US Pharm. 2018;43(12):12.
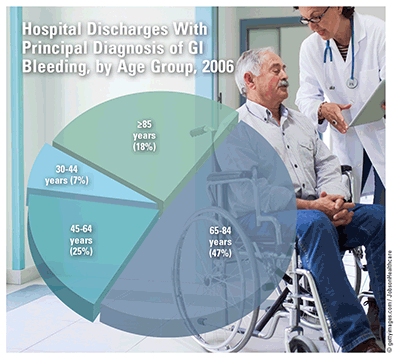
According to the CDC, gastrointestinal (GI) hemorrhage was the commonest diagnosis for all GI-related hospital stays in 2006, followed by diverticulosis and diverticulitis. In 2006, the majority of GI-bleed patients (47%) were aged 65 to 84 years, whereas patients aged 30 to 44 years were least likely (7%) to have this diagnosis; patients aged 45 to 64 years and those aged 85 years and older accounted for 25% and 18% of cases, respectively. Despite advances in diagnosis and treatment, overall inpatient mortality from GI bleeding remained about 4% from 1998 to 2006; however, it declined 31% in patients aged 30 to 44 years.
Lower-GI Bleeding: Lower-GI bleeding occurs at a rate of 36.5 per 100,000 in the adult population, and each year approximately 20 patients per 100,000 are hospitalized. It is estimated that diverticular bleeding occurs in 70,000 of 200,000 diverticulitis patients hospitalized each year. From 1998 to 2006, the number of hospitalizations for lower-GI bleeding increased by 8%. In 2006, among inpatients with lower-GI bleeding, diverticulosis/diverticulitis and hemorrhage (63.7%) were the most frequent diagnoses. Additionally, 16.3% of patients were diagnosed with rectal and anal hemorrhage, 12.3% with diverticulosis/diverticulitis of the small intestine, and 7.6% with perforation of the large intestine. During this period, the largest increase was seen in rectal and anal hemorrhage (up 41%). Lower-GI bleeding accounted for 24.2% of all hospital diagnoses of GI bleeding.
Upper-GI Bleeding: Of all hospital discharges for GI bleeding, upper-GI bleeding was the most frequent diagnosis (100,000 annually; 45.1%), but it resulted in the least number of deaths (2.7%). More than 53% of cases of upper-GI bleeding were caused by an underlying gastric or duodenal condition, gastrojejunal ulcers, or perforations, and in nearly 6% of cases the cause was stomach and duodenal angiodysplasia with hemorrhage. Esophageal varices, ulcer, perforation, and other hemorrhage accounted for 14% of cases. Hematemesis occurred in 8% of cases of upper-GI bleeding, and gastritis or duodenitis and hemorrhage occurred in nearly 18%. The hospitalization rate for upper-GI bleeding decreased 15% (from 96 to 82 cases per 100,000) between 1998 and 2006, with the largest declines in gastritis/duodenitis (–31%) and upper-GI ulcers (–25%). The number of hospital patients who died from upper-GI bleeding decreased from 20,013 in 1998 to 16,344 in 2006.
Unspecified GI Bleeding: Among patients discharged from the hospital with unspecified GI bleeding (nearly 31%)—i.e., with neither an upper-GI nor a lower-GI bleeding diagnosis—about 130,000 had hemorrhage of the GI tract and 38,000 had melena.
To comment on this article, contact rdavidson@uspharmacist.com.





