US Pharm. 2018;12(43):8-10.
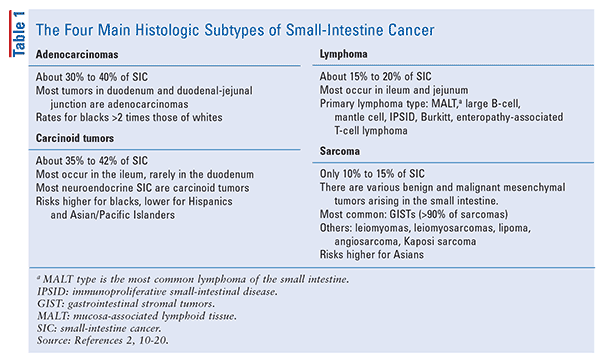
The small intestine accounts for 75% of the length of the alimentary tract.1 Cancer of the small intestine, however, is uncommon, accounting for only 3% to 6% of gastrointestinal tumors.1 Four main histologic subtypes (TABLE 1) exist: adenocarcinomas, carcinoid tumors, lymphomas, and sarcomas.2 Over the past several decades, the incidence of small-intestine cancer has increased, with a fourfold increase in carcinoid tumors, a less dramatic rise in adenocarcinoma and lymphoma, and stable rates of sarcoma.2 The prognosis for these carcinomas is poor (5-year relative survival <30%); the prognosis is better for lymphomas and sarcomas, and best for carcinoid tumors.2
While little is known about their etiology, it has been observed that cancers of the small intestine are more common in individuals with a number of inflammatory bowel diseases (IBDs) and other conditions (TABLE 2).2
It is currently accepted that a number of bacterial factors interact with the immune system in order for inflammation to occur, and there has been a recent shift in thinking toward the concept of dysbiosis (microbiota disequilibrium); therefore, the role of microbiota in IBD will be discussed to raise awareness about microbiota therapies and to underscore the importance of antibiotic stewardship in the prevention of antibiotic-induced microbiome dysbiosis.3,4
Pharmacists should note that with regard to decreasing the incidence and mortality rates of cancer of the small intestine, obesity and cigarette smoking may be the only established modifiable risk factors that provide a basis for prevention recommendations.2 Interestingly, some alterations of the intestinal microbiome secondary to smoking resemble those demonstrated in conditions such as IBD and obesity; Savin and colleagues indicated that further studies should be performed to investigate this connection. Smoking has an effect on the intestinal microbiome, and it has been suggested that smoking may modify its composition.5 The development of intestinal and systemic diseases, particularly IBDs, may be due in part to this interaction.5
Inflammatory Bowel Disease
IBD is a result of chronic inflammation caused, in some part, by dysbiosis of intestinal microbiota; this mainly occurs with commensal bacteria—those that derive benefit without harming or benefiting the host.6 It has been suggested that dysbiosis is the result of gut microbiota interacting with genetic contributions (risk loci), which subsequently leads to the development of IBD.6 In addition to the possibility of dysbiosis, bacterial factors are now thought to interact with the immune system in order for inflammation to occur.3 TABLE 3 lists factors that can cause dysbiosis, including abnormal immune responses and the administration of antibiotics. Notably, IBD is known to have multiple etiologies and severities.
Treatment of IBD usually includes medications such as corticosteroids, 5-aminosalicylates, antibiotics, immunomodulators, and anti–tumor necrosis factor agents; however, it appears that a safer and more sustainable approach is the restoration of microbiota disequilibrium (gut dysbiosis).6 Microbiota therapies (bacteriotherapies) and dietary interventions are effective ways to modulate gut microbiota.3 Holleran and colleagues discuss the main therapeutic modalities for treating IBD by affecting gut microbiota: probiotics, prebiotics, fecal microbiota transplantation, and emerging dietary intervention.3 Eom and colleagues discuss the potential use of microbiota therapies as one approach with promise in the treatment of IBD and underscore that future research should study individual gut microbiota differences to develop personalized therapy for IBD.6
Aging, Gut Microbiota, and Antibiotic Stewardship
With regard to the gut microbiota, there is a decline in diversity of microbes with age; additionally, immunity and metabolism decline over time, increasing an older adult’s susceptibility to infections.7 An increase in opportunistic-pathogen invasion in the gut, such as Clostridium difficile, leading to C difficile infection, is more common in older adults.7 Vemuri and colleagues discuss a variety of therapeutic interventions for gut dysbiosis and gastrointestinal disorders in older adults.7 In order to control infections, long-term use of broad-spectrum antibiotic therapy (ABT) is being monitored; treatment of nosocomial infections and mono- or combination-ABT has been shown to lead to gastroenteritis followed by Clostridium-associated diarrhea or antibiotic-associated diarrhea.7 The use of broad-spectrum antibiotics is currently debated because of growing antimicrobial resistance; use of narrow-spectrum antibiotics may be helpful to some extent.7
Fecal microbiota transplantation (FMT) is increasingly used to treat recurrent and refractory Clostridium-associated diarrhea.8,9 The premise of FMT is to reintroduce a healthy diversity of bacteria into the colon to reestablish colonization resistance and prevent C difficile from becoming a dominant organism in the patient’s gut microbiota.
Conclusion
Cancers of the small intestine are more common in individuals with a number of IBDs and other conditions. Over the past decade, there have been major advances in the understanding of the pathogenesis of IBD. It is now accepted that the microbiome is a significant, multifaceted key player in the development of inflammation. Older adults experience changes in their gut microbiota with advancing age, increasing their susceptibility to infection when combined with waning immunity. The role of the pharmacist in antibiotic stewardship regarding the use of broad spectrum ABT is supported, particularly in light of evidence for a role for microbiota therapies and dietary interventions as effective ways to modulate gut microbiota. These therapies hold promise in the treatment of IBD and the future development of personalized therapy for IBD.
REFERENCES
1. Crawford JM. The gastrointestinal tract. In: Cotran RS, Kumar V, Collins T, eds. Robbins Pathologic Basis of Disease. 6th ed. Philadelphia, PA: W.B. Saunders Company; 1999:826-828.
2. Pan SY, Morrison H. Epidemiology of cancer of the small intestine. World J Gastrointest Oncol. 2011;3(3):33-42.
3. Holleran G, Lopetuso LR, Ianiro G, et al. Gut microbiota and inflammatory bowel disease: so far so gut! Minerva Gastroenterol Dietol. 2017;63(4):373-384.
4. Kho ZY, Lai SK. The human gut microbiome—a potential controller of wellness and disease. Front Microbiol. 2018;9:1835.
5. Savin Z, Kivity S, Yonath H, et al. Smoking and the intestinal microbiome. Arch Microbiol. 2018;200(5):677-684.
6. Eom T, Kim YS, Choi CH, Yehuda S. Current understanding of microbiota- and dietary-therapies for treating inflammatory bowel disease. J Microbiol. 2018;56(3):189-198.
7. Vemuri RC, Gundamaraju R, Shinde T, Eri R. Therapeutic interventions for gut dysbiosis and related disorders in the elderly: antibiotics, probiotics or faecal microbiota transplantation? Benef Microbes. 2017;8(2):179-192.
8. Zagaria MA. Fecal transplantation for recurrent Clostridium difficile infection. US Pharm. 2014;39(12):20-22.
9. Orenstein R, Griesbach CL, DiBaise JK. Moving fecal microbiota transplantation into the mainstream. Nutr Clin Pract. 2013; 28(5):589-598.
10. Hamilton SR, Aaltonen LA. World Health Organization Classification of Tumours. Pathology and Genetics of Tumours of the Digestive System. Lyon, France: IARC Press; 2000:69-92.
11. Schottenfeld D, Beebe-Dimmer JL, Vigneau FD. The epidemiology and pathogenesis of neoplasia in the small intestine. Ann Epidemiol. 2009;19:58-69.
12. Bilimoria KY, Bentrem DJ, Wayne JD, et al. Small bowel cancer in the United States: changes in epidemiology, treatment, and survival over the last 20 years. Ann Surg. 2009;249:63-71.
13. Haselkorn T, Whittemore AS, Lilienfeld DE. Incidence of small bowel cancer in the United States and worldwide: geographic, temporal, and racial differences. Cancer Causes Control. 2005;16:781-787.
14. Qubaiah O, Devesa SS, Platz CE, et al. Small intestinal cancer: a population-based study of incidence and survival patterns in the United States, 1992 to 2006. Cancer Epidemiol Biomarkers Prev. 2010;19:1908-1918.
15. Howe JR, Karnell LH, Scott-Conner C. Small bowel sarcoma: analysis of survival from the National Cancer Data Base. Ann Surg Oncol. 2001;8:496-508.
16. Katz SC, DeMatteo RP. Gastrointestinal stromal tumors and leiomyosarcomas. J Surg Oncol. 2008;97:350-359.
17. Miettinen M, Kopczynski J, Makhlouf HR, et al. Gastrointestinal stromal tumors, intramural leiomyomas, and leiomyosarcomas in the duodenum: a clinicopathologic, immunohistochemical, and molecular genetic study of 167 cases. Am J Surg Pathol. 2003;27:625-641.
18. Vij M, Agrawal V, Kumar A, Pandy R. Gastrointestinal stromal tumors: a clinicopathological and immunohistochemical study of 121 cases. Indian J Gastroenterol. 2010;29:231-236.
19. Gustafsson BI, Siddique L, Chan A, et al. Uncommon cancers of the small intestine, appendix and colon: an analysis of SEER 1973-2004, and current diagnosis and therapy. Int J Oncol. 2008;33:1121-1131.
20. Zagaria MA. Treatment nuances for Kaposi sarcoma in older adults. US Pharm. 2018;43(8):8-11.
21. Davis LE, Sun W, Medina PJ. Colorectal cancer. In: DiPiro JT, Talbert RL, Yee GC, et al. Pharmacotherapy: A Pathophysiologic Approach. 9th ed. New York, NY: McGraw-Hill Education; 2017:2162-2163, 2166-2167.
To comment on this article, contact rdavidson@uspharmacist.com.