U.S. Pharm. 2018:4(43)16-18.
Osteomyelitis, the inflammation of bone secondary to infection, is a common infectious disease among older patients.1 This condition may be localized or generalized, and antibiotics and bone debridement are indicated in most patients. Inadequate treatment results in progression to a chronic form of infection.2 Osteomyelitis may be termed chronic if it endures more than 6 weeks, recurs, or is not cured after the initial infection.1 The possibility of chronicity increases with a delay in diagnosis and treatment.2
Risk With Prosthetic Joint Replacement
Older adults may develop osteomyelitis subsequent to total knee or total hip replacement. Prosthetic joints are at risk of acute and chronic infection; infections are notably more common in prosthetic joints than in natural joints.3 Additionally, prosthetic joint infections (PJIs) can cause sepsis, morbidity—they are particularly difficult to cure—and mortality.3,4 Of particular interest to pharmacists who monitor older adults, patients often have a history of a recent fall.3
While osteomyelitis may be caused by a variety of microorganisms, in the elderly population it is most often caused by pyogenic organisms.1 Within 1 year of surgery, PJIs develop in two-thirds of cases; data indicate Staphylococcus aureus as the causative organism in 50% of cases during the first few months after surgery (TABLE 1).3 Not surprisingly, rheumatoid arthritis patients (i.e., immunocompromised hosts) are predisposed to a higher incidence of prosthetic joint–related infections as compared with patients who have osteoarthritis.5-7
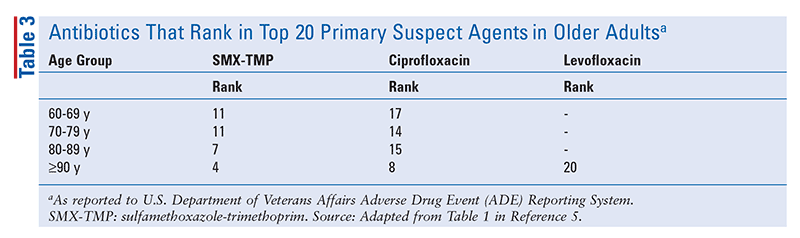
In general, trauma, ischemia, and foreign bodies predispose patients to osteomyelitis. Older age is a risk factor (TABLE 2) because people in this group are predisposed to osteomyelitis either because of an increased incidence of associated, predisposing disorders (e.g., peripheral vascular disease, diabetes mellitus, poor dentition) or surgical interventions that are frequently performed in the older adult population (e.g., dental extractions, open-heart surgery, prosthetic joint replacement).1,8 Frequent causes of PJI are perioperative inoculations of bacteria into the joint and postoperative bacteremia resulting from a variety of causes—including dental procedures and, possibly, falls—that are common in the elderly (TABLE 3). Of note, osteomyelitis also may form under deep pressure ulcers.8
From an etiological standpoint, the infection of bone occurs subsequent to 1) dissemination of bacteria via the bloodstream; 2) invasion from an infection in contact or close proximity (i.e., contiguous spread, as seen in PJI); and 3) breakdown of skin in conjunction with vascular insufficiency (TABLE 2).2 Symptoms of PJI include joint pain, swelling, and limited motion; temperature may be normal.3 In approximately 25% of patients, there is a history of a fall within 2 weeks of the onset of symptoms; prior surgical revisions have been noted in about 20% of patients.3
Diagnosis and Treatment of PJI
Diagnosis of PJI frequently necessitates considering a combination of criteria, including3:
• Clinical: Communication between a sinus tract and the prosthesis (possibly diagnostic of infection; see Prevention, below)
• Microbiologic: Synovial fluid should be sampled for cell count and culture
• Pathologic: Periprosthetic tissue collected at the time of surgery for culture and histologic analysis, and
• Imaging: X-rays (e.g., regarding loosening of the prosthesis, although not diagnostic), Technetium-99m bone scanning, indium-labeled WBC scanning
The clinical setting and the treatment approaches available ultimately determine the selection of antibiotic therapy and the duration of the antibiotic regimen in the management of bone and joint infections.9 Treatment of PJI consists of prolonged antibiotic therapy and, usually, arthrotomy (i.e., for prosthesis removal and cement/tissue debridement).3 A prosthesis is revised or a spacer (antibiotic-impregnated) is set in place for future prosthesis implantation (infection develops in 38% of replacement prostheses). Long-term systemic antibiotic therapy—required for either option—is empiric following an intraoperative culture, with combination coverage for3:
• Methicillin-resistant gram-positive organisms (e.g., vancomycin 1 g IV q12h) and
• Aerobic gram-negative organisms (e.g., piperacillin/tazobactam 3.375 g IV q6h or ceftazidime 2 g IV q8h)
Based on renal function and the results of culture and sensitivity tests, the above empiric therapy is revised; long-term antibiotic therapy may be tried alone if a patient cannot tolerate surgery.3 Oral quinolone therapy (e.g., ciprofloxacin 750 mg twice daily for 6-8 weeks) may be effective for chronic osteomyelitis with susceptible organisms; when caused by S aureus, quinolones are usually combined with rifampin (i.e., 300 mg orally twice daily).2 Careful dosage adjustment and monitoring in the elderly is recommended.
Prevention
At many medical centers, nasal cultures are used to screen patients for S aureus colonization; intranasal mupirocin ointment is then used prior to prosthetic joint implantation surgery (i.e., surgical prophylaxis) to decolonize carriers and prevent wound infections.3,10 Decolonization with this agent should be restricted to methicillin-resistant S aureus outbreaks and recurrent infections.10,11 For prevention of orthopedic-implant infection in patients undergoing dental procedures, refer to the Resource sidebar.
Conclusion
Infections of the bone and joints, particularly those associated with prosthetic implants, are difficult to cure. Bone and joint infections are caused most commonly by staphylococci. Long-term antibiotic therapy is required and is combined with surgery and the removal of prostheses. Early recognition, diagnosis, and treatment may potentially decrease the chronicity of the outcome.
REFERENCES
1. Yoshikawa TT, Cunha BA. Osteomyelitis in elderly patients. Clin Infect Dis. 2002;35(3):287-293.
2. Hellman DB, Imboden JB. Rheumatologic, immunologic, & allergic disorders. In: Papadakis MA, McPhee SJ, Rabow MW, eds. Current Medical Diagnosis & Treatment. 56th ed. New York, NY: McGraw Hill Education; 2017:870-871.
3. Schmitt S. Prosthetic joint infectious arthritis. Merckmanuals.com. Last full review/revision May 2017. www.merckmanuals.com/professional/musculoskeletal-and-connective-tissue-disorders/infections-of-joints-and-bones/prosthetic-joint-infectious-arthritis. Accessed March 1, 2018.
4. Kim B, Kim ES, Oh M. Oral antibiotic treatment of staphylococcal bone and joint infections in adults. J Antimicrob Chemother. 2014;69(2):309-322.
5. Saccente M. Periprosthetic joint infections: a review for clinicians. Infect Dis Clin Pract. 1998;7:431-441.
6. Kegel-Szerejko M, Maderazo EB, Cunha BA, et al. Host factors and prosthetic joint infections. Am J Infect Control. 1981;9:39-43.
7. Cunha BA. Diagnosis of infected joint replacements. Infect Dis Pract. 2000;3:24-65.
8. Schmitt S. Osteomyelitis. merckmanuals.com. Last full review/revision May 2017. www.merckmanuals.com/professional/musculoskeletal-and-connective-tissue-disorders/infections-of-joints-and-bones/osteomyelitis. Accessed February 25, 2018.
9. Trampuz A, Zimmerli W. Antimicrobial agents in orthopaedic surgery: prophylaxis and treatment. Drugs. 2006;6:1089-1105.
10. Epocrates.com. Epocrates Plus Version 15.12.1. Updated March 1, 2018.
11. Reuben DB, Herr KA, Pacala JT, et al. Geriatrics at Your Fingertips: 2016. 18th ed. New York, NY: The American Geriatrics Society; 2016:163.
To comment on this article, contact rdavidson@uspharmacist.com.