US Pharm. 2020;45(7/8):18-24.
ABSTRACT: Establishing asthma symptom control using pharmacologic and nonpharmacologic interventions improves quality of life and prevents exacerbations in patients with asthma. The Global Initiative for Asthma 2019 guidelines provide recommendations for asthma treatment organized into five steps that correlate with disease severity. Medication options include inhaled corticosteroids (ICS), long-acting beta2 agonists, short-acting beta2 agonists (SABAs), leukotriene receptor antagonists, and oral corticosteroids. Recent data show unfavorable outcomes for SABAs used alone for as-needed treatment of symptoms of mild asthma. Guideline changes include the use of a low-dose ICS with formoterol for as-needed treatment in adults with mild asthma, or for use whenever a SABA would be used. Appropriate, effective medication regimens combined with counseling on proper inhaler technique will help patients achieve asthma-management goals.
Asthma, a chronic inflammatory airway disease characterized by airway hyperresponsiveness, may present with symptoms such as wheezing, shortness of breath, chest tightness, and cough.1 These symptoms may vary over time and in intensity, making effective management of asthma important. Symptom triggers may include exercise, viral respiratory infections, and environmental factors, such as smoking. Symptoms that are left untreated may lead to exacerbations. An exacerbation is an acute episode in which symptoms worsen drastically and lung function progressively declines. Any occurrence of an exacerbation warrants a discussion regarding the patient’s current asthma treatment regimen because of the risks of hospitalization, emergency-care visits, and asthma-related death.
The 2019 Global Initiative for Asthma (GINA) guidelines do not recommend the use of a short-acting beta2 agonist (SABA) inhaler alone for the treatment of mild asthma; instead, they recommend low-dose inhaled corticosteroid (ICS)-formoterol use as needed and for maintenance therapy.2 In patients who present with severe or difficult-to-treat asthma, other options may be considered as add-ons to inhaler therapy, such as leukotriene receptor antagonists (LTRAs), tiotropium, biologics, azithromycin, and oral corticosteroids (OCS).
ASSESSMENT
Asthma control denotes the extent to which asthma features can be observed in the patient or have been reduced or eliminated by treatment.2 Asthma control should be reviewed over the previous 4 weeks. The patient should be asked the following questions: “In the previous 4 weeks, have you had: 1) daytime asthma symptoms more than twice per week? 2) any nighttime awakenings due to asthma? 3) to use an asthma reliever for symptoms more than twice per week? 4) any activity limitations due to asthma?” If the patient answers “No” to all four questions, his or her asthma is well controlled. If the patient answers “Yes” to one or two of the questions, the asthma is partially controlled, but if the answer is “Yes” to three to four of the questions, the asthma is not well controlled.2 Risk factors that may cause an exacerbation include uncontrolled asthma, smoking, allergen exposure, air pollution, comorbidities such as obesity, and high SABA use.
Assessing adherence to the patient’s inhaled medication is another important step. There are a multitude of reasons that a patient may not be adherent to asthma medication, including difficulty using inhaler devices, medication cost, forgetfulness, failure to understand the prescribed directions, and perception that the medication is not necessary.2
MANAGEMENT AND TREATMENT
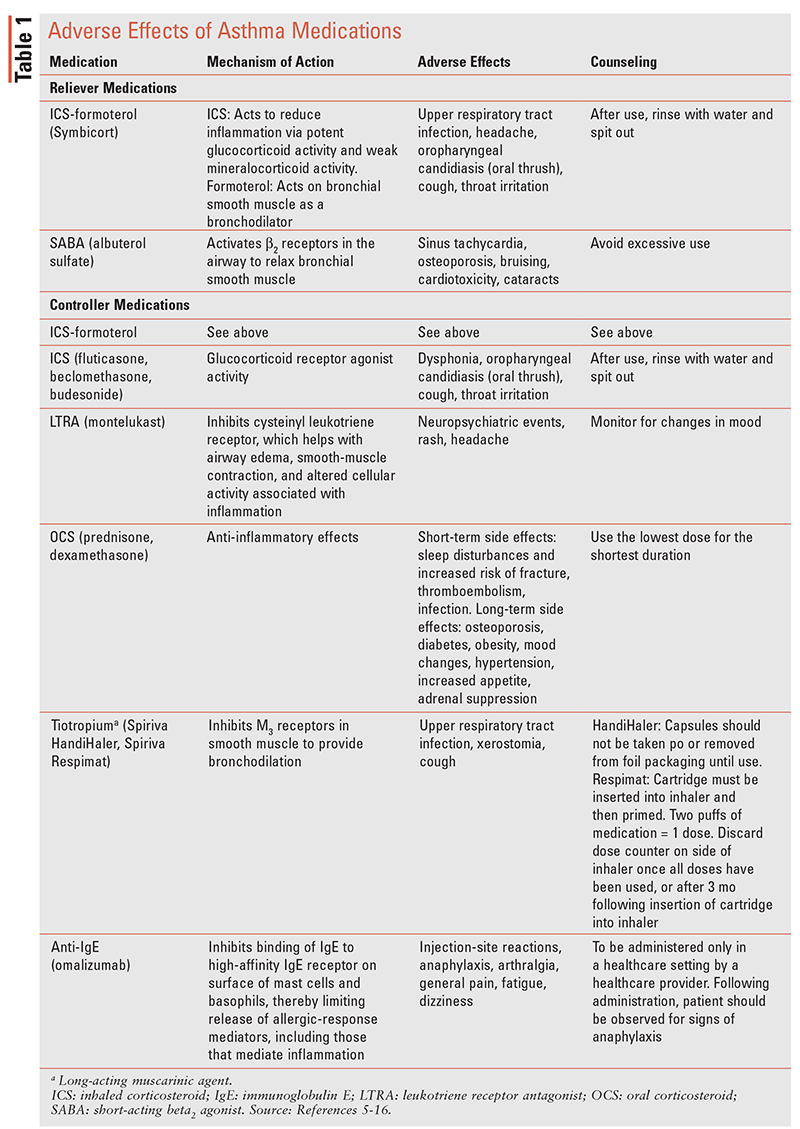
Goals of therapy for asthma include achieving control of symptoms to maintain normal activity levels, preventing persistent airflow limitation, and reducing adverse effects of the medications discussed in TABLE 1. Pharmacologic and nonpharmacologic interventions reduce the risk of future exacerbations leading to hospitalization or asthma-related death.2
Nonpharmacologic Management
Nonpharmacologic interventions for all asthma patients include breathing exercises, increased physical activity, incorporation of a healthy diet, and avoidance of exposure to smoke and other substances.2 The practice of yoga and breathing methods such as the Buteyko and Papworth techniques alters breathing patterns to reduce hyperventilation, thereby promoting voluntary reduction in reliever use and improving asthma symptoms.3 In obese patients, weight loss combined with twice-weekly aerobic and strength exercises is more effective than physical activity alone for symptom control.2 Counseling on proper inhaler technique will help patients achieve asthma-management goals.
Pharmacologic Management
Adjustments are made to asthma-medication regimens through the control-based asthma-management cycle depicted in FIGURE 1.2
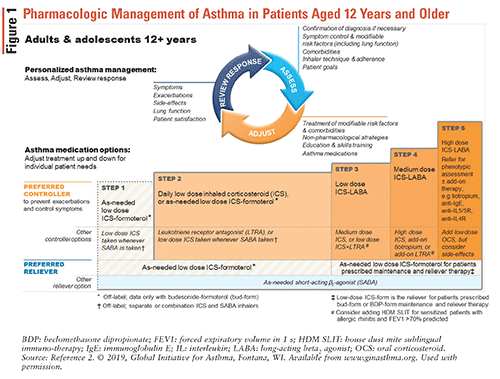
Once a diagnosis of asthma has been made, an ICS-containing controller treatment should be initiated because of the greater improvement in lung function than when ICS controller treatment is not used. This is an important change in the 2019 GINA guidelines, as it was previously recommended to give newly diagnosed patients a SABA alone. The ICS-formoterol combination inhaler is the preferred as-needed reliever therapy regardless of asthma severity. The alternative reliever therapy is a SABA; however, it must be paired with a second inhaler containing ICS. ICS-formoterol inhalers are safe and efficacious, and their ability to be used both as needed and for maintenance therapy makes them easy for patients to use.2
GINA recommends the following asthma-treatment steps2:
• Step 1: This step is advised for patients with mild asthma who have symptoms less than twice per month and no risk of exacerbations. As mentioned previously, based on new evidence, the 2019 GINA guidelines no longer recommend SABA use alone to treat asthma.
• Step 2: The preferred controller regimen is as-needed low-dose ICS-formoterol or daily low-dose ICS plus as-needed SABA. The ICS-formoterol regimen avoids the need for daily ICS while providing similar benefits for exercise-induced bronchoconstriction as daily ICS with as-needed SABA.
• Step 3: Preferred controller treatments include a low-dose ICS–long-acting beta2 agonist (LABA) plus as-needed SABA or low-dose ICS-formoterol for both maintenance and reliever therapy.
• Step 4: The preferred controller treatment is low-dose ICS-formoterol as maintenance and reliever therapy or medium-dose ICS-LABA as maintenance plus as-needed SABA. Note that ICS-formoterol should not be combined with an ICS-LABA containing a different LABA.
• Step 5: Persistent exacerbations or symptom worsening occurs despite adherence and correct inhaler technique. These patients are considered to have severe or difficult-to-treat asthma and should be referred to a pulmonologist.
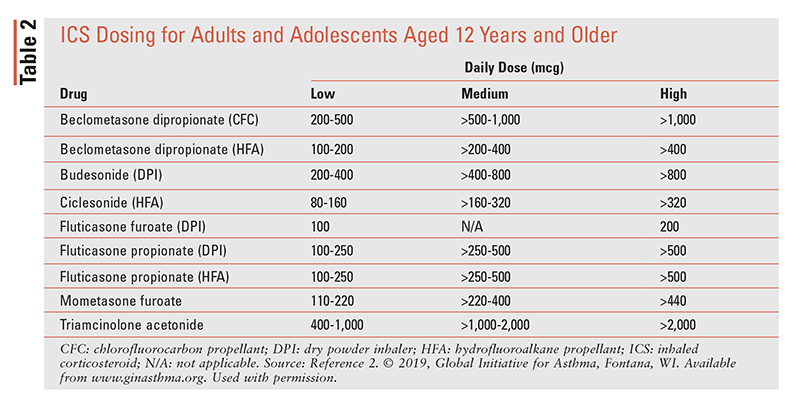
Stepping up through the stages outlined above is appropriate when patients have persistently poor symptom control or exacerbations despite low-dose ICS treatment for 2 to 3 months. Stepping down is appropriate when the patient has good symptom control and stable lung function for at least 3 months. Options for stepping down depend on which medication the patient is taking and which step the patient is on, but for most patients, the outcome is worse if the ICS or LABA is stopped completely.2 ICS dosing is outlined in TABLE 2.
Symptoms can be assessed with tools such as the Asthma Control Questionnaire, the Asthma Control Test, and the Royal College of Physicians’ Three Questions.2 These questionnaires enable a score to be associated with symptoms and ask patients about the frequency and types of symptoms such as nighttime awakenings and limitations in daily activities.
Exacerbations
The term asthma exacerbation refers to the acute worsening of lung function and symptoms beyond what the patient usually experiences. The preferred reliever treatment during an exacerbation is low-dose ICS-formoterol that can be increased as needed when symptoms worsen. Use of an ICS-LABA (beclomethasone or budesonide and formoterol) as both reliever and controller medication improves symptom control and reduces hospitalizations and OCS use compared with the same or higher dose of a controller plus as-needed SABA.4
A short OCS course is a treatment option during an exacerbation when the patient fails to respond to an increased dose of reliever and controller after 2 to 3 days, has a history of sudden severe exacerbations, or has rapidly deteriorating lung function (peak expiratory flow or forced expiratory volume in 1 second <60% of personal best or predicted value).4
Adverse Effects of Asthma Medications
See TABLE 1 for a summary of adverse effects of various asthma medications.5-16
SEVERE OR DIFFICULT-TO-TREAT ASTHMA
Severe or difficult-to-treat asthma refers to uncontrolled asthma at treatment steps 4 and 5 despite adequate adherence to treatment and treatment of contributory factors. After initial assessment, patients aged 12 years and older with inadequately controlled asthma who are taking a medium-dose ICS plus a LABA and/or a third controller, such as LTRA or sustained-release theophylline, are switched to a trial of a high-dose ICS for 3 to 6 months. In addition to increasing the ICS, a trial of an add-on nonbiologic such as tiotropium, a leukotriene modifier, or OCS may be considered. For adult patients who have persistent asthma symptoms despite moderate-dose or high-dose ICS and LABA, the 2019 GINA guidelines recommend azithromycin as an add-on.17
If nonbiologics such as LABA, tiotropium, and leukotriene modifiers fail to manage a patient’s asthma symptoms, then biologics may be considered depending on the price and the patient’s resources. Anti–immunoglobulin E therapy, such as omalizumab, may be considered in those with allergic asthma. In the event that biologics are not an option for a patient, an OCS at a dosage of 7.5 mg or less per day prednisone equivalent may be considered. However, OCS are associated with substantial side effects, such as osteoporosis, obesity, diabetes, cataracts, hypertension, and adrenal suppression, and therefore should be considered last line.17
STUDIES
A double-blind trial conducted by O’Byrne and colleagues investigated the benefit of using an ICS plus a SABA compared with conventional treatment.18 A total of 3,849 patients aged 12 years or older with mild asthma were randomly assigned to terbutaline (twice-daily placebo plus terbutaline 0.5 mg prn), budesonide-formoterol (twice-daily placebo plus budesonide-formoterol 200 mcg/6 mcg prn), or budesonide maintenance (twice-daily budesonide 200 mcg plus terbutaline prn). The primary objective was to determine whether as-needed budesonide-formoterol was superior to as-needed terbutaline for symptom control. This outcome was measured via data obtained from an electronic symptom diary.
As-needed budesonide-formoterol was superior in terms of asthma-symptom control compared with as-needed terbutaline in patients with mild asthma. Budesonide-formoterol patients showed well-controlled asthma for 34.4% of weeks versus 31.1% of weeks in the terbutaline group (P = .046). Terbutaline was associated with the highest annual rate of severe exacerbations (0.20) compared with budesonide-formoterol (0.07) and budesonide maintenance (0.09). A benefit of budesonide-formoterol use was that exposure to corticosteroids was reduced because of the 17% lower budesonide dose in this group compared with the budesonide-maintenance group (57 mcg vs. 340 mcg, respectively).18
Bateman and colleagues researched the effectiveness of an inhaled glucocorticoid component with a fast-acting reliever for mild asthma.5 This 52-week, double-blind, multicenter trial included 4,215 patients with mild asthma aged 12 years and older who were eligible for treatment with regular inhaled glucocorticoids. Participants were divided into two groups to assess whether as-needed budesonide-formoterol or budesonide maintenance therapy twice daily had better efficacy with regard to annual rates of severe exacerbations. The budesonide-formoterol group was noninferior to the budesonide-maintenance group for severe exacerbations. In addition, the median daily metered dose of inhaled glucocorticoid was lower in the budesonide-formoterol group (66 mcg) than in the budesonide-maintenance group (267 mcg). The time to first exacerbation was similar between the groups; however, there was a difference of 0.11 U in favor of the budesonide-maintenance group, which had lower scores on the Asthma Control Questionnaire-5 (ACQ-5) compared with the budesonide-formoterol group. The minimal clinically important difference in ACQ-5 scores is 0.5 U. Additionally, there was no difference in adverse events, asthma-related discontinuations, or mortality rate between the two groups. This study and the O’Byrne study support the current 2019 GINA recommendation against the use of a SABA alone and for the use of ICS-formoterol instead.
A study by Gibson and colleagues investigated the efficacy and safety of oral azithromycin as add-on therapy in patients with uncontrolled persistent asthma also taking a medium-dose or high-dose ICS plus a LABA.17 In this randomized, double-blind, placebo-controlled, parallel-group trial, 420 patients were randomly assigned to one of two treatment groups (azithromycin 500 mg or placebo three times per week for 48 weeks). The primary efficacy endpoints included rate of total (severe and moderate) asthma exacerbations and overall asthma-related quality of life over the study period.
In the Gibson study, azithromycin was found to reduce asthma exacerbations; 44% of azithromycin patients experienced at least one exacerbation, compared with 61% of placebo patients (P <.0001). Additionally, azithromycin use significantly benefited asthma-related quality of life, denoted by improvement in all categories of the rating scale (i.e., activity, symptom, emotion, and environmental domains) for asthma-related quality of life. The only other notable difference between the study groups was in the occurrence of diarrhea, which was significantly higher in azithromycin patients (34% vs. 19% of placebo patients). For safety monitoring, ECGs were conducted at screening, after 6 weeks of treatment, and at the end of treatment. A QTc prolongation longer than 480 ms resulted in withdrawal from the trial in two patients (one from each group).17
CHANGES IN THE 2019 GUIDELINES
The 2019 guidelines include five notable changes with regard to asthma treatment in adults. The first change is the switch from SABA-only treatment to ICS-containing treatment for as-needed treatment of symptoms in mild asthma.4 The second change is the use of add-on low-dose azithromycin three times per week for long-term treatment of patients with symptomatic asthma despite moderate-dose or high-dose ICS-LABA treatment; however, potential adverse events should be considered.17
The third change is the recommendation for dupilumab, an anti–interleukin-4 receptor alpha monoclonal antibody, as an additional treatment option for patients aged 12 years and older with severe type 2 asthma or OCS-dependent asthma.19 A trial by Wenzel and colleagues demonstrated that dupilumab increased lung function and reduced severe exacerbations in patients with uncontrolled persistent asthma.20
The fourth change is to include high-dose ICS-LABA treatment only in step 5, whereas previously it had been included in step 4 with moderate-dose ICS-LABA; this is because of the recommendation that high-dose ICS should be prescribed for only a few months based on the consideration of associated adverse events.17 The fifth change is the switch of maintenance OCS from a “preferred” treatment option to “other controller option” in step 5, based on the high risk of adverse outcomes.19
CONCLUSION
Based on new data, the updated 2019 GINA guidelines do not recommend the use of a SABA inhaler alone for the treatment of mild asthma; instead, low-dose ICS-formoterol is recommended for as-needed and maintenance therapy. For patients who present with severe or difficult-to-treat asthma, other options may be considered as add-on treatment to inhaler therapy, including LTRA, tiotropium, biologics, azithromycin, and OCS. To ensure better medication adherence, asthma therapy regimens should be patient-specific, with a stepwise approach taken to find a regimen that controls the patient’s asthma symptoms while keeping the patient on the lowest dose possible, and should also be cost-effective.
REFERENCES
1. Asthma and Allergy Foundation of America. Asthma. www.aafa.org/asthma-symptoms. Accessed April 8, 2020.
2. Global Initiative for Asthma. Global strategy for asthma management and prevention, 2019. www.ginasthma.org. Accessed April 8, 2020.
3. Santino TA, Chaves GS, Freitas DA, et al. Breathing exercises for adults with asthma. Cochrane Database Syst Rev. 2020;3(3):CD001277.
4. O’Byrne PM, FitzGerald JM, Bateman ED, et al. Inhaled combined budesonide-formoterol as needed in mild asthma. N Engl J Med. 2018;378(20):1865-1876.
5. Bateman ED, Reddel HK, O’Byrne PM, et al. As-needed budesonide-formoterol versus maintenance budesonide in mild asthma. N Engl J Med. 2018;378(20):1877-1887.
6. Symbicort (budesonide-formoterol) package insert. Wilmington, DE: AstraZeneca Pharmaceuticals LP; January 2017.
7. Reed CE. Asthma in the elderly: diagnosis and management. J Allergy Clin Immunol. 2010;126(4):681-687.
8. ProAir HFA (albuterol) package insert. Frazer, PA: Teva Respiratory, LLC; February 2019.
9. Flovent HFA (fluticasone) package insert. Research Triangle Park, NC: GlaxoSmithKline; January 2019.
10. Singulair (montelukast) package insert. Whitehouse Station, NJ: Merck & Co, Inc; April 2020.
11. Waljee AK, Rogers MA, Lin P, et al. Short term use of oral corticosteroids and related harms among adults in the United States: population based cohort study. BMJ. 2017;357:j1415.
12. Foster JM, McDonald VM, M Guo, Reddel HK. “I have lost in every facet of my life”: the hidden burden of severe asthma. Eur Respir J. 2017;50(3):1700765.
13. Rayos (prednisone) package insert. Deerfield, IL: Horizon Pharma, Inc; 2012.
14. Spiriva HandiHaler (tiotropium) package insert. Ridgefield, CT: Boehringer Ingelheim Pharmaceuticals, Inc; February 2018.
15. Spiriva Respimat (tiotropium) package insert. Ridgefield, CT: Boehringer Ingelheim Pharmaceuticals, Inc; March 2019.
16. Xolair (omalizumab) package insert. South San Francisco, CA: Genentech, Inc; May 2019.
17. Gibson PG, Yang IA, Upham JW, et al. Effect of azithromycin on asthma exacerbations and quality of life in adults with persistent uncontrolled asthma (AMAZES): a randomised, double-blind, placebo-controlled trial. Lancet. 2017;390(10095):659-668.
18. O’Byrne PM, Barnes PJ, Rodriguez-Roisin R, et al. Low dose inhaled budesonide and formoterol in mild persistent asthma: the OPTIMA randomized trial. Am J Respir Crit Care Med. 2001;164(8):1392-1397.
19. Castro M, Corren J, Pavord ID, et al. Dupilumab efficacy and safety in moderate-to-severe uncontrolled asthma. N Engl J Med. 2018;378(26):2486-2496.
20. Wenzel S, Castro M, Corren J, et al. Dupilumab efficacy and safety in adults with uncontrolled persistent asthma despite use of medium-to-high-dose inhaled corticosteroids plus a long-acting beta2 agonist: a randomised double-blind placebo-controlled pivotal phase 2b dose-ranging trial. Lancet. 2016;388(10039):31-44.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





