US Pharm. 2015;40(10):HS5-HS11.
ABSTRACT: New molecular entities (NMEs), as defined by the FDA, are drug products containing as their active ingredient a chemical substance marketed for the first time in the United States. The following descriptions of NMEs approved in the past year (TABLE 1) detail the basic clinical and pharmacologic profiles for each new drug, as well as its pharmacokinetics, adverse reactions, drug interactions, and dosing data. Note that the information for each NME was obtained primarily from sources published prior to FDA approval; thus, it is essential that practitioners become aware of changes in a drug’s therapeutic profile as reported by their own patients and in the pharmaceutical literature, such as the emergence of additional adverse reactions and boxed warnings.

Edoxaban (Savaysa, Daiichi Sankyo)
Indication and Clinical Profile1,2: Edoxaban (Savaysa) is a new anticoagulant approved to reduce the risk of stroke and systemic embolic event (SEE) in patients with nonvalvular atrial fibrillation (NVAF). It is also approved to treat venous thromboembolism (VTE), including deep venous thrombosis (DVT) and pulmonary embolism (PE) in patients already treated with 5 to 10 days of a parenteral anticoagulant. Atrial fibrillation, one of the most prevalent arrhythmias, is characterized by asynchronous and improper contraction of the atria resulting in an abnormal, irregular, and rapid heartbeat. This allows blood to pool and clots to form in the atria, which can then break off and travel in the body, putting patients with atrial fibrillation at an increased risk of stroke and SEE. DVT is a clot that is formed typically in the thighs or lower legs and can become deadly if it breaks off and travels to pulmonary arteries, causing a PE.
FDA approval of edoxaban for stroke and SEE risk reduction in patients with NVAF was based on the results of the ENGAGE AF-TIMI 48 study. It was a randomized, double-blind, noninferiority study of edoxaban 30 mg and 60 mg compared to warfarin (international normalized ratio [INR] 2.0-3.0) involving 21,105 participants with NVAF. Results of the study demonstrated both regimens of edoxaban were noninferior to warfarin for the primary efficacy endpoint of first occurrence of stroke or SEE. However, the 30-mg (15-mg dose-reduced) treatment arm was numerically less effective than warfarin for the primary endpoint, and was also markedly inferior in reducing the rate of ischemic stroke. Edoxaban demonstrated significantly less major bleeding compared to warfarin.
Approval of edoxaban for VTE treatment was based on the Hokusai-VTE study. It was a randomized, multinational, double-blind, noninferiority study comparing edoxaban 60-mg orally once daily to warfarin (INR 2.0-3.0) in 8,292 patients with acute symptomatic VTE. Results of the study demonstrated edoxaban to be noninferior to warfarin for the primary efficacy endpoint of preventing symptomatic recurrent VTE, with 3.2% of those taking edoxaban experiencing a symptomatic recurrent VTE versus 3.5% of patients taking warfarin.
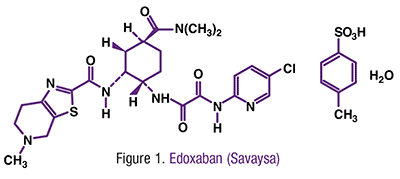
Pharmacology and Pharmacokinetics1,2: Edoxaban (FIGURE 1) indirectly decreases clot formation by reversibly inhibiting free and clot-bound clotting factor Xa (FXa) at the active site. Inhibition of FXa in the clotting cascade results in a decrease in the generation of the procoagulant thrombin, which in turn leads to an overall reduction in thrombus formation. Edoxaban is 62% bioavailable, reaches peak plasma concentration in 1 to 2 hours, is 55% plasma protein–bound, and has a half-life of 10 to 14 hours. It undergoes minimal metabolism via hydrolysis, conjugation, and oxidation by CYP3A4, and its predominant metabolite is active. The drug is 50% eliminated renally, and the remaining drug is cleared via metabolic and biliary/intestinal excretion pathways. Edoxaban does not alter the activity of any major CYP450 enzymes or transporter proteins.
Adverse Reactions and Drug Interactions1,2: The most common adverse reactions (ARs) reported by patients receiving edoxaban in clinical trials included bleeding and anemia, along with rash and liver function test abnormalities. Because edoxaban increases the risk of bleeding, including serious, potentially fatal bleeding, the drug is contraindicated in patients with active pathologic bleeding. All signs or symptoms of blood loss while on edoxaban should be promptly evaluated, as there is currently no reversal agent available. The label carries a boxed warning about the increased risk of stroke in NVAF patients who discontinue edoxaban prematurely without initiation of another anticoagulant. Edoxaban also carries a boxed warning for patients with creatinine clearance (CrCl) >95 mL/min, as these patients had an increased rate of ischemic stroke with edoxaban 60 mg once daily compared with patients treated with warfarin.
Concomitant use of drugs that inhibit the P-glycoprotein (Pgp) transporter (e.g., amiodarone, cyclosporine, erythromycin, ketoconazole, quinidine, verapamil) should be exercised with caution, as they may increase serum concentrations of edoxaban. Concomitant use of the Pgp inducer rifampin should also be avoided. Administration with drugs that interfere with hemostasis (e.g., nonsteroidal anti-inflammatory drugs, anticoagulants, thrombolytics, selective serotonin reuptake inhibitors, antiplatelet drugs) increases bleeding risk and should be avoided. Edoxaban carries a boxed warning against the use of the drug in patients receiving neuraxial anesthesia or undergoing spinal puncture, as this may result in epidural or spinal hematomas. There have not been adequate studies of the effects of edoxaban in pregnant women; thus, it should be avoided in pregnancy unless the potential benefit to the patient outweighs the potential risk to the fetus (Pregnancy Category C).
Dosage and Administration1,2: Edoxaban is supplied as 15-, 30-, and 60-mg tablets for oral administration, and the recommended starting dose for both approved indications is 60 mg once daily. Patients with CrCl between 15 and 50 mL/min should have their dose reduced to 30 mg once daily, along with patients being treated for DVT or PE who weigh 60 kg. Edoxaban should not be used in patients with CrCl <15 mL/min or on hemodialysis, and it is not recommended for patients with moderate-to-severe hepatic impairment (Child-Pugh B and C). There are no dose adjustments required for elderly patients or those with mild hepatic impairment. Specific recommendations regarding transitioning between edoxaban and other anticoagulants are given in the prescribing information. All patients taking edoxaban should be properly counseled about the increased risk of bleeding before starting the medication.
Ceftazidime-Avibactam (Avycaz, Forest Pharmaceuticals)
Indication and Clinical Profile3,4: The FDA has approved Avycaz, a fixed-combination product containing ceftazidime and avibactam, for IV treatment of complicated urinary tract infections (cUTIs) and complicated intra-abdominal infections (cIAIs) in patients aged ≥18 years who have limited or no other treatment options. cUTIs usually occur in patients with indwelling urinary catheters or anatomical or functional abnormalities of the urinary tract, and are often caused by antibiotic-resistant, gram-negative bacilli (including Escherichia coli, Klebsiella pneumoniae, Proteus mirabilis, Pseudomonas aeruginosa) or enterococci. In hospitalized patients, the recommended empirical therapies typically include a fluoroquinolone such as levofloxacin or ciprofloxacin, a third-generation cephalosporin (e.g., cefepime, ceftriaxone), piperacillin-tazobactam, or a carbapenem.
Most IAIs, such as cholangitis and diverticulitis, are polymicrobial and are caused by enteric gram-negative organisms (most commonly E coli ), but enterococci and anaerobes such as Bacteroides fragilis are also often involved. For community-acquired infections of mild-to-moderate severity, such as acute appendicitis, monotherapy with ertapenem or moxifloxacin is often employed. In severely ill patients and those with prolonged hospitalization, treatment should include an antipseudomonal penicillin (piperacillin-tazobactam) or a carbapenem (imipenem, meropenem, or doripenem) to provide coverage for P aeruginosa.
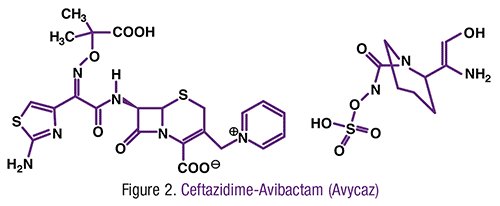
Ceftazidime is a previously approved third-generation cephalosporin antibacterial, and avibactam is a new beta-lactamase inhibitor (FIGURE 2). Ceftolozane-tazobactam (Zerbaxa), another cephalosporin and beta-lactamase inhibitor combination, was approved in 2014. Avycaz is the fifth approved antibacterial drug product designated as a Qualified Infectious Disease Product (QIDP), a designation given to antibacterial products to treat serious or life-threatening infections under the Generating Antibiotic Incentives Now (GAIN) title of the FDA Safety and Innovation Act. As part of its QIDP designation, Avycaz was given priority review, which also qualifies this drug for an additional 5 years of marketing exclusivity. Avycaz’s indication for cUTIs includes pyelonephritis caused by the gram-negative bacilli E coli, K pneumoniae, and P aeruginosa and Citrobacter, Enterobacter, and Proteus species. For treatment of cIAIs caused by the same gram-negative pathogens, ceftazidime-avibactam in combination with metronidazole is indicated.
The approval of Avycaz was based primarily on two randomized, active-controlled, phase II trials. In one study, 135 patients with cUTIs were treated with either ceftazidime-avibactam 500/125 mg every 8 hours or imipenem-cilastatin 500 mg every 6 hours. A favorable microbiologic response occurred in 19 of 27 (70.4%) microbiologically evaluable patients treated with the ceftazidime combination and in 25 of 35 (71.4%) patients treated with imipenem. In another trial, 203 adults with cIAI requiring surgical intervention were randomized to ceftazidime-avibactam 2,000/500 mg plus metronidazole 500 mg, or to meropenem 1,000 mg, both given every 8 hours for 5 to 14 days. The clinical response in microbiologically evaluable patients was favorable in 71 of 76 (93.4%) treated with ceftazidime-avibactam and in 62 of 68 (91.2%) treated with meropenem.
Pharmacology and Pharmacokinetics3,4: The ceftazidime component of Avycaz is a third-generation cephalosporin with activity against enteric gram-negative bacilli, but with minimal to no activity against anaerobic or gram-positive pathogens. The bactericidal action of ceftazidime results from its ability to inactivate essential penicillin-binding proteins (PBPs) of bacteria. The avibactam component of Avycaz is a non–beta-lactam/beta-lactamase inhibitor that inactivates Ambler class A and C, and some class D beta-lactamases, thereby protecting ceftazidime from beta-lactamase–mediated resistance. Thus, the addition of avibactam enhances ceftazidime’s activity against P aeruginosa and many extended-spectrum beta-lactamase (ESBL)–producing gram-negative pathogens seen in cUTIs and cIAIs. In addition, this is the first beta-lactam/beta-lactamase inhibitor combination to have activity against some carbapenem-resistant Enterobacteriaceae, including those that produce K pneumoniae carbapenemase (KPC), the most common carbapenemase in the United States. The combination is not active against organisms that produce metallo-beta-lactamase.
Both components in this product appear to have linear kinetics, and neither drug accumulates in healthy adults upon multiple dosing. The time above the minimum inhibitory concentration (MIC) best correlates with antibacterial efficacy. The drug products are <10% protein-bound, and the volumes of distribution are 17 and 22 L for ceftazidime and avibactam, respectively. Both components in this product are eliminated renally in unmetabolized form; thus, dose reduction is recommended in patients with moderate-to-severe renal impairment. Dosing in patients with hepatic impairment has not been established.
Adverse Reactions and Drug Interactions3,4: The most common adverse effects associated with Avycaz in clinical trials included vomiting, nausea, constipation, and anxiety. Patients should be informed of these risks and advised that decreased efficacy, seizures, and other neurologic events were seen in patients with renal impairment. Serious skin reactions and anaphylaxis may occur in patients with penicillin allergies and, as with other beta-lactam antibiotics, Clostridium difficile–associated diarrhea and serious hypersensitivity reactions can occur with ceftazidime-avibactam. Avibactam is a substrate of organic anion transporters (OAT1 and OAT3); thus, coadministration with a potent OAT inhibitor such as probenecid could decrease avibactam elimination and is not recommended. Ceftazidime-avibactam is classified as a Pregnancy Category B drug.
Dosage and Administration3,4: Avycaz is supplied as a solution for IV infusion. The recommended dosage is 2.5 g (2 g ceftazidime and 0.5 g avibactam) infused IV over 2 hours, every 8 hours. Dosage reductions are recommended for patients with renal impairment (CrCl <50 mL/min) per the manufacturer’s guidelines. For treatment of cIAI, addition of metronidazole is needed for anaerobic coverage. The recommended duration of treatment is 7 to 14 days for cUTIs and 5 to 14 days for cIAIs.
Atazanavir-Cobicistat (Evotaz, Bristol-Myers Squibb)
Indication and Clinical Profile5,6: The FDA has approved atazanavir-cobicistat (Evotaz) to be used in combination with other antiretrovirals (ARVs) to treat HIV-1 in adults. Atazanavir is a previously approved HIV-1 protease inhibitor, and cobicistat is a novel CYP3A4 inhibitor–boosting agent. Cobicistat also is a component of the four-drug, fixed-dose combination HIV treatment Stribild (elvitegravir-cobicistat-emtricitabine-tenofovir) and the two-drug combination Prezcobix (darunavir-cobicistat).
The safety and efficacy of atazanavir-cobicistat were evaluated in a randomized, double-blind, active-controlled trial (Study 114) involving 692 HIV-1 infected, treatment-naïve adults. In this study, participants were randomized in a 1:1 ratio to receive either atazanavir 300 mg/cobicistat 150 mg once daily or atazanavir 300 mg/ritonavir 100 mg once daily. All subjects received concomitant treatment with 300 mg of tenofovir and 200 mg of emtricitabine administered once daily as a single tablet. Trial participants had a baseline estimated CrCL >70 mL/min, a mean baseline plasma HIV-1 RNA of 4.8 log10 copies/mL, and a mean baseline CD4+ cell count of 352 cells/mm. At 48 weeks, 85% of patients in the atazanavir-cobicistat arm achieved HIV-1 RNA levels of <50 copies/mL compared to 87% of patients in the atazanavir-ritonavir arm. Six percent of patients in the atazanavir-cobicistat arm and 4% of those in the atazanavir-ritonavir arm experienced virologic failure (defined as HIV-1 RNA >50 copies/mL) at 48 weeks, making atazanavir-cobicistat the only protease inhibitor pharmacoenhanced with cobicistat with virologic failure rates as low as 6%. The safety profiles in the two arms of the study were comparable.
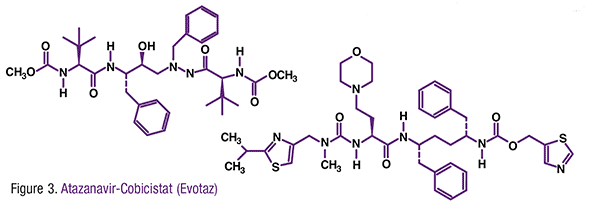
Pharmacology and Pharmacokinetics5,6: Evotaz is a fixed-dose combination of atazanavir and the CYP3A4 inhibitor cobicistat (FIGURE 3). Atazanavir is an azapeptide HIV-1 protease inhibitor that selectively inhibits the virus-specific processing of viral Gag and Gag-Pol polyproteins in HIV-1 infected cells, thus preventing formation of mature virions. Atazanavir exhibits anti–HIV-1 activity with a mean 50% effective concentration (EC50 value) 2-5 nM against a variety of laboratory and clinical HIV-1 isolates, but it is less effective versus HIV-2 isolates (EC50 1.9-35 nM). Atazanavir shows no antagonism with other drug classes used in the treatment of HIV infection. HIV-1 isolates with a decreased susceptibility to atazanavir have been selected in cell culture and obtained from patients treated with the drug alone or when coadministered with ritonavir.
Cobicistat is a mechanism-based inhibitor of CYP3A, an enzyme that metabolically inactivates atazanavir. Thus, coadministration of cobicistat with atazanavir increases the systemic exposure of atazanavir.
Adverse Reactions and Drug Interactions5,6: The most common ARs (all grades) in clinical trials and reported in >10% of subjects in the atazanavir coadministered with cobicistat group were jaundice (13%), ocular icterus (15%), and nausea (12%); the most common ARs in the atazanavir plus ritonavir group were jaundice (11%), ocular icterus (17%), nausea (11%), and diarrhea (11%). The proportion of subjects who discontinued study treatment due to adverse events, regardless of severity, was 7% in both groups. Atazanavir-cobicistat should be used in pregnancy only if the potential benefit justifies the potential risk (Pregnancy Category B). Nursing mothers should be instructed not to breastfeed due to the potential for postnatal HIV transmission. The atazanavir component of the drug also has warnings and precautions for rash, cardiac conduction abnormalities, nephrolithiasis, hepatotoxicity, hyperbilirubinemia, immune reconstitution syndrome, diabetes, fat redistribution, and hemophilia similar to those for other protease inhibitors.
Atazanavir is an inhibitor of CYP3A and UGT1A1 and a weak inhibitor of CYP2C8, while cobicistat is an inhibitor of CYP3A and CYP2D6 and the transporters Pgp, breast cancer–resistance protein (BCRP), OATP1B1, and OATP1B3. Thus, coadministration of atazanavir-cobicistat with drugs highly dependent on CYP3A for clearance and for which elevated plasma concentrations are associated with serious and/or life-threatening events is contraindicated. Coadministration of this drug product with CYP3A inducers may lead to lower exposure of atazanavir and cobicistat and loss of efficacy of atazanavir and possible resistance. The potential for drug interactions prior to and during atazanavir-cobicistat therapy should be considered; review concomitant medications and monitor patients for ARs.
This agent is not recommended in combination with other antiretroviral drugs that require CYP3A inhibition to achieve adequate exposures (e.g., other HIV protease inhibitors or elvitegravir) because dosing for such combinations has not been established and coadministration may lead to loss of therapeutic effect and development of resistance. In addition, this product is not recommended in combination with other drugs containing the individual components (atazanavir or cobicistat) or in combination with ritonavir-containing products. Finally, atazanavir solubility decreases as pH increases; therefore, reduced plasma concentrations of atazanavir are expected if proton pump inhibitors, antacids, buffered medications, or histamine2-receptor antagonists (H2RAs) are administered with atazanavir-cobicistat.
Dosage and Administration5,6: Evotaz is supplied as a tablet containing 300 mg of atazanavir and 150 mg of cobicistat. The recommended dosage in adults is one tablet once daily with food. When coadministered with H2RAs or proton pump inhibitors, dose separation may be required.
Palbociclib (Ibrance, Pfizer)
Indication and Clinical Profile7,8: Palbociclib (Ibrance) has been approved for use, in combination with letrozole, for the treatment of estrogen receptor (ER)-positive, human epidermal growth factor receptor 2 (HER2)-negative metastatic breast cancer in postmenopausal women who have not yet received an endocrine-based therapy. Breast cancer is the second most common cancer in the U.S., with 232,670 American women diagnosed with breast cancer and 40,000 deaths from the disease in 2014. The FDA granted palbociclib breakthrough-therapy designation and a priority review, as it could offer a substantial improvement over available therapies. It was also approved under the accelerated-approval program, as it was likely to provide clinical benefit to patients with a life-threatening disease.
FDA approval of palbociclib was based on results of the PALOMA-1 trial. It was a phase II, randomized, open-label, multicenter study of palbociclib plus letrozole versus letrozole alone conducted in 165 postmenopausal women with ER-positive, HER2-negative advanced breast cancer who had not received previous systemic treatment for their advanced disease. Palbociclib was given orally at a dose of 125 mg daily for 21 consecutive days followed by 7 days off treatment. Subjects received study treatment until progressive disease, unmanageable toxicity, or consent withdrawal. The primary efficacy outcome was progression-free survival (PFS) evaluated according to Response Evaluation Criteria in Solid Tumors Version 1.0 (RECIST 1.0). Patients who received palbociclib plus letrozole experienced an increase in median PFS versus those treated with letrozole alone (20.2 months vs. 10.2 months). Palbociclib plus letrozole also demonstrated improvements of overall response rate versus letrozole alone (55.4% vs. 39.4%). Overall survival data from the study are currently not available.
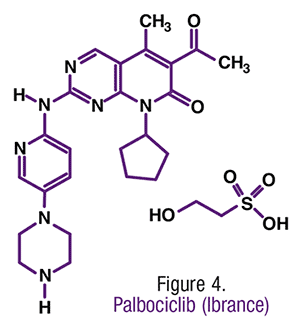
Pharmacology and Pharmacokinetics7,8: Palbociclib is a pyridopyrimidine derivative (FIGURE 4) that functions as a reversible inhibitor of cyclin-dependent kinase (CDK) 4 and 6. CDKs help regulate cell cycle progression at the G1/S phase by blocking retinoblastoma (Rb) hyper-phosphorylation. By inhibiting CDKs, palbociclib inhibits Rb phosphorylation, which in turn reduces proliferation of breast cancer cell lines by preventing progression from the G1 to the S cell cycle phase. These actions are bolstered by addition of letrozole, which provides for increased inhibition of Rb phosphorylation, downstream signaling, and tumor growth compared with the effects of each agent alone.
The absolute bioavailability of palbociclib is 46%, and its absorption is increased with high-fat, high-calorie food. Peak plasma concentrations of palbociclib are reached between 6 and 12 hours, and the drug is ~85% bound to plasma proteins. It undergoes extensive hepatic metabolism primarily by CYP3A4 oxidation and sulfotransferase 2A1 enzyme sulfonation, along with some minor acylation and glucuronidation. Palbociclib has a half-life of 24 to 36 hours and is excreted primarily as metabolites in feces (74%) and urine (18%).
Adverse Reactions and Drug Interactions7,8: The most common ARs reported by patients receiving palbociclib in clinical trials included bone marrow suppression (neutropenia, leukopenia, thrombocytopenia, anemia), upper respiratory infection, fatigue, asthenia, alopecia, gastrointestinal (GI) toxicity (stomatitis, nausea, diarrhea, vomiting, decreased appetite), peripheral neuropathy, and epistaxis. Providers should monitor patients’ CBC before initiating therapy and at the beginning of each cycle, as well as on day 14 of the first two cycles and as clinically indicated. Doses of palbociclib may have to be adjusted based on CBC. PE also occurred more frequently in patients receiving palbociclib, and patients should be monitored for signs and symptoms of PE such as shortness of breath, chest pain, tachypnea, and tachycardia. Women of reproductive potential taking palbociclib should use effective contraception during treatment and for at least 2 weeks after the last dose, as adverse events were observed in animal reproduction studies.
Due to its metabolism by CYP3A4, coadministration of palbociclib with drugs that are strong CYP3A inhibitors (e.g., azole antifungals, clarithromycin, indinavir, nefazodone, protease inhibitors, telaprevir, telithromycin, verapamil) may require dose reduction (75 mg once daily). In addition, drugs that are moderate-to-strong CYP3A inducers (e.g., bosentan, efavirenz, etravirine, modafinil, nafcillin, rifampin) and grapefruit juice should be avoided. Furthermore, palbociclib may affect the metabolism of other medications metabolized by CYP3A4; therefore, CYP3A drug substrates with a narrow therapeutic index (e.g., alfentanil, cyclosporine, ergotamines, everolimus, fentanyl, pimozide, quinidine, sirolimus, tacrolimus) may require dose reduction.
Dosage and Administration7,8: Palbociclib is supplied as 75-, 100-, and 125-mg capsules for oral administration, and the recommended dose is 125 mg once daily for 21 days, followed by a 7-day rest period. It should be taken with food in combination with letrozole 2.5 mg once daily given continuously throughout the 28-day cycle. There are no dose adjustments required for elderly patients or those with mild-to-moderate renal impairment or mild hepatic impairment. Palbociclib has not been studied in pediatric patients or patients with moderate-to-severe hepatic impairment or severe renal impairment (CrCl <30 mL/min). Patients may require treatment interruption, dose reduction, or discontinuation for some ARs. For an initial reduction, the recommended dose is 100 mg daily and then 75 mg daily if further reduction is warranted. Patients who experience ARs while taking 75 mg of palbociclib daily should discontinue treatment. All patients should administer palbociclib with food at approximately the same time each day.
REFERENCES
1. Savaysa (edoxaban) package insert. Parsippany, NJ: Daiichi Sankyo, Inc; January 2015.
2. Giugliano RP, Ruff CT, Braunwald E, et al; ENGAGE AF-TIMI 48 Investigators. Edoxaban versus warfarin in patients with atrial fibrillation. N Engl J Med. 2013;369(22):2093-2104.
3. Avycaz (ceftazidime-avibactam) package insert. Cincinnati, OH: Forest Pharmaceuticals, Inc; February 2015.
4. Vazquez JA, González Patzán LD, Stricklin D, et al. Efficacy and safety of ceftazidime-avibactam versus imipenem-cilastatin in the treatment of complicated urinary tract infections, including acute pyelonephritis, in hospitalized adults: results of a prospective, investigator-blinded, randomized study. Curr Med Res Opin. 2012;28(12):1921-1931.
5. Evotaz (atazanavir-cobicistat) package insert. Princeton, NJ: Bristol-Myers Squibb Company; June 2015.
6. Elion R, Cohen C, Gathe J, et al. Phase 2 study of cobicistat versus ritonavir each with atazanavir plus fixed-dose emtricitabine/tenofovir DF in the initial treatment of HIV infection. AIDS. 2011;25(15):1881-1886.
7. Ibrance (palbociclib) package insert. New York, NY: Pfizer Inc; February 2015.
8. Rocca A, Farolfi A, Bravaccini S, et al. Palbociclib (PD 0332991): targeting the cell cycle machinery in breast cancer. Expert Opin Pharmacother. 2014;15(3): 407-420.
To comment on this article, contact rdavidson@uspharmacist.com.






