US Pharm. 2023;48(4):24.
Proper use of preexposure prophylaxis (PrEP; the administration of medication before and throughout periods of potential HIV exposure) can reduce the risk of sexually transmitted HIV infection by up to 99% and transmission from injection drug use by 74%. According to the CDC, only about 25% of the 1.2 million people eligible for PrEP in the United States were prescribed medication in 2020. Although this is a substantial increase from 3% in 2015, PrEP remains underutilized nationwide. To address this gap, the U.S. Department of Health and Human Services launched the cross-agency initiative Ending the HIV Endemic, whose goals are to increase PrEP use among PrEP-eligible individuals to 50% and reduce new HIV infections at least 90% by 2030.
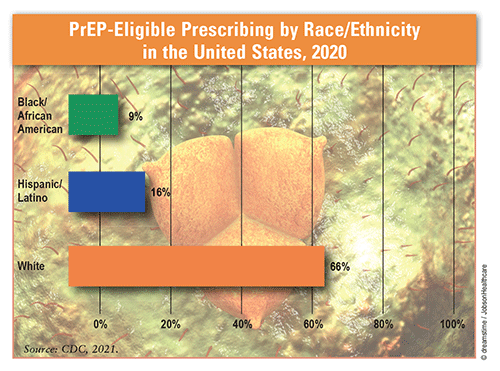
PrEP Prescribing: Rates of new HIV infections among blacks/African Americans and Hispanics/Latinos are more than eight times and almost four times, respectively, the rate in whites. Despite representing populations for whom PrEP is most recommended, only 9% of blacks/African Americans and 16% of Hispanics/Latinos received PrEP prescriptions in 2020, versus 66% of whites. PrEP use also varied by sex and age group: The percentage of females receiving PrEP coverage was almost three times lower than that for males (10% vs. 28%, respectively), and about 16% of PrEP-eligible individuals aged 16 to 24 years received PrEP compared with 27% and 30% of PrEP-eligible individuals aged 25 to 34 years and 35 to 44 years, respectively.
COVID-19 Impact: Analysis of the IQVIA Real World Data Longitudinal Prescriptions Database (representing 92% of prescriptions dispensed by U.S. retail pharmacies and >60% of those from U.S. mail-order outlets) revealed a 22% reduction in predicted PrEP prescriptions and a 25% reduction in predicted new PrEP users during the COVID-19 pandemic (March 2020 to March 2021). The greatest reductions in PrEP use during this time were among persons aged 16 to 29 years and persons with commercial health insurance for whom out-of-pocket costs may have been a barrier.
Pharmacist Authority: Most U.S. healthcare professionals who prescribe PrEP are physicians (68.1%), followed by nurse practitioners (20.8%), physician assistants (8.9%), and other provider types (2.2%). The CDC has identified pharmacists as key healthcare professionals who can improve PrEP use, as more than 85% of U.S. PrEP prescriptions are dispensed at commercial pharmacies. A recent study found a 24% increase in PrEP prescriptions after 1 year of expanding pharmacist prescriber authority for HIV PrEP medications, and a 110% increase after 2 years. Another study determined that patients strongly support pharmacists: 100% of surveyed patients agreed or strongly agreed that pharmacist-prescribed PrEP services would benefit their community. Twenty states have enacted or proposed legislation allowing pharmacists to initiate PrEP and/or HIV postexposure prophylaxis without a prescription.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





