US Pharm. 2024;49(4):38-42.
ABSTRACT: Childhood abuse, which manifests in adverse childhood events such as neglect and physical, sexual, and emotional abuse, is widespread in the United States. Each year, the Child Protective Services agency rescues more than one-half million children from maltreatment. Because of their accessibility, pharmacists are well positioned to save lives and enhance overall societal health by identifying and reporting child abuse. The pharmacist’s role includes being knowledgeable about child abuse, recognizing signs of abuse, identifying characteristics of perpetrators, handling disclosures, and reporting suspected abuse to the appropriate authorities. Being equipped with information on identifying and reporting child abuse enables pharmacists to break the cycle of abuse across the U.S., thereby safeguarding the most vulnerable members of society.
Child abuse, a known issue across the United States, has a high incidence; more than 61% of persons report having experienced at least one adverse childhood event (ACE) before age 18 years.1 ACEs encompass a variety of traumatic situations, including physical, sexual, and emotional abuse as well as neglect and household dysfunction, and they have widespread effects on both the individual and society as a whole. Child abuse, maltreatment, and neglect impact children of all ages, races, ethnicities, and sociodemographic backgrounds.2
Trauma related to ACEs lingers into adulthood, with survivors having an increased risk of chronic health conditions (e.g., severe obesity, diabetes, heart disease, cancer, chronic obstructive pulmonary disease, stroke, mental health conditions) and early death.3 Mental health problems associated with ACEs and trauma include posttraumatic stress disorder (PTSD), anxiety, depression, substance use, suicidal ideation, smoking, inefficient coping mechanisms, decreased emotional self-regulation, and lower likelihood of thriving in adulthood.4 The 1998 CDC–Kaiser Permanente ACE Study found a robust link between the breadth of ACEs experienced and adult health outcomes.5 In a 2013 study conducted in urban Philadelphia, up to 83% of participants had experienced at least one ACE in their lifetime.6
Given the severe consequences and poor health outcomes in survivors of childhood trauma, healthcare professionals (HCPs) have a key responsibility to identify and report abuse. Pharmacist involvement has expanded beyond the hospital setting to include community-based clinical services, which continue to grow. Pharmacists can immunize children in 50 states and provide oral contraceptive care in 25 states and the District of Columbia.7,8 Additionally, because patients visit a pharmacist 12 times more often than they see their primary care physician, pharmacists have more opportunities for identifying abuse.9 This article will explore the pharmacist’s role in knowing the specifics of child abuse, recognizing signs of abuse, identifying traits of perpetrators, handling disclosures sensitively, and reporting suspected abuse to the appropriate authorities. Child abuse is a rampant nationwide issue that cycles down through the generations. As the most accessible HCPs in the country, pharmacists can not only save lives but also affect overall health for generations to come.10
Types of Childhood Trauma and Abuse
The National Children’s Alliance reported that in 2018, an estimated 678,000 U.S. children were survivors of abuse and neglect.11 Each year, the Child Protective Services (CPS) agency rescues more than 650,000 children from maltreatment.12 Childhood trauma can consist of either a single incident (known as acute trauma) or repeated or continuous incidents (called chronic trauma). Additionally, trauma is not always one specific type but can be a mix of multiple kinds of abuse or several unrelated circumstances (referred to as complex trauma).
Individual trauma is often described as a set of circumstances that a person experiences as physically or emotionally harmful or life-threatening and has lasting adverse effects on the person’s functioning and mental, physical, social, emotional, or spiritual well-being.13,14 Although trauma is individualized and adverse effects are subjective among individuals, common types of trauma include ACEs, sociocultural trauma, generational trauma, institutional and structural racism, and collective or community-level trauma.15 Circumstances such as threatened death, severe illness or injury, accidents, death of loved ones, divorce, mental health conditions, substance use, interpersonal violence, and incarceration of family members are other sources of trauma.16 Types of trauma experienced differ among individuals, but trauma is generally considered anything that causes a person harm and involves a heightened sense of fear, helplessness, feelings of being overwhelmed, or isolation.14
Effects of Trauma and Abuse
For the millions of survivors of childhood abuse and trauma, effects occurring during and after the abuse can precipitate significant mental and physical distress. Trauma and abuse initially trigger physiological responses such as stress, increased cortisol, and wiring of the brain for “fight, flight, freeze, or fawn” responses. The fight, flight, freeze, or fawn responses originate in the amygdala (the brain’s fear and emotion processing center), bypassing the executive-function section of the brain, which helps process decisions and solve problems.17 In the fight response, the reaction to a perceived threat is to confront the perceived threat with aggression. The flight response is the desire to flee from perceived threats, and the freeze response is the inability to move or respond to the threat. The fawn reponse is an attempt to please others in hopes of avoiding a conflict or danger.18
Being in a chronic state of fight, flight, freeze, or fawn responses can alter brain chemistry and emotional-regulation pathways, resulting in reduced resiliency and impaired executive cognitive function and limiting natural coping ability.17 These chronic stress and learned-response patterns in the brain often lead survivors to have difficulty with daily performance, such as at work and school, as well as impaired relationships with family, friends, children, colleagues, and intimate partners.
Survivors are three to four times more likely to experience mental health conditions such as PTSD, dissociative and personality disorders, anxiety, sleep disturbances, eating disorders, suicidal ideation, and depression.19 Additionally, survivors of rape and sexual assault have up to a 70% incidence of severe psychological effects and are 26 times more likely to have chronic substance use disorder.20,21 Unfortunately, because of inaccessibility, unaffordability, fear of disclosure, and many other factors, these mental health conditions often go untreated and cause more suffering for survivors.22
Survivor Signs and Symptoms
Pharmacists who are trained in trauma and how to detect it can perceive signs of abuse during encounters with children, whether in the inpatient or outpatient setting.23 Acute cognitive signs and symptoms in survivors may include changes in attitude, personality, or behavior, such as hostility, aggression, fearfulness, withdrawal, avoidance behaviors, and limiting or avoiding being alone or having physical contact.24 Acute biological indicators include unexplained injuries, bruises, fractures, and other injuries inconsistent with the explanation the patient provides when questioned.25 Survivors may also have long-term health conditions such as diabetes, obesity, asthma, gastrointestinal disorders, pain syndromes, sexually transmitted infections, substance use disorder, HIV, and direct injuries from self-harm or abuse.26
Perpetrator Characteristics
Because of limited reporting, research is conflicting on many factors of childhood abuse. However, it has been found that abusers or perpetrators are often individuals who are close to the survivor.27 The majority of children and adolescents report family members, specifically parents, as the main perpetrators, whereas adult survivors name primarily intimate partners as perpetrators, and only one-third of perpetrators are nonfamily or acquaintances. Not only are abusers typically close to their victims, traditionally they are also well-liked by others, are considered charming and charismatic, and are seen as successful or well-known in the community.28 It is essential to note, however, that the personality traits of some perpetrators may differ because of the increasing use of online and technological modalities as avenues for childhood abuse.29
Although personality traits may differ, there are some behavioral signs that are common in abusers. Behavioral characteristics include impulsive decision-making and the inability to stop one’s reaction despite consequences; being narcissistic or overly critical; having poor self-concept or low self-esteem; being jealous; lacking empathy; being hypersensitive or overactive; and, lastly, controlling or manipulating others.30 Environmental signs can also help identify individuals at risk for being or becoming a perpetrator. Environmental characteristics include personally being a survivor of childhood abuse or neglect, having minimal friendships or emotional support, experiencing life crises, having poor mental or physical health, and having marital or relationship problems.31
The Cycle of Abuse
Social, familial, or community attitudes of secrecy toward and normalizing of abuse have led these behaviors to be perpetuated from generation to generation. Abuse is often passed down through the generations, resulting in a cycle of trauma. Those who were once survivors have a fourfold risk of becoming perpetrators themselves, and female survivors tend to continue being victimized throughout adulthood.32 Therefore, it is critical that observers take action to report any signs, symptoms, or red flags even without confirmation or evidence that abuse is occurring. Hesitation over reporting helps perpetuate the cyclical nature of abuse, and it takes vigilance on the part of others, including pharmacists, to break the cycle.33
Disclosure and Suspicion of Abuse
The pharmacist’s role in recognizing child abuse is critically important, and it typically starts when the pharmacist suspects harm or when the patient discloses that abuse has been or is occurring. Accordingly, the pharmacist should be prepared to handle these situations, which typically occur when least expected. A disclosure plan can help the pharmacist safely and appropriately navigate situations that may arise during medication counseling, OTC recommendations, vaccine administration, point-of-care testing, and other activities that may reveal possible signs of abuse.
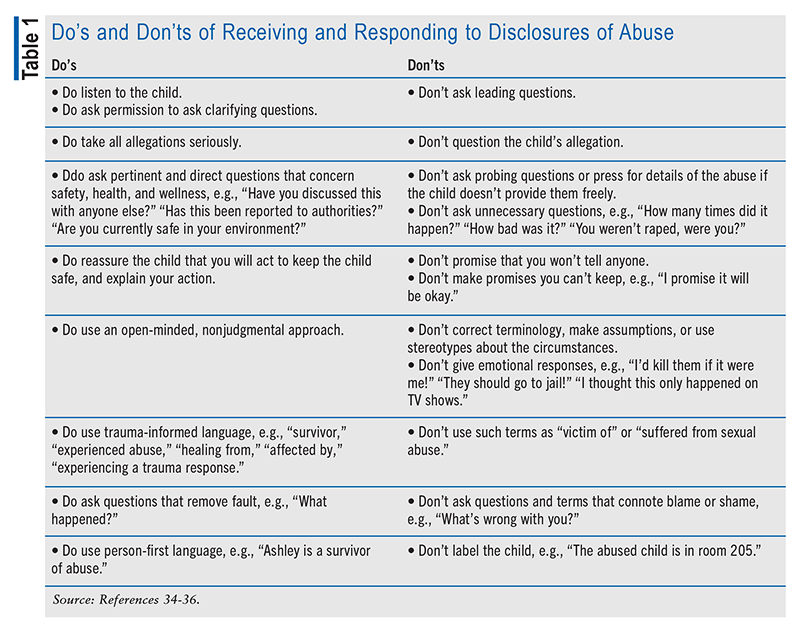
A pharmacist’s disclosure plan should always begin with providing a safe, comfortable space for patients to discuss any issues they are experiencing. It is essential for pharmacists to inform a patient who reports harm, abuse, or neglect that they are required to report this information for the patient’s own protection. TABLE 1 presents additional best practices for receiving and responding to disclosures of abuse, including critical steps to avoid alienating the survivor (e.g., keeping all questions pertinent to the survivor’s safety and well-being). The pharmacist should refrain from asking clarifying questions without the patient’s permission and avoid questions that have no bearing on reporting (e.g., the severity or exact details of the abuse), which could come across as intrusive, embarrassing, and even dismissive.34-36
Reporting Abuse
A lack of reporting contributes greatly to the perpetuation of abuse cycles, and it is estimated that only around 12% of cases in the U.S. are reported.37 Because patients visit a pharmacist—one of the most trusted HCPs in the U.S.—far more more than their primary care provider, pharmacists are ideally situated to address this issue nationwide.38,39 Pharmacists should report all red flags observed, regardless of the patient’s age or whether abuse is disclosed or confirmed. It should be remembered that reporting is anonymous and that if no abuse is taking place, there are no negative consequences for the reporter because the report was made in good faith and in the patient’s best interest. If a pharmacist suspects that a vulnerable party is experiencing any harm or neglect, including but not limited to physical, emotional, and sexual abuse, the pharmacist should immediately report these concerns to local authorities.
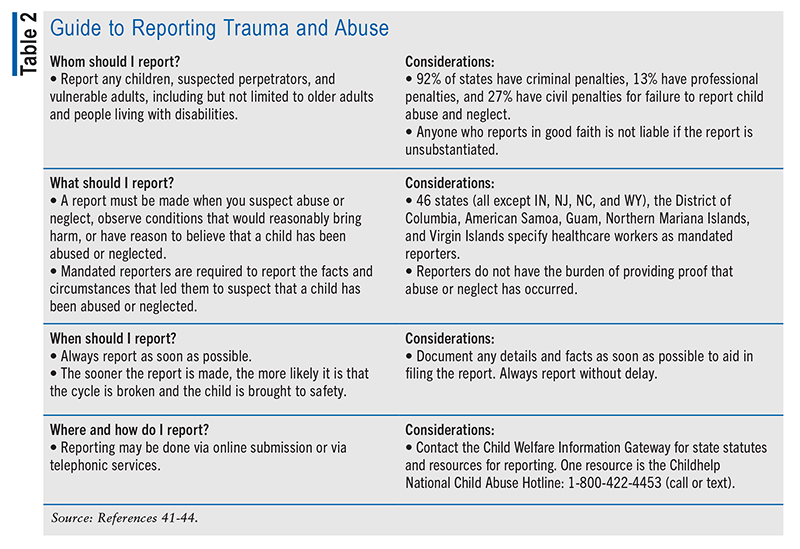
To make a report, it is not necessary to know the details or severity of the circumstances or event or to have confirmation. Pharmacists are required to report only what they know about the circumstances leading to the suspicion of abuse or neglect, and they do not have to provide proof.40 Even if the pharmacist does not know the name of the child or any individuals who are with the child, suspicions or observations should be reported without delay; lack of details has no bearing on the pharmacist’s responsibility to report, and authorities will determine the details. Prompt reporting of any suspicious signs or activities will increase the likelihood that the child is spared further harm. It also must be kept in mind that the situation will be investigated by authorities, so pertinent information should be shared only with necessary parties. TABLE 2 offers a simple guide to reporting trauma and abuse.41-44
In some states, a mandated reporter who fails to report suspected neglect or abuse may be held legally liable. Because pharmacists may find themselves in the position to report child abuse, they should keep abreast of state-specific reporting requirements. In most U.S. states and territories, pharmacists are specified as mandated reporters of child abuse.45 Some patient-centered measures pharmacists can take include identifying local referral sources, learning about reporting protocols, providing patients with educational pamphlets, and preparing to properly and safely manage potential disclosures.37 Pharmacists’ ability to identify and report suspected child abuse helps save children from the cycle of abuse and enhances society as a whole.
Conclusion
As part of their job, pharmacists routinely interact with patients, including children. The indispensable nature of the role of pharmacists in identifying and reporting child abuse cannot be overstated. As frontline HCPs, pharmacists are well positioned to observe and recognize potential signs of abuse during their interactions with children and their caregivers. Pharmacists should be equipped with the knowledge to identify red flags, formulate disclosure plans, and act in the child’s best interest by reporting to authorities. Fostering a collaborative healthcare environment that includes pharmacists within the more extensive network of CPS enables improved safeguarding of the most vulnerable members of society and assists in breaking the cycle of abuse.
REFERENCES
1. CDC.gov. Fast facts: preventing adverse childhood experiences. www.cdc.gov/violenceprevention/aces/fastfact.html. Accessed February 2, 2024.
2. Schilling S, Christian CW. Child physical abuse and neglect. Child Adolesc Psychiatr Clin N Am. 2014;23(2):309-319.
3. Sebalo I, Königová MP, Sebalo Vňuková M, et al. The associations of adverse childhood experiences (ACEs) with substance use in young adults: a systematic review. Subst Abuse. 2023;17:11782218231193914.
4. Goldenson J, Kitollari I, Lehman F. The relationship between ACEs, trauma-related psychopathology and resilience in vulnerable youth: implications for screening and treatment. J Child Adolesc Trauma. 2021;14:151-160.
5. Felitti VJ, Anda RF, Nordenberg D, et al. Relationship of childhood abuse and household dysfunction to many of the leading causes of death in adults. The Adverse Childhood Experiences (ACE) Study. Am J Prev Med. 1998;14(4):245-258.
6. Dempsey S, Fein J, Kuykendall SA, et al. Findings from the Philadelphia Urban ACE Survey. Robert Wood Johnson Foundation. www.rwjf.org/en/insights/our-research/2013/09/findings-from-the-philadelphia-urban-ace-survey.html. Accessed February 2, 2024.
7. Hughes RH IV, Choudhury S. Recognizing pharmacists as Vaccines For Children providers. Health Affairs Forefront. February 23, 2023. www.healthaffairs.org/content/forefront/recognizing-pharmacists-vaccines-children-providers. Accessed February 2, 2024.
8. National Conference of State Legislatures. State contraception policies. www.ncsl.org/health/state-contraception-policies. Accessed February 2, 2024.
9. Strand MA, Bratberg J, Eukel H, et al. Community pharmacists’ contributions to disease management during the COVID-19 pandemic. Prev Chronic Dis. 2020;17:e69.
10. Hedima EW, Adeyemi MS, Ikunaiye NY. Community pharmacists: on the frontline of health service against COVID-19 in LMICs. Res Social Adm Pharm. 2021;17(1):1964-1966.
11. National Children’s Alliance. National statistics on child abuse. www.nationalchildrensalliance.org/media-room/national-statistics-on-child-abuse. Accessed February 2, 2024.
12. Cerulli C, Inoue S, Cerulli J. How to identify, assess, and refer patients experiencing interpersonal violence across the lifespan: the role of US pharmacists in integrated pharmacy research and practice. Integr Pharm Res Pract. 2019;8:115-125.
13. Berliner L, Kolko DJ. Trauma informed care: a commentary and critique. Child Maltreat. 2016;21(2):168-172.
14. Center for Substance Abuse Treatment. Trauma-Informed Care in Behavioral Health Services. Rockville, MD: Substance Abuse and Mental Health Services Administration; 2014.
15. Cénat JM. Complex racial trauma: evidence, theory, assessment, and treatment. Perspect Psychol Sci. 2023;18(3):675-687.
16. Child and Adolescent Health Measurement Initiative. Data Resource Center for Child & Adolescent Health. www.childhealthdata.org. Accessed February 2, 2024.
17. Šimić G, Tkalčić M, Vukić V, et al. Understanding emotions: origins and roles of the amygdala. Biomolecules. 2021;11(6):823.
18. Davis S. Rejection trauma and the freeze/fawn response. CPTSD Foundation. https://cptsdfoundation.org/2022/02/21/rejection-trauma-and-the-freeze-fawn-response. Accessed February 2, 2024.
19. RAINN. Children and teens: statistics. www.rainn.org/statistics/children-and-teens. Accessed February 2, 2024.
20. Kilpatrick DG. The mental health impact of rape. National Violence Against Women Prevention Research Center. https://mainweb-v.musc.edu/vawprevention/research/mentalimpact.shtml. Accessed February 2, 2024.
21. RAINN. Victims of sexual violence: statistics. www.rainn.org/statistics/victims-sexual-violence. Accessed February 2, 2024.
22. Mongelli F, Georgakopoulos P, Pato MT. Challenges and opportunities to meet the mental health needs of underserved and disenfranchised populations in the United States. Focus. 2020;18(1):16-24.
23. Center for Substance Abuse Treatment. Screening and assessment. In: Trauma-Informed Care in Behavioral Health Services. Rockville, MD: Substance Abuse and Mental Health Services Administration; 2014.
24. Whitten C. What to know about being an adult survivor of child abuse. WebMD. www.webmd.com/sex-relationships/features/what-to-know-adult-survivor-child-abuse. Accessed February 2, 2024.
25. Christian CW; Committee on Child Abuse and Neglect, American Academy of Pediatrics. The evaluation of suspected child physical abuse. Pediatrics. 2015;135(5):e1337-e1354.
26. Springer KW, Sheridan J, Kuo D, Carnes M. The long-term health outcomes of childhood abuse. An overview and a call to action. J Gen Intern Med. 2003;18(10):864-870.
27. Levine JA, Dandamudi K. Prevention of child sexual abuse by targeting pre-offenders before first offense. J Child Sex Abus. 2016;25(7):719-737.
28. National Coalition Against Domestic Violence. Signs of abuse. https://ncadv.org/signs-of-abuse. Accessed February 2, 2024.
29. Lim YY, Wahab S, Kumar J, et al. Typologies and psychological profiles of child sexual abusers: an extensive review. Children (Basel). 2021;8(5):333.
30. Petherbridge L. 12 traits of an abuser. Christian Broadcasting Network. www2.cbn.com/article/marriage/12-traits-abuser. Accessed February 2, 2024.
31. Rokach A, MacFarlane K. Abused children and their relationships as adults. J Psychol Mental Health Care. 2021;5(3):1-14.
32. Egeland B, Jacobvitz D, Sroufe LA. Breaking the cycle of abuse. Child Dev. 1988;59(4):1080-1088.
33. Rakovec-Felser Z. Domestic violence and abuse in intimate relationship from public health perspective. Health Psychol Res. 2014;2(3):1821.
34. Barnert E, Kelly M, Godoy S, et al. Understanding commercially sexually exploited young women’s access to, utilization of, and engagement in health care: “work around what I need.” Womens Health Issues. 2019;29(4):315-324.
35. Lederer LJ, Wetzel CA. The health consequences of sex trafficking and their implications for identifying victims in healthcare facilities. Ann Health Law. 2014;23:61-91.
36. James D. What is trauma informed language? Friends Association. https://friendsassoc.org/what-is-trauma-informed-language/. Accessed January 25, 2024.
37. Hanson RF, Resnick HS, Saunders BE, et al. Factors related to the reporting of childhood rape. Child Abuse Negl. 1999;23(6):559-569.
38. Advisory Board. Charted: the most trusted professions in America, according to Gallup. www.advisory.com/daily-briefing/2023/01/18/trusted-professionals. Accessed February 2, 2024.
39. Newman TV, Hernandez I, Keyser D, et al. Optimizing the role of community pharmacists in managing the health of populations: barriers, facilitators, and policy recommendations. J Manag Care Spec Pharm. 2019;25(9):995-1000.
40. Child Welfare Information Gateway. Penalties for Failure to Report and False Reporting of Child Abuse and Neglect. Washington, DC: U.S. Department of Health and Human Services, Children’s Bureau; 2019.
41. Healthwise Staff. Abuse in vulnerable adults. Kaiser Permanente. https://healthy.kaiserpermanente.org/health-wellness/health-encyclopedia/he.abuse-in-vulnerable-adults.abs2272. Accessed February 2, 2024.
42. Weigensberg EC, Islam N, Knab J, et al. State Child Abuse and Neglect (SCAN) policies database 2019. www.ndacan.acf.hhs.gov/datasets/dataset-details.cfm?ID=245. Accessed March 5, 2024.
43. Child Welfare Information Gateway. Mandatory reporters of child abuse and neglect. www.flls.org/wp-content/uploads/2013/10/Mandatory-Reporting-State-Statutes.pdf. Accessed February 2, 2024.
44. Child Welfare Information Gateway. State statutes search. www.childwelfare.gov/resources/states-territories-tribes/state-statutes. Accessed February 2, 2024.
45. Barnard M, Sinha A, Sparkmon WP, Holmes ER. Reporting interpersonal violence and abuse: what pharmacists need to know. J Am Pharm Assoc (2003). 2020;60(6):e195-e199.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





