US Pharm. 2023;48 [ePub September 19, 2023].
ABSTRACT: Early detection and management of thyroid disorders in the pediatric population is vital for optimal growth and development. Pharmacists play a critical role in identifying patients at risk, understanding risk factors, signs and symptoms, and interpreting laboratory results. Long-term medication therapy is standard in treatment for most thyroid disorders. Regular communication and counseling between the pharmacist and caregivers on medication regimens, nutrition, and follow-up screenings is critical to optimize patient health outcomes and overall well-being.
Congenital hypothyroidism, defined as thyroid hormone deficiency present at birth, has been observed in approximately one out of every 3,000 to 4,000 newborns in the United States1,2 Prevalence is higher in Hispanic and Asian infants, female births, multiple births, and preterm infants.2 Acquired hypothyroidism, which develops later in a child’s life, is commonly caused by Hashimoto’s disease. This condition is characterized by an autoimmune response in which the immune system generates antibodies that target the thyroid gland. The accumulation of white blood cells within the thyroid gland leads to its impairment and subsequent insufficiency in the production of thyroid hormones.1
In contrast, hyperthyroidism is characterized by excessive production of thyroid hormones by the thyroid gland. It occurs in approximately one out of every 5,000 children and adolescents.3 It can oftentimes be attributed to the autoimmune disorder Graves’ disease. Research findings indicate that neonatal Graves’ disease is the predominant cause of hyperthyroidism among neonates. The thyroid-stimulating antibodies responsible for Graves’ disease are transmitted from the mother to the child. Neonatal Graves’ disease typically resolves subsequent to the clearance of maternal antibodies from the infant’s bloodstream. Both pharmacologic and nonpharmacologic interventions can effectively manage the disorder.4
Thyroid Function
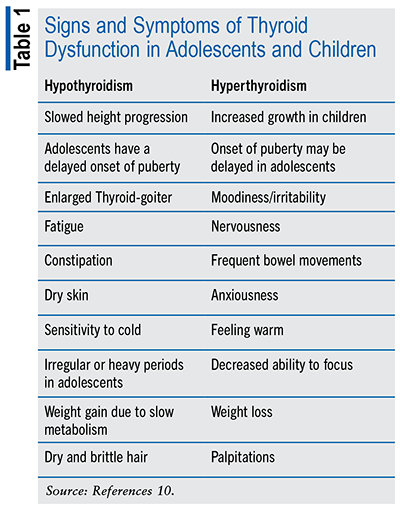
The thyroid gland plays a crucial role in the endocrine system by regulating and synthesizing thyroid hormones. The thyroid gland is responsible for the production of iodothyronines, specifically T4 (thyroxine) and T3 (triiodothyronine), which are the inactive and active forms of the hormone, respectively. Consequently, a significant proportion of the hormone generated is rendered inactive, with a mere 10% present in its active state. While the hormone remains inactive, it has the potential to undergo conversion into either an alternative inactive thyroid hormone or an activated hormone. Type 1 deiodinase facilitates the conversion of T4 into T3. This process allows for the regulation of thyroid hormone homeostasis and facilitates the targeted signaling of T3 between hormonal levels and tissue response. The function of T3 is to enhance the metabolic rate and protein synthesis processes within the human body.5 Dysfunction of the thyroid gland can result in signs of either hypothyroidism or hyperthyroidism. Hypothyroidism symptoms include bradycardia, increased sensitivity to cold temperatures, and weight gain. Conversely, hyperthyroidism may cause symptoms of weight loss, frequent bowel movements, and muscle weakness.6 (See TABLE 1.)
Thyroid Disorder Causes
Multiple risk factors are associated with the development of thyroid disorders in individuals. These factors encompass a wide spectrum, including family history, dietary habits, and gender. The presence of a thyroid disorder in a first-degree family member is considered a significant risk factor. In addition, the female population exhibits a higher susceptibility to the development of Graves’ disease or Hashimoto’s disease. Additional factors, such as inadequate or excessive iodine intake and exposure to radiation in the neck region, are associated with an increased risk of developing thyroid dysfunction.
Diagnosis and Management
Early diagnosis and treatment are paramount for optimal neurodevelopmental outcomes in this patient population. Diagnosis is determined by means of a thyroid-stimulating hormone (TSH) assay, which indicates whether TSH levels are elevated or reduced. Elevated levels of TSH are indicative of hypothyroidism. The typical range of TSH values for children aged 6 to 10 years is 0.8 mU/L to 6.0 mU/L. The diagnosis of hyperthyroidism is indicated by low levels of TSH, which is a consequence of excessive thyroid hormone production.7 A repeat TSH test is conducted to verify the underlying diagnosis. In specific circumstances, it was observed that patients who were pregnant or using oral contraceptives exhibited a slight increase in their thyroid hormone levels. Likewise, individuals who were taking corticosteroids exhibited reduced levels of T4. Various factors can impact TSH levels, thereby necessitating follow-up testing and comprehensive review of the patient’s medical history to ensure an accurate diagnosis.
Thyroid antibody tests are also valuable in the diagnosis of autoimmune disorders like Graves’ disease and Hashimoto’s disease. Following the onset of autoimmune thyroiditis, the thyroid gland becomes the target of the immune system, leading to the production of thyroid antibodies. Imaging, such as an ultrasound, allows practitioners to identify the malignancy status of thyroid nodules. In cases where a healthcare practitioner suspects the presence of a lump, a biopsy is typically performed as a means of conducting a more comprehensive examination. The thyroid scan is an alternative examination that facilitates healthcare practitioners in assessing the morphology and dimensions of the thyroid gland to determine the etiology of hyperthyroidism. This procedure utilizes radioactive iodine. It is recommended to abstain from consuming iodine-rich foods for a week before undergoing the scan to prevent any potential discrepancies in the results. Finally, the radioactive iodine uptake test is utilized to assess thyroid function and identify the etiology of hyperthyroidism. The objective of this test is to measure the ability of the thyroid gland to absorb iodine from the bloodstream for the production of thyroid hormones. Substantial uptake of radioactive iodine by the thyroid gland is indicative of Graves’ disease.8
Nutrition
Iodine deficiency is a major factor contributing to the development of hypothyroidism, as the proper functioning of the thyroid gland is dependent on the availability of iodine in the body. Since the human body is incapable of endogenously synthesizing iodine, it is important to obtain this essential element from a diverse range of dietary sources. Several sources of iodine include seaweed; shellfish; dairy products; eggs; iodized table salt; saltwater fish like cod, salmon, tuna, and sardines; and multivitamins that contain iodine. It has been reported that Kosher salt and noniodized table salt lack iodine content and, therefore, are not advisable for use in this patient cohort. To prevent iodine deficiency, it is imperative to ensure that the patient’s dietary intake of iodine is adequate. Individuals with hypothyroidism should consume adequate amounts of iodine; however, it is also essential to avoid excessive intake beyond the recommended dosage. Additionally, regular laboratory tests are necessary to monitor iodine levels in such patients. Excessive iodine is discouraged in hyperthyroid patients as it can exacerbate their condition.9
Treatment
Thyroid disorders typically require long-term to lifelong medication therapy. The standard approach for managing individuals with hypothyroidism involves the administration of levothyroxine (T4) replacement therapy. Levothyroxine works by acting as a synthetic version of thyroxine, which binds to thyroid receptor proteins located within the cell nucleus. This binding process effects DNA transcription and leads to an increase in metabolism through increased protein synthesis and gluconeogenesis. Initial levothyroxine dosage is based on the child’s body weight (kg) and age and titrated according to thyroid function tests results. Dosage adjustments are most frequently required throughout the child’s growth and development and when fluctuations in metabolism occur. Regular monitoring of laboratory results and dose adjustments is important, particularly in neonates. According to the FDA, it is recommended to administer levothyroxine at the full daily dosage. Newborns should be initiated on a low dose, particularly if they have an increased risk of cardiac failure.10 Laboratory testing should be conducted every 1 to 2 months until they reach age 6 months. It is recommended that they have a check-up every 2 to 4 months until age 3 years and assessed every 3 to 12 months until the child reaches full growth and has undergone puberty.
Hyperthyroidism is treated by reducing the amount of thyroid hormone produced. The most common form of therapy is anti-thyroid medication. Alternative treatments include thyroid surgery or radioactive iodine abscission.11 Graves’ disease is not likely to resolve on its own, thus patients will need either abscission or thyroid surgery. The only anti-thyroid medication that is approved for use in children and adolescents in the United States is methimazole.
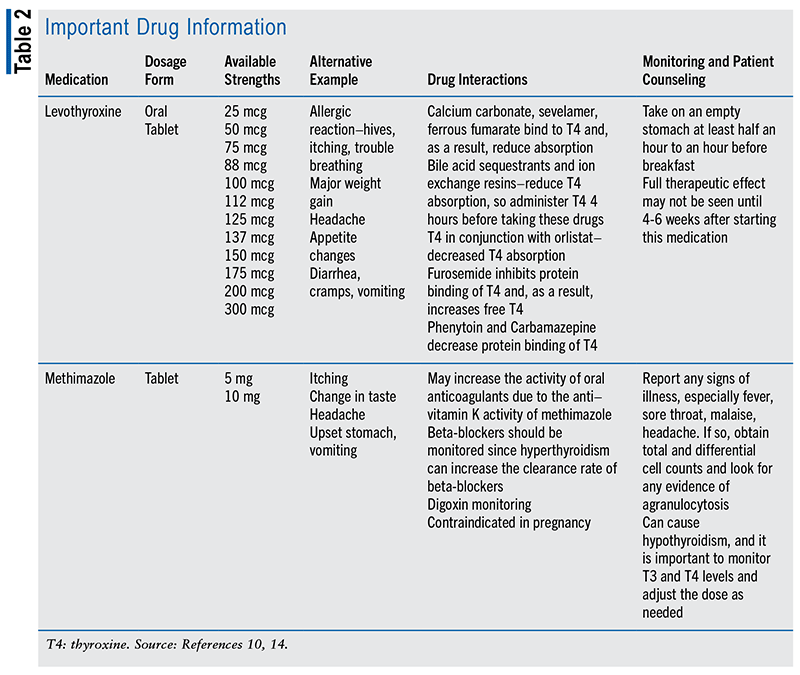
Methimazole interferes with the first step in thyroid hormone biosynthesis and acts as a substrate for thyroid peroxidase. It also inhibits iodide from absorbing into thyroglobulin.12 The initial dose is 0.4 mg/kg of body weight divided into three dosages administered every 8 hours. The maintenance dose is approximately half of the initial dose. Methimazole is available in 5-mg and 10-mg tablets. Radioactive iodine is not recommended in children aged younger than 10 years who have uncontrolled hyperthyroidism. A thyroidectomy is recommended in patients aged between 5 and 10 years who present with a goiter, uncontrolled hyperthyroidism, or who want an immediate cure. (See TABLE 2.)
The Pharmacist’s Role
Pharmacists are integral in the management of patients diagnosed with thyroid disorders. The ability to identify signs and symptoms indicating thyroid dysfunction is a crucial skill for pharmacists. Among the various thyroid disorders, hyper- and hypothyroidism are the prevailing conditions. Pharmacists can ensure the appropriate administration of medication dosage and regimen to patients, as well as assist them in monitoring for any medication-related signs or symptoms. In addition, pharmacists possess the ability to provide guidance to patients regarding appropriate dietary practices that may aid in the optimization of iodine consumption. Providing guidance to patients regarding the significance of adhering to medication regimens is essential to optimize treatment outcomes.
Conclusion
Early detection is key for thyroid disorders among pediatric and adolescent populations. Examination of the thyroid should therefore be incorporated into regular physical examinations. The identification of signs and symptoms, evaluating diet, and assessing thyroid function tests will help guide treatment regimens and allow patients to effectively experience uninterrupted healthy and productive lives. Pharmacists possess the skills necessary to differentiate between the various thyroid disorders and, subsequently, can assist in determining appropriate courses of treatment. By understanding these factors, pharmacists can effectively educate patients and caregivers, enabling them to manage symptoms and comprehend the significance of adhering to diverse treatment regimens in conjunction with specific dietary requirements.
REFERENCES
1. Johns Hopkins Medicine. Hypothyroidism in children. January 27, 2020. www.hopkinsmedicine.org/health/conditions-and-diseases/hypothyroidism-in children. Accessed May 16, 2023.
2. Bowden SA, Goldis M. Congenital hypothyroidism. [Updated 2023 Feb 26]. In: StatPearls [Internet]. Treasure Island, FL: StatPearls Publishing; 2023. www.ncbi.nlm.nih.gov/books/NBK558913/.
3. Boston Children’s Hospital. Hyperthyroidism. www.childrenshospital.org/conditions/hyperthyroidism. Accessed May 18, 2023.
4. National Institute of Diabetes and Digestive and Kidney Diseases. Hyperthyroidism (overactive thyroid). www.niddk.nih.gov/health-information/endocrine-diseases/hyperthyroidism#what-is. Accessed May 16, 2023.
5. Armstrong M, Asuka E, Fingeret A. Physiology, thyroid function. [Updated 2023 Mar 13]. In: StatPearls [Internet]. Treasure Island, FL: StatPearls Publishing; 2023 Jan-www.ncbi.nlm.nih.gov/books/NBK537039/.
6. NIH MedlinePlus. Hypothyroidism vs. hyperthyroidism. https://magazine.medlineplus.gov/article/hypothyroidism-vs-hyperthyroidism-whats-the-difference. Accessed May 16, 2023.
7. UpToDate. Normal ranges for thyroid function tests. www.uptodate.com/contents/image?imageKey=PEDS%2F60095. Accessed May 16, 2023.
8. National Institute of Diabetes and Digestive and Kidney Diseases. Thyroid tests. www.niddk.nih.gov/health-information/diagnostic tests/thyroid. Accessed May 16, 2023.
9. American Thyroid Association. Iodine deficiency. www.thyroid.org/iodine-deficiency/. Accessed May 16, 2023.
10. Levothyroxine sodium [package insert]. Caguas, Puerto Rico: Neolpharma, Inc; 2017. Accessed May 16, 2023.
11. American Thyroid Association. Thyroid hormone treatment in children and adolescents. www.thyroid.org/thyroid-hormone treatment-children-adolescents/. Accessed May 16, 2023.
12. PDR.net. Tapazole (methimazole) dose, indications, adverse effects, interactions. www.pdr.net/drug-summary/Tapazole-methimazole-1493. Accessed May 16, 2023.
13. Tapazole methimazole tablets package insert. Spring Valley, NY: PAR Pharmaceutical Companies, Inc. Accessed May 16, 2023.
14. Eghtedari B, Correa R. Levothyroxine. Treasure Island, FL: StatPearls Publishing; 2023 [Updated 2022 Sep 4]. www.ncbi.nlm.nih.gov/books/NBK539808/.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.





