US Pharm. 2015;40(10):33-38.
ABSTRACT: Historically, millions of Americans have been uninsured or underinsured owing to the disjointed nature of the U.S. healthcare system. Sweeping changes to the healthcare system are being made by federal legislation known as the Affordable Care Act, which was signed into law in 2010. Although U.S. healthcare spending far exceeds that of any other country, the United States has poorer health outcomes with respect to preventable disease. It is speculated that the Affordable Care Act will benefit the U.S. population in many ways. It is to be hoped that this act will be a source of expanded future opportunities for pharmacists to improve patient outcomes through provision of comprehensive services.
Historically, the U.S. healthcare system has been disjointed and rigid, with millions of Americans either uninsured or underinsured. In 2010, President Barack Obama signed into law a new healthcare statute, the Affordable Care Act (ACA).1 The ACA comprises two pieces of legislation: the Patient Protection and Affordable Care Act (enacted March 23, 2010) and the Health Care and Education Reconciliation Act (enacted March 30, 2010).1
Objectives of the ACA
The main objectives of the ACA (informally referred to as Healthcare Reform or ObamaCare) are to expand health insurance coverage to an estimated 32 million uninsured Americans and to strengthen existing coverage.1 The ACA is intended to increase benefits and lower costs for consumers; provide new funding for public health and disease prevention; bolster the healthcare and public-health workforce and infrastructure; and foster innovation and quality in the system. Furthermore, the ACA is expected to improve health quality; lower healthcare costs; provide new consumer protections; expand access to care through the healthcare marketplace; hold insurance companies accountable; and benefit certain special populations (TABLE 1).2

Under the new law, a Patient’s Bill of Rights confers upon individuals the flexibility essential for making informed choices concerning their health.3 The Patient’s Bill of Rights has three areas of focus: coverage, costs, and care. Under the coverage section, the ACA ends preexisting-condition exclusions for children, keeps young adults covered, ends arbitrary withdrawals of insurance coverage, and guarantees an individual’s right to appeal.4 The ACA is also designed to end lifetime limits on coverage, review insurance premiums, and help maximize funds to enable patients to get the most for their money.3 The ACA covers preventive care at no cost, protects patients’ choice of physician, and removes insurance companies’ barriers to emergency services.3
The ACA is designed to ensure that health plans offered in individual and small-group markets offer a comprehensive package of items and services called essential health benefits.5 Essential health benefits include ambulatory patient services; emergency services; hospitalization; maternity and newborn care; mental health and substance-use disorder services; prescription drugs; rehabilitative and habilitative services and devices; laboratory services; preventive and wellness services, including chronic disease management; and pediatric services.5 Insurance policies must cover these health benefits in order to be certified and included in the Health Insurance Exchange Marketplace (explained later).5 As of April 2014, >13.5 million people were eligible to enroll in a marketplace plan, and >8 million people had actually selected a plan.6 Approximately 8.75 million adults are uninsured and eligible for Medicaid under the ACA.6 Almost 5 million adults are classified as being in the coverage gap6; i.e., they do not have health insurance coverage because they earn too much to qualify for Medicaid, but too little to qualify for Health Insurance Exchange Marketplace premium tax credits.
Special Populations
The health reform law is intended to provide more health security for people who need insurance coverage. The ACA is structured to enable >3 million young adults aged 21 to 26 years to receive health insurance under a parent’s plan; >3 million senior citizens to receive a 50% discount on their prescription drugs; and millions more individuals to gain access to free preventive services.6 Elimination of abusive insurance practices by third-party insurance companies is a target of the ACA, as well.6
Insurers can no longer put a lifetime cap on how much care they will pay for if a patient becomes sick, or cancel patients’ coverage if their paperwork contains an error.6 As of 2014, health insurance companies are prohibited from charging women more for their healthcare coverage and from denying coverage to children younger than 19 years of age who have a preexisting condition.6 Moreover, health insurers are prohibited from discriminating against any patient for preexisting conditions, and in every state a Preexisting Condition Insurance Plan is to be offered for these patients.6 Additionally, the new 80/20 rule mandates that insurance companies spend at least 80 cents of each premium dollar on healthcare or improvements to care.6 Finally, insurance companies must publicly justify their reasoning and actions if they want to raise monthly premiums by ≥10%.6
The new provisions set forth by the ACA were developed to protect patients and to reduce the burden of uncompensated care on physicians and hospitals.6 Small-business owners have the ability to seek better coverage options for their employees and build on the employer-based insurance market already in place.6 Given that consumers and business owners have more control, small-business owners are expected to be able to make healthcare coverage more affordable for their workers.6 Elderly and disabled patients can now obtain private insurance without fear of discrimination based on preexisting conditions.6 In addition, new long-term and community-based care options have been made accessible for purchase by disabled and elderly persons.
Individual Mandate
A requirement of the ACA was for most persons to have health insurance or health coverage as of January 1, 2014, and that health insurance could be through an employer or an individual plan.7 Health coverage may be through programs such as Medicare, Medicaid, Florida Healthy Kids, TRICARE, federal employee health benefit plans, Veterans Health Care, and the Indian Health Service.7
There are several populations that may not be eligible under the ACA. These include, but are not limited to, persons for whom coverage would be unaffordable, undocumented immigrants, and members of healthcare-sharing ministries, as well as Amish, Mennonite, and Indian tribal communities.7 Also ineligible are individuals with a hardship that prevents them from obtaining health coverage and persons at or below 100% of the federal poverty level and eligible for Medicaid expansion (discussed in greater detail later).7
Persons without health coverage who are not exempt from the federal requirement may be subject to making a shared-responsibility payment to the Internal Revenue Service. Individuals will not have to make a payment if they cannot afford coverage, go <3 consecutive months without coverage, or qualify for an exemption.7 The total annual tax penalty is the greater of either a flat dollar amount or a percentage of taxable income: $95 per person or 1% of taxable income in 2014; $326 per person or 2% of taxable income in 2015; $695 per person or 2.5% of taxable income in 2016; and, after 2016, annual increases will be based on a cost-of-living adjustment.7
Perceived Need for the ACA
In July 2012, the Congressional Budget Office estimated that 53 million Americans aged <65 years were uninsured (1 in 5 persons in this population). Most uninsured individuals go without health coverage because they cannot afford it, and they would purchase it given an affordable opportunity. Uninsured persons are less likely to receive preventive care services or to seek care quickly when they become sick or injured, resulting in higher costs when they finally do seek treatment. Healthcare spending represented approximately 17% of the gross domestic product in 2012.8 Expenditure is expected to reach 20% by the year 2020, and the U.S. already spends far more on medical care than does any other industrialized nation (FIGURE 1).8 In 2011, the life expectancy for U.S. citizens was nearly 79 years, and the U.S. ranked 27 among countries associated with the Organisation for Economic Co-operation and Development (FIGURE 2).8
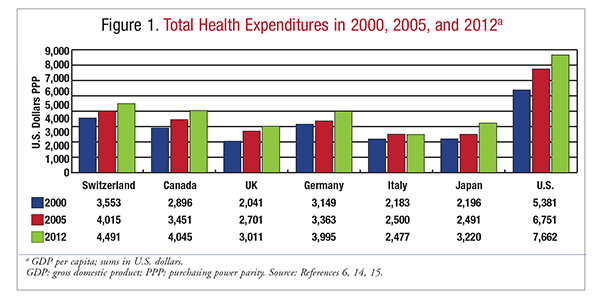
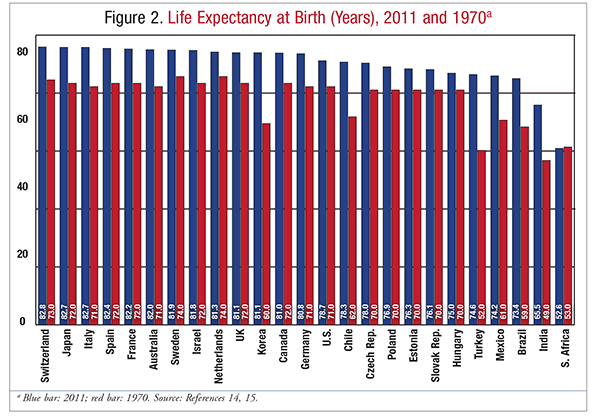
According to the CDC in 2010, the majority of deaths in the U.S. are related to preventable diseases such as obesity, diabetes, high blood pressure, heart disease, and cancer.9 Moreover, while inequities related to income and access to coverage exist across demographic lines, population-based disparities are demonstrable. For example, among women of all racial and ethnic backgrounds, African Americans have the highest death rates from heart disease, breast and lung cancer, stroke, and pregnancy.9 Prevention efforts, such as smoking cessation, could drastically reduce the occurrence of these chronic conditions, diminish the number of health disparities across the board, and decrease the incidence rate over time.
How Pharmacy Is Affected
Pharmacists have an unparalleled opportunity to spearhead improvements in overall quality of care and to create a better-coordinated healthcare system. Pharmacists can be part of medical home teams and can help improve the health of high-risk patients and patients with chronic conditions in primary care settings. Five areas of the ACA focus on pharmacy involvement: delivery systems reform, payment reform and quality, comparative effectiveness research, workforce issues, and the 340B Drug Pricing Program (DPP).10 Hospital and health-system pharmacists must promote their own clinical and economic value within their organizations.
Patients will have greater access to pharmacy services through medical homes and a new program providing medication therapy management (MTM) services as part of collaborative patient care and coordinated home-based care for high-need patients.10 It is expected that more patients with chronic diseases will receive pharmacist-provided MTM services under a new program established to improve quality of patient care and reduce overall treatment costs.10 This program will provide grants or contracts for pharmacists’ MTM services to collaboratively treat patients who have certain risk factors or other high-risk problems.
Health Insurance Exchange Marketplace
The Health Insurance Exchange Marketplace was established to provide an easier means of shopping for and purchasing individual and small-group health coverage.7 There are two types of federal exchanges: the Individual Marketplace and the Small Business Health Options Program (SHOP).7 The Individual Marketplace allows individuals to purchase qualified coverage. SHOP, which enables small businesses of two to 50 employees to purchase a Qualified Health Plan, will increase the number to a maximum of 100 employees on January 1, 2016.7 Self-employed individuals can participate in the Individual Marketplace. To be offered on the marketplace, health plans must be certified by the Department of Health and Human Services (HHS) and meet certain minimum standards.7 The four coverage tiers are based on the percentage of the total allowed cost of benefit paid by a health plan, on average: platinum plans cover 90%, gold plans cover 80%, silver plans cover 70%, and bronze plans cover 60%.11
Enrollment
For coverage in 2016, the open-enrollment period is October 15, 2015, through December 7, 2015, with an effective date of January 1, 2016. The Individual Marketplace may be accessed at www.healthcare.gov; the Call Center operates 7 days per week, 24 hours a day, and is closed only on Memorial Day, July 4, and Labor Day. SHOP service is available Monday through Friday from 9:00 am to 7:00 pm Eastern Standard Time.
Home-Based Care and Accountable Care Organizations
Home-based care and accountable care organizations (ACOs) are two strategies being used to improve quality of care and healthcare outcomes in high-need patients. Home-based care includes a variety of services, such as rehabilitative care and nursing care. ACOs manage and coordinate care for Medicare fee-for-service patients by meeting quality performance standards.12 One example of an effective program is the Independence at Home Medical Practice Demonstration program. This program is testing a payment incentive and service delivery model that uses home-based primary care teams.12 The Medicare Shared Savings Program was established for groups of providers and suppliers. In terms of payment reform and quality, hospitals will undergo payment adjustments for healthcare-acquired conditions, and rates will reflect whether the hospital meets performance standards. Pharmacists can serve as medication-use system experts, meet pay-for-performance measures, and prevent hospital readmissions.12
Outcomes Research
Outcomes research is the study of end results of health services, taking into account patient experiences, preferences, and values.12 Outcomes research assists patients, clinicians, purchasers, and policy makers in making informed health decisions.12 These health decisions will help prevent, diagnose, treat, monitor, and manage diseases and other health conditions, ensuring that there are enough healthcare professionals to meet patient demand and that they are trained to handle the evolving healthcare landscape. Taking advantage of these training opportunities will help pharmacists—and the health systems they work in—meet healthcare reform goals.12
Other Factors Affecting Pharmacists
The National Health Care Workforce Commission was established to evaluate education and training activities to ensure that current and future requirements of the healthcare workforce are met. Grants or contracts will be awarded to encourage health professionals to specialize in providing care to elderly patients. In addition, more types of hospitals will be eligible to receive lower outpatient drug prices under the 340B DPP.12 Expanded participation and program integrity will make medications more affordable for new and existing covered entities, and there are two ways of ensuring that affordable 340B DPPs will be used.12 The 340B DPP will expand coverage of outpatient drug costs for specific federal grantees and federally qualified healthcare look-alikes such as public or nonprofit private entities (i.e., tribal, faith-based, and community-based organizations), whereas disproportionate-share hospitals will be expanded to specialty hospitals. Specialty hospitals are primarily engaged in the care and treatment of patients with a cardiac or orthopedic condition or who are undergoing a surgical procedure. The HHS will develop a system to ensure that drug manufacturers do not overcharge for related medications.12
Medicaid Expansion
Medicaid expansion aims to extend Medicaid coverage to most low-income people. Beginning in 2014, the ACA expanded Medicaid eligibility to 138% of the federal poverty level for citizens and qualified immigrants (in 2012, $15,415 for an individual and $26,344 for a family of three).10 The government has pledged to fund 100% of Medicaid expansion costs for the first 3 years (2014-2016).13 At least 90% of these costs will be federally funded thereafter. Nearly 5 million poor, uninsured adults will fall into the coverage gap resulting from state decisions not to expand Medicaid.13
Conclusion
The ACA is designed to make healthcare coverage available to millions of Americans, and each year a new aspect of the ACA will be implemented. With an expanded role in the healthcare system, pharmacists will have opportunities to deliver more comprehensive care to the public via mechanisms such as collaborative therapy-management structures, and they also will be able to demonstrate their capability for improving health outcomes in the patients they serve. It is to be hoped that Americans will benefit from these changes to the U.S. health system over time.
REFERENCES
1. Whitehouse.gov. Health care that works for Americans. www.whitehouse.gov/healthreform/healthcare-overview#consumer-rights. Accessed September 8, 2015.
2. HHS.gov/HealthCare. Key features of the Affordable Care Act. www.hhs.gov/healthcare/facts/timeline/index.html. Accessed September 8, 2015.
3. HHS.gov/HealthCare. About the law. www.hhs.gov/healthcare/rights. Accessed September 8, 2015.
4. Sebastian C, Bailey K, Stoll K. Health Reform: Help for Americans with Pre-Existing Conditions. Washington, DC: Families USA; May 2010. Estimates on preexisting conditions prepared for Families USA by the Lewin Group.
5. HealthCare.gov. Essential health benefits. www.healthcare.gov/glossary/essential-health-benefits. Accessed September 8, 2015.
6. Whitehouse.gov. Women and families. www.whitehouse.gov/healthreform/relief-for-americans-and-businesses#women. Accessed September 8, 2015.
7. MyFloridaCFO.com. Health insurance reform & you. www.myfloridacfo.com/division/consumers/HealthReform.htm#.U_F1EYBdWur. Accessed September 8, 2015.
8. Organisation for Economic Co-operation and Development (OECD). OECD health statistics 2014. www.oecd.org/unitedstates/Briefing-Note-UNITED-STATES-2014.pdf. Accessed September 8, 2015.
9. National Center for Health Statistics. Deaths, percent of total deaths, and death rates for the 15 leading causes of death: United States and each state, 2010. www.cdc.gov/nchs/data/dvs/LCWK9_2010.pdf. Accessed September 9, 2015.
10. Holahan J, Buettgens M, Carroll C, Dorn S. The Cost and Coverage Implications of the ACA Medicaid Expansion: National and State-by-State Analysis. Washington, DC: Henry J. Kaiser Family Foundation; 2012.
11. Profile of Affordable Care Act coverage expansion enrollment for Medicaid/CHIP and the Health Insurance Marketplace. http://aspe.hhs.gov/health/reports/2014/MarketPlaceEnrollment/Apr2014/pdf/fl.pdf. Accessed September 8, 2015.
12. American Society of Health-System Pharmacists. The Patient Protection Affordable Care Act and the Health Care and Education Reconciliation Act. www.ashp.org/DocLibrary/SM2010/Health-Care-Reform-Reportsm2010.aspx. Accessed September 8, 2015.
13. Henry J. Kaiser Family Foundation. Summary of coverage provisions in the Affordable Care Act. http://kff.org/health-costs/issue-brief/summary-of-coverage-provisions-in-the-patient. Accessed September 8, 2015.
14. OECD. Health expenditure. www.oecd.org/els/health-systems/health-expenditure.htm. Accessed September 8, 2015.
15. OECD. Compare your country health profile. www.compareyourcountry.org/health?cr=oecd&lg=en&page=3. Accessed September 8, 2015.
To comment on this article, contact rdavidson@uspharmacist.com.





