US Pharm. 2-16;41(7):25.
In 2013, acute respiratory infections (including influenza and pneumonia) claimed nearly 57,000 lives (15.9 deaths per 100,000 population). One-third of vaccinations were given in nontraditional settings (i.e., pharmacies), whereas approximately two-thirds were administered by other sources (i.e., physicians, nurses, and clinics). Although vaccinations reduce morbidity and mortality, vaccination uptake among certain populations remains low, and national health objectives have not been met.
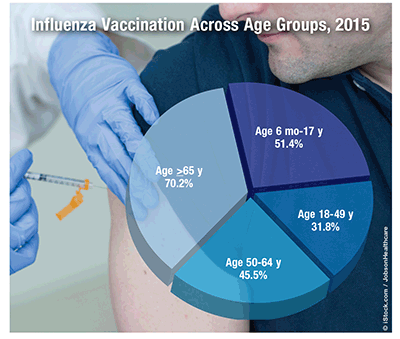
Influenza Vaccination: Influenza caused nearly 3,700 deaths (1.2 deaths per 100,000 population) in 2015, even though vaccination rates in children and adults increased by 5.1% and 2.7%, respectively, in 2012-2013 over 2011-2012. Influenza vaccine remained the most common immunization (88%) in 2013, with 77% of pharmacies offering vaccination on a walk-in basis. As people aged, so did the proportion of those who received the influenza vaccine. Vaccination was most common among non-Hispanic white persons (46%), followed by Asian (45%) and non-Hispanic black and African American persons (34.4%); Hispanic persons had the lowest rate (31%). One-fifth more females than males (46.1% vs. 37.9%) were vaccinated. The Northeast (45%) had the highest incidence of influenza vaccination; the West had the lowest incidence (39.7%), and the Midwest and the South were similar at 43.6% and 41.5%, respectively.
Pneumonia: Pneumococci cause up to 36% of cases of adult community-acquired pneumonia, which occurs at a rate of 915,900 episodes annually in adults aged 65 years and older. About 25% to 30% of patients with pneumococcal pneumonia also experience pneumococcal bacteremia, at an incidence of 12,000 cases per year. Pneumococcal pneumonia causes 400,000 hospitalizations annually. The number of inpatient deaths from pneumonia was 37,000 (3.3 deaths per 100 discharges), and 40% more deaths (4.6 deaths per 100 discharges) occurred in persons aged 65 years and older. Pneumonia mortality in children dropped 97% in the last century, but respiratory infections remained a leading cause of pediatric hospitalizations and outpatient visits, according to the CDC.
Pneumococcal Vaccination: The vaccination rate increased with age progression (18-44 years, 8.3%; 45-64 years, 18.4%; 65-74 years, 55.8%; 75 years and older, 69.3%). The vaccination rate was appreciably higher (18-44 years, 11.3%; 45-64 years, 28.3%) for high-risk persons with comorbid conditions such as diabetes, emphysema, coronary heart disease, angina, and heart attack. Among persons aged 65 years and older, women outnumbered men (63.7% vs. 58.4%); across racial and ethnic groups, the highest vaccination rate was in non-Hispanic white persons (64.7%), followed by non-Hispanic black (49.8%), Asian (47.7%), and Hispanic persons (49.8%). Disparities in the rate of vaccination were observed geographically: The Midwest had the highest frequency (65.4%), followed by the South (60.9%), Northeast (59.6%), and West (59.3%).
To comment on this article, contact rdavidson@uspharmacist.com.





