US Pharm. 2021;46(3):31-35.
ABSTRACT: Ramsay Hunt syndrome (RHS) begins with an attack of herpes zoster (i.e., shingles) inside the ear canal. RHS primarily affects the facial nerve, but it can also affect cranial nerves that communicate with the facial nerve. Damage to cranial nerves causes otic pain, otic rash, hemifacial paralysis, and several other complications. Prompt administration of antiviral therapy can improve the prognosis, lessening the risk of permanent sequelae, such as facial distortion. Being aware of RHS enables the pharmacist to recognize its possible presence. The pharmacist can then explain the nature of the condition to the patient and stress the vital need for immediate physician care. The pharmacist can also assist the patient with relieving pain and other troublesome symptoms that often accompany RHS.
Ramsay Hunt syndrome (RHS), also known as herpes zoster (HZ) oticus, is a rare, self-limiting peripheral neuropathy that affects one ear and may cause additional symptoms on the same side of the face.1-7 Experts estimate that five cases per 100,000 U.S. residents occur each year.2 It is also believed that 20% of all cases of Bell’s palsy are due to RHS.3 Early recognition of this condition by a pharmacist can be critical in enabling the patient to obtain rapid treatment that will increase the chances of a full recovery.
Etiology and Epidemiology
RHS begins with an attack of HZ (i.e., shingles) inside the ear canal. The etiology of RHS is varicella zoster virus (VZV), the causal agent of chickenpox—a disease that the vast majority of adults had in childhood.4 VZV lies dormant in cranial-nerve (CN) neurons and dorsal root ganglia.1 Stress or natural or medically induced immunosuppression (e.g., azathioprine therapy) may cause the dormant virus to reactivate.5,8 The reactivation of VZV causes HZ.2,4,9-11 Although HZ attacks often occur on the torso, 35% of cases, including RHS, involve the dermatomes of the head and neck.10 Age is a strong risk factor for RHS, as most patients are older than age 60 years.4 Children seldom contract RHS.2
Symptoms and Complications
RHS has a complex symptomatology, and its complications range from minor and transient to profound and permanent. The range and severity vary from patient to patient.2 RHS primarily affects the facial nerve (CN VII), but it can also affect CNs that communicate with the facial nerve, such as III, V, VIII, IX, X, XI, and XII.8 The prognosis of RHS differs radically from that of idiopathic Bell’s palsy in that fewer than 50% of persons with RHS experience full recovery.3,12
Prodromal and Continual Otic Pain: An early sign of RHS is paroxysmal pain that appears to originate deep in the face or in one ear.1,3 The pain may radiate to the outer ear. Involvement of the outer ear causes a different type of pain that is described as a constant, dull, and diffuse ache.3 Severe otalgia may continue for the duration of the rash described below and may radiate to the jaw or neck.2
VZV Rash: Within a few hours of onset of otic pain, a VZV-induced rash develops. This rash is a set of erythematous vesicles or ulcerations inside the external ear canal, perhaps extending to the tympanic membrane and auricle (in which case it is called VZV auricularis).13 In rare cases, a patient experiences the constellation of RHS symptoms in the absence of the otic rash, a condition known as zoster sine herpete.1,2,4
Hearing Loss: As many as 50% of RHS patients experience sensorineural hearing loss in the affected ear.2-4 Although it may remit as the condition improves, some people suffer severe and permanent hearing loss in the affected ear, requiring artificial hearing augmentation. Otic involvement may include tinnitus or hyperacusis (heightened sensitivity to sound).4,14
Facial Weakness, Paralysis, and Asymmetry: RHS is the second most common cause of facial paralysis not caused by trauma.1 Hemifacial paralysis, or palsy, usually reaches a peak in 1 week.1 Complete hemifacial paralysis is twice as common as partial paralysis and occurs more frequently in patients older than age 50 years. The patient commonly experiences the initial symptoms in the early morning, first noticing a minor but alarming facial asymmetry manifested by a drooping of one side of the lip that distorts the smile.2,13 The face feels stiff and the muscles cannot fully respond. Normal facial landmarks on the affected side disappear, including the forehead frown wrinkles, nasolabial fold, and smile lines around the mouth. The patient rapidly loses the ability to speak clearly and may also experience facial numbness, tingling, and/or muscle twitching. In the most severe cases, the condition progresses to profound facial paralysis and resultant flaccidity.
Ophthalmic Involvement: When the eye is involved, the upper and lower eyelids on the affected side cannot be completely closed.2 Gravity causes the upper eyelid to droop over the eye, sometimes enough to cover the ophthalmic pupil, and the lower lid turns outward from the eye. The patient cannot blink, leading to further complications. Blinking is critical for lubricating the eye; with each blink, the upper lid carries tears upward to cover the eye’s surface. Blinking also allows tears to drain into the tear ducts. Because the upper lid cannot disperse the tears, excess lacrimal fluid accumulates in the pocket created by the sagging lower lid. This leads to an excess amount of collected tears, which run down the cheek. The loss of tears leads to xerophthalmia (abnormally dry eye), which is worsened by evaporation caused by the inability to close the eye. Chronic xerophthalmia causes corneal ulcers and infection.13
Oral Complications: Salivary glands are partially controlled by the seventh cranial nerve, and dysfunction of this nerve results in xerostomia (dry mouth) and contributes to intraoral food retention following a meal.14 The combination of xerostomia and retained food particles can cause plaque, calculus, caries, and gingivitis.15 Caries and untreated gingivitis can lead to periodontitis and tooth loss.16
Postherpetic Neuralgia (PHN): PHN is a painful condition that follows an attack of shingles; it can last for months or years.17-19 The cause of PHN is VZV-induced damage to the nerve fibers.4 PHN affects about 50% of persons older than age 60 years, and it may occur years after the patient had shingles.17 PHN that occurs after RHS, as discussed in the accompanying case study (SIDEBAR 1), can produce deep pain on the side where the RHS originally manifested. The pain may start slightly below the ear and radiate to the upper jaw, and the patient may feel that the associated jaw muscle is undergoing a spasm. The pain of PHN that occurs on the torso can be triggered by a cool breeze, but with RHS, other potential triggering cold exposures include instillation of refrigerated ophthalmic drops or application of cool shampoo to the head during a shower.17

Pharmacologic Therapies
Recommended pharmacologic therapy for RHS includes a combination of antiviral and corticosteroid medications. Prompt initiation within 72 hours of symptom onset has been associated with significant improvement versus delayed treatment, so rapid diagnosis and management are critical.1,2,20
Antivirals: Recommended antivirals include valacyclovir 1 g orally three times daily, famciclovir 500 mg orally three times daily, or acyclovir 800 mg orally five times daily for 7 to 10 days. In more serious cases or in immunocompromised patients, IV acyclovir therapy may be initiated at 10 mg/kg/dose every 8 hours and then be transitioned to oral therapy upon clinical improvement.1,21 Adverse effects (AEs) of valacyclovir include abdominal pain, nausea, headache, and nasopharyngitis. Headache and nausea are often associated with famciclovir use, whereas malaise is the most likely AE experienced with acyclovir.22
Corticosteroids: Prednisone 1 mg/kg for 5 days has been recommended in conjunction with antiviral therapy, with or without a tapering regimen.1,21 Although IV high-dose methylprednisolone is not typically used in the treatment of RHS, it may provide some clinical benefit in patients who do not respond to standard therapy.3,23 AEs of short-term corticosteroid use include elevations in blood pressure and blood glucose levels, fluid retention, changes in mood, nausea, and headache.22
Pain Management: Pain management for PHN may be necessary in some RHS patients. Topical treatment with capsaicin cream or patches may provide relief, but application-related AEs such as burning, stinging, and redness might limit use. Patches containing 5% lidocaine have also been approved for the treatment of PHN and have exhibited mixed results in clinical trials.22 In patients with moderate-to-severe PHN, gabapentin and pregabalin are considered first-line agents. Patients should be started on low doses and titrated to the desired effect.24,25 Fatigue, dizziness, and drowsiness are among the most common AEs of these medications, and dosing should be modified in patients with renal dysfunction.22 The use of tricyclic antidepressants (TCAs) such as amitriptyline may be considered in patients with PHN who are unable to tolerate the gabapentinoids or are not experiencing adequate relief with their use. Initial amitriptyline dosing is 10 mg orally each night, and the dosage may be titrated up to a maximum of 150 mg daily.24,25 Anticholinergic AEs such as sedation, dry mouth, and urinary retention are common. TCAs should be used with caution in elderly patients and in those with heart disease, seizure disorders, or glaucoma.22 Given the risk of abuse and addiction, opioids and tramadol are considered third-line agents for PHN and should be used only under the close supervision of a prescribing physician.24
Prevention via Vaccination
To reduce the risk of RHS, preventive vaccinations for VZV and HZ are recommended.
VZ Vaccine: The VZ vaccine, which is indicated for children aged 12 months and older, has a mean effectiveness of 92% in preventing varicella infection.26 It is given SC in two doses, with the first dose typically administered between ages 12 and 15 months and the second dose given between ages 4 and 6 years. In children aged 13 years and older and in adults who did not receive the vaccine in childhood and have no evidence of active varicella infection, the two doses should be separated by 4 to 8 weeks. Varicella immunization is particularly important for healthcare providers, contacts of immunocompromised patients, and others at high risk for exposure or transmission.27,28 This vaccine is well tolerated, with local injection-site reactions, fever, and rash being the most common AEs. Two VZ vaccines are currently approved in the U.S.: a single-antigen varicella vaccine and a combination vaccine for measles, mumps, rubella, and varicella.22
HZ Vaccine: Zostavax, a live attenuated virus, was the first shingles vaccine to be approved in the U.S., but it has been replaced by Shingrix, a recombinant glycoprotein E vaccine, which has superior efficacy.29,30 Shingrix decreases the risk of shingles and PHN development in patients aged 50 years and older and in those who previously received Zostavax. The vaccine is administered IM in two doses, with the second dose given 2 to 6 months after the first.29 Shingrix is not approved for prevention of VZ or for treatment of HZ infection. In patients with a history of HZ, vaccination should be delayed until the acute stage of illness has passed and symptoms resolve. Although Shingrix is generally well tolerated, AEs are relatively common and include injection-site pain, myalgias, fatigue, headache, shivering, and fever. These symptoms typically remit after 2 to 3 days.22,29
Nonprescription Products
RHS presents several opportunities for the pharmacist to assist patients in managing ophthalmic and oral complications.
Dry Eye: Dry eye associated with RHS requires more care than simple dry eye because the affected eye cannot be completely closed. The pharmacist can instruct the patient on proper self-care. TABLE 1 lists some products suitable for RHS-associated dry eye. Effective products for daytime use are drops or gels containing ingredients such as cellulose, polyvinyl alcohol, and glycerin. At bedtime, the patient should place a liberal amount of an ointment containing mineral oil and white petrolatum inside the lower eyelid; after application, the upper eyelid should be gently and completely pulled down to meet the lower eyelid and a strip of hypoallergenic paper tape should be applied to both lids to keep the eye closed during sleep.14 Two or three additional strips placed in an X pattern over the first strip will help secure the lids. If the eye is not taped shut, it will dry out despite the use of ointment.
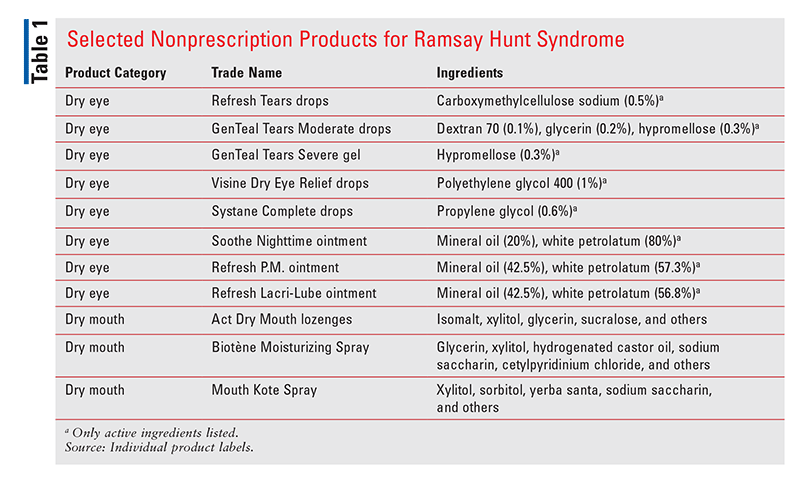
Dry Mouth: The pharmacist should advise the patient to alleviate dry mouth with liberal use of such products as Act Lozenges, Biotene, and Mouth Kote.31 More information on these products is provided in TABLE 1.
Conclusion
It is vital for the pharmacist to recognize possible RHS and urge an immediate physician visit. Treatment initiated within 3 days of symptom onset reduces the risk of long-term complications.4 The pharmacist can also stress to patients the importance of vaccination for chickenpox and shingles and provide assistance in the treatment of PHN, dry eye, and dry mouth.
REFERENCES
1. Sweeney CJ, Gilden DH. Ramsay Hunt syndrome. J Neurol Neurosurg Psychiatry. 2001;71(2):149-154.
2. National Organization for Rare Disorders. Ramsay Hunt syndrome. https://rarediseases.org/rare-diseases/ramsay-hunt-syndrome/. Accessed January 30, 2021.
3. Muengtaweepongsa S. Ramsay Hunt syndrome. https://emedicine.medscape.com/article/1166804-overview. Accessed January 30, 2021.
4. Mayo Clinic. Ramsay Hunt syndrome. www.mayoclinic.org/diseases-conditions/ramsay-hunt-syndrome/symptoms-causes/syc-20351783. Accessed January 30, 2021.
5. Facial Palsy UK. Ramsay Hunt syndrome. www.facialpalsy.org.uk/causesanddiagnoses/ramsay-hunt-syndrome/. Accessed January 30, 2021.
6. Kanerva M, Jones S, Pitkaranta A. Ramsay Hunt syndrome: characteristics and patient self-assessed long-term facial palsy outcome. Eur Arch Otorhinolaryngol. 2020;227(4):1235-1245.
7. Wagner G, Klinge H, Sachse MM. Ramsay Hunt syndrome. J Dtsch Dermatol Ges. 2012;10(4):238-244.
8. National Institute of Neurological Disorders and Stroke. Herpes zoster oticus information page. www.ninds.nih.gov/Disorders/All-Disorders/Herpes-Zoster-Oticus-Information-Page#disorders-r1. Accessed January 30, 2021.
9. Shaikh S, Ta CN. Evaluation and management of herpes zoster ophthalmicus. Am Fam Physician. 2002;66(9):1723-1730.
10. Jeon Y, Lee H. Ramsay Hunt syndrome. J Dent Anesth Pain Med. 2018;18(6):333-337.
11. Liesegang TJ. Herpes zoster ophthalmicus natural history, risk factors, clinical presentation, and morbidity. Ophthalmology. 2008;115(suppl 2):S3-S12.
12. Zainine R, Sellami M, Charfeddine A, et al. Ramsay Hunt syndrome. Eur Ann Otorhinolaryngol Head Neck Dis. 2012;129(1):22-25.
13. MedlinePlus. Ramsay Hunt syndrome. https://medlineplus.gov/ency/article/001647.htm. Accessed January 30, 2021.
14. Callen ED, Pray WS. Bell’s palsy and the pharmacist. US Pharm. 2019;44(1):26-30.
15. WebMD. Dental health and dry mouth. www.webmd.com/oral-health/guide/dental-health-dry-mouth#1. Accessed January 30, 2021.
16. Mayo Clinic. Gingivitis. www.mayoclinic.org/diseases-conditions/gingivitis/symptoms-causes/syc-20354453. Accessed January 30, 2021.
17. Area Agency on Aging 1-B. Postherpetic neuralgia: treating nerve pain after shingles. https://aaa1b.org/?s=postherpetic. Accessed January 30, 2021.
18. Watson PN. Postherpetic neuralgia. www.ncbi.nlm.nih.gov/pmc/articles/PMC3217735/. Accessed January 30, 2021.
19. MedlinePlus. Postherpetic neuralgia—aftercare. https://medlineplus.gov/ency/patientinstructions/000555.htm. Accessed January 30, 2021.
20. Murakami S, Hato N, Horiuchi J, et al. Treatment of Ramsay Hunt syndrome with acyclovir-prednisone: significance of early diagnosis and treatment. Ann Neurol. 1997;41(3):353-357.
21. Coulson S, Croxson GR, Adams R, Oey V. Prognostic factors in herpes zoster oticus (Ramsay Hunt syndrome). Otol Neurotol. 2011;32(6):1025-1030.
22. Acyclovir. Lexi-Drugs. Lexicomp. Riverwoods, IL: Wolters Kluwer Health, Inc. http://online.lexi.com. Accessed December 11, 2020.
23. Donati D, De Santi L, Ginanneschi F, et al. Successful response of non-recovering Ramsay Hunt syndrome to intravenous high dose methylprednisolone. J Neurol Sci. 2012;318(1-2):160-162.
24. Johnson RW, Rice AS. Clinical practice. Postherpetic neuralgia. N Engl J Med. 2014;371(16):1526-1533.
25. Finnerup NB, Attal N, Haroutounian S, et al. Pharmacotherapy for neuropathic pain in adults: a systematic review and meta-analysis. Lancet Neurol. 2015;14(2):162-173.
26. Marin M, Marti M, Kambhampati A, et al. Global varicella vaccine effectiveness: a meta-analysis. Pediatrics. 2016;137(3):e20153741.
27. Marin M, Güris D, Chaves SS, et al. Prevention of varicella: recommendations of the Advisory Committee on Immunization Practices (ACIP). MMWR Recomm Rep. 2007;56(RR-4):1-40.
\28. Freedman M, Kroger A, Hunter P, Ault KA. Recommended adult immunization schedule, United States, 2020. Ann Intern Med. 2020;172(5):337-347.
29. CDC. Shingles (herpes zoster). Vaccination. www.cdc.gov/shingles/vaccination.html. Accessed January 30, 2021.
30. Tricco AC, Zarin W, Cardoso R, et al. Efficacy, effectiveness, and safety of herpes zoster vaccines in adults aged 50 and older: systematic review and network meta-analysis. BMJ. 2018;363:k4029.
31. Salinas TJ. Dry mouth treatment: tips for controlling dry mouth. www.mayoclinic.org/diseases-conditions/dry-mouth/expert-answers/dry-mouth/faq-20058424. Accessed January 30, 2021.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





