US Pharm. 2016;41(6)(Generic Drug Review suppl):36-41.
ABSTRACT: As the cost of healthcare continues to rise, insurers and the federal government will continue to seek ways to reduce cost. Generic drug substitution commonly is used to decrease costs for medication use, and the use of generic drugs will continue to increase. Numerous studies have shown that negative patient perceptions of generic drugs are commonly based on misconceptions. Pharmacists, as the most accessible healthcare provider, have the greatest opportunity to educate patients on the use and safety of generic drugs. Better communication between pharmacists and patients about generic drugs may lead to improved perceptions, increased adherence, and avoidance of patient confusion.
As national healthcare spending continues to rise, the use of generic medications is encouraged by insurers and the federal government as a cost-saving strategy.1,2 According to the Generic Pharmaceutical Association’s 2015 report, generic pharmaceutical products saved the U.S. healthcare system $254 billion in 2014.3 Third-party payers typically incentivize generic drug use by offering a lower or $0 copayment when patients fill a prescription with a generic substitute drug.2,4 Subsequently, patients are more likely to be dispensed a generic drug. Much discussion concerning the quality of generic medications has taken place in the media, which ultimately influences patient perceptions.5 It is important for pharmacists to understand patient perceptions about generic drugs in order to provide education and information that can help patients make informed decisions. Surveys have shown that patients are more comfortable with, and more likely to accept, a generic medication when the pharmacist or physician discusses the generic with them.6
Patient Perceptions of Generic Drugs
The FDA has identified some common misconceptions about generic medications: that they are less effective, take longer to start working, are not safe, and are manufactured in substandard facilities.7 Additionally, numerous studies have aimed to determine public and professional perceptions of generic products.
A study by Iosifescu and colleagues showed that safety, efficacy, tolerability, and ease of use are frequent patient concerns about generic medications, even among patients with high monthly out-of-pocket prescription costs.8 The study compared elderly patients’ perspectives about generic and brand medications in a hospital-based primary care setting. Most patients believed generic medications to be less expensive than their brand counterparts; however, one-fourth thought that generics were less effective and one-fifth believed that generics were less safe. Twenty percent to 40% of the time, patients were uncertain whether generic medications were equivalent to brand medications. Among patients with inadequate health literacy, about one-half believed generics to be less effective and less safe. Negative beliefs about generic medications were associated with nonwhite race, low education level, low health literacy, low income, possession of Medicaid coverage, worse functional status, and worse physician-communication scores.8
Similarly, a recent meta-analysis evaluating perceptions of physicians, pharmacists, and patients found that patients with less education were more skeptical of generic medications.5 A national survey reported that American patients think that generic medications are less expensive, are a better value, and are just as safe as brand-name medications; however, only 37.6% of survey participants preferred to use generics.2 In a randomized, controlled trial conducted in Germany, 804 primary care patients were surveyed regarding their attitudes toward generic medications.9 About two-thirds of patients said that they knew the differences between brand and generic medications (responses were influenced by how many years of education the patient had received). One-third of patients were dissatisfied with the information they received from their general practitioner when a generic substitute was used, and nearly one-third were skeptical of generic medications because of their lower cost. Patients aged >60 years were more likely to have negative views of generic medications.9 In a study by Quintal and Mendes, who administered a questionnaire to >400 patients in Portugal to identify patients’ perceptions about drug substitution, significantly higher levels of acceptance of generic substitution were found in patients with higher education levels or in patients who obtained recommendations from a pharmacist or physician.10
Although perceptions of generic products may be improving, considerable skepticism and mistrust still exist,2,5 and the question remains whether this mistrust affects the use of generics. Shrank and colleagues evaluated whether beliefs or communication was associated with the use of generic medications and found that generic medication use was most significantly associated with patient communication by healthcare providers about generics.2 Patients were comfortable with generic substitution, but use was not associated with general preferences for generics, generic efficacy or safety, or generic cost.2 Despite patients’ reluctance concerning generic products, evidence has shown increased adherence with generics compared with brand medications.11 This is likely because of the affordability of generic equivalents.
Patient Education
As discussed above, there are a variety of reasons that patients often are hesitant to use generic drugs. Generally, when consumers compare generic and brand-name products such as common household items, the more inexpensive generic product is often of lesser quality. It is understandable, then, how patients may apply this concept to drugs, reasoning that the more inexpensive generic medication must be inferior. At a minimum, healthcare providers should take the initiative to discuss any monetary concerns their patients may have. This may create an opportunity to emphasize the financial benefit of generic medications while addressing common misconceptions. Several studies have shown increased patient acceptability of generic drugs when healthcare providers communicate the differences between brand and generic drugs.6,12 Pharmacists should be familiar with these misconceptions and know how to address them. Therefore, patient education should be directed at dispelling these misconceptions.
Misconception No. 1: Generic drugs are less effective and take longer to work. This misconception can be addressed by educating patients about the concept of bioequivalence. The FDA has strict regulations for bioequivalence. In order for a drug to be considered bioequivalent to its brand counterpart, it must perform the same way in the body and have the same active ingredient(s), strength, dosage form, and route of administration. It should be remembered that the generic drug is not required to have the same excipients or inactive ingredients as the brand equivalent.13 Patients tend to be more comfortable with generic drugs when they know that the generic drug contains the same active ingredient(s) and thereby has the same risk-benefit profile as the brand-name medication.
Misconception No. 2: Generic drugs are not safe. The FDA requires that generic drugs be manufactured according to the same Good Manufacturing Practices (GMP) regulations required for brand medications. Generic drugs are reviewed by the FDA just as brand drugs are, but under an abbreviated review. The review is abbreviated because the generics manufacturer is not required to repeat the research previously performed and reviewed for the brand drug.7
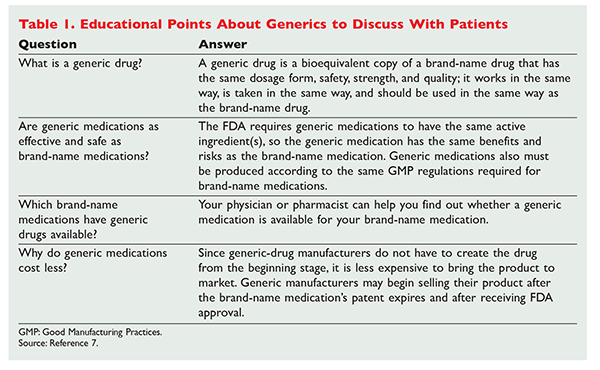
Misconception No. 3: Generic drugs are manufactured in substandard facilities. The FDA requires that generic drugs be manufactured in accordance with current GMP. Furthermore, regulatory oversight of generic-drug manufacturing is the same as for brand drugs.14 Education that addresses common patient misconceptions is important, but other educational points to discuss are given in TABLE 1. Motivational interviewing techniques may be helpful for counseling patients on generic medications. In this method, healthcare providers collaborate with patients and exchange information in order to make an informed team decision about the patient’s care. The goal of motivational interviewing is to spur motivation and obtain commitment to behavior change. The communication should be conducted in an “ask, provide, ask” manner.15 Pharmacists, as the most accessible type of healthcare provider, have the best opportunity to discuss generic-medication concerns with patients, but studies have shown that physician communication also has a significant effect on patients’ beliefs about and use of generics.2,8,15 This fact emphasizes the need for both pharmacists and physicians to have better and more frequent communication with patients about generic medications.
Generic Substitution
It is common practice for pharmacists to automatically substitute a generic drug for a prescribed medication if the prescriber allows for generic substitution (also known as drug product selection or generic drug interchange). Furthermore, generic substitution for medications considered to have a narrow therapeutic index (NTI) is controversial. In fact, some states do not allow generic substitutions for NTI drugs. It is important to provide the patient with the option for substitution as early as possible in the filling process. This may help avoid confusion when the patient arrives to pick up the prescription and finds that it was filled with a generic substitute. Moreover, addressing this subject initially may help a patient feel more comfortable about receiving a generic drug. Efforts to empower patients to actively play a role in their medication-selection process may have a positive effect on the use of generic medications.
Conclusion
Although the use of generic medications is improving, patients still lack confidence in generic drugs and view them with mistrust. Pharmacists are in a unique position to educate patients about the value, safety, and efficacy of generic drugs. Educating patients and addressing their concerns and misconceptions may improve their confidence in, and willingness to take, generic medications. Communication between healthcare providers and patients concerning generic drugs has been shown to improve patients’ overall perception of these products.
REFERENCES
1. World Health Organization. WHO drug information volume 29, no 4, 2015. www.who.int/medicines/publications/druginformation/issues/DrugInformation2015_Vol29-4/en. Accessed February 11, 2016.
2. Shrank WH, Cox ER, Fischer MA, et al. Patients’ perceptions of generic medications. Health Aff (Millwood). 2009;28:546-556.
3. Generic Pharmaceutical Association. Generic drug savings in the U.S.: seventh annual edition: 2015. www.gphaonline.org/media/wysiwyg/PDF/GPhA_Savings_Report_2015.pdf. Accessed April 27, 2016.
4. Godman B, Malmström RE, Diogene E, et al. Are new models needed to optimize the utilization of new medicines to sustain healthcare systems? Expert Rev Clin Pharmacol. 2015;8:77-94.
5. Dunne SS, Dunne CP. What do people really think of generic medicines? A systematic review and critical appraisal of literature on stakeholder perceptions of generic drugs. BMC Med. 2015;13:173.
6. Shrank WH, Cadarette SM, Cox E, et al. Is there a relationship between patient beliefs or communication about generic drugs and medication utilization? Med Care. 2009;47:319-325.
7. FDA.gov. What you want to know about generic drugs. www.fda.gov/downloads/Drugs/ResourcesForYou/Consumers/BuyingUsingMedicineSafely/UnderstaningGenericDrugs/UCM169283.pdf. Accessed February 7, 2016.
8. Iosifescu A, Halm EA, McGinn T, et al. Beliefs about generic drugs among elderly adults in hospital-based primary care practices. Patient Educ Couns. 2008;73:377-383.
9. Himmel W, Simmenroth-Nayda A, Niebling W, et al. What do primary care patients think about generic drugs? Int J Clin Pharmacol Ther. 2005;43:472-479.
10. Quintal C, Mendes P. Underuse of generic medicines in Portugal: an empirical study on the perceptions and attitudes of patients and pharmacists. Health Policy. 2012;104:61-68.
11. Gagne JJ, Choudhry NK, Kesselheim AS, et al. Comparative effectiveness of generic and brand-name statins on patient outcomes: a cohort study. Ann Intern Med. 2014;161:400-407.
12. Vallès JA, Barreiro M, Cereza G, et al. A prospective multicenter study of the effect of patient education on acceptability of generic prescribing in general practice. Health Policy. 2003;65:269-275.
13. FDA. Guidance for industry: bioavailability and bioequivalence studies submitted in NDAs or INDs—general considerations. www.fda.gov/downloads/drugs/guideancecomplianceregulatoryinformation/guidances/ucm389370.pdf. Accessed April 27, 2016.
14. FDA.gov. Generic drugs: questions and answers. www.fda.gov/Drugs/ResourcesForYou/Consumers/QuestionsAnswers/ucm100100.htm. Accessed February 7, 2016.
15. Possidente CJ, Bucci KK, McClain WJ. Motivational interviewing: a tool to improve medication adherence? Am J Health Syst Pharm. 2005;62:1311-1314.
To comment on this article, contact rdavidson@uspharmacist.com.






