US Pharm. 2022;47(8):26-30.
ABSTRACT: The COVID-19 pandemic has unveiled the significant impact of social determinants of health on health outcomes, including mental health outcomes. Social determinants of health are the conditions in which we live, work, and play, but they are a leading cause of health disparities, particularly in marginalized communities. This article will discuss the implications of COVID-19 on the mental health of marginalized groups and the role that pharmacists can engage in, providing critical resources to aid individuals of marginalized communities in meeting their physical and mental health needs.
Uncertainty, loneliness, and job burnout from the COVID-19 pandemic contribute to the prevalence of mental disorders in Americans.1 A CDC report comparing mental health from June 2019 to June 2020 found a significant increase in mental illnesses, with 40% of adults experiencing symptoms of anxiety and/or depressive disorder.2 Such mental illnesses are disproportionately pronounced in marginalized communities, and long-standing inequities compound stress on socioeconomic minorities.3 Vulnerable groups—including racial and ethnic minorities, essential workers, low-income households, and underserved neighborhoods—are more likely to experience suboptimal patient outcomes and mental health harms associated with the COVID-19 pandemic.4
Social determinants of health (SDOH) are the different nonmedical factors that contribute to health outcomes (see FIGURE 1).4,5 Characteristics such as race, income, geographic location, education, and housing stability help determine well-being. Social and environmental contexts are key to accessing high-quality healthcare.5,6 Political and economic agendas that underlie conditions of daily life, and thus SDOH, are structurally rooted in lack of opportunity and inequitable access to resources.5,7 Many of the SDOH encountered by marginalized groups are intricately linked and coexisting: poverty, limited access to healthcare, racism, and education.5,8
The result of the health barriers caused by social determinants are health disparities.5 Health disparities refer to the preventable differences that disadvantaged groups face in attaining optimal health outcomes.7 The SDOH across demographic, economic, neighborhood, and sociocultural characteristics cause significant variations in mortality, life expectancy, and mental illness between populations.8 In order to address the impact of the COVID-19 pandemic on the mental health of vulnerable populations and how unfavorable characteristics of SDOH are a leading cause of health disparities, we must first understand how structural racism is the root cause of SDOH (see FIGURE 1).
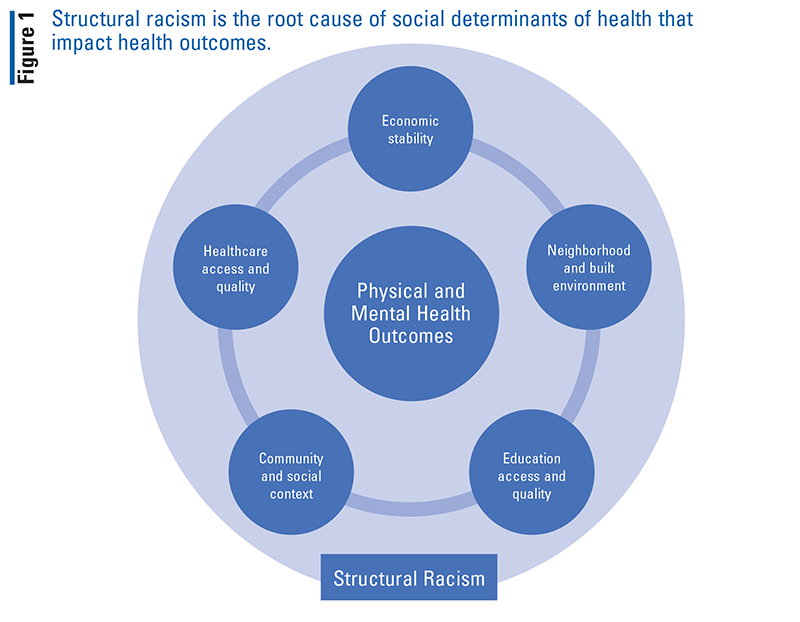
Structural Racism
Structural racism emphasizes the history of oppression in America and the many institutions that work against racial and ethnic minorities. Structural racism is the root cause of the health disparities and inequities that have shaped the circumstances and contexts of people’s lives. Generations of structural racism affect financial, housing, and food security, with major consequences of health inequities, poverty, and discrimination.8 Among African American adults, health inequities during the pandemic have led to higher rates of substance-use disorders and a 20% increase in mental health issues.3,8-10 Increased exposure with limited access to testing and treatment produce a fatal combination10,11; death rates of Pacific Islanders, Latino, Indigenous, and black groups are at least double that of their white and Asian American counterparts.10-12 With racism linked to multiple other SDOH, the repercussions of health barriers are especially burdensome on the mental health of racial and ethnic minorities during the COVID-19 pandemic.
Impact of SDOH on Mental Health Outcomes
Economic Stability
As the single largest determinant of health and one of the many indicators of socioeconomic status, poverty is characterized by a financial inability to meet basic needs.13 Unemployment during the COVID-19 pandemic aggravated financial stresses; by the end of 2021, 20 million households described having inadequate food during the week, and 10 million households struggled to pay rent.14 Poverty also contributes to other SDOH, including food insecurity, low education levels, and poor housing conditions. Individuals often lack resources to advance out of poverty, thus affecting families for multiple generations.13 This cycle of poverty increases risk for chronic diseases, premature death, and depression.13,15
Unable to work remotely, essential workers are critical to the country’s economy. Frontline workers require close interaction with consumers or coworkers in settings such as public-facing stores and hospitals.16,17 Increased risk of exposure is likely due to the outward nature of their occupations, increased use of public transportation, and inadequate social distancing at work.5,16 Despite this, essential workers persist in low-wage jobs to endure economic hardship.18 White-collar, remote-friendly jobs tend to pay higher average wages than jobs held by essential workers.16,18,19 Most essential workers, including over 6.5 million healthcare workers, earn less than the national median wage and are more likely to have lower education and socioeconomic class.17,18 Black, Hispanic, and undocumented immigrants largely overrepresent essential jobs.5,16,17,19 These occupations frequently lack workplace benefits and health insurance that allow workers to seek treatment.16,18 In oversaturated health systems, healthcare workers record higher rates of insomnia, fatigue, and emotional distress.20,21 Black and Hispanic essential healthcare workers disproportionately experience anxiety and depression symptoms, respectively.22 Essential workers also suffer increased risk of substance use and suicidal ideation.20
Education Access and Quality
Education level can serve as both a predictor and consequence of SDOH. Parental levels of education, poverty, and poorly resourced neighborhoods may mediate low education.23 In contrast, high-quality education increases chances of employment with livable wages, safe housing conditions, and access to healthcare.23,24 Socioeconomic advancements promote health equity, ultimately preventing comorbidities and mental illnesses associated with less education.23 As an indicator of health literacy, increased comprehension of health information allows for more informed decisions regarding health choices, from medication adherence to practice of COVID safety precautions.25
As a result of lockdown orders, children have been immeasurably impacted by school closures. Because many programs offer free meals during school hours, many children went hungry and suffered more food insecurity as a result. Children depend on schools to access the Internet and other resources to meet educational outcomes, but poor households are less likely to have access to the Internet or help for their schoolwork.5 Less education is associated with greater health risks, including but not limited to obesity, risky health behaviors, and substance abuse.7,24 These enlarged education gaps and adverse childhood experiences project a potentially challenging future for these children.5
Neighborhood and Built Environment
Neighborhood and community conditions impact well-being and development. Exposure to contaminants, homelessness, food insecurity, and increased rates of violence endanger the safety and health of residents.26 When neighborhoods are unstable as a result of vacant properties, foreclosures, predatory landlords, crime, and other socioeconomic problems, mistrust and violence increase.27 Increased suicides among middle-aged adults during the Great Recession between 2007 and 2009 were attributed to increased foreclosures.28
People of color are more likely to occupy unsafe neighborhoods and multigenerational households, with black and Hispanic households twice as likely as white households to be cost-burdened.5,27,29 These congested and overcrowded living conditions make social distancing difficult and increase risk of infectious disease transmission.5,29,30 Moreover, the pandemic’s stay-at-home and quarantine directives resulted in increased stress and domestic violence cases.31
Healthcare Systems
Populations who lack access to healthcare cannot receive necessary services for physical and mental illnesses. This is further compounded by economic instability, lack of affordable services, and global disruptions and defunding of mental health services.32,33 In rural areas, mental healthcare deserts highlight the scarcity of trained mental health professionals. Timely travel distances are challenged by inadequate transportation, lack of insurance, and poverty concurrent with rural geographical locations.34 Racial and ethnic minorities without proper mental health education may be less likely to utilize mental health services. Linguistic and cultural differences create communication barriers and can contribute to mistrust of health systems among some marginalized communities.25,35,36 Treatment for mental health illnesses can consequently be delayed. Investigators reviewing data from the National Latino and Asian American Study (2002-2003) identified the barriers that negatively impact the use of mental health–related services, including cultural barriers (stigma, loss of face), culturally unresponsive services (lack of language or ethnic match), limited access to care (cost, lack of insurance coverage), and lack of awareness or understanding of services.36 Due to these barriers, mental health concerns are likely underreported, so that it seems that these individuals do not need mental health services, when in fact seeking help has been stigmatized.
Community and Social Context
Discrimination contributes to trauma and is a direct effect of inadequate public policies in underprivileged communities.4,35 Racial discrimination, precipitated by conspiracy theories and political systems, is associated with psychological distress, depression, and anxiety. Recent murders of unarmed black people demonstrate social injustices and fear that are conducive to the mental health inequities vulnerable populations already experience.35 In addition, xenophobic beliefs regarding the origin of the COVID-19 pandemic have led to a rapid increase in hate crimes against Asian Americans and Pacific Islanders.37 Learned helplessness has been positively associated with depression in the literature.38 Marginalized groups (e.g., Asian Americans) succumb to social injustices and racial discrimination, which then perpetuates the narrative of being submissive and silent. The learned helplessness makes it difficult for these individuals to express emotions and vulnerability because they have become conditioned to accept the injustices that they face.39
A large body of literature has demonstrated that racism is associated with poor physical and mental health, including depression, anxiety, and psychological stress. According to a meta-analysis published in 2015, based on self-reported discrimination, there was no difference in mental health outcomes when it came to the age, sex, or birthplace of an individual, but ethnicity was a significant predictor in mental health outcomes. The association between racism and poor mental health was significantly greater for Asian Americans and Latin Americans compared with African Americans. However, the limitation to this meta-analysis was that only 9.4% of total individuals included were Asian; African American and European Americans made up the bulk of the study population, at 37% and 30%, respectively. One may theorize that Asian Americans may not report on acts of racism or discrimination, and thus, the full impact of racial violence is likely underreported beyond what studies have captured.40
Understanding the structural inequities of SDOH can help contextualize the disproportionate number of marginalized groups affected by COVID-19.7,25,41 While these SDOH and health inequities have defined our healthcare system for decades, the COVID-19 pandemic continues to amplify gaps in patient care.4,11 Social and health inequities aggravate one another, with marginalized groups having higher rates of infection, hospitalization, and mortality.42
Although mental health is necessary for achieving good overall health, it is often overlooked among COVID-related harms.11 In addition to increased risk for comorbidities and decreased health outcomes, SDOH disproportionately affect the mental health of vulnerable populations.4,6,35 While some may lack accessibility to adequate mental health services, the occupations, living conditions, and structural oppression experienced by marginalized groups increase allostatic load and worsen mental health inequities.15,18,34 With barriers to healthcare made more severe, expensive, and risky during the pandemic, mental health disparities have become increasingly widespread among disadvantaged groups.4
All healthcare providers, including pharmacists, have a responsibility to not only provide care to patients experiencing mental health illness and substance-use disorders but ultimately help to dismantle structural racism that underlies these SDOH.43
The Role of the Pharmacist
Pharmacists are in prime positions to facilitate resource navigation and direct patients to the help that they need. Community pharmacies are often more accessible to the public than a primary care office and can thus serve as safe havens for patients who are in need. By being aware of their community’s resources, pharmacists can serve as the bridge between a patient’s cry for help and the help that they need.
In a community or ambulatory setting, pharmacists can become trained to conduct SBIRT (Screening, Brief Intervention, and Referral to Treatment).44 By screening patients using this evidence-based approach, pharmacists can identify patients who screen positive for substance-use disorder and facilitate interventions towards behavioral changes through motivational interviewing or direct them to more specialized treatment. Similarly, because community pharmacists see patients frequently, they likely have established rapport and relationships with patients to a greater degree, allowing them to identify mental health disorders, such as depression and anxiety. By conducting these screenings, pharmacists can connect patients experiencing depression and/or even suicidal ideation to the proper help.
The local health department may have mental health resources that patients can turn to under certain circumstances. Pharmacists can familiarize themselves with their local or state department of health’s resources and direct their patients accordingly. The U.S. government has a website (www.usa.gov/state-social-services) with a directory of each state’s social services listings that pharmacists can access.45 Pharmacists can also utilize websites such as www.findhelp.org, which is a network that houses over 300,000 free or low-cost programs available through the search engine.46 By entering one’s ZIP code, one can filter out results by category or search for a specific program. Resource categories include health (including mental health), housing, food, and other SDOH resources. There may also be similar state or city-specific resources; one such example is the Health Information Tool for Empowerment (HITE) in New York City.47 The tool, available through www.hitesite.org, is an online directory listing over 6,000 resources for low-income, uninsured, and underinsured individuals and families. Search results can be filtered into categories specific to an individual’s needs; for mental health, categories include “hotlines” (e.g., for mental health and substance use) and “mental health & substance use.”
Local resources may include community-based organizations (CBOs), whose missions and objectives are specifically centered on addressing their communities’ needs.48 Pharmacies and healthcare institutions can develop partnerships with CBOs to provide a multitude of services that address any barriers patients may be facing, whether related to physical health or mental health. These CBOs are oftentimes most in tune with the norms, beliefs, and culture of the community they are situated in. By partnering with CBOs and understanding the root causes of the inequities that exist in the community, services can be tailored more strategically to produce the best outcomes.49
In a hospital setting, pharmacists on an interprofessional team can collaborate with behavioral health providers, social workers, case managers, and community health workers.50 They can conduct SDOH screening and use the results to facilitate resource navigation upon discharge. Screening tools are incorpocrated into the health system’s electronic medical record, and referral processes are designed to direct patients to the appropriate specialists or resources.51 Recent literature has also highlighted the significance of community pharmacies conducting SDOH screening and the need for more pharmacies to do so.52,53 Examples of SDOH-screening tools include the PRAPARE screening tool and the Health Leads screening toolkit, both available in multiple languages.54,55
Regardless of the practice setting, pharmacists can pursue mental health first aid training. Similar to SBIRT, CPR, or First Aid certification, mental health first aid is a means for an individual to identify and address signs of mental distress and substance-use disorders.56 Local departments of health or other institutions may host trainings that pharmacists can participate in to become certified. Pharmacists can also become trained as instructors of these courses to expand the reach of potentially lifesaving aid.
Conclusion
The COVID-19 pandemic has unmasked the inequities and disparities that patients of historically marginalized populations experience. Adverse health outcomes—both physical and mental—resulting from these disparities can be attributed to SDOH. As healthcare providers, pharmacists play vital roles in aiding patients facing mental health illnesses. Clinicians need to proactively conduct mental health screenings and be armed with the resources to provide culturally competent care. As public health advocates, pharmacists are able to provide equitable care for all individuals, but they also need to be engaged in the work to address the systemic barriers and determinants in communities at large in order to achieve health equity.
REFERENCES
1. Mayo Clinic Staff. COVID-19: How to manage your mental health during the pandemic. Mayo Clinic. November 23, 2021. www.mayoclinic.org/diseases-conditions/coronavirus/in-depth/mental-health-covid-19/art-20482731. Accessed February 22, 2022.
2. Czeisler MÉ, Lane RI, Petrosky E, et al. Mental health, substance use, and suicidal ideation during the COVID-19 pandemic—Unit ed States, June 24–30, 2020. Morb Mortal Wkly Rep. 2020;69:1049-1057. http://dx.doi.org/10.15585/mmwr.mm6932a1
3. Shim RS. Mental health inequities in the context of COVID-19. JAMA Netw Open. 2020;3(9):e2020104.4. Bernardini F, Attademo L, Rotter M, Compton MT. Social determinants of mental health as mediators and moderators of the mental health impacts of the COVID-19 pandemic. Psychiatr Serv. 2021;72(5):598-601.
5. COVID-19 and the social determinants of health and health equity: evidence brief. Geneva: World Health Organization; 2021.
6. Artiga S, Hinton E. Beyond health care: the role of social determinants in promoting health and health equity. KFF. May 10, 2018. Accessed February 25, 2022. www.kff.org/racial-equity-and-health-policy/issue-brief/beyond-health-care-the-role-of-social-determinants-in-promoting-health-and-health-equity/. Accessed February 25, 2022.
7. CDC. Health Disparities. www.cdc.gov/healthyyouth/disparities/index.htm. Updated November 24, 2020. Accessed February 28, 2022.
8. Kola L, Kohrt BA, Hanlon C, et al. COVID-19 mental health impact and responses in low-income and middle-income countries: reimagining global mental health [published correction in Lancet Psychiatry. 2021 Mar 8]. Lancet Psychiatry. 2021;8(6):535-550.
9. Ibrahimi S, Yusuf KK, Dongarwar D, et al. COVID-19 devastation of African-American families: impact on mental health and the consequence of systemic racism. Int J MCH AIDS. 2020;9(3):390-393.
10. Office of Behavioral Health Equity. Double jeopardy: COVID-19 and behavioral health disparities for black and Latino communities in the U.S. www.samhsa.gov/sites/default/files/covid19-behavioral-health-disparities-black-latino-communities.pdf?emci=125d59be-2b93-eb11-85aa-0050f237abef&emdi=7ed33923-4196-eb11-85aa-0050f237abef&ceid=7719978. Accessed February 22, 2022.
11. Dickinson KL, Roberts JD, Banacos N, et al. Structural racism and the COVID-19 experience in the United States. Health Security. 2021;19(S1):S-14-S-26.
12. APM Research Lab. Color of coronavirus: COVID-19 deaths analyzed by race and ethnicity. www.apmresearchlab.org/covid/deaths-by-race. Accessed February 28, 2022.
13. Healthy People 2020. Poverty. www.healthypeople.gov/2020/topics-objectives/topic/social-determinants-health/interventions-resources/poverty. Accessed February 22, 2022.
14. Center on Budget and Policy Priorities. Tracking the COVID-19 economy’s effects on food, housing, and employment hardships. September 10, 2021. www.cbpp.org/research/poverty-and-inequality/tracking-the-covid-19-economys-effects-on-food-housing-and. Accessed February 22, 2022.
15. Compton MT, Shim RS. The social determinants of mental health. FOC. 2015;13(4):419-425.
16. Casura L, Lowe Jr R, Martinez C, et al. Frontline workers in the U.S.: race, ethnicity, and gender. N-IUSSP. September 7, 2020. www.niussp.org/education-work-economy/frontline-workers-in-the-u-s-race-ethnicity/. Accessed February 28, 2022.
17. School of Public Health, University of Illinois Chicago. Black, Hispanic Americans are overrepresented in essential jobs. https://publichealth.uic.edu/news-stories/black-hispanic-americans-are-overrepresented-in-essential-jobs/. Accessed February 28, 2022.
18. Damian AJD, Armah T, Lee-Winn AE. An intersectional approach to understanding the mental health challenges of America’s essential workers. http://info.primarycare.hms.harvard.edu/review/mental-health-essential-workers. Accessed February 28, 2022.
19. Gent E. What remote jobs tell us about inequality. www.bbc.com/worklife/article/20200921-what-remote-jobs-tell-us-about-inequality. Accessed February 28, 2022.
20. Magill E, Siegel Z, Pike KM. The mental health of frontline health care providers during pandemics: a rapid review of the literature. Psychiatr Serv. 2020;71(12):1260-1269.
21. Mental Health America. The mental health of healthcare workers in COVID-19. https://mhanational.org/mental-health-healthcare-workers-covid-19. Accessed February 22, 2022.
22. Grooms J, Ortega A, Rubalcaba JA-A, Vargas E. Racial and ethnic disparities: Essential workers, mental health, and the coronavirus pandemic. The Review of Black Political Economy. Publ online August 10, 2021.
23. Healthy People 2020. Enrollment in higher education. www.healthypeople.gov/2020/topics-objectives/topic/social-determinants-health/interventions-resources/enrollment-in-higher. Accessed February 28, 2022.
24. Social determinant of health: education is crucial. https://publichealth.tulane.edu/blog/social-determinant-of-health-education-is-crucial/. Accessed February 28, 2022.
25. CDC. Office of Disease Prevention and Health Promotion. Healthy People 2020. Health literacy. www.healthypeople.gov/2020/topics-objectives/topic/social-determinants-health/interventions-resources/health-literacy.
26. Center on Budget and Policy Priorities. Tracking the COVID-19 economy’s effects on food, housing, and employment hardships. www.cbpp.org/research/poverty-and-inequality/tracking-the-covid-19-economys-effects-on-food-housing-and. Accessed February 22, 2022.
27. Kingsley GT, Smith R, Price D. The impacts of foreclosures on families and communities. The Urban Institute, Washington DC. May 2009. www.urban.org/sites/default/files/publication/30426/411909-The-Impacts-of-Foreclosures-on-Families-and-Communities.PDF. Accessed March 1, 2022.
28. Houle JN, Light MT. The home foreclosure crisis and rising suicide rates, 2005 to 2010. Am J Public Health. 2014;104(6):1073-1079.
29. Housing instability. Healthy People 2030. ODPHP. https://health.gov/healthypeople/objectives-and-data/social-determinants-health/literature-summaries/housing-instability. Accessed March 1, 2022.
30. The Center for Public Integrity. Map: COVID put America’s multigenerational homes at higher risk. December 21, 2021. https://publicintegrity.org/health/coronavirus-and-inequality/map-covid-multigenerational-homes-higher-risk/. Accessed February 22, 2022.
31. SAMHSA. Intimate partner violence and child abuse considerations during COVID-19. Publ online 2020. www.samhsa.gov/sites/default/files/social-distancing-domestic-violence.pdf. Accessed March 1, 2022.
32. ODPHP. Healthy People 2030. Neighborhood and built environment. https://health.gov/healthypeople/objectives-and-data/browse-objectives/neighborhood-and-built-environment. Accessed March 1, 2022.
33. Healthy People 2030. ODPHP. Health care access and quality. https://health.gov/healthypeople/objectives-and-data/browse-objectives/health-care-access-and-quality. Accessed February 28, 2022.
34. COVID-19 is taking a heavy toll in America’s mental health-care deserts. Science. www.nationalgeographic.com/science/article/coronavirus-is-taking-heavy-toll-america-mental-health-care-deserts. Accessed February 25, 2022
35. Cokley K, Krueger N, Cunningham SR, et al. The COVID‐19/racial injustice syndemic and mental health among Black Americans: the roles of general and race‐related COVID worry, cultural mistrust, and perceived discrimination [published online ahead of print, 2021 Nov 19]. J Community Psychol. 2021.
36. Abe-Kim J, Takeuchi DT, Hong S, et al. Use of mental health-related services among immigrant and US-born Asian Americans: results from the National Latino and Asian American Study. Am J Public Health. 2007;97(1):91-98.
37. Zhou S, Banawa R, Oh H. The mental health impact of COVID-19 racial and ethnic discrimination against Asian American and Pacific Islanders. Front Psychiatry. 2021;12:708426. Published 2021 Nov 17.
38. Kalibatseva Z, Leong FTL. Depression among Asian Americans: review and recommendations. Depress Res Treat. 2011;2011:320902.
39. Smallheer BA, Vollman M, Dietrich MS. Learned helplessness and depressive symptoms following myocardial infarction. Clin Nurs Res. 2018;27(5):597-616.
40. Paradies Y, Ben J, Denson N, et al. Racism as a determinant of health: a systematic review and meta-analysis. PLoS ONE. 2015;10(9):e0138511.
41. Egede LE, Walker RJ. Structural racism, social risk factors, and COVID-19—a dangerous convergence for Black Americans. N Engl J Med. 2020;383(12):e77.
42. Lopez L 3rd, Hart LH, Katz MH 3rd. Racial and ethnic health disparities related to COVID-19. JAMA. 2021;325(8):719-720.
43. Arya V, Butler L, Leal S, et al. Systemic racism: pharmacists’ role and responsibility. J Am Pharm Assoc (2003). 2020;60(6):e43-e46.
44. Screening, Brief Intervention, and Referral to Treatment (SBIRT). www.samhsa.gov/sbirt. Accessed February 18, 2022.
45. USAGov. State social service agencies. www.usa.gov/state-social-services. Accessed February 25, 2022.
46. The Social Care Network. Findhelp.org. www.findhelp.org/. Accessed February 19, 2022.
47. HITE | About us. https://hitesite.org/about. Accessed February 21, 2022.
48. National Academies of Sciences, Engineering, and Medicine. 2018. Exploring equity in multisector community health partnerships: proceedings of a workshop. Washington, DC: The National Academies Press.
49. CDC–Division of Community Health. A practitioner’s guide for advancing health equity: community strategies for preventing chronic disease. Atlanta, GA: US Department of Health and Human Services. 2013.
50. Schechter SB, Lakhaney D, Peretz PJ, Matiz LA. Community health worker intervention to address social determinants of health for children hospitalized with asthma. Hosp Pediatr. 2021;11(12):1370-1376.
51. Bradywood A, Leming-Lee TS, Watters R, Blackmore C. Implementing screening for social determinants of health using the Core 5 screening tool. BMJ Open Qual. 2021;10(3):e001362.
52. Foster AA, Daly CJ, Logan T, et al. Addressing social determinants of health in community pharmacy: Innovative opportunities and practice models. J Am Pharm Assoc (2003). 2021;61(5):e48-e54. Epub 2021 May 4.
53. Kiles TM, Borja-Hart N, Wofford BR, Renfro CP. Screening for social determinants of health in community pharmacy: Identifying best practices, barriers, and strategies for success. J Am Pharm Assoc (2003). 2021 Sep-Oct;61(5):e59-e63. Epub 2021 May 14.
54. PRAPARE. The PRAPARE Screening Tool. Accessed February 25, 2022. https://prapare.org/the-prapare-screening-tool/
55. Health Leads. The Health Leads Screening Toolkit. Accessed February 25, 2022. https://healthleadsusa.org/resources/the-health-leads-screening-toolkit/
56. About MHFA. Mental health first aid. www.mentalhealthfirstaid.org/about/. Accessed February 25, 2022.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.






