US Pharm. 2023;48(1):14.
Epilepsy is one of the most common neurologic diseases worldwide. Caused by abnormal neuronal activity within the brain, it is usually characterized by seizures (episodes of involuntary body movements). The U.S. National Institute of Neurological Disorders and Strokes estimates that 20% of persons with epilepsy experience nonepileptic seizures, while 30% and 60% experience generalized and focal seizures, respectively. In addition to movement disturbances, epilepsy may involve a loss of awareness or consciousness.
Prevalence and Incidence: According to the CDC, more than 3.4 million people in the U.S. currently have epilepsy. Approximately 150,000 Americans are diagnosed annually, with one in 26 people diagnosed over a lifetime. Epilepsy occurs more frequently in Hispanic persons than in non-Hispanic persons. Black persons have a higher lifetime incidence than white persons, whereas active epilepsy is more common in white persons.
Risk Factors and Management: Although the exact etiologies of epilepsy are unknown, genetic, infectious, metabolic, and immune causes have been linked to the underlying mechanisms. Examples include prenatal/perinatal brain damage, genetic predispositions associated with brain malformations, severe head injury, stroke, meningitis, encephalitis, neurocysticercosis, and brain tumors. Studies have also determined that adults aged 40 to 59 years, adults who are unmarried/not living with a partner, and adults with sleep disorders are at significantly higher risk for developing epilepsy. The World Health Organization estimates that nearly 70% of persons with epilepsy could live seizure-free with prompt diagnosis and treatment. Diagnosis, consisting of a documented cause of epilepsy and an abnormal electroencephalography pattern, is key to predicting seizure recurrence and selecting appropriate pharmacotherapy. Reevaluation of the need for continued pharmacotherapy may be performed after 2 years of no seizure occurrences. In persons with medically refractory epilepsy, surgical interventions may be considered.
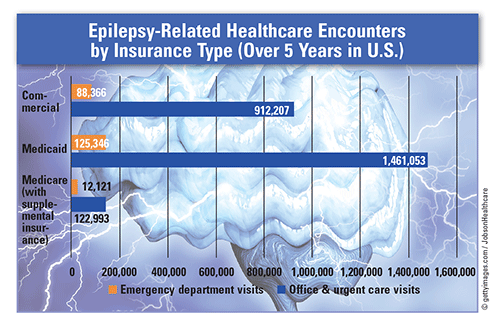
Consequences and Disparities: Epilepsy can lead to changes in vision, hearing, taste, or mood, as well as increases in anxiety, depression, and other psychiatric conditions. Studies have found that 20% of children with epilepsy have some type of intellectual disability, and up to 50% have a specific learning disability. In addition, children without commercial insurance receive fewer surgical interventions for medically refractory epilepsy. Data over a 5-year period show that adults and children aged 12 years and older with Medicaid insurance have more healthcare encounters related to their epilepsy than those with commercial insurance. Epilepsy may also lead to sudden unexplained death, which is reported to be three times more common in regions with lower socioeconomic status (SES) than in regions with higher SES across the U.S. An estimated 80% of persons with epilepsy live in these low- and middle-income areas or rural areas where healthcare access and treatment availability may be barriers to proper management.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





