use. Patients should receive six to nine doses (nebulizations) per day during waking hours with a minimum of 2 hours between doses. The ampules should be stored at 20°-25°C (68°-77°F). The most common adverse reactions (≥3% placebo adjusted) are vasodilation/flushing, cough, headache, trismus, insomnia, nausea, hypotension, vomiting, increased alkaline phosphatase, flu syndrome, back pain, tongue pain, palpitations, syncope, increased gamma-glutamyltransferase, muscle cramps, hemoptysis, and pneumonia.20
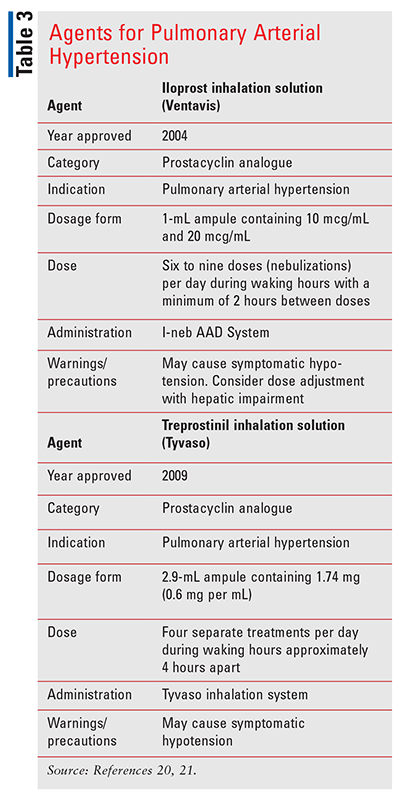
Treprostinil inhalation solution (Tyvaso; TABLE 3) is a prostacyclin mimetic indicated for treatment of pulmonary arterial hypertension.21 Each 2.9-mL ampule of Tyvaso contains 1.74 mg of treprostinil (0.6 mg per mL) that must be delivered undiluted via the Tyvaso Inhalation System—an ultrasonic, pulsed delivery device. One ampule of Tyvaso contains a sufficient volume of medication for all four treatment sessions in a single day. A single breath of Tyvaso delivers approximately 6 mcg of treprostinil. Ampules of Tyvaso are stable until the date indicated when stored in the unopened foil pouch at 20°-25°C (68°-77°F) with excursions permitted to 15°-30°C (59°-86°F). Once the foil pack is opened, ampules should be used within 7 days. Because Tyvaso is light-sensitive, unopened ampules should be stored in the foil pouch. The most common adverse reactions (≥4%) are cough, headache, nausea, dizziness, flushing, throat irritation, pharyngolaryngeal pain, diarrhea, and syncope.21
Other Agents Labeled for Inhalation
Dornase alfa inhalation solution (Pulmozyme; TABLE 4) is a recombinant DNase enzyme indicated in conjunction with standard cystic fibrosis therapies to improve pulmonary function.22 Dosage forms come in 2.5 mg/2.5 mL single-use ampules inhaled via jet nebulizer/compressor or eRapid Nebulizer System once or twice daily. Pulmozyme must be refrigerated (2°-8°C, 36°-46°F) and cannot be exposed to room temperature for more than 24 hours. Ampules come in pouches with protective foil and must not be exposed to light. The most common adverse reactions (>3% over placebo) include voice alterations, pharyngitis, rash, laryngitis, chest pain, conjunctivitis, rhinitis, decrease in forced vital capacity ≥10%, fever, and dyspnea.22
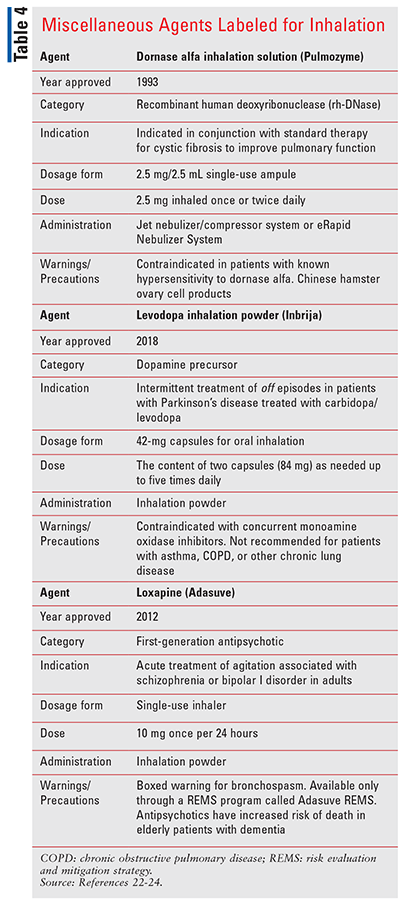
Levodopa inhalation powder (Inbrija; TABLE 4) is indicated for intermittent treatment of off episodes in patients with Parkinson’s disease being treated with carbidopa/levodopa.23 Inbrija is an inhalation powder with individual capsules containing 42 mg of levodopa to be used with the Inbrija inhaler. Dosing is 84 mg (two capsules) as needed for off symptoms, not to exceed five doses (420 mg) daily. The medication comes in blister packs that should be stored at 20°-25°C (68°-77°F); temporary temperature variations from 15°-30°C (59°-86°F) are permitted. The most common adverse reactions (≥5%) were cough, nausea, upper respiratory tract infection, and discolored sputum. Other important side effects included falling asleep during activities of daily living, withdrawal hyperpyrexia and confusion, hallucinations, psychosis, dyskinesia, and broncho-spasm with underlying lung disease.23
Loxapine inhalation powder (Adasuve; TABLE 4) is a first-generation antipsychotic indicated for the treatment of acute agitation related to schizophrenia or bipolar I disorder in adults.24 Adasuve must be administered by a healthcare professional. The dose is 10 mg by oral inhalation, and only a single dose can be given within any 24-hour period. Adasuve can cause bronchospasm with the potential for respiratory distress/arrest. Accordingly, all patients should be screened for pulmonary disease (by history and physical exam) prior to initiating therapy. After each administration, patients should be monitored every 15 minutes for at least 1 hour for evidence of bronchospasm. Most common adverse reactions (incidence≥2% and greater than placebo) are dysgeusia, sedation, and throat irritation.24
AGENTS USED OFF-LABEL FOR INHALATION THERAPY
Acute Respiratory Distress Syndrome
Epoprostefol products (Flolan, Veletri) are injectable prostanoid vasodilators indicated for treatment of pulmonary arterial hypertension.25,26 This treatment is off-label as inhaled therapy for acute lung injury and acute respiratory distress syndrome (ARDS).27 Inhaled nitric oxide gas is also used off-label for the management of ARDS.28 These agents improve ventilation-perfusion matching and anecdotally demonstrate improved oxygenation measurements. While inhaled nitric oxide is a respiratory therapy, it will often be documented on the medication administration record of the medical chart.
Antibiotics
Other antibiotics have been used off-label as inhaled treatments for pulmonary infections in populations where there is concern for antimicrobial resistance. Examples include colistin (cystic fibrosis, ventilator associated pneumonia, post-lung transplant), gentamicin (noncystic fibrosis bronchiectasis), amphotericin B (post–lung transplant), and ceftazidime (ventilator–associated pneumonia).12,29 Several fluoroquinolone inhalation products are currently under development.30
Miscellaneous Off-Label Treatments
Inhaled tranexamic acid (TXA) is used off-label to treat patients with pulmonary hemorrhage in pediatric and adult patients. Systemic TXA is FDA-approved as antifibrinolytic therapy in patients with hemophilia to reduce the risk of hemorrhage intra- and postoperatively following tooth extractions. The most common reported inhalation dosing is 500 mg three times daily using TXA solution delivered via nebulizer. The TXA-containing solution often consists of 500-mg TXA mixed with 50 mL of sodium chloride for a dose of 10 mg/mL. TXA is recommended to be stored between 20°-25°C (68°-77°F) with excursions from 15°-30°C (59°-86°F). No significant adverse effects have been reported.31-33
Heparin nebulization therapy has been used off-label in patients with acute lung injury of varying etiologies (e.g., smoke inhalation) to reduce extravascular fibrin deposition during pulmonary hemorrhage. Based on an informal literature review, dosing is typically between 30,000 and 400,000 U/day delivered by mesh or jet nebulizers. In general, heparin is recommended to be stored at 20°-25°C (68°-77°F) while avoiding excessive heat and freezing. No significant adverse reactions are noted in the literature, including no increased risk of bleeding.34-36
Milrinone is a phosphodiesterase type III inhibitor with potent pulmonary vasodilator properties that has been used with success off-label as an inhaled therapy for pulmonary hypertension during cardiac surgery.37 Acetyl-cysteine has a long history of aerosolized administration as a mucolytic. However, there are no randomized trials supporting the use of acetylcysteine in this role, and this treatment can paradoxically provoke bronchospasm and tracheal mucositis.38
Inhaled chemotherapy is being explored as a strategy in lung cancer to increase efficacy while minimizing systemic toxicity.39
ROLE OF THE PHARMACIST
Pharmacists should be familiar with these inhaled medications’ dosing, preparation, and potential adverse effects to ensure their safe and appropriate use. A basic understanding of labeled indications, medication storage, safety precautions, and required delivery devices is essential for administration of inhalation therapies. The pharmacist has responsibility for drug-use control in all patient-care settings—including respiratory therapy medications—and, as such, should work closely with physicians, respiratory therapists, nurses, and other healthcare professionals who provide inhalation therapy to patients.40
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
REFERENCES
1. Patton JS, Fishburn CS, Weers JG. The lungs as a portal of entry for systemic drug delivery. Proc Am Thorac Soc. 2004;1:338-344.
2. Newman SP. Drug delivery to the lungs: challenges and opportunities. Ther Deliv. 2017;8(8):647-661.
3. Labiris NR, Dolovich MB. Pulmonary drug delivery. Part I: Physiological factors affecting therapeutic effectiveness of aerosolized medications. Br J Clin Pharmacol. 2003;56:588-599.
4. National Heart, Lung, and Blood Institute. 2020 Focused updates to the asthma management guidelines: A report from the National Asthma Education and Prevention Program Coordinating Committee Expert Panel Working Group. J Allergy Clin Immunol. 2020;146:1217-1270.
5. Global Initiative for Asthma. Global strategy for asthma management and prevention, 2020. www.ginasthma.org. Accessed June 30, 2021.
6. Halpin DMG, Criner GR, Popi A, et al. Global Initiative for the Diagnosis, Management, and Prevention of Chronic Obstructive Lung Disease. The 2020 GOLD Science Committee Report on COVID-19 and chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2021;203(1):24-36.
7. Insulin human (rDNA origin) inhalation powder (Exubera®) package insert. New York, NY: Pfizer Labs; January 2006.
8. Heinemann L. The failure of Exubera: are we beating a dead horse? J Diabetes Sci Technol. 2008;2(3):518-529.
9. Oleck J, Kassam S, Goldman JD. Commentary: why was inhaled insulin a failure in the market? Diabetes Spectr. 2016;29(3):180-184.
10. Odegard PS, Capoccia KL. Inhaled insulin: Exubera. Ann Pharmcother. 2005;39:843-853.
11. Afrezza (insulin human inhalation powder) package insert. Danbury, CT: Mannkind Corporation; October 2018.
12. Maselli DJ, Keyt H, Restrepo MI. Inhaled antibiotic therapy in chronic respiratory disease. Int J Mol Sci. 2017;18(5):1062.
13. Arikayce (amikacin liposomal inhalation suspension) package insert. Bridgewater, NJ: Insmed; October 2020.
14. Cayston (aztreonam inhalation solution) package insert. Foster City, CA: Gilead Sciences Inc; November 2019.
15. Bethkis (tobramycin inhalation solution) package insert. Woodstock, IL: Catalent Pharma Solutions, LLC; December 2019.
16. TOBI (tobramycin inhalation solution) package insert. East Hanover, NJ: Novartis; October 2018.
17. TOBI Podhaler (tobramycin inhalation powder) package insert. Morgantown, WV: Mylan Specialty, L.P.; July 2020.
18. Nebupent (pentamidine isothianate) package insert. Lake Zurich, IL: Fresenius Kabi; October 2016.
19. Virazole (ribavarin) package insert. Bridgewater, NJ: Bausch Health; May 2019.
20. Ventavis (iloprost inhalation solution) package insert. South San Francisco, CA: Actelion Pharmaceuticals; December 2019.
21. Tyvaso (trepostinil inhalation solution) package insert. Research Triangle Park, NC: United Therapeutics Corp; March 2021.
22. Pulmozyme (dornase alfa package) insert. South San Francisco, CA:Genentech, Inc; January 2018.
23. Inbrija (levodopa inhalation powder) package insert. Ardsley, NY: Acorda Therapeutics Inc; August 2020.
24. Adasuve (loxapine package insert). Souderton, PA: Galen US Inc; August 2017.
25. Flolan (epoprostenol sodium) package insert. Research Triangle Park, NC: GlaxoSmithKline; November 2019.
26. Veletri (epoprostenol) package insert. South San Francisco, CA: Actelion Pharmaceuticals; December 2018.
27. Dzierba AL, Abel EA, Buckley MS, Lat I. A review of inhaled nitric oxide and aerosolized epoprostenol in acute lung injury or acute respiratory distress syndrome. Pharmacotherapy. 2014;34(3):279-290.
28. Griffiths MJD, Evans TW. Inhaled nitric oxide therapy in adults. N Engl J Med. 2005;353:2683-2695.
29. Quon, BS, Goss CH, Ramsey BW. Inhaled antibiotics for lower airway infections. Ann Am Thorac Soc. 2014;11(3):425-434.
30. Hurley M, Smyth A. Fluoroquinolones in the treatment of bronchopulmonary disease in cystic fibrosis. Ther Adv Respir Dis. 2012;6(6):363-373.
31. Cyklokapron (tranexamic acid) package insert. New York, NY: Pfizer Inc; March 2021.
32. Wand O, Guber E, Guber A, et al. Inhaled tranexamic acid for hemoptysis treatment: a randomized controlled trial. Chest. 2018;154(6):1379-1384.
33. O’Neil ER, Schmees LR, Resendiz K, et al. Inhaled tranexamic acid as a novel treatment for pulmonary hemorrhage in critically ill pediatric patients: an observational study. Crit Care Explor. 2020;2(1):e0075.
34. Heparin sodium package insert. Lake Zurich, IL: Fresenius Kabi; August 2017.
35. Glas GJ, Neto AS, Horn J, et al. Nebulized heparin for patients under mechanical ventilation: an individual patient data meta-analysis. Ann Intensive Care. 2016;6(1):33.
36. Juschten J, Tuinman PR, Juffermans NP, et al. Nebulized anticoagulants in lung injury in critically ill patients—an updated systematic review of preclinical and clinical studies. Ann Transl Med. 2017;5(22):444.
37. Haraldsson A, Kieler-Jensen N, Ricksten SE. The additive pulmonary vasodilatory effects of inhaled prostacyclin and inhaled milrinone in postcardiac surgical patients with pulmonary hypertension. Anesth Analg. 2001;93:1439-1445.
38. Rubin BK. Aerosol medications for treatment of mucus clearance disorders. Respir Care. 2015;60(6):825-832.
39. Mangal S, Gao W, Tonglei K, Zhou QT. Pulmonary delivery of nanoparticle chemotherapy for the treatment of lung cancers: challenges and opportunities. Acta Pharmacol Sin. 2017;38:782-797.
40. ASHP statement on the pharmacist’s responsibility for distribution and control of drug products. Am J Hosp Pharm. 1992;49(8):2009-2010.
To comment on this article, contact rdavidson@uspharmacist.com.






