US Pharm. 2013;38(2):43-60.
ABSTRACT: The most common manifestation of myocardial ischemia is stable angina pectoris. Symptoms include a pain or pressure sensation in the chest, which may radiate to the left arm, shoulder, or jaw. Symptoms occur upon exertion and emotional stress and are relieved with sublingual nitroglycerin. The goals of treatment are to reduce or eliminate symptoms and prevent complications, such as myocardial infarction, left ventricular failure, and life-threatening arrhythmias. Treatment consists of lifestyle modifications, medication therapy, and, in some cases, revascularization.
Stable angina pectoris (SAP) is the most common manifestation of myocardial ischemia. Myocardial ischemia occurs when the oxygen demand of the heart exceeds the supply. There are three factors that determine myocardial oxygen demand—heart rate, contractility, and intra-myocardial wall tension, with the latter considered the most important.1 Oxygen demand increases in response to an increase in heart rate or an increase in left ventricular preload or afterload. A higher end-diastolic volume will raise left ventricular preload, and increased systolic blood pressure and/or arterial stiffness will increase left ventricular afterload and consequently myocardial oxygen demand. Blood supply to the heart can become compromised through atherosclerotic plaque buildup and/or coronary artery spasm. Often patients will have both.2
PATHOPHYSIOLOGY
Oxygen is delivered to the heart by larger surface vessels (epicardial vessels) and intramyocardial arteries and arterioles, which branch out into capillaries. In a healthy heart, there is little resistance to blood flow in the epicardial vessels. When atherosclerotic plaques are present, blood flow is impeded, but the process of autoregulation can compensate to a degree. Autoregulation is the dilation of the myocardial vessels in response to decreased oxygen delivery. Through autoregulation, blood flow to the heart changes rapidly as a result of higher demand. The most important mediators involved in myocardial perfusion are adenosine (a potent vasodilator), other nucleotides, nitric oxide, prostaglandins, carbon dioxide, and hydrogen ions.1 Obstructions to the coronary blood flow can be fixed, as with atherosclerosis, or dynamic, as with coronary spasm. Some patients may have both characteristics, and this is termed mixed angina.2
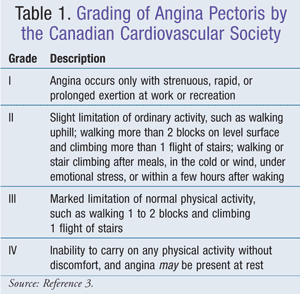
A single-cell endothelial layer separates the vascular smooth muscle from the blood. When intact, this vascular endothelium permits vasodilation and prevents thrombus and sclerotic plaque formation. The coronary artery endothelium synthesizes fibronectin, interleukin-1, tissue plasminogen activator, certain growth factors, prostacyclin, platelet-activating factor, endothelin-1, and nitric oxide (NO). NO is synthesized from L-arginine by nitric oxide synthase. NO then causes relaxation of the arterial smooth muscle. Loss of endothelial layer results in less NO and can occur because of mechanical or chemical assaults or from oxidized low-density lipoprotein (LDL). Endothelial function can be improved with angiotensin-converting enzyme inhibitors (ACEIs), statins, and exercise.1 The Canadian Cardiovascular Society developed a system of grading angina that is generally well accepted (TABLE 1).3
PROGNOSIS
Two characteristics affecting prognosis are the number of vessels obstructed and the extent of vessel obstruction. The number of vessels obstructed by atherosclerotic plaques is a strong predictor of mortality. The 12-year survival rate for patients with zero-, one-, two-, and three-vessel disease is 88%, 74%, 59%, and 40%, respectively.4 When vessels become 80% obstructed or greater, the risk of vasospasm and thrombosis is greatly increased. Other factors that impact survival are age, comorbid congestive heart failure and/or diabetes, smoking history, ejection fraction, and previous myocardial infarction (MI).1,4
SYMPTOMS
Symptoms include pain or a sensation of pressure in the chest, which may radiate to the left arm, shoulder, and jaw. The pain can last anywhere from 30 seconds to 30 minutes and is usually relieved with sublingual nitroglycerin (SLNTG). Any change in the quality, frequency, or duration of the pain or the precipitating factors suggests unstable angina, which requires immediate medical attention.1
CHRONIC STABLE ANGINA PECTORIS
Although experts cannot agree on a definition of SAP, the consensus is that symptoms should be present for at least 2 months and should not vary in severity, character, or triggering factors. The most common cause of SAP is obstructive coronary artery disease.2
SAP is characterized by chest pain that occurs upon exertion or emotional stress. The pain may radiate to the jaw, shoulder, and arm on the left side. The pain may subside with rest, or SLNTG may be needed to relieve the pain. Patients with exertional SAP often have severe anemia, hyperthyroidism, or another condition that affects the myocardial oxygen supply-demand balance.2
Typically, ischemic episodes are transient and do not result in myocardial cell death. With chronic prolonged ischemia, left ventricular dysfunction may occur, and arrhythmias can occur following an ischemic episode.1,2
Nonmodifiable risk factors include gender, age, family history, environmental factors, and comorbid diabetes. Modifiable risk factors include smoking, hypertension, dyslipidemia, obesity, a sedentary lifestyle, hyperuricemia (gout), stress, and use of progestins, corticosteroids, and calcineurin inhibitors.1
TREATMENT
The goals of treatment are to reduce or eliminate symptoms and prevent long-term complications, such as MI, left ventricular failure, and life-threatening arrhythmias. Lifestyle modifications, medications, and myocardial revascularization are all employed in the treatment of angina.2
The American College of Cardiology Foundation (ACCF) and the American Heart Association (AHA) have developed joint guidelines. The guidelines address lifestyle modifications, blood pressure control, lipid and diabetes management, and pharmacotherapy.5
Lifestyle Modifications
Smoking cessation and avoidance of secondhand smoke are strongly advised. Nicotine replacement may be used to assist in smoking cessation. SAP patients should also remain active. If individuals are healthy enough, the ACCF and AHA recommend 30 to 60 minutes of moderate-intensity exercise such as brisk walking 7 days a week (5 days minimum). The addition of strength training is reasonable if the patient’s health permits. The exercise prescription may need to be tailored based on the results of an exercise test. For high-risk patients, such as those with a recent MI, revascularization, or heart failure, a medically supervised cardiac rehabilitation is indicated.5
Weight management is strongly encouraged. The target body mass index (BMI) is between 18.5 and 24.9 kg/m2. If weight loss is necessary, the initial goal is a gradual loss of 5% to 10% of the baseline weight. If the patient succeeds with a 10% loss, further weight loss may be attempted. A waist circumference of <102 cm (40 in.) in men and <88 cm (35 in.) in women is the target. A diet high in fresh fruits, vegetables, and low-fat dairy should be adhered to. Alcohol and sodium consumption should be limited. Alcohol consumption should not exceed 1 drink a day (4 oz. of wine, 12 oz. of beer, or 1 oz. of spirits) for nonpregnant women and 1 or 2 drinks a day for men. The intake of saturated fats should not exceed 7% of the total calories, and no more than 200 mg/day of cholesterol should be consumed. Trans-fatty acids should be avoided if possible, and a minimum of 10 g/day of viscous fiber is recommended.5
Blood Pressure Control
In accordance with the Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC 7), blood pressure should be <140/90 mmHg or <130/80 mmHg for patients with diabetes or chronic kidney disease. For patients with coronary artery disease and high blood pressure, medication therapy with a beta-adrenergic antagonist (beta-blocker [BB]) or ACEI is indicated. Additional drugs may be needed to achieve target blood pressure.5
Lipid Management
LDL cholesterol (LDL-C) should be <100 mg/dL. If at baseline the LDL-C is ≥100 mg/dL, lipid-lowering medication therapy should be started. In high-risk or moderately high-risk patients, a reduction of 30% to 40% from baseline is the recommendation. If at baseline the LDL-C is 70 to 100 mg/dL, a reduction to <70 mg/dL is reasonable.5
If triglycerides (TGs) are between 200 and 499 mg/dL, the target non–high-density lipoprotein (total cholesterol minus high-density lipoprotein cholesterol [HDL-C]) is <130 mg/dL. With TGs between 200 and 499 mg/dL, lowering non–HDL-C to <100 mg/dL is reasonable. If TGs need to be lowered after LDL-C–lowering therapy is initiated, niacin or fibrate therapy is a therapeutic option. In patients with TGs ≥500 mg/dL, niacin or fibrate treatment should be started before LDL-C–lowering therapy.5
Diabetes Management
Patients with diabetes should be treated with a target hemoglobin A1c (A1C) of 7% or less. Depending on the patient’s age, history of hypoglycemia, presence of vascular complications and/or comorbidities, an A1C between 7% and 9% is reasonable. Modification of risk factors (e.g., physical activity, weight management, blood pressure control, lipid management) should be aggressively initiated and maintained. Rosiglitazone should not be initiated in diabetic patients with SAP.5
Pharmacologic Therapy
Anticoagulants/Antiplatelets: Unless contraindicated, 75 to 162 mg of aspirin daily should be initiated and continued indefinitely. If aspirin is contraindicated or not tolerated, clopidogrel may be used. Dipyridamole is not recommended for use in SAP patients. There is currently no evidence demonstrating additional benefit with anticoagulation therapy, and the use of anticoagulants is not recommended.5
Renin-Angiotensin-Aldosterone System Blockers: Patients with hypertension, diabetes, chronic kidney disease, or a left ejection fraction ≤40% should be started on an ACEI unless contraindicated. ACEIs block the conversion of angiotensin I to angiotensin II (a vasoconstrictor). Inhibition of vasoconstriction decreases both left ventricular preload and afterload.2 ACEIs may also be used on lower-risk patients. Angiotensin receptor blockers (ARBs) may be used in patients who cannot tolerate ACEIs. Combination therapy with an ACEI and an ARB is an option in patients with heart failure due to left ventricular systolic dysfunction (a reduction in left ventricular contractility).5
Beta-Blockers: Unless contraindicated, BBs should be started in all patients who have had an MI or acute coronary syndrome.5 BBs reduce oxygen demand by decreasing heart rate, blood pressure, myocardial contractility, and left ventricular afterload.1,2 These agents also improve exercise tolerance in those with exertional angina. BBs reduce silent ischemic episodes and early morning ischemia and improve mortality post-MI more effectively than nitrates and calcium channel blockers (CCBs).1 In patients with normal left ventricular function, BB therapy should be continued for 3 years. In patients with left ventricular dysfunction (ejection fraction ≤40%), BB therapy with carvedilol, metoprolol, or bisoprolol should be initiated, and long-term treatment with BBs may be considered for any patient with coronary or other vascular disease.5
Beta1-selective BBs should be used, keeping in mind that at high doses they lose their selectivity. These include metoprolol, atenolol, bisoprolol, and nebivolol.6 The third generation BBs offer additional protection. Carvedilol causes peripheral vasodilation through alpha1-adrenergic receptor blockade, and it is a good option for patients with congestive heart failure. Nebivolol has greater selectivity for the beta1 receptor than bisoprolol, metoprolol, and carvedilol. Nebivolol also induces peripheral vasodilation by stimulating the release of NO. The mechanism by which this happens is probably through beta3-receptor stimulation. This combination of beta1-receptor blockade and beta3 stimulation has been shown to increase insulin sensitivity, whereas other BBs impair insulin sensitivity.6 Nebivolol is currently indicated for hypertension only and has not been studied in patients with angina or who have had a recent MI.7
Calcium Channel Blockers: CCBs decrease oxygen demand by reducing blood pressure, contractility, and afterload.2 This is achieved through vasodilation of arterioles and the coronary arteries.1 Good candidates for CCBs are those who cannot tolerate BBs and those with variant angina or peripheral vascular disease.1,2 CCBs should be used with caution in patients with heart failure.2 The nondihydropyridine CCBs diltiazem and verapamil may be used as first-line therapy when BBs are contraindicated. CCBs may also be added to a BB regimen when there is insufficient response.5
Nitrates: Nitrates can be used for both acute attacks and for prophylaxis.1 They reduce oxygen demand through vasodilation and reduced left ventricular preload.2 SLNTG provides symptomatic relief to approximately 75% of patients within 3 minutes. The dosage is 0.3 or 0.4 mg. The patient should sit when taking SLNTG. If there is no relief after 5 minutes, the dose should be repeated up to a maximum of three tablets. If after 15 minutes the patient continues to experience pain, he or she should seek immediate medical attention. SLNTG can also be used prophylactically when the patient anticipates symptoms upon exertion. The patient should take it 5 to 10 minutes prior to activity, and it will last approximately 30 to 40 minutes. Adverse effects of SLNTG include postural hypotension, headaches, flushing, reflex tachycardia, and occasionally nausea. The patient should be counseled to keep sublingual tablets in their original container to preserve potency and to replace them after 6 to 12 months.5
Since nitroglycerin has a half-life of 1 to 5 minutes, sustained-release formulations are needed for prophylaxis.1 These longer-acting formulations may also increase exercise tolerance.2 Sustained-release nitrates are good for patients whose angina is characterized by vasospasm. They are usually given with a BB when monotherapy is insufficient. They may also be an option if the patient cannot tolerate a BB.1 Since tolerance develops with prolonged nitrate use, patients should have an 8- to 12-hour nitrate-free period every 24 hours.2
Ranolazine: Ranolazine was approved in January 2006 for the treatment of chronic angina. Current guidelines recommend ranolazine therapy in place of a BB when BBs are contraindicated or not tolerated. Ranolazine can also be added to a BB when BB monotherapy is insufficient.5 Ranolazine does not lower blood pressure or heart rate; it inhibits the late sodium current, thereby reducing intracellular sodium and calcium accumulation.8
There are two phases to the sodium influx during the ventricular action potential—a stronger phase that lasts only a few milliseconds and a weaker phase that lasts hundreds of milliseconds. This final weak phase is called the late sodium current. Even though the sodium flow of the late sodium current is very weak—only 1% to 2% of the early phase, since it lasts 50 to 100 times longer—the total sodium influx of the two phases is nearly equal. By reducing the late sodium current, approximately half of the total sodium loading is decreased.9
A greater influx of sodium results in intracellular calcium overload because of an increased influx of calcium through the sodium-calcium exchange. Angina is often associated with increases in intracellular sodium, thus resulting in increases in intracellular calcium. Calcium overload of myocardial cells is associated with an increase in oxygen demand and electrical instability.10 Ultimately, myocardial cell injury and death may occur.1 By inhibiting the late sodium current, ranolazine increases oxygen supply and reduces oxygen demand.2 Ranolazine is also associated with small decreases in A1C, though it should not be considered a treatment for diabetes.8
Ranolazine should be used as second-line treatment for angina when other medications are inadequate.1 Because ranolazine is mainly metabolized by CYP3A, it should not be given with potent CYP3A inhibitors (e.g., ketoconazole, clarithromycin, nefazodone, ritonavir, or nelfinavir) or inducers (e.g., rifampin, phenobarbital, carbamazepine, phenytoin, or St. John’s wort). Ranolazine is also contraindicated in patients with liver cirrhosis. QT-interval prolongation may occur while taking ranolazine. Common adverse reactions include dizziness, headache, nausea, and constipation.8
CONCLUSION
SAP results from an imbalance of myocardial oxygen supply and demand. SLNTG is used for acute attacks or for prophylaxis of expected exertional symptoms. Important counseling points include the appropriate use of SLNTG (e.g., remain seated while and immediately after taking it), the need to store it in its original container, and the need to seek medical attention if no symptomatic relief is achieved after three tablets in 15 minutes.
The pharmacist should counsel patients on the use of prophylactic medications. Patients should be warned that these drugs do not arrest an acute attack, and they should have SLNTG on them at all times. Replacing SLNTG every 6 to 12 months is critical, and patient adherence should be monitored. Patients need to be educated on modifiable risk factors, including smoking cessation, greater physical activity, and the importance of treating hypertension, dyslipidemia, and diabetes. The pharmacist should also recommend an annual influenza vaccination to all SAP patients per current ACCF/AHA guidelines.5
REFERENCES
1. Talbert RL. Chapter 23. Ischemic heart disease. In: Talbert RL, DiPiro JT, Matzke GR, et al, eds. Pharmacotherapy: A Pathophysiologic Approach. 8th ed. New York, NY: McGraw-Hill; 2011.
2. Kaski J, Arrebola-Moreno A, Dungu J. Treatment strategies for chronic stable angina. Expert Opin Pharmacother. 2011;12:2833-2844.
3. Campeau L. Grading of angina pectoris [letter]. Circulation. 1976;54:522-523.
4. Emond M, Mock MB, Davis KB, et al. Long-term survival
of medically treated patients in the Coronary Artery Surgery Study
(CASS) registry. Circulation. 1994;90:2645-2657.
5. Fihn S, Gardin J, Abrams J, et al. 2012
ACCF/AHA/ACP/AATS/PCNA/SCAI/STS guideline for the diagnosis and
management of patients with stable ischemic heart disease: a report of
the American College of Cardiology Foundation/American Heart Association
Task Force on Practice Guidelines, and the American College of
Physicians, American Association for Thoracic Surgery, Preventive
Cardiovascular Nurses Association, Society for Cardiovascular
Angiography and Interventions, and Society of Thoracic Surgeons. Circulation. 2012;126:e354-e471.
6. Kamp O, Metra M, Bugatti S, et al. Nebivolol:
haemodynamic effects and clinical significance of combined beta-blockade
and nitric oxide release. Drugs. 2010;70:41-56.
7. Bystolic (nebivolol) package insert. St. Louis, MO: Forest Pharmaceuticals, Inc; June 2011.
8. Ranexa (ranolazine) package insert. Foster City, CA: Gilead Sciences, Inc; December 2011.
9. Noble D, Noble P. Late sodium current in the
pathophysiology of cardiovascular disease: consequences of
sodium-calcium overload. Heart. 2006;92(suppl 4):iv1-iv5.
10. Belardinelli L, Shryock J, Fraser H. Inhibition of the
late sodium current as a potential cardioprotective principle: effects
of the late sodium inhibitor ranolazine. Heart. 2006;92(suppl 4):iv6-iv14.
To comment on this article, contact rdavidson@uspharmacist.com.





