US Pharm. 2013;38(11):35-38.
ABSTRACT: Pediatric
autoimmune neuropsychiatric disorders associated with streptococcal
infections (PANDAS) manifest as a phenomenon prominently associated with
obsessive-compulsive disorder (OCD), tic disorder, or both, in
children. The phenomenon is associated with a distinctive temporal
association with group A streptococcal infection and evidence of
neurologic abnormalities. Recognition of PANDAS in the pediatric
population is important so that appropriate treatment options are
provided. Therapy is primarily focused on antibiotic treatment of the
streptococcal infection; however, in certain populations, antibiotic
prophylaxis may be effective in preventing poststreptococcal
neuropsychiatric exacerbations.
Pediatric autoimmune neuropsychiatric disorders associated with streptococcal infections (PANDAS) were first described in a subset of patients by Swedo et al.1 It was proposed that childhood obsessive-compulsive disorder (OCD) and/or tics may arise as a result of a poststreptococcal autoimmune process.
A temporal relationship between symptom exacerbation and group A streptococcal (GAS) infection is crucial to PANDAS diagnosis.1 Determination that a child fits the PANDAS profile is made through prospective evaluation and documentation of the presence of streptococcal infections in con-junction with at least two episodes of neuropsychiatric symptoms, as well as demonstrating a negative throat culture or stable titers during a time of neuropsychiatric symptom remission.2 Symptoms are generally described as sudden and severe, and remain at peak severity for several weeks or longer and then gradually subside. Symptoms may remit completely, with patients remaining asymptomatic until they are again infected with GAS.1,2
Epidemiology
PANDAS syndrome is generally known as a
childhood disorder. Some studies indicate the possibility of adult
cases, but incidence of these cases and even studies exploring delayed
onset of OCD due to PANDAS infection are areas that must be further
explored.3 History of mild OCD is sometimes a
characteristic of a patient’s past medical history, but that is not
always the case. The neurologic symptoms eventually dissipate, but
children may display OCD characteristics for the remainder of their
lives. The experience of one young patient is described in the CASE STUDY.4

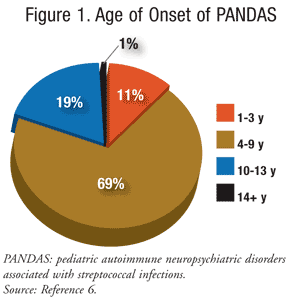
It is estimated that 148,000 children are
diagnosed with Tourette syndrome in the United States and 500,000 are
diagnosed with OCD.5 Children in the PANDAS subgroup make up to 25% of children diagnosed with tic and OCD disorders.5 For PANDAS, the mean age at presentation is 7 years (FIGURE 1).6
It has been proposed that effective treatments and education of both
patients and healthcare providers significantly increase the
identification of OCD overall.
Pathology
The process by which PANDAS occurs in the body is proposed to be an antibody response directed toward group A beta-hemolytic streptococci (GABHS) that have a cross-reaction with the host.7 In theory, the cross-reaction of the immune system targets the basal ganglia within the caudate nucleus and putamen of the brain. However, it should be noted that basal ganglia in other areas of the brain can also be affected. Genetic predisposition may also be a factor in this process, and certain individuals may be more susceptible to developing this syndrome. The attack of the immune system triggers an inflammatory reaction that enlarges the basal ganglia. This in turn is proposed to bring about the tics and OCD that develop postinfection.8
Clinical Presentation and Differential Diagnosis
Based on clinical descriptions of 50
cases, a research program of the National Institute of Mental Health
(NIMH) developed a diagnostic model for PANDAS.1 Diagnosis depends upon five criteria (TABLE 1), all of which must be satisfied.1,7,9

When symptoms of PANDAS first occur, laboratory tests should be performed to facilitate clinical management. A throat swab can determine the presence of antistreptococcal antibodies, although a negative culture does not rule out PANDAS.9,10 In addition to a throat swab, a blood test for antistreptolysin O (ASO) may be performed.9 An elevated titer is not sufficient to prove that OCD symptoms resulted from the infection, but may support the clinical therapy.7 Laboratory tests, including the ones mentioned above, have not yet been proven to be reliable markers for diagnosis.10
According to the Diagnostic and Statistical Manual of Mental Disorders (DSM-IV-TR or DSM-5 ), clinical presentation of OCD is described by manifestations of obsessions and compulsions.11,12 Obsessions include recurrent thoughts/impulses/images that lead to anxiety, are beyond excessive worry, cannot be suppressed, and are not perceived as being a product of the individual’s own mind. Compulsions include repetitive behaviors or mental acts, with the belief that these behaviors or mental acts will prevent a given event or situation. These manifestations are disruptive to normal routine, occupational functioning, or social relationships.11,12
Treatment
Because PANDAS-associated OCD is due to
an infection, treatment of the infection is key to treating the disease.
Unfortunately, there is no established treatment plan specifically for
PANDAS-associated OCD, although antibiotics are indicated for all GAS
infections, and therefore they are used in the treatment of PANDAS.13
However, there is a trend to initiate antibiotic therapy as a
prophylactic measure to prevent further deterioration and subsequent
episodes of the disorder. A higher risk of infection exisits in children
who have had PANDAS, rheumatic fever, and Sydenham chorea. Prophylaxis
in these children may potentially decrease the chances of reinfection.
Examples of antibiotics that can be used for treatment and/or
prophylaxis include penicillin, amoxicillin-clavulanate, clindamycin,
cephalexin, and azithromycin (TABLE 2).14-16
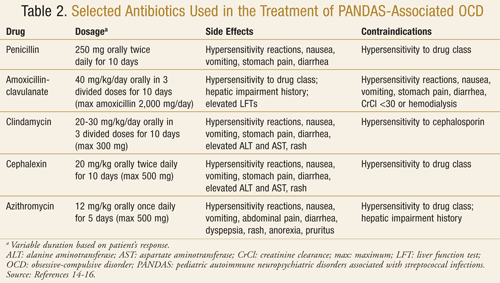
Duration of antibiotic prophylaxis has been reviewed and recommended in guidelines by the American Academy of Pediatrics (AAP) and World Health Organization.14 The AAP reported a length of prophylaxis for 5 years after the last attack or until age 21 years, whichever is longer.14 Drawbacks to long-term prophylactic antibiotic use include the potential for the evolution of drug-resistant strains, an increased risk for allergic reactions, and shifts in the normal flora that may make patients more susceptible to infections such as thrush and Clostridium difficile.9 Clinicians should weigh the risks and benefits to determine the most appropriate action for the patient.
Because PANDAS-associated OCD is related to infection, the symptoms will not usually subside until the infections are fully treated. Clinicians should consider obtaining follow-up throat cultures as well as checking the family members of the patient.9 However, more studies need to be done to verify the necessity of this procedure.
Cognitive behavioral therapy (CBT), including exposure and response prevention (ERP), has been shown to help PANDAS patients as well as their families.9,17 While this effect is based on a small study of only 7 patients,17 it is reasonable to assume CBT can aid patients, as it is often successfully used to benefit others with psychiatric disorders. Parents can seek accommodations at school like those appropriate for children with OCD.9
Selective serotonin reuptake inhibitors (SSRIs) are considered first-line treatment for children with OCD.18
The FDA-approved SSRIs for the treatment of OCD in children are
fluoxetine, fluvoxamine, and sertraline; a tricyclic antidepressant,
clomipramine, is also FDA-approved (TABLE 3).19

In the Pediatric OCD Treatment Study (POTS), a randomized, controlled trial, the authors found that both SSRIs and CBT were more helpful than placebo, but that the greatest benefit was found when SSRIs were combined with CBT.20 While clinicians may consider the results of this study when they treat children with PANDAS-associated OCD, this study was focused on children who had OCD from any cause. Patients with PANDAS-associated OCD may be more sensitive to behavioral side effects of SSRIs such as aggression, hyperactivity, sleep problems, and suicidal thinking.9 More data are needed to confirm if the use of SSRIs is beneficial in this specific patient population.
Another practical consideration is symptomatic control of patients’ tics/OCD symptoms through the use of classical or atypical antipsychotics.10 Overall, it may be more beneficial to focus on antibiotic treatment to prevent symptoms rather than on antipsychotics to achieve symptomatic control.19
One study on OCD disorders caused by GABHS explored the possibility of immunomodulatory therapy.21 In this study, treatments such as plasma exchange and intravenous immunoglobulin (IVIG) were compared to placebo. The results of IVIG were very promising, as “striking improvements” in OCD symptoms were shown at 1 month and were maintained for 1 year. Both plasma exchange and IVIG were more effective in lessening symptom severity than placebo, but the authors of the study acknowledge that further studies are needed to determine the active mechanism of these treatments, as well as to determine which children with OCD would benefit from them.21
Conclusion
Recognition of the differential diagnosis between childhood onset of OCD/tics and PANDAS-associated OCD is crucial in determining proper treatment of the condition. The PANDAS subgroup has a distinct clinical presentation and an identifiable course of symptoms that coincide with a clear relationship between streptococcal infections and neuropsychiatric symptom exacerbations.5 Selecting the proper therapy to eradicate streptococcal infection at the sentinel episode of PANDAS may be of benefit.6 Pharmacists can make a significant impact on the recognition and diagnosis of this subgroup of patients. Selection of proper treatment options and optimization of therapy can help to improve quality of life and aid in symptom remittance.
REFERENCES
1. Swedo SE, Leonard HL, Garvey M, et al.
Auto-immune neuropsychiatric disorders associated with streptococcal
infections: clinical description of the first 50 cases. Am J Psychiatry. 1998;155:264-271.
2. Snider LA, Swedo SE. PANDAS: current status and directions for research. Mole Psychiatry. 2004;9:900-907.
3. Bodner SM, Morshed SA, Peterson BS. The question of PANDAS in adults. Biol Psychiatry. 2001;49:807-810.
4. James SD. PANDAS: strep throat can lead to OCD in children. ABC News.
October 5, 2011.
http://abcnews.go.com/Health/pandas-strep-throat-trigger-obsessive-compulsive-disorder-children/story?id=14668292.
Accessed April 26, 2013.
5. Swedo SE, Leonard HL, Rapoport JL. The
pediatric autoimmune neuropsychiatric disorders associated with
streptococcal infection (PANDAS) subgroup: separating fact from fiction.
Pediatrics. 2004;113:907-911.
6. Murphy ML, Pichichero ME. Prospective
identi-fication and treatment of children with pediatric autoimmune
neuropsychiatric disorder associated with group A streptococcal
infection (PANDAS). Arch Ped Adoles Med. 2002;156:356-361.
7. Swedo SE, Leckman JF, Rose NR. From
research subgroup to clinical syndrome: modifying the PANDAS criteria to
describe PANS (pediatric acute-onset neuropsychiatric syndrome). Pediatr Therapeut. 2012;2:113.
8. Moretti G, Pasquini M, Mandarelli G, et al. What every psychiatrist should know about PANDAS: a review. Clin Pract Epidemol Ment Health. 2008;4:13.
9. Stewart E, Murphy T. PANDAS Fact Sheet. Boston, MA: International OCD Foundation; 2010.
www.ocfoundation.org/uploadedfiles/maincontent/find_help/pandas%20fact%20sheet.pdf. Accessed April 26, 2013.
10. Kurlan R, Kaplan EL. The pediatric
autoimmune neuropsychiatric disorders associated with streptococcal
infection (PANDAS) etiology for tics and obsessive-compulsive symptoms:
hypothesis or entity? Practical considerations for the clinician. Pediatrics. 2004;113:883-886.
11. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision (DSM-IV-TR). Washington, DC: American Psychiatric Publishing; 2000.
12. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5). Washington, DC: American Psychiatric Publishing; 2013.
13. Tan J, Smith CH, Goldman RD. Pediatric autoimmune neuropsychiatric disorders associated with streptococcal infection. Can Fam Physician. 2012;58:957-959.
14. Pohlman D. Antibiotics. PANDAS Network. June 7, 2010. http://pandasnetwork.org/treatment-2/antibiotics. Accessed May 1, 2013.
15. Schulman ST, Bisno AL, Clegg HW, et
al. Clinical practice guideline for the diagnosis and management of
group A streptococcal pharyngitis: 2012 update by the Infectious
Diseases Society of America. Clin Infect Dis. 2012;55:1279-1282.
16. Lexi-Comp Online [online database]. Hudson, OH: Lexi-Comp, Inc; 2013. www.lexi.com. Accessed October 7, 2013.
17. Storch EA, Murphy TK, Geffken GR, et
al. Cognitive-behavioral therapy for PANDAS-related obsessive-compulsive
disorder: findings from a preliminary waitlist controlled open trial. J Am Acad Child Adolesc Psychiatry. 2006;45:1171-1178.
18. Stewart SE. Medicines for OCD in
children and teens. International OCD Foundation.
www.ocfoundation.org/meds_kids.aspx. Accessed May 1, 2013.
19. Micromedex Healthcare Series
[Internet database]. Greenwood Village, CO: Thomson Healthcare. Updated
periodically. www.micromedex.com. Accessed May 1, 2013.
20. Cognitive-behavior therapy,
sertraline, and their combination for children and adolescents with
obsessive-compulsive disorder: the Pediatric OCD Treatment Study (POTS)
randomized controlled trial. JAMA. 2004;292:1969-1976.
21. Perlmutter SJ, Leitman SF, Garvey MA,
et al. Therapeutic plasma exchange and intravenous immuno-globulin for
obsessive-compulsive disorder and tic disorders in childhood. Lancet. 1999;354:1153-1158.
To comment on this article, contact rdavidson@uspharmacist.com.





