US Pharm. 2022;47(12):14.
Eosinophilic esophagitis (EoE) is a chronic, immune-mediated disease in which eosinophils accumulate in the esophagus, leading to inflammation and esophageal dysfunction. Commonly characterized by heartburn, chest or abdominal pain, dysphagia, difficulty eating, esophageal damage, and/or food impaction, EoE can mimic other gastrointestinal (GI) conditions involving elevated eosinophils in the esophagus (e.g., gastroesophageal reflux disease, inflammatory bowel disease, celiac disease). Appropriate diagnosis of EoE via upper endoscopy and esophageal-lining biopsy is essential to decrease eosinophil levels in the esophagus, prevent or minimize damage to esophageal tissue, and manage symptoms.
Etiology and Risk Factors: According to the American Gastroenterological Association, EoE is believed to be caused by a chronic T helper type 2 immune hypersensitivity response to one or more allergens. Individuals with food or environmental allergies, asthma, eczema, chronic respiratory disease, family history of EoE, or living in a cold or dry climate are at greatest risk for developing the disease. EoE has a bimodal peak, with most cases diagnosed in the pediatric age group or in the third decade of life. It has also been diagnosed in 2% to 6.5% of patients undergoing esophagogastroduodenoscopy (the rate increases to 12% to 22% in those with manifestations of dysphagia).
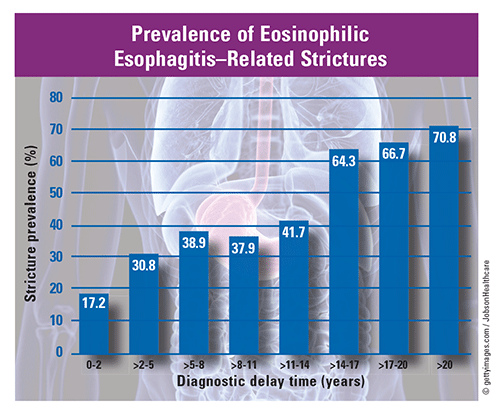
Prevalence and Consequences: EoE prevalence has increased over the past 2 decades, nearly doubling in both adults and children, and occurring in an estimated one in 1,500 to 2,000 persons. EoE affects more adults than children (19.1 cases/100,000 vs. 5.1 cases/100,000 persons per year, respectively) and is three times more prevalent in men than women. The National Institute for Occupational Safety and Health notes that EoE prevalence among individuals exposed to aeroallergens during World Trade Center (WTC) rescue efforts is 13-fold greater than in those with GI symptoms but no WTC aeroallergen exposure. In addition to dysphagia and food impaction, EoE can lead to serious complications (e.g., esophageal strictures, ulcers, polyps), frequently due to diagnostic delays. Over a 10-year period, National (Nationwide) Inpatient Sample data revealed increases in annual numbers of EoE-related hospital discharges (56,440 to 63,456 patients), average total hospital costs ($23,967 to $57,361), and average length of stay (5.6 days to 6.3 days).
Management: In May 2022, the FDA approved dupilumab (Dupixent), a monoclonal antibody already indicated for several other conditions, as the first and only medication to treat EoE. According to the American College of Gastroenterology, GI signs and symptoms consistent with EoE should be addressed promptly after an accurate diagnosis. Therapeutic interventions include dietary changes, pharmacologic treatment, and/or endoscopic procedures to reduce the eosinophils and inflammation in the esophagus. Although EoE has no cure, symptoms can be managed, and many individuals can maintain their quality of life.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





