Infectious disease has plagued humankind throughout history. However, the ability to prevent disease with vaccines did not exist until Edward Jenner inoculated a youngster with cowpox in 1796.1 Ongoing vaccine development and vaccination recommendations have enabled people to live healthier lives.2 Currently, the Advisory Committee on Immunization Practices (ACIP), which reviews and updates vaccination standards, recommends immunization for U.S. adults and children against 17 infectious diseases (TABLE 1).3,4
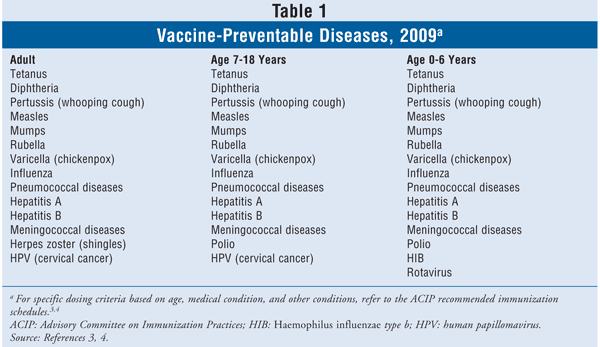
Overall, the number of cases of vaccine-preventable diseases (VPDs) is at an all-time low, with impressive decreases in morbidity and mortality. Comparison between the incidence of VPDs before national vaccination recommendations were issued and the rate in 2006 show that the number of cases of diphtheria, measles, paralytic poliomyelitis, rubella, congenital rubella syndrome, and smallpox dropped by more than 99%.5 Nevertheless, vaccination rates remain suboptimal for adults and children, with particularly low levels in some impoverished and minority communities.1
Pharmacists have the opportunity to promote public health through immunization.6 The purpose of this paper is to educate pharmacists about the ongoing need to promote public health through aggressive immunization practices and to provide information about practical methods for accomplishing this task.
IMMUNITY
Immunity may be actively or passively acquired. Active immunity occurs when the body generates its own protection, either naturally (after surviving an infection) or following vaccination. Vaccines contain disease-specific antigenic material that provokes the body to produce antibodies. If a person is later exposed to that disease, the antibodies assist the immune system in recognizing and destroying the infectious organism and in preventing illness.1,7 Passive immunity develops when a person receives already-formed antibodies. This may be a natural process, as in maternal-fetal transfer, or it may occur when a person receives exogenous antibodies (such as rabies or tetanus) via injection. Active immunity is long-term, whereas passive immunity is short-term.1,7
VPDs IN THE NEWS
VPDs are frequent headliners in the lay press. The Associated Press reported in January 2008 that the 2007 National Immunization Survey-Adult revealed disappointingly low vaccination rates for the three newest adult vaccines.8 Of eligible recipients, only 2% had been vaccinated for shingles, 2% had received a pertussis booster, and 10% had obtained at least the first of a three-dose series to protect against cervical cancer caused by human papillomavirus (HPV).9 In a press conference discussing these data, Anne Schuchat, MD, director of the CDC's National Center for Immunization and Respiratory Diseases, lamented, "We are at the infancy of developing the strong adult immunization program that we'd like to have. We really need to get beyond the mentality that vaccines are for kids."10 While this mindset may partially account for low adult vaccination rates, other factors contribute to the problem. Among the reasons surveyed adults offered for not getting vaccinations were concerns about vaccine safety or efficacy, being too busy to get shots, lack of awareness about which diseases are vaccine-preventable, not being worried about contracting a VPD, and expense.10 The shingles vaccine may cost about $150, and the price tag for the three-dose HPV series is approximately $300.8
On April 2, 2008, the CDC issued an official Health Advisory warning of multiple measles outbreaks in the United States secondary to importation from endemic countries.11 The CDC made clear that not only immigrants and foreign tourists bring measles into the country; U.S. citizens who lack immunity to measles may carry the infection home with them after traveling abroad. Newspapers across the country disseminated the story and urged vaccination of unimmunized individuals.12
In May 2008, the New York Times highlighted a study in which Johns Hopkins researchers uncovered a strong link between certain oral cancers in males and HPV type 16 (HPV-16), which can enter the mouth during oral sex.13,14 The lead researcher commented that the high risk of HPV-associated cancers in males should prompt serious thought about vaccinating all adolescents against HPV. The quadrivalent HPV vaccine, marketed as Gardasil, protects against HPV-6, HPV-11, HPV-16, and HPV-18. HPV-6 and HPV-11, which are considered low-risk HPV types, are associated with genital warts in both males and females, but do not cause cancer. HPV-16 and HPV-18, which are high-risk oncogenic HPV types, are associated with approximately 70% of cervical cancers, as well as with vulvar, vaginal, anal, penile, and oropharyngeal cancers. Although HPV vaccine currently is recommended only for females aged 11 through 26 years to prevent cervical cancer caused by sexual transmission of HPV, ongoing studies are evaluating the efficacy and safety of this vaccine for males.15
PHARMACIST INVOLVEMENT
History
From the mid-1800s until shortly before the 21st century, pharmacist involvement in immunization efforts consisted primarily of the acquisition, storage, and distribution of vaccines and the education of physicians and laypersons about vaccines.16 In 1994, fifty pharmacists attended the first organized immunization training program in Seattle. The following year, two Washington State pharmacists began administering influenza vaccine under collaborative practice agreements, thus ushering in the modern role of the pharmacist in preventing VPD.16
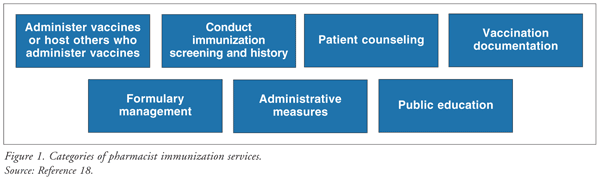
Current Roles and Opportunities
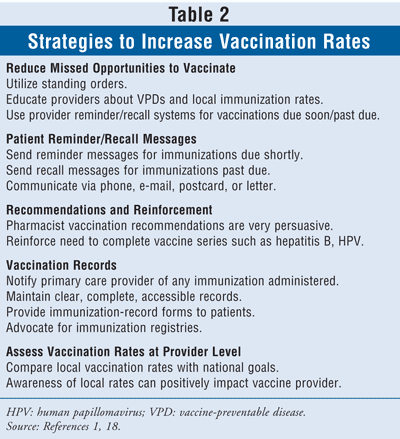
One of the 28 focus goals of Healthy People 2010, "Immunization and Infectious Diseases," is aimed at preventing disease, disability, and death from infectious diseases, including VPDs.17 The American Society of Health-System Pharmacists (ASHP) has identified several ways in which pharmacists in both community and organized health care settings can help minimize VPD (FIGURE 1).18 The ACIP recommends strategies to increase vaccination rates; these are encompassed in the ASHP guidelines for the role of the pharmacist in immunization (TABLE 2).1,18
Vaccine Administration: Pharmacists in all 50 states are now allowed to administer at least some vaccines.19 Pharmacists must become knowledgeable to best protect their patients against VPDs.18 The American Pharmacists Association offers a certificate program about VPDs and immunization techniques.20,21 At least 30,000 pharmacists have received immunization training.21 The National Community Pharmacists Association has a free online home-study program, "Creating an Immunization Niche in the Community Pharmacy: A Business Guide," approved by the Accreditation Council for Pharmacy Education for 8 continuing-education contact hours.22 Practitioners must stay informed about current trends in VPD and immunization recommendations.18 Pharmacists who do not administer vaccinations may host other health care professionals to do so, but they still have an obligation to educate and promote full immunization for their patients.18 While immunizations may be provided upon physician order for an individual patient, standing orders or protocols may help increase vaccination levels for some VPDs, such as influenza and pneumococcal disease. This type of practice is promoted by the ACIP.1,23
In a recent study, standing orders allowed pharmacists to vaccinate eligible inpatients against pneumococcal disease and influenza, resulting in significantly increased vaccination rates among high-risk patients.24 In another study, pharmacists in a lipid clinic vaccinated high-risk cardiovascular patients against influenza under a standing-order protocol, significantly improving vaccination rates.25
Screening and Counseling: Careful screening of patients' immunization history and appropriate counseling are valuable pharmacist contributions.18 Reminding providers of vaccines that are due soon or past due may help ensure that no patient needing vaccination is overlooked.1 Pharmacist vaccination or referral to other sources should be offered to eligible patients. Such activities may help reduce missed opportunities to vaccinate.1
Opportunities for screening arise in a variety of situations. For example, a patient who comes to the pharmacy to purchase bandages and antibiotic ointment for a cut might be questioned about the need for a tetanus booster.18 A new diagnosis of heart disease, diabetes, or chronic obstructive pulmonary disease should prompt the pharmacist to recommend influenza or pneumococcal immunization.18 Appropriate counseling must include provision of the most current Vaccine Information Statement developed by the CDC to provide accurate and authoritative information to persons being vaccinated or their guardians.18
Education and Guidance: Formulary management, including procurement, transportation, and proper storage of vaccines, is vitally important.18 Failure to store vaccines as recommended or the use of outdated products may leave vaccine recipients unprotected against disease.7 The pharmacist is well-suited to assume the role of educator in this area, offering guidance and instruction to other health care providers. Additionally, pharmacists may promote appropriate use of vaccines through various administrative measures, such as developing protocols to provide hepatitis B pre-exposure prophylaxis or increase vaccination rates among health care workers.18
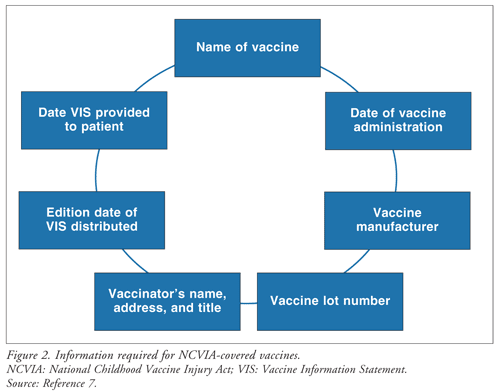
Documentation: Accurate documentation of vaccinations is crucial to ensure that patients who need vaccines receive them, while minimizing unnecessary revaccinations.7 All pharmacists who provide any vaccine covered by the National Childhood Vaccine Injury Act to a patient of any age must maintain a vaccination record with data specified by law, as noted in FIGURE 2.7 It is advisable to record this information for all vaccines administered. Records should be clear, accurate, and accessible, and the pharmacist should notify the recipient's primary care provider when a vaccination has been administered.1 Patients may be given immunization record cards, although these may become inaccurate if not presented for updating with every immunization.1 Pharmacists also may lobby for state immunization registries to enhance exchange of immunization-status information among providers.1
Public Education: Pharmacists have many opportunities to promote public education about VPDs, and these efforts are effective.18 New York, the next-to-last state to grant pharmacists the right to vaccinate, has immunization rates in the bottom third of all states.22,26 Pharmacists in a rural New York primary care clinic identified high-risk patients by chart review and mailed them education packets about influenza immunization; nurses later administered the influenza shots to patients. The vaccination rate increased from 28% prior to initiation of the intervention to 54% afterward.26 Pharmacists can utilize a variety of methods to disseminate information and provide education: phone, postcards, letters, brochures (mailed or distributed in the pharmacy or other practice sites), e-mail, radio, television, newspapers and other printed material, presentations to community and professional groups, and participation in public events such as health fairs. Regardless of venue or modality, it is critically important that pharmacists always provide accurate information. Several credible sources for pharmacists, other health care providers, and the public are listed in TABLE 3.

Areas for Improvement
Physician Involvement: In the U.S., significant progress has been made in improving vaccination coverage and reducing VPDs, but much work remains to be done.17 Serious vaccine-preventable illnesses such as influenza and pneumonia occur among adults, particularly those over age 65, or in people of any age with certain chronic diseases.17 With the aging of the baby boomers, larger numbers of Americans will be at increased risk for morbidity and mortality from VPDs.17 Healthy People 2010 set a goal for influenza and pneumococcal-disease immunization rates of 90% for persons aged 65 and older, yet coverage rates as of 2007 were only 69% and 66%, respectively, for these diseases.17,27
Statistics such as these prompted the American College of Physicians (ACP) to state that physicians are obligated to champion and deliver all recommended immunizations or refer patients to settings where they can receive these services.28 In a position statement on pharmacist scope of practice, the ACP-American Society of Internal Medicine (ACP-ASIM) supported the role of pharmacists as immunizers, immunization-information sources, and hosts of immunization sites.29 The ACP-ASIM also affirmed its willingness to work with pharmacy organizations to promote immunization awareness.
Noncompliance: Modern vaccines are safe, effective, and capable of preventing a host of deadly or debilitating diseases.5,7,30 Nevertheless, Americans are alarmingly complacent and inadequately informed about VPDs, and many citizens remain unvaccinated either by choice or by circumstance.17,30,31 Annually in the U.S., influenza accounts for approximately 36,000 deaths, hepatitis A claims 100 lives, and cervical cancer kills 3,700 women.32 In fact, VPDs kill more Americans annually than breast cancer, HIV/AIDS, or traffic accidents.27
Unfortunately, laypersons are not alone in failing to avail themselves of life-saving vaccines. A 2006 National Health Interview Survey showed a 41.7% influenza vaccination rate for health care workers.33 Pharmacists could lead the way in improving these statistics by complying with ACIP vaccination recommendations and urging other health care workers to follow suit.
CONCLUSION
Pharmacists have made great strides in their efforts to reduce VPDs since becoming involved in the immunization initiative. The potential positive impact on public health is enormous, and this new role may be an important stimulant to pharmacists transitioning from dispensers to providers of direct patient care.16 The Oath of a Pharmacist seems to speak directly to those pharmacists who choose to participate in the fight against VPDs: "I will consider the welfare of humanity and relief of human suffering my primary concerns.…I will embrace and advocate changes that improve patient care."34
Acknowledgment: The author thanks Linda K. Ohri, PharmD, MPH, for her expertise regarding vaccine-preventable diseases, and Edward M. DeSimone II, RPh, PhD, FAPhA, for reviewing a draft of the manuscript.
REFERENCES
1. Atkinson W, Hamborsky J, McIntyre L, Wolfe S, eds. Epidemiology and Prevention of Vaccine-Preventable Diseases. 10th ed. Washington, DC: Public Health Foundation; 2008.
2. US Department of Health and Human Services (HHS). Healthy People 2010. Midcourse Review. 14: Immunization and infectious diseases. Emerging issues.
www.healthypeople.gov/data/
3. Centers for Disease Control and Prevention (CDC). Recommended immunization schedules for persons aged 0-18 years--United States, 2009. MMWR. 2009;57:Q1-Q4.
4. CDC. Recommended adult immunization schedule--United States, 2009. MMWR. 2009;57:Q1-Q4.
5. Roush SW, Murphy TV, Vaccine-Preventable Disease Table Working Group. Historical comparisons of morbidity and mortality for vaccine-preventable diseases in the United States. JAMA. 2007;298:2155-2163.
6. Stergachis A. Promoting the pharmacist's role in public health. J Am Pharm Assoc. 2006;46:311-312.
7. CDC. General recommendations on immunization: recommendations of the Advisory Committee on Immunization Practices (ACIP). MMWR. 2006;55:1-48.
8. Associated Press. Too many adults skip vaccines, officials say. January 23, 2008.
www.msnbc.msn.com/id/22801165. Accessed May 23, 2008.
9. Euler GL, Lu P, Singleton JA. Vaccination coverage among U.S. adults. National Immunization Survey-Adult, 2007. CDC.
www.cdc.gov/vaccines/stats-
10. Smith M. Americans found indifferent to adult immunizations. MedPage Today.
www.medpagetoday.com/
11. CDC Health Advisory. Measles outbreaks in the United States: public health preparedness, control and response in healthcare settings and the community.
www2a.cdc.gov/HAN/ArchiveSys/
12. Immunization Action Coalition. Vaccines in the news.
www.immunize.org/vaccinenews/. Accessed May 23, 2008.
13. Bakalar N. Oral cancer in men associated with HPV. New York Times. May 13, 2008.
www.nytimes.com/2008/05/13/
14. Worden FP, Kumar B, Lee JS, et al. Chemoselection as a strategy for organ preservation in advanced oropharynx cancer: response and survival positively associated with HPV 16 copy number. J Clin Oncol. 2008;26:3138-3146.
15. Atkinson W, Wolfe S, Hamborsky J, McIntyre L, eds. Epidemiology and Prevention of Vaccine-Preventable Diseases. 11th ed. Washington, DC: Public Health Foundation; 2009:123-133.
16. Hogue MD, Grabenstein JD, Foster SL, Rothholz MD. Pharmacist involvement with immunizations: a decade of professional advancement. J Am Pharm Assoc. 2006;46:168-182.
17. HHS. Healthy People 2010. 14: Immunization and infectious diseases.
www.healthypeople.gov/
18. ASHP Council on Professional Affairs. ASHP guidelines on the pharmacist's role in immunization. Am J Health Syst Pharm. 2003;60:1371-1377.
19. Egervary A. Maine legislature approves pharmacist immunization. American Pharmacists Association (APhA).
www.pharmacist.com/AM/
20. Pharmacy-based immunization delivery. APhA.
www.pharmacist.com/Content/
21. APhA. States where pharmacists can immunize.
www.pharmacist.com/AM/
22. National Community Pharmacists Association. Creating an immunization niche in the community pharmacy: a business guide.
www.cecity.com/ce-bin/owa/pkg_
23. CDC. Prevention and control of influenza: recommendations of the Advisory Committee on Immunization Practices (ACIP), 2007. MMWR. 2007;56:1-54.
24. Bourdet SV, Kelley M, Rublein J, Williams DM. Effect of a pharmacist-managed program of pneumococcal and influenza immunization on vaccination rates among adult inpatients. Am J Health Syst Pharm. 2003;60:1767-1771.
25. Loughlin SM, Mortazavi A, Garey KW, et al. Pharmacist-managed vaccination program increased influenza vaccination rates in cardiovascular patients enrolled in a secondary prevention lipid clinic. Pharmacotherapy. 2007;27:729-733.
26. Amburgh JA, Waite NM, Hobson EH, Migden H. Improved influenza vaccination rates in a rural population as a result of a pharmacist-managed immunization campaign. Pharmacotherapy.
27. Boyles S. CDC: adult vaccination rates too low. WebMD Health News.
www.medicinenet.com/script/ 2001;21:1115-1122.
28. Poland GA, Schaffner W. Adult immunization guidelines: a patient safety and quality-of-care issue. Ann Int Med. 2007;147:735-737.
29. Keely JL, American College of Physicians-American Society of Internal Medicine. Pharmacist scope of practice. Ann Int Med. 2002;136:79-85.
30. National Foundation for Infectious Diseases (NFID). National survey on adult vaccination reports low consumer awareness of vaccines and the risks of vaccine-preventable diseases.
www.nfid.org/pdf/factsheets/
31. HHS. Healthy People 2010. Midcourse Review. 14: Immunization and infectious diseases. Progress toward healthy people 2010 targets.
www.healthypeople.gov/data/
32. NFID. Facts about adult immunization.
www.nfid.org/pdf/factsheets/
33. CDC. Table: Self-reported influenza vaccination coverage trends 1989-2006 among adults by age group, risk group, race/ethnicity, health-care worker status, and pregnancy status, United States, National Health Interview Survey (NHIS).
www.cdc.gov/flu/professionals/
34. American Association of Colleges of Pharmacy. Oath of a pharmacist.
www.aacp.org/resources/





