US Pharm. 2009;34(6):44-47.
With the introduction of the Beers Criteria, there has been a virtual explosion of literature regarding the inappropriate use of medications in older adults. The Beers Criteria focus on prescription medications, with only a few OTC medications being addressed (diphenhydramine, mineral oil, cimetidine).1 However, this provides little guidance for practitioners when making recommendations with respect to appropriate medications, particularly among many available OTC products.
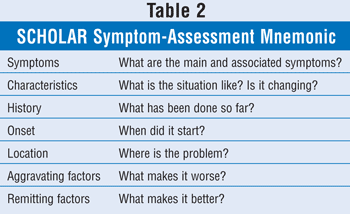
Older adults generally have more medical problems and use more medications, both prescription and OTC, when compared to younger adults. Many older adult patients self-treat using OTC medications. Older adults account for about 13% of the United States population and purchase 40% of all OTCs consumed.2 Pharmacists, as one of the most accessible health care providers, have an opportunity to assist these patients when making decisions in the OTC aisle. As the baby boomers age, there will be even more opportunities for pharmacists to assist older adults with making appropriate OTC medication choices. To do this successfully, it is essential for pharmacists to be able to evaluate and assess patient symptoms. One quick and effective method for determining the needs of patients and to see if they are candidates for self-care is the QuEST/SCHOLAR process.3,4 QuEST is a mnemonic for assessing and counseling the patient (TABLE 1). SCHOLAR is a mnemonic to assist with symptom assessment (TABLE 2). The purpose of this article is to provide the practicing pharmacist with a review of various OTC options, for some of the more common medical problems or disease states, that are generally safe for older adults.

Allergy
Allergic rhinitis has an estimated prevalence of between 9% and 40% in the U.S. adult population.5 It can be seasonal if occurring only during certain parts of the year, or perennial if symptoms occur year round. Mild-to-moderate symptoms are most often treated with antihistamines and decongestants. Cromolyn sodium is an intranasal mast cell stabilizer that prevents the release of histamine and other mediators of allergic rhinitis. The nasal spray is approved for the treatment and prevention of seasonal and perennial allergic rhinitis symptoms such as sneezing and runny, stuffy, and itchy noses. As a topical nasal spray, it exhibits a local effect with minimal systemic absorption. The most common adverse effects relate to the local action and include sneezing and nasal stinging and burning. Since it exerts only a local effect, no drug interactions are reported. No dosage adjustments are needed for renal or hepatic impairment. The minimal adverse effects and no drug interactions therefore make cromolyn sodium a good choice for treating allergic rhinitis in older adults.
Ketotifen is an ocular antihistamine, mast cell stabilizer, and eosinophil inhibitor that prevents the release of histamine and other mediators of allergic conjunctivitis. The ophthalmic solution is approved for the prevention of ocular itching due to allergic conjunctivitis. Previously available only by prescription, ketotifen is now available OTC. Most of the OTC eye drops contain an antihistamine and a decongestant to treat the itching and redness associated with allergic conjunctivitis. Ocular decongestants have the same problem of rebound congestion as the nasal decongestants. As a result, patients should be counseled not to use the products longer than 3 to 5 days consecutively. Ketotifen is not a decongestant and therefore does not have the rebound congestion problem. As a topical ophthalmic solution, it exhibits a local effect with minimal systemic absorption. The most common adverse effects include conjunctiva congestion, headache, and rhinitis. No systemic drug interactions have been reported with ketotifen since it has only a local effect. No dosage adjustments are needed for renal or hepatic impairment. The lack of rebound congestion and lack of reported drug interactions make ketotifen a good choice for treating allergic conjunctivitis in older adults.
Loratadine is a second-generation oral antihistamine. It is approved for the relief of seasonal and perennial allergic rhinitis symptoms, such as sneezing, itching, and rhinorrhea. As a large protein-bound lipophobic molecule with charged side chains, it does not cross the blood-brain barrier easily. This is what accounts for the lack of sedating effects. Unlike the sedating, first-generation antihistamines, loratadine does not activate alpha-adrenergic receptors or block cholinergic receptors. Therefore, it does not produce substantial anticholinergic adverse effects such as dry mouth, dry eye, urinary retention, and constipation, which are commonly seen with the sedating antihistamines. Older adults are also more susceptible to the cognitive side effects associated with antihistamines having anticholinergic effects. The lack of sedating and anticholinergic effects makes loratadine one of the better choices for treating allergic rhinitis in older adults.
Patients with more severe symptoms or with symptoms that do not resolve with a trial of OTC medications should be referred to their primary care provider (PCP). Patients should also be referred to their PCP if sinusitis is suspected.
The Common Cold
The common cold, which is caused by rhinoviruses or coronoviruses, cannot be cured with any available drug therapies at this time. As a result, recommended treatments are primarily symptomatic. The most common symptoms include sore throat, runny nose, congestion, sneezing, coughing, muscle aches, and fatigue. Although there is an abundance of OTC products available to treat cold symptoms, most products contain combinations of antihistamines, decongestants, expectorants, and cough suppressants. Many of these medications may not be appropriate for patients who have other medical problems (hypertension, diabetes) or take other medications.
Oxymetazoline is an alpha-adrenergic receptor agonist available as a nasal spray. It causes vasoconstriction of the mucous membranes resulting in decreased nasal mucosa edema. This promotes drainage and improves breathing. The nasal spray is approved for relief of stuffy nose symptoms associated with the common cold, sinusitis, hay fever, and nonseasonal, seasonal, and perennial allergic rhinitis. When administered intranasally, it exhibits a local effect with minimal systemic absorption. Unlike oral decongestants that can increase blood pressure, the topical decongestants do not have this effect; therefore, patients who are taking blood pressure-lowering medication would not need to worry about oxymetazoline raising their blood pressure. The most common adverse effects relate to the local action and include nasal stinging and burning, dryness, and sneezing. The use of oxymetazoline can result in rebound nasal congestion, so patients should be counseled not to use the product longer than 3 to 5 days consecutively. It has only a local effect, so little to no drug interactions are suspected. No dosage adjustments are needed for renal or hepatic impairment. Minimal adverse effects and no drug interactions make oxymetazoline a good choice for the short-term treatment of nasal congestion symptoms associated with the common cold in older adults.
In older adults, viral infections can increase the risk of developing secondary bacterial infections, such as bronchitis, pneumonia, or sinusitis. If one of these is suspected, patients should be referred to their PCP.
Osteoarthritis
Osteoarthritis affects nearly 50 million adults in the U.S., and the prevalence increases substantially with age.6 Pain due to osteoarthritis is one of the most common medical complaints among older adults.7 Limitations in physical activity and physical functioning are strongly associated with pain symptoms in osteoarthritis. Acetaminophen is a centrally acting analgesic. It is approved for the treatment of mild pain, fever, osteoarthritis, and migraine headaches. It is also approved for the temporary relief of headache, myalgia, back pain, dental pain, dysmenorrhea, arthralgia, or minor aches and pain associated with the common cold or influenza. Acetaminophen is the drug of choice for osteoarthritis when there is little to no inflammation involved. The American College of Rheumatology recommends acetaminophen as the first-line treatment option for osteoarthritis of the hip and knee.8 Compared to the alternative OTC pain relievers, nonsteroidal anti-inflammatory drugs (NSAIDs), acetaminophen has a more favorable adverse-effect profile. Older adults are at increased risk for the renal dysfunction, gastrointestinal irritation and bleeding, and exacerbations of hypertension that NSAIDs can cause. Acetaminophen's adverse effects are mainly seen at high doses used long-term or when the medication is used inappropriately (overdose). Acetaminophen should be used with caution in patients with hepatic impairment or history of alcohol use/abuse. It is the drug of choice for pain relief in patients with renal impairment, but dosage titration based on clinical effect is encouraged. When used as directed in doses not exceeding 4 g per day, acetaminophen is a safe and effective pain reliever for older adults. Despite its relative safety, some older patients may not get adequate analgesic effects from acetaminophen because of age-related changes in gastric motility, disease-related changes such as diabetic gastroparesis, or anticholinergic drug effects. Acetaminophen is primarily absorbed in the small intestine, and delayed presentation of the drug to the site of absorption may lead to inadequate analgesic effects.
Although not a pharmacologic agent, continuous low-level heat wrap therapy products are available in the OTC pain relief aisle. Low-level heat wrap therapy is approved for the treatment of arthritis and muscle pain. Low-level heat helps to relax sore and tight muscles, increasing flexibility and range of motion.9 With one application, the wraps provide heat for 8 to 12 hours. On the other hand, topical treatments such as counterirritants require application three to four times daily to maintain pain relief. Counterirritants, available as creams and ointments, can be messy, greasy, and are generally not acceptable to patients for long-term use. The heat wraps contain no medication, so there are no drug interactions and no dosage adjustments are required for renal or hepatic impairment. Neither heat nor occlusive dressings should be used in combination with other topical analgesics. Using the combination can increase the risk of systemic side effects. Low-level heat wraps provide a safe and effective alternative to OTC pain relief medications as well as an adjunct to oral therapy for older adults.
Heartburn
Heartburn and gastroesophageal reflux are very common symptoms in adults in the U.S., with an estimated 10% to 20% of adults having reflux symptoms on a weekly basis.10 Repeated exposure of the esophagus to refluxed stomach contents can lead to inflammation and erosions. However, for many patients, lifestyle changes and use of OTC acid-blocking medications can control symptoms and prevent complications of esophagitis.11 Famotidine and nizatidine, as histamine2-receptor antagonists, decrease gastric acid by blocking the effect of histamine on gastric cell receptors. They are approved for the prevention and treatment of mild-to-moderate, infrequent heartburn associated with acid indigestion or sour stomach. One dose taken 1 hour prior to anticipated heartburn or at the onset of heartburn can provide relief for up to 12 hours. This is useful for patients who experience heartburn at night. Histamine2-receptor antagonists in general have a low incidence of adverse effects. Famotidine and nizatidine are not metabolized by the CYP450 system and, therefore, lack the drug interactions commonly seen with cimetidine. Ranitidine is metabolized by the CYP450 system, but to a lesser extent than cimetidine, so drug interactions are possible but are not seen clinically with OTC doses. The main drug interactions reported with famotidine and nizatidine are related to their acid-lowering effects. Medications that require an acidic environment to be absorbed, such as ketoconazole and itraconazole, will have reduced bioavailability. Dosage adjustments are needed for patients with renal impairment but not with hepatic impairment. The limited adverse effects and minimal drug interactions associated with famotidine and nizatidine make these two histamine2-receptor antagonists, with dosage adjustments as needed, a good choice for patients with heartburn.
Omeprazole, as a proton pump inhibitor, decreases gastric acid by inhibiting acid secretion. It is approved for the treatment of frequent heartburn in patients experiencing symptoms 2 or more days per week. Omeprazole is not indicated for immediate relief of infrequent heartburn, and it may take up to 4 days for the full benefit to be seen. Omeprazole is taken once daily 30 minutes prior to the morning meal for 14 days and can be repeated after 4 months if symptoms return, or as directed by a physician. If heartburn symptoms persist or return before the 4-month time period, the patient should be instructed to consult with a physician. Omeprazole has a low incidence of adverse effects. No dosage adjustments are required for renal impairment, but dosage reductions are recommended for patients with severe hepatic impairment. One caution for pharmacists and something that patients should be aware of relates to drug interactions. Omeprazole has the same interaction as the histamine2-receptor antagonists with regard to lower bioavailability of medications that require an acidic environment. Also, omeprazole is an inhibitor of the CYP450 system and therefore will interact with other medications metabolized by this system.
Patients who have frequent symptoms or symptoms that do not respond to OTC medications or who experience what is termed alarm symptoms (continual pain, chest pain, dysphagia, odynophagia, weight loss, or choking) should be referred to their PCP.11
Constipation
Constipation is a common problem among older adults, and many patients choose to initiate self-treatment. Although it is often considered a fairly benign issue, constipation not appropriately addressed can lead to bowel obstruction and hospitalization. Constipation is defined on the basis of stool frequency, stool consistency, and difficulty passing stools.12,13 In the U.S., insufficient dietary fiber is a frequent underlying issue for many patients with constipation. Commonly used medications are also associated with constipation, including opiate analgesics, anticholinergics, and calcium or iron products. General nondrug approaches to improving constipation include dietary fiber (at least 10 g daily of crude fiber), adequate fluid intake, and exercise. Fruits, vegetables, and cereals are among the best foods to increase dietary fiber intake. There are numerous OTC medications to treat constipation, but not all are appropriate in all situations. For patients who have symptoms of obstruction (nausea, vomiting, abdominal pain or distention) or fecal impaction, OTC treatments should not be recommended, and these patients should be referred to their PCP for evaluation or disimpaction prior to the use of oral laxative agents.
Bulk-forming laxatives, including psyllium and methylcellulose, can be used to supplement dietary fiber if patients do not have adequate intake of dietary fiber. Bulk-forming laxatives are generally safe since they are not systemically absorbed. However, these agents must be taken with adequate fluid to prevent intestinal obstruction. Bulk-forming agents can be useful for ongoing treatment and for preventing chronic constipation. These agents are not optimal for patients who have acute constipation, as they can take several days to produce the desired effect. Some patients may experience abdominal distention and flatus with increases in dietary fiber, but these symptoms typically decline over time.
Emollient laxatives, such as docusate sodium, are not exceptionally effective for treating constipation but may be useful in situations where straining during defecation should be avoided, such as with hemorrhoids or following rectal surgery or a myocardial infarction.
Polyethylene glycol 3350 is an osmotic laxative that is generally safe to use for older patients with constipation. It does not cause electrolyte disturbances, as can be seen with other saline-type osmotic laxatives, including magnesium citrate or sodium phosphate. As a result, polyethylene glycol-containing products are safer for patients with significant renal dysfunction or with congestive heart failure. The laxative works by osmotic action and retention of fluid in the gastrointestinal tract, which leads to softening of the stool. Unlike some of the saline-type osmotic laxatives, which work quickly (hours), polyethylene glycol takes slightly longer to produce the desired effect (1 to a few days).
Acute constipation can be relieved with the use of glycerin suppositories. Glycerin is considered very safe, and the onset of action is usually less than 30 minutes. Occasionally, patients may experience mild rectal irritation.
Insomnia
Complaints regarding sleep increase dramatically with advancing age. Aging is associated with changes in sleep architecture, including decreased sleep efficiency, total sleep time, and restful sleep stages.14 Numerous factors can also impact sleep, such as pain, urinary symptoms associated with benign prostatic hyperplasia or overactive bladder, restless legs syndrome, sleep apnea, issues with sleep hygiene, or side effects of medications. It is very important to look for underlying causes of sleep problems before initiating medications to treat sleep symptoms. Improving sleep hygiene and healthy sleep habits (limit napping, avoid late-day exercise, avoid late-day caffeine and fluid intake, etc.) are also important to consider prior to initiating medications for sleep.15
Many OTC sleep products contain sedating antihistamines, such as diphenhydramine. These products are generally not recommended for older adults because of the anticholinergic side effects. The food supplement melatonin has been advocated for sleep in older adults, since aging has been associated with a decrease in this natural hormone secreted by the pineal gland.16 Supplementation with melatonin in older adults with low levels of melatonin does improve sleep efficiency.17 There have been several studies of melatonin in elderly patients with insomnia, but most have been small and the melatonin products have been varied, including both controlled-release and immediate-release products in dosages ranging from 0.5 mg to 6 mg dosed at bedtime.18,19 One study also showed improvements in sundowning symptoms in patients with dementia and agitated nighttime behaviors.19 Melatonin is considered fairly safe, and reported side effects have been minimal in the available published studies.
REFERENCES
1. Fick DM, Cooper JW, Wade WE, et al. Updating the Beers Criteria for potentially inappropriate medication use in older adults. Arch Int Med. 2003;163:2716-2724.
2. Berardi RR, Kroon LA, McDermott JH, et al. Handbook of Nonprescription Drugs: An Interactive Approach to Self-Care. 15th ed. Washington DC: American Pharmacist Association; 2006:5.
3. Han, PK, Leibowitz K, Meldrum H. Assisting self-treating patients quickly and effectively. In: Partners in Self-care: A Continuing Education Monograph Series for Pharmacists. Vol 7. Washington, DC: American Pharmacists Association; 2003.
4. Wheeler SQ, Windt JH. Telephone Triage: Theory, Practice and Protocol Development. Albany, NY: Delmar Publishers, Inc; 1993.
5. Plaut M, Valentine MD. Allergic rhinitis. N Engl J Med. 2005;353:1934-1944.
6. Hootman JM, Helmick CG. Projections of U.S. prevalence of arthritis and associated activity limitations. Arthritis Rheum. 2006;54:226-229.
7. AGS Panel on Persistent Pain in Older Persons. The management of persistent pain in older persons. J Am Geriatr Soc. 2002;50(suppl 6):S205-S224.
8. American College of Rheumatology Subcommittee on Osteoarthritis Guidelines. Recommendations for the medical management of osteoarthritis of the hip and knee: 2000 update. Arthritis Rheum.
9. McCarberg W, Erasala G, Goodale M, et al. Therapeutic benefits of continuous low-level heat wrap therapy for osteoarthritis of the knee. The Journal of Pain. 2005;6:S53.
10. Dent J, El-Serag HB, Wallander MA, Johansson S. Epidemiology of gastro-esophageal reflux disease: a systematic review. Gut. 2005;54:710-717.
11. DeVault KR, Castell DO. Updated guidelines for the diagnosis and treatment of gastroesophageal reflux disease. Am J Gastroenterol. 2005;100:190-200.
12. Koch A, Voderholzer WA, Klauser AG, Muller-Lissner S. Symptoms in chronic constipation. Dis Colon Rect. 1997;40:902-906.
13. Romero Y, Evans JM, Fleming KC, Phillips SF. Constipation and fecal incontinence in the elderly population. Mayo Clin Proc. 1996;71:81-92.
14. Vitiello MV. Sleep disorders and aging: understanding the causes. J Gerontol.
15. Marin J, Shochat T, Ancoli-Israel S. Assessment and treatment of sleep disturbances in older adults. Clin Psychol Rev. 2000;20:783-805.
16. Haimov I, Laudon M, Zisapel N, et al. Sleep disorders and melatonin rhythms in elderly people. Br Med J. 1994;309:167.
17. Haimov I, Lavie P, Laudon M. Melatonin replacement therapy of elderly insomniacs. Sleep.
18. Garfinkel D, Laudon M, Nof D, Isapel N. Improvement of sleep quality in elderly people by controlled-release melatonin. Lancet. 1995;346:541-544.
19. Fainstein I, Bonetto AJ, Brusco LI, Cardinali DP. Effects of melatonin in elderly patients with sleep disturbances: a pilot study. Curr Therapeutic Research. 1997;58:990-1000. 2000;43:1905-1915. 1997;52A:M189-M191. 1995;18:598-603.
To comment on this article, contact rdavidson@jobson.com.






